Abstract
Objective
To evaluate the utility of point-of-care COVID-19 testing for identifying infected patients in an otolaryngology practice.
Study Design
Retrospective review of 947 patients tested with a point-of-care nucleic acid amplification test for SARS-CoV-2 (Abbott ID Now).
Setting
Tertiary otolaryngology clinic setting from July to November 2020.
Methods
Tests were characterized by provider-specified indication (symptomatic, preprocedural, and universal), subspecialty, provider type, and contemporaneous regional COVID-19 positivity rate, defined as 12%. Positive results were further classified as true or false positive (TP or FP) based on repeat polymerase chain reaction testing wherever available, and true positivity rates were compared among groups by multiway chi-square and Fisher’s exact tests. FP rates within 48 hours of a TP result were also evaluated to assess for batch contamination.
Results
A total of 947 SARS-CoV-2 nucleic acid amplification tests were performed, yielding 9 TPs (0.95%) and 5 FPs (0.53%). TP rates were significantly different by testing indication, with higher rates among symptomatic patients (P = .012; vs universal, odds ratio = 7.86 [95% CI, 1.27-83.52]; vs preprocedural, odds ratio = 4.91 [95% CI, 0.79-52.17]); by subspecialty (P = .011), as driven by higher positivity rates in laryngology; and by encounter, with higher rates among advanced practice practitioners than physicians (P = .002; odds ratio = 9.97 [95% CI, 2.11-51.16]). TP rates were not significantly different during periods of uncontrolled local outbreak (P = .660). FP rates were not significantly higher within a 48-hour window of a TP (P = .192).
Conclusion
Point-of-care COVID-19 nucleic acid amplification tests in an outpatient otolaryngology clinic identified a low TP rate (<1%) with most cases being clinically suspected. Laryngology and advanced practice practitioner encounters may have higher positivity rates.
Level of evidence: 3.
Keywords
The novel coronavirus strain (2019-nCoV) first identified in January 2020 precipitated the spread of coronavirus disease 2019 (COVID-19) globally.1,2 Initial descriptions commonly highlighted symptoms of fever, cough, and shortness of breath, as well as rarer symptoms of throat pain, loss of smell, loss of taste, and hearing loss.3-5 A concern with COVID-19 is that asymptomatic or presymptomatic patients may account for 15.6% of disease transmission.6,7 Transmission of the virus, SARS-CoV-2, occurs through respiratory droplets and aerosol particles, where the virus can remain viable for several hours. 8
Otolaryngology clinics are uniquely stressed during this pandemic due to the overlapping nature of typical otolaryngology complaints and COVID-19 symptoms, the anatomy closely examined by otolaryngologists, and the frequent need for in-office procedures with potential for aerosol generation. 9 Notably, the first documented physician fatality in the pandemic was that of an otolaryngology practitioner from Wuhan, China, in January 2020, and otolaryngologists had the highest specialty infection rate during the early pandemic.10,11 The examination of the upper respiratory tract, which harbors particularly high viral loads of SARS-CoV-2 in symptomatic and asymptomatic patients, is an essential part of otolaryngology visits that put practitioners at risk.4,12 To ensure the safety of otolaryngologists, telehealth visits have been employed in an effort to reduce transmission, 13 but this is not universally feasible given the importance of examination of the upper airway in the diagnosis, management, and treatment of otolaryngologic complaints. When telehealth is not possible, other recommendations for workforce protection include using personal protective equipment during aerosol-generating procedures, such as N95 respiratory masks, gown, gloves, and negative pressure face shields.14,15 Despite these measures, risks remain to examining providers, the staff, and patients in clinic.
Preappointment screening of patients through temperature checks, epidemiologic history, and clinical symptoms has been recommended to limit transmission through clinical visits. 11 With finite testing resources, it is imperative to utilize COVID-19 tests in an efficient manner. 16 Universal presurgical COVID-19 testing and evaluation of surgical urgency 17 have been recommended as a feasible way to safely conduct essential surgery while minimizing the impact on quality of care. 18 However, due to the larger volume of outpatient ambulatory appointments and frequent need for minor procedures in this setting, universal previsit testing may prove to be a barrier in access to otolaryngologic care.
