Abstract
Acrodermatitis continua of Hallopeau (ACH) is a rare and localized form of pustular psoriasis that can lead to irreversible anonychia whereas Jaccoud’s arthropathy (JA) is a rare non-articular condition characterized by a deforming non-erosive arthropathy involving the digits. This case describes the first reported association of these two rare conditions in a 73-year-old Filipino male who was treated topically until remission of ACH. Because calcipotriol/betamethasone ointment works better and faster than clobetasol ointment, it may be considered as a preferred first-line treatment for ACH. This case also highlights the evaluation of joint symptoms in the context of psoriatic arthritis and JA, along with a discussion of its management. A multidisciplinary approach involving dermatology, rheumatology, and physiatry is essential in the care of these two rare conditions.
Keywords
Introduction
Acrodermatitis continua of Hallopeau (ACH) is a rare, inflammatory, pustular dermatosis of the fingers and toes with a chronic and relapsing course. It is characterized by sterile pustules that coalesce to form “lakes of pus” in peri- and subungual areas and lead to scarring and nail plate destruction. 1 The disease always involves the nail and is often limited to one or two digits, extending proximally, with more chronic cases showing osteitis and osteolysis of the distal finger or toe. 2 Similar to other pustular variants, mutations of the IL-36 receptor antagonist (IL36RN) and Caspase recruitment domain-containing protein 14 (CARD14) gene have been found. 2 However, its exact pathophysiology remains unknown. 2
Jaccoud’s arthropathy (JA) is a rare deforming arthropathy of the metacarpophalangeal (MCP) and proximal interphalangeal joints (PIP), wrists, and knees typically seen in lupus. 3 Deformities resemble a rheumatoid hand but involve tendon and ligament laxity rather than erosive arthritis. 3 Despite the characteristic laxity of the joint capsule and ligaments leading to deviation of tendons, the exact mechanism behind its development is yet to be determined. 3
Due to the rarity of ACH and JA, there is an absence of data on epidemiology, thereby making the occurrence of both diseases in a single patient worthy of study.2,3 This case explores two recommended first-line topical treatment options for plaque psoriasis that resulted in symptomatic and cosmetic improvement of ACH. It also highlights the evaluation of joint symptoms in the context of psoriatic arthritis (PsA), along with a discussion of management for JA.
Case report
A 73-year-old Filipino diabetic male patient consulted at the skin clinic of a tertiary hospital in the Philippines for a 4-month history of pain, swelling, and pustulosis of the 3rd, 4th, and 5th digits of the left hand accompanied by finger deformities. He had unsuccessfully tried several courses of antibiotics. On the day of consult, the yellowish-to-greenish nail discoloration led to an impression of green nail syndrome. He was started on a regimen of diluted acetic acid drops once a day, bacitracin ointment twice a day, and mefenamic acid 500 mg thrice a day for the pain. On follow-up after a week, the pain and swelling were only slightly decreased and the subungual discoloration persisted, prompting hospitalization for intravenous anti-pseudomonal antibiotic therapy.
Inflammation, dystrophy, and “lakes of pus” in the nails of the 3rd, 4th, and 5th digits of the left hand were noted (Figure 1(a)). The digits were tender, and the affected fingers resembled the Boutonniere deformity of rheumatoid arthritis (Figure 1(b)). The potassium hydroxide mount, Gram stain, and culture of the blood and pustular lesions were all negative. Bone erosion was likewise absent on the hand X-ray (Figure 1(c)). Apart from the elevated liver enzymes, the baseline blood chemistry test was normal.

Initial presentation. (a) Inflamed, purulent, and dystrophic nails of the 3rd, 4th, and 5th digits of the left hand. (b) Flexion contracture of the PIP joints of the 3rd, 4th, and 5th digits of the left hand. (c) Jaccoud’s arthropathy of the left hand shows a visible deformity with an absence of damage to either bone or cartilage.
The patient had a history of biopsy-proven plaque psoriasis and was lesion-free for over a year. Due to the patient’s history of psoriasis and nail changes with finger deformity on physical examination, he was then diagnosed with ACH and PsA and was subsequently started on clobetasol propionate 0.05% ointment twice a day. After a normal repeat liver enzyme test, methotrexate at 10 mg per week with folic acid was started for the PsA. He was also given tramadol and topical diclofenac for pain relief. Furthermore, the patient underwent physiotherapy and was discharged after 1 week.
On follow-up a month after discharge, the pustules partially dried up but the nails were still thick, crumbled, dystrophic, and onycholytic with dry periungual skin (Figure 2(a)–(c)); clobetasol propionate 0.05% ointment was continued due to the partial improvement seen. Conversely, the flexion deformities of the PIP joints involving the 3rd, 4th, and 5th digits of the left hand remained. Methotrexate was then continued at the same dose, and celecoxib was given for the pain.

(a–c) After 1 month of clobetasol propionate 0.05% ointment: Thick, crumbled, dystrophic, and onycholytic nails, surrounded by xerotic skin.
