Abstract
There are few reports describing adverse events associated with nasopharyngeal swab specimen collection in patients tested for SARS-Cov-2 (COVID-19). Despite the lack of data, providers should be aware of complications associated with swab collection. Instances of nasopharyngeal swab as a syncope trigger are mostly anecdotal and not well described in the medical literature. We present a case of neural reflex mediated syncope associated with the nasopharyngeal swab specimen collection process in a healthy patient undergoing COVID-19 testing prior to elective surgery. This response may be mediated by the trigeminocardiac reflex or via glossopharyngeal nerve stimulation. Less invasive collection practices, such as saliva sampling, may be warranted, particularly in those predisposed to syncopal episodes.
Introduction
Robust pre-procedure testing protocols and guidelines were established early in the SARS-Cov-2 (COVID-19) pandemic to safely resume elective care. 1 As the gold standard for viral respiratory infection testing, nasopharyngeal specimen collection has become common in many hospital and ambulatory COVID-19 screening programs.2,3 Generally considered safe, there have been recent reports in the literature of adverse events associated with nasopharyngeal swabs. 4 Here we describe a case of neurally mediated syncope associated with the nasopharyngeal swab specimen collection process in a patient undergoing COVID-19 testing prior to elective surgery.
Case Presentation
A 73-year-old female with a past medical history of deep vein thrombosis, hypothyroidism, gastroesophageal reflux disease, and rheumatoid arthritis, and no history of presyncopal or syncopal symptoms, presented following syncope during COVID-19 specimen collection by nasopharyngeal swab as part of a universal pre-procedure screening protocol. During the collection process, the patient experienced a pain in her throat and while leaning forward from a seated position to sneeze, she transiently lost consciousness and fell to the ground, resulting in midface injury (Figure 1).
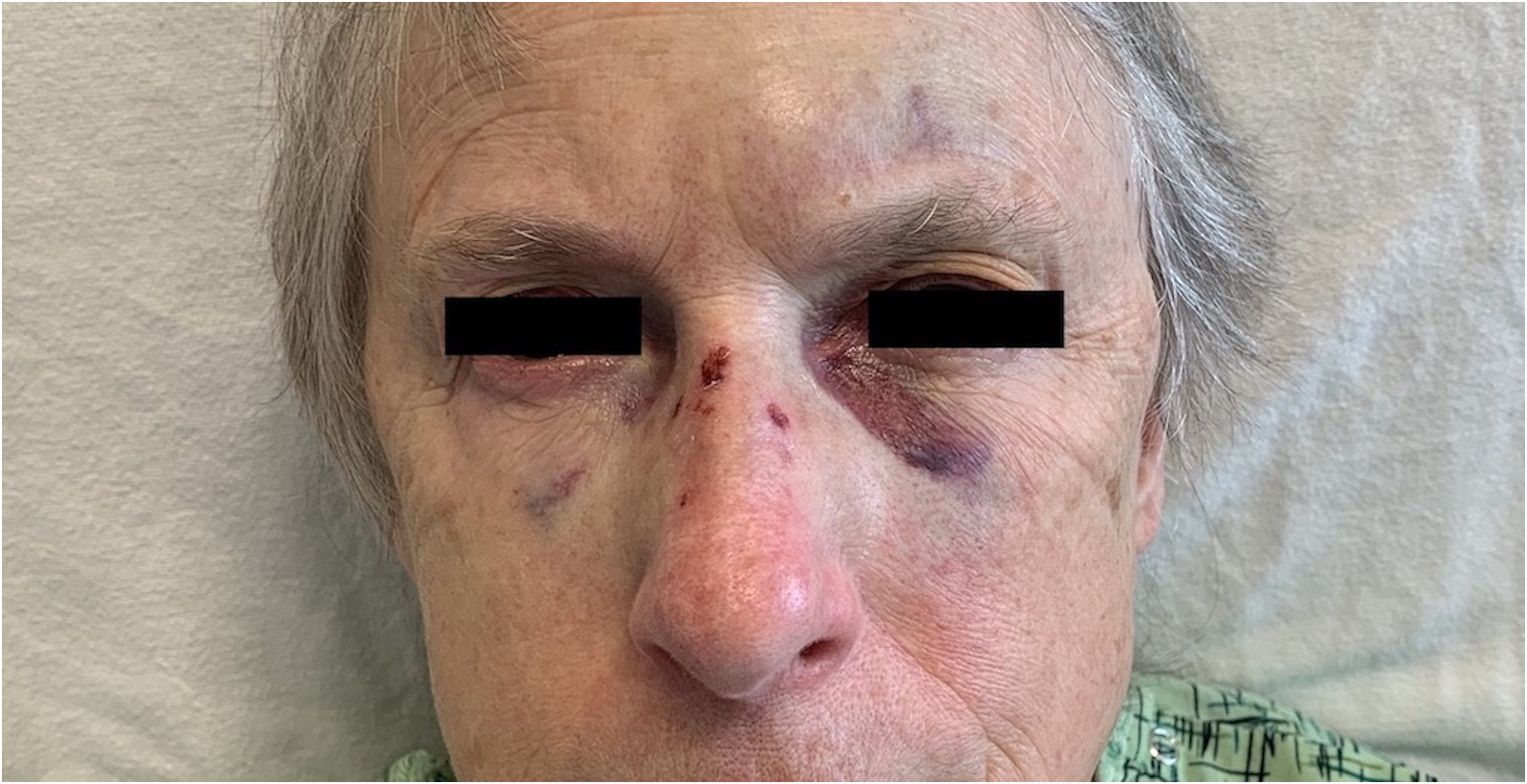
A photograph showing midface trauma two days after a syncopal episode following nasopharyngeal specimen collection for COVID-19 testing as part of a universal pre-procedure screening protocol prior to elective surgery.