There are multiple testing modalities that can be used for detection of COVID-19: nucleic acid detection (eg, reverse transcription polymerase chain reaction [RT-PCR] or other nucleic acid tests), rapid antigen testing, and serologic testing. 19 Currently, viral detection of COVID-19 via RT-PCR of a bronchoalveolar lavage, sputum specimen, or nasopharyngeal swab 20 is considered the most reliable method. 21 RT-PCR testing has an estimated sensitivity of 70% from a nasopharyngeal swab, 22 a false-negative rate of 54%, 23 and a minimal turnaround time of 3.5 hours to several days. 24 In contrast, testing options at the point of care (POC) that can be performed by clinical personnel include the rapid antigen test. 25 However, its sensitivity of 32% makes it an ineffective POC rule-out test. 26 While serologic antibody testing can be used to detect antibodies to SARS-CoV-2, IgM and IgG seroconversion in patients to detectable levels takes time, reaching high levels in the second or third week of illness, and does not reflect active or transmissible illness, making this a poor choice for POC testing. 21
On March 27, 2020, the Abbott ID Now COVID-19 test was one of the first POC tests approved by the Food and Drug Administration for detection of COVID-19 from nasal, nasopharyngeal, or throat swabs of individuals clinically suspected for COVID-19 within a week of symptom onset, 27 and it can produce a positive result in as fast as 5 minutes. 28 The test uses an isothermal nucleic acid amplification technique, which has a high percentage positivity agreement with other emergency use authorized RT-PCR COVID-19 detection methods, such as the Cepheid Xpert Xpress SARS-CoV-2 method and the Roche Cobas SARS-CoV-2 assay at medium and high viral loads (each 100%). 29 However, these POC tests have extended run times of 45 minutes and 3.5 hours, respectively, as compared with the 5-minute run time of the Abbott ID Now COVID-19 test. 28
Over time, rapid antigen testing has become a viable POC testing option. However, these tests are reliant on high viral loads for detection, with specificities of 76% at median viral load levels and 8.8% at low viral loads.30-32 Since patients presenting to otolaryngology clinics are less likely to have multiple clinical symptoms of COVID-19 and thus a lower viral load if infected, the utility of the test at lower loads is paramount for reducing transmission. Due to the development timeline—specifically, antigen tests were approved a month after the Abbott ID Now COVID-19 test was approved 33 —and to institutional constraints, nucleic acid amplification tests (NAATs) were the POC test of choice for this study.
This article summarizes our experience with use of this POC test (Abbott ID Now COVID-19) in an outpatient otolaryngology clinic. Specifically, we evaluated whether the test positivity rate is affected by a selective approach versus a universal screening protocol, the subspecialties within the field, and the ambient incidence of COVID-19.
Materials and Methods
Study Participants
After review and approval from the Northwestern Institutional Review Board, a retrospective review was conducted of all patients tested with the Abbott ID Now COVID-19 rapid NAAT at a tertiary medical center outpatient otolaryngology clinic from July 2020 to November 2020. Patients were evaluated across subspecialties in the clinic: general otolaryngology, rhinology, head and neck surgery, laryngology, facial plastic surgery, otology, and sleep surgery. No patient diagnoses were excluded from analysis. Patients received their COVID-19 tests at their clinic visits or prior to in-office procedures. Dry nasopharyngeal swabs were administered by trained medical assistants, nurses, physician assistants, and physicians in accordance with the instructions for the Abbott ID Now COVID-19 rapid NAAT. In the clinic, universal precautions were taken to limit transmission: patients wore surgical masks during the encounters except during testing or procedures. Clinic staff wore surgical or N95 masks and exercised universal precautions at all times.