After 6 months, the pustules were gone and new nails were growing out (Figure 3(a)). After 17 months of daily application of clobetasol propionate 0.05% ointment with two-week breaks in between to prevent atrophy, the nails became brittle and onycholytic (Figure 3(b)), prompting the change to calcipotriol/betamethasone dipropionate ointment once a day. After only 2 weeks on this combination, significantly better cosmetic appearance was achieved (Figure 4(a)). At 4 weeks, the nail plate and the periungual area were free from scales with new normal-looking nails (Figure 4(b)). Since then, there has been no recurrence of pustulosis with continuous improvement of the affected nails, hence discontinuation of treatment.

Evolution of lesions with clobetasol propionate 0.05% ointment. (a) After 6 months. (b) After 17 months.
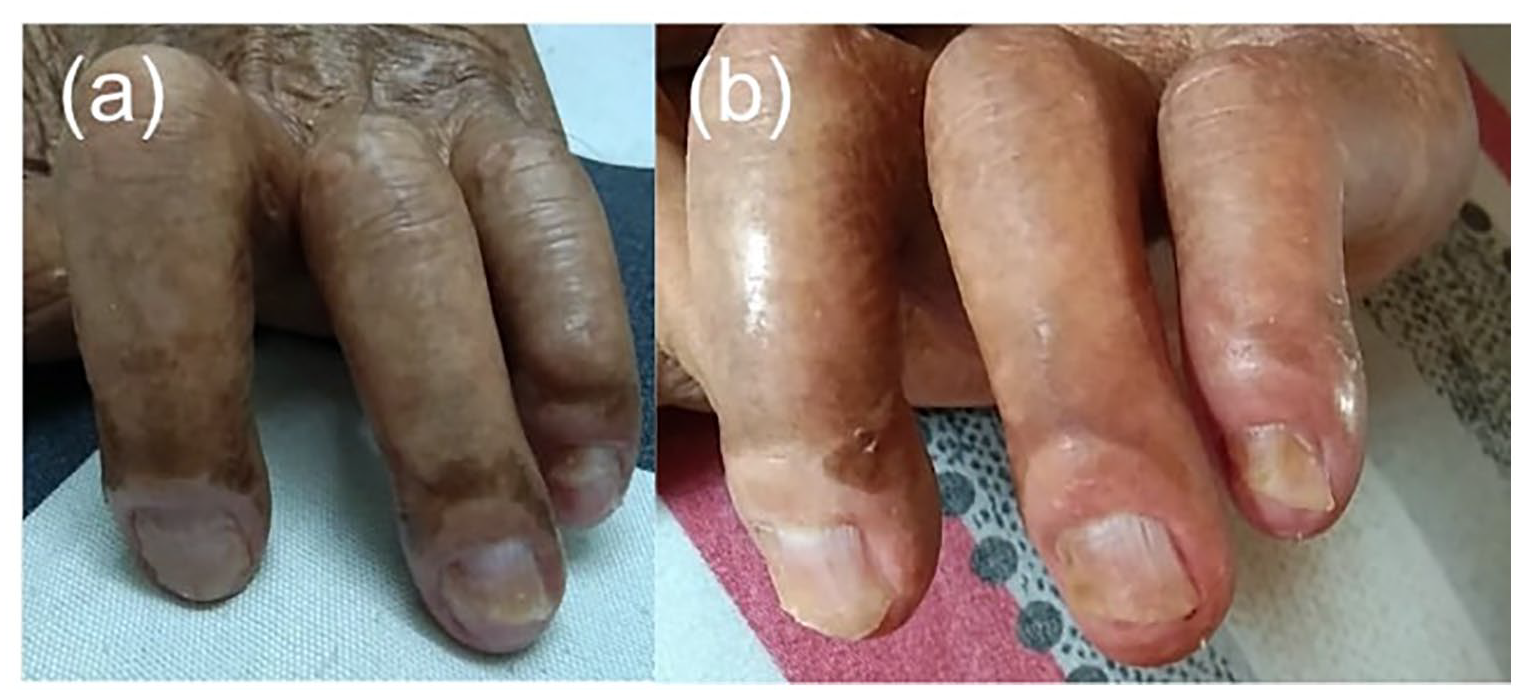
Evolution of lesions with calcipotriol 50 mcg/betamethasone dipropionate 500 mcg ointment. (a) Significantly better cosmetic improvement after 2 weeks. (b) Progressive growth of normal nails without scaling and periungual desquamation after 4 weeks.
Despite 6 months of methotrexate, the painful finger deformities had not improved. On re-evaluation of his reducible deformities with an absence of osteolysis or bone formation on hand X-ray, he was finally diagnosed with JA with subsequent discontinuation of methotrexate. The patient was recommended physiotherapy but has been non-compliant due to logistic reasons.