The patient quickly regained consciousness and was immediately taken to the ED in the same facility for further evaluation. In the ED, the patient denied prodromal symptoms prior to this episode aside from the reported pain. Laboratory results and orthostatic vitals were both within normal limits. An electrocardiogram showed sinus bradycardia, but was otherwise unremarkable. Computed tomography of the head demonstrated a nondisplaced left nasal bone fracture due to the associated fall with no additional acute pathologic findings (Figure 2).

Computed tomography of the head which demonstrates a nondisplaced left nasal bone fracture (white arrow).
Electrophysiology was consulted and concluded the patient experienced an isolated, neurally mediated, non-cardiogenic syncopal event and was discharged after stabilization and reassurance. She had no previous diagnosis of COVID-19 and received the first and second dose of the mRNA-1273 (Moderna) vaccine three and four months prior to the syncopal episode, respectively. A negative nucleic acid amplification COVID-19 test was returned and the patient underwent scheduled cataract surgery two days later.
Discussion
Neural reflex mediated syncope, which classically includes vasovagal syncope, situational syncope, and carotid sinus syndrome, is a common cause of transient loss of consciousness. 5 Many triggers of neural reflex mediated syncope have been identified, but the exact pathogenesis is less clear and appears to be quite heterogeneous. Known triggers include pain, fear, long periods of standing, coughing, swallowing, and even micturition.6,7 This list is by no means exhaustive, and in many instances of neural reflex mediated syncope no inciting trigger is identified. Instances of syncope following nasopharyngeal swab are mostly anecdotal and not well documented in the medical literature. We presented a case of neural reflex mediated syncope associated with COVID-19 testing by nasopharyngeal swab.
Syncopal events have been described in a small percentage of patients undergoing rhinologic manipulation procedures. Radvansky et al reported 8 out of 4973 patients experienced a syncopal event during a minimally invasive endoscopic in-office procedure. 8 A recent study identified neural reflex mediated reductions in heart rate in 30.2% of patients undergoing nasoendoscopy, but no instances of syncope among the 53 enrolled patients. 9 The exact mechanism of neural reflex syncope involving the nasopharynx is not well understood. One possible mechanism associates the trigeminocardiac reflex (TCR) with syncope. The classic TCR mechanism suggests mechanical stimulation of the trigeminal nerve or its peripheral branches results in activation of the cardioinhibitory parasympathetic neurons of the vagus nerve. In recent years, the TCR was discovered to be more complex than originally thought and the nasal-cardiac reflex was recognized as a subtype of the classic TCR. Of concern, there are reports of cardiac arrest induced by the activation of the nasal-cardiac reflex. 10 A recent case report described an episode of asystole during nasopharyngeal swab specimen collection for COVID-19 testing. 11 Unlike the healthy patient we presented, the patient in the aforementioned report was sedated and ventilated while inpatient for complicated COVID-19 infection, which itself has been associated with syncope.11,12
Alternatively, a syncopal response could be triggered by swab-induced stimulation of the glossopharyngeal nerve. Syncope has been reported in patients with nasopharyngeal carcinoma, where the tumor irritates the glossopharyngeal nerve causing a cascade of events ultimately resulting in increased vagal tone. 13 Similar to the patient described in this report, syncope in patients with nasopharyngeal carcinoma was found to be associated with throat or facial pain immediately preceding the episode.13–15 Syncope with pain has been more associated with recurrent glossopharyngeal neuralgia, but the pain described by our patient and the depth with which nasopharyngeal swabs are inserted suggests a similar mechanism of isolated neurally mediated syncope with neuralgia. While the mechanism cannot be completely elucidated, healthcare providers collecting nasopharyngeal samples should remain vigilant of this potential complication.
In a recent meta-analysis, saliva sampling was found to have similar sensitivity and be less costly when compared to nasopharyngeal swabs. 2 As demonstrated by this case, saliva sampling may also be a safer alternative to nasopharyngeal swabs, particularly in patients predisposed to syncopal episodes. Guidance from public health and regulatory authorities is needed as patients return for routine care requiring COVID-19 screening and as hospitals assess existing protocols.
Conclusion
Complications of nasopharyngeal swabs are important to consider when implementing universal COVID-19 screening protocols. Less invasive collection methods may be warranted. This case highlights one of the potential unintended, albeit rare, consequences of the nasopharyngeal swab collection procedure.
Footnotes
Statement of Informed Consent
Written informed consent was obtained from the patient for the information and photographs to be published in this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Ethical Approval
Not applicable, because this article does not contain any studies with human or animal subjects.
Informed Consent
Not applicable, because this article does not contain any studies with human or animal subjects.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