Outcome Measures
Thirty-one providers (18 otolaryngologists, 13 advanced practice practitioners [APPs]) individually selected indications for testing patients. Providers were stratified by subspecialty—4 general otolaryngology, 7 rhinology and skull base surgery, 7 head and neck surgery, 2 laryngology, 3 facial plastics surgery, 7 otology, and 1 sleep surgery—and role (MD vs APP). Four providers (2 general otolaryngology, 1 rhinology and skull base surgery, 1 head and neck surgery) opted for universal testing of all their patients prior to examination. All other providers opted for preprocedural testing, including but not limited to nasal or laryngeal endoscopy, tracheostomy tube exchange, in-office turbinate reduction, plastic surgery procedures, or anything with significant exposure of the patient’s nose or mouth. 34 Upon obtaining history, some patients with symptoms of COVID-19 (eg, fever, cough, fatigue, myalgias, headache, sore throat, new-onset smell loss, and abdominal pain 35 ) were also selected for symptomatic testing. Test results were thus stratified into 3 categories per the rationale of administration: preprocedural, symptomatic, and universal testing. In instances where the indication for testing a patient could be placed into multiple categories, priority for categorization was given to the universal testing category, followed by symptomatic tests and procedural indications. Tests were classified by regional contemporaneous COVID-19 test rate positivity. The period between November 6 and 26, 2020, was classified as uncontrolled outbreak, and the rest of the study period was classified as below threshold, defined by regional positivity being above and below the Illinois Department of Public Health threshold of 12%. 36
Positive results were further classified as true or false positive (TP or FP), with FP defined as a negative polymerase chain reaction test result within 48 hours of a positive result per the POC Abbott ID Now COVID-19 NAAT. Only TP was considered for analyses of test positivity.
Statistical Analysis