Discussion
ACH is commonly mistaken for an infection. 4 It presents with tender sterile pustules and erythema on the distal fingers and toes, 5 leaving a sharply defined, shiny erythema with a crusted, keratotic or fissured surface. 2 It involves the nail bed and matrix, leading to onychodystrophy or anonychia. It can also lead to osteitis and osteolysis of the distal finger or toe, causing disability and impairment of quality of life. 6 The patient had chronic painful pustulation of the fingers that was misdiagnosed as pyoderma, which prompted treatment for pseudomonas nail infection. Candidal paroncyhia was also considered. However, workup for any infection was negative.
PsA on the contrary is a rare complication with significant distal phalanx osteolysis. On the hands, it may present as polyarticular, mono/oligoarticular, distal interphalangeal disease, or arthritis mutilans. Arthritis mutilans, the least common form of synovitis, may present with finger flexion deformities and may also manifest as non-articular dactylitis or sausage digit; the hand X-ray may likewise show joint damage.
The patient’s finger deformities were initially diagnosed as PsA. However, upon re-examination, joint space narrowing, bone formation or erosion, and osteolysis were absent on the hand X-ray. Furthermore, the patient failed to meet the cutoff score of at least three points in the Classification criteria for Psoriatic Arthritis (CASPAR) 7 to be diagnosed with PsA. Apart from a history of psoriasis, there was no history of typical psoriatic nail dystrophy, dactylitis, and juxta-articular new bone formation, which ruled out PsA. The patient was then re-evaluated and the Boutonniere deformity-looking fingers were found to be reducible, which led to a diagnosis of JA.
JA, a reversible non-erosive arthropathy involving tendon and ligament laxity, has been associated with PsA, an irreversible erosive arthritis. 8 However, this is the first reported association of ACH, a localized form of pustular psoriasis, and JA where both conditions existed concurrently. Physical therapy and use of an orthotic device are treatment options for JA, which were both recommended to our patient. Soft tissue surgery may also be considered. 3
There is no standard treatment for ACH since its rarity has made treatment options limited, with nail plate involvement implying poor drug penetration. 5 A variety of topical, phototherapy, and systemic treatments for psoriasis have been tried, all with equivocal and inconsistent results; there is also insufficient evidence to determine which treatment is the most effective.6,9 The presence of extracutaneous symptoms such as bone and joint involvement often complicates management, highlighting the importance of a multidisciplinary approach.
Management of ACH should start with the most conservative and least toxic treatment, and an algorithm suggesting topical therapy as first-line treatment followed by systemic agents has been suggested in several studies.6,10 The patient was started on a super-potent topical corticosteroid. The pustules disappeared but brittle onycholytic nails grew out. Since the response was unsatisfactory, he was then shifted to a fixed-dose combination of topical calcipotriol and betamethasone. Calcipotriol magnifies the corticosteroid’s anti-inflammatory, antiproliferative, and immunosuppressive effects while decreasing proliferation and increasing keratinocyte differentiation. Their synergism subsequently led to a better and faster response after only 4 weeks of once-a-day application. Since discontinuation of treatment, there has been no recurrence of pustulation with continuous growth of normal-looking nails, making the treatment a success.
Other topical therapies for ACH include tacrolimus and calcipotriol; phototherapy may be added if response from topical therapy is only partial.9,10 Systemic therapies for ACH include acitretin, methotrexate, and cyclosporine. Failing these systemic agents, biologics such as anti-TNF, IL-12/23 and IL-17 inhibitors may be tried.5,9,10
Since ACH is known to be chronic and recalcitrant,5,6,9,10 our patient’s complete response to topical treatment with a fixed-dose combination of calcipotriol and betamethasone at 4 weeks with no recurrence may provide further evidence for ongoing research. To the authors’ knowledge, this is the second reported case of ACH that was successfully treated with the combined drug with no recurrence after discontinuation. 11 In the era of expensive biologics, the role of topical treatment may still provide a practical and valuable role in ACH. 11 Controlled clinical trials to prove its efficacy and superiority are hereby suggested to provide a stronger level of evidence.
In terms of long-term treatment, studies have shown that maintenance therapy with a fixed-dose combination of topical calcipotriol and betamethasone is safe and effective for as long as 52 weeks when done in a proactive, twice weekly approach. 12
Conclusion
Due to the rarity of ACH and JA, the occurrence of both diseases in a single patient makes this case worthy of study. Because calcipotriol/betamethasone ointment works better and faster than clobetasol ointment, it may be considered as a preferred first-line treatment for ACH. This case also highlights the evaluation of joint symptoms in the context of PsA and JA, along with a discussion of its management. A multidisciplinary approach involving dermatology, rheumatology, and physiatry is essential in the care of these two rare conditions.
Footnotes
Author contributions
All authors contributed equally to the acquisition of data and its analysis, writing, and approval of the final version to be published. All authors agree to be accountable for all aspects of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This study was granted exemption from ethical review by the Rizal Medical Center Institutional Review Board.
Informed consent
The patient in this manuscript has given written informed consent to the publication of his case details including images that illustrated the improvement of his condition.