A multiway chi-square test and, for rare outcomes, a Fisher’s exact test were performed to compare testing and positivity rates based on testing indication, provider subspecialty and type, and contemporaneous regional positivity rate. Where relevant, significant results (P < .05) were tested with individual 2 × 2 Fisher tests to determine the pairwise differences driving the significance.
All statistical tests were conducted with R version 3.6.3 (R Foundation for Statistical Computing).
Results
There were 11,902 visits to the otolaryngology clinic during the study period: 1144 general otolaryngology, 2519 rhinology and skull base surgery, 1492 head and neck surgery, 796 laryngology, 1375 facial plastics surgery, 4288 otology, and 288 sleep surgery. A total of 951 Abbott ID Now NAATs were administered in the clinic. When possible, patients were retested with traditional RT-PCR testing (43%) within 1 day after an initial positive result. Of the 951 administered tests, 947 yielded valid results: 14 positives (1.47%), of which 9 were deemed TP (0.95%) and 5 FP (0.53%; Table 1 ).
Results Stratified by Otolaryngology Subspecialty.
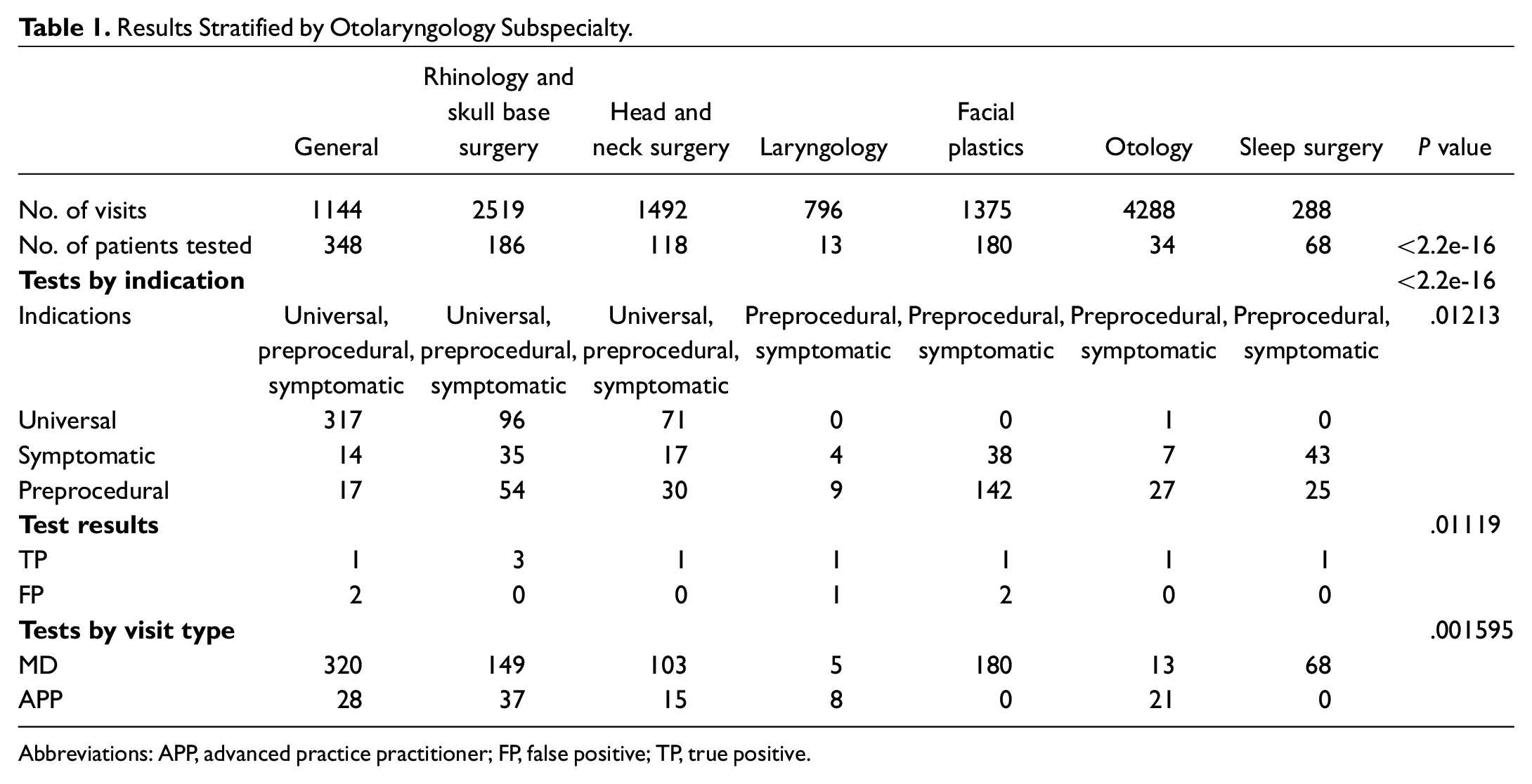
Abbreviations: APP, advanced practice practitioner; FP, false positive; TP, true positive.
Of the 947 valid results, 485 patients were classified under the universal testing criteria, of which 2 (0.41%) were TPs and 2 (0.41%) were FPs. There were 304 patients who were classified under the procedural testing category, of which 2 (0.66%) were TPs and 1 (0.33%) was an FP. The remaining 158 patients were classified as testing for symptomatic indications, of which 5 (3.16%) were TPs and 2 (1.27%) were FPs. There were significant differences in true test positivity among these testing indications (P = .012). Pairwise analysis revealed significantly higher true test positivity between symptomatic and universal testing (P = .011; OR = 7.86 [95% CI, 1.27-83.52]). There was also significantly higher true test positivity among symptomatic patients as compared with preprocedural patients (P = .049; OR = 4.90 [95% CI, 0.79-52.17]; Figure 1 ). There was no significant difference in positivity rates between universal and procedural testing (P = .641). Calculating the positive predictive value (PPV) by testing indication, we found the PPVs to be 50%, 66.7%, and 71.4% for universal, procedural, and symptomatic testing, respectively.
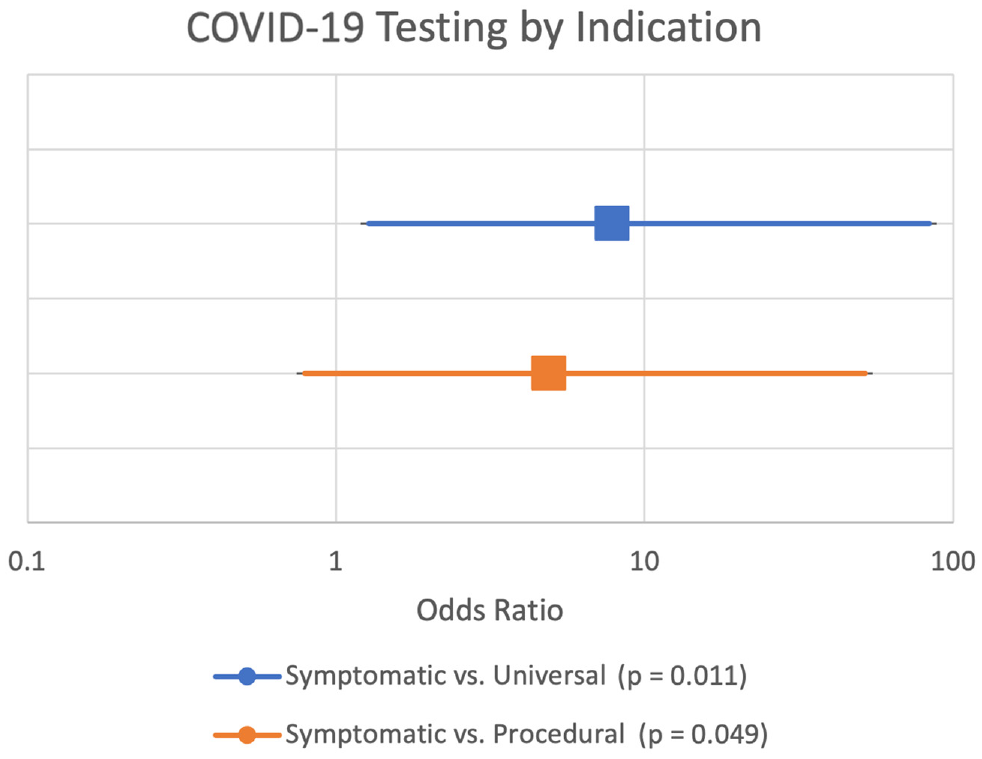
The odds ratio (95% CI) of a true positive result for symptomatic and preprocedural testing indications as compared with the universal testing indication as a reference. Results of pairwise Fisher’s exact test analyses.
Of the 947 valid results, the patients were categorized into 7 subspecialties: general otolaryngology (n = 348), rhinology and skull base surgery (n = 186), head and neck surgery (n = 118), laryngology (n = 13), facial plastics (n = 180), otology (n = 34), and sleep surgery (n = 68). There was a significant difference in testing indications (P < 2.2e-16) and positivity rates (P = .011) by subspecialties. On individual pairwise testing, there were significantly higher rates when the laryngology practice was compared with general otolaryngology (P = .004, OR = 59.61 [95% CI, 2.91-3612.79]), rhinology (P = .035, OR = 10.77 [95% CI, 0.821-104.67]), head and neck surgery (P = .026, OR = 20.16 [95% CI, 0.98-1252.29]), and facial plastic surgery (P = .012, OR = 30.81 [95% CI, 1.50-1899.42]; Figure 2 ). Positivity rates for APP encounters (n = 109) as compared with physician encounters (n = 838) were also significantly different, with higher positivity rates in APP encounters (P = .002; OR = 9.97 [95% CI, 2.11-51.16]).
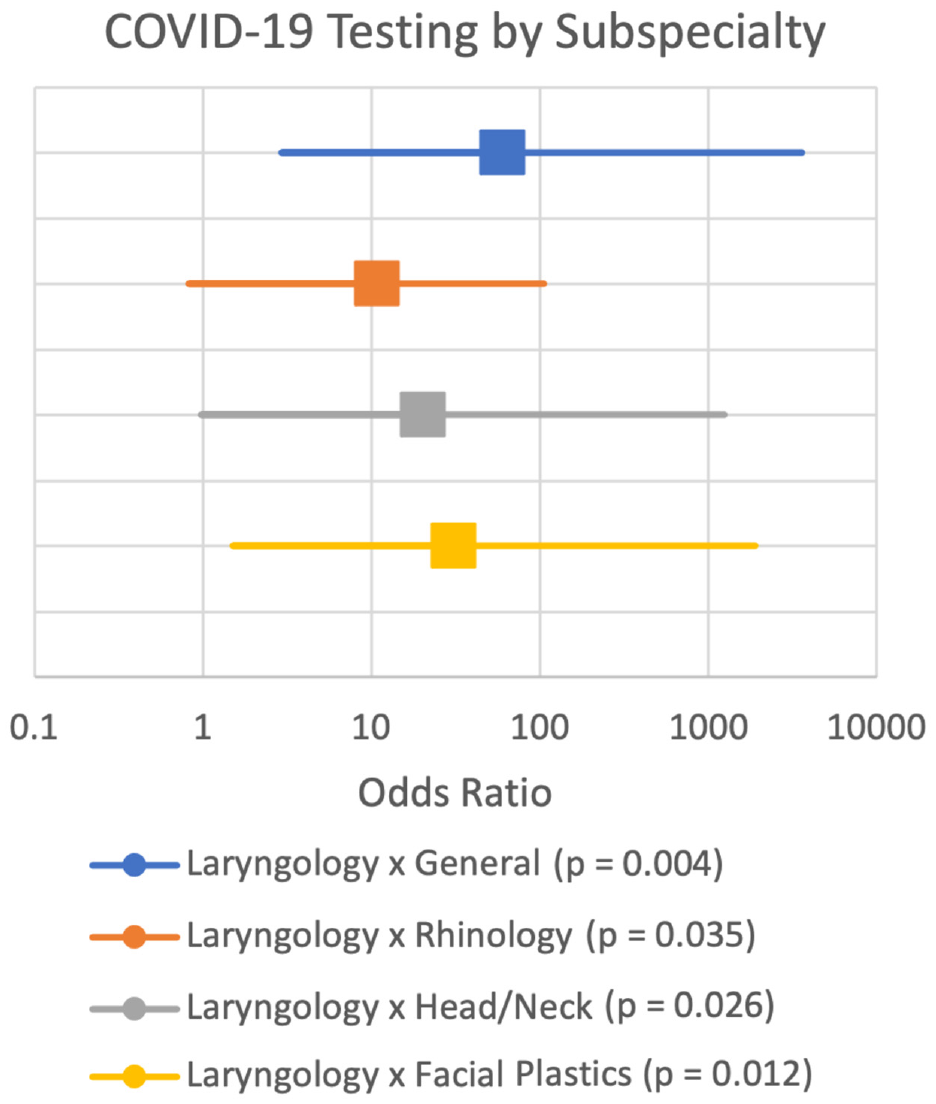
Significant individual pairwise comparisons of the odds ratio (95% CI) for a true positive result in laryngology as compared with general otolaryngology, rhinology, head and neck surgery, and facial plastics. Results of pairwise Fisher’s exact test analyses.
During the time frame of the study, the city of Chicago, where this study was carried out, had periods where the outbreak was considered uncontrolled or below threshold based on clinical test positivity. On our POC testing platform, the positivity rates during a time of uncontrolled outbreak were not significantly greater than times under the threshold (P = .660). There was no significant difference of FP rates within or outside a 48-hour window of a TP result (P = .192).
Discussion
This study is the first to compare the utility of POC testing protocols for outpatient otolaryngology visits based on indication, subspecialty, provider type, and regional incidence of COVID-19. We compared positivity rates using distinct testing indications for outpatient otolaryngology visits and found that testing for COVID-19–suggestive symptoms yielded the highest positivity rate (3.16%) and had the highest PPV (71%) among indications. Universal and procedural testing yielded positivity rates <1% but nonetheless did discover some unanticipated positive cases. TP results occurred in all subspecialties and in visit to APPs and physicians. Visits with APPs and the laryngology clinic as compared with visits to physicians and other subspecialties, respectively, had significantly higher true test positivity, although significant differences existed in testing indications by provider type and subspecialties. There was no difference in positivity rates during times of uncontrolled outbreak, and the likelihood of FP did not increase if the test was made within 48 hours of a TP test.
There is significant clinical utility to implementing a rationalized testing policy to implement personal protective equipment and room isolation procedures to protect staff and patients. The study findings suggest that obtaining a patient history has a 5- to 8-fold increased odds for identifying COVID-19 as compared with universal testing. Nonetheless, some unanticipated cases were detected through the universal and preprocedural testing strategies, but the benefits of identifying these rare unanticipated cases (<1%) must be weighed against the associated testing utilization and cost. Since there was no significant difference in clinic positivity rates during a period of uncontrolled outbreak, symptomatic testing should remain the indication of choice regardless of locoregional COVID-19 incidence. The availability of POC testing may help confirm the presence of COVID-19 in patients with concerning symptoms that bypassed the previsit screen. Given that COVID-19 has some overlap with otolaryngologic symptoms, including cough, throat pain, loss of smell, loss of taste, tinnitus, and hearing loss, 3 testing patients with clinically suspicious histories yielded the highest test positivity.
In our study, APP visits had significantly higher positivity rates than physician visits. This may be explained by differences in testing indications given that none of the APPs utilized the universal testing protocol. However, it may be explained by the acuity of illness seen by our APPs. Forty-five percent of patients were seen in the APP clinic in <7 days from referral, as opposed to 29% of patients who were evaluated by physicians. Thus, APPs evaluated patients with acute-onset illnesses that may have been hard to distinguish from COVID-19 due to nonspecific symptoms, such as sore throat, cough, and smell loss.
We found that our laryngology clinic had significantly higher positivity rates than other subspecialties. Similar to the findings of the APPs, this may be due to decreased utilization of testing for universal and procedural testing in our laryngology practice but may reflect the nature of patient complaints that present to the laryngology clinic, such as nonspecific globus sensation, laryngeal irritation, and hoarseness—all of which can present for patients with COVID-19.37,38 However, this result could be explained by the relatively higher proportion of patients who were tested for symptomatic indications as compared with other subspecialties.
In our study, we found that over a third of our positive tests were FPs. Although POC FPs do not confer risk for transmission, the significant disruption of clinical operations and induced patient anxiety have to be considered seriously. We hypothesized that this may have been due to test batch contamination; however, given the lack of a significant difference in FP rates in the 48 hours following a TP test, test batch contamination was an unlikely cause. Other studies have shown low to no FPs when using the Abbott ID Now COVID-19 tests.28,39 Although not statistically significant, the PPVs of the test were related to clinical suspicion for COVID-19, yielding values of 71.4% for symptomatic testing, 66.7% for procedural testing, and 50% for universal testing. This finding follows from Bayes theorem wherein the predictive capability of a test is related to the prevalence of the disease in a population.40,41 In this clinic population, the lower pretest probability of infection due to prescreening of patients increases the likelihood of FPs.
There are a few limitations to this study. Due to its retrospective nature, the inability to conduct repeat testing on all positive cases—just 43% of the positives were retested—may obscure the true FP rate. Since providers chose their testing indications, patients were not randomized to testing protocols, which means that the conclusions drawn regarding causality must be done cautiously. Additionally, since this is a single-center study, it may not reflect the dynamics at other institutions or geographies.
Overall, this study describes the implementation of a POC testing protocol for COVID-19 in an otolaryngology clinic during the COVID-19 pandemic. While the implications for this study are most directly relevant to otolaryngology practices, it can help elucidate efficient test resource usage in other outpatient practices as well. With the current COVID-19 vaccine rollout, case prevalence and the risk of patient to health care worker transmission are currently decreasing in the United States. However, the risk of COVID-19 may well persist due to vaccine hesitancy and the development of new variants, which may even cause the pandemic to continue in a seasonal cycle.42,43 As of this writing, India and Brazil continue to report high daily new case loads, and there are reports of a third-wave resurgence in Africa.44-46 Even highly vaccinated countries such as the United Kingdom and the United States are experiencing a resurgence of cases. 47 Our study provides estimated test positivity rates for otolaryngology practices using a POC testing platform to help providers decide the value of the testing strategies studied here. Individual practice decisions on whether to implement any of these testing strategies will vary by immune status and risks posed by COVID-19 to the otolaryngology providers and their patients.
Conclusion
COVID-19 presented a unique challenge to otolaryngology clinicians, who had to balance the risk of transmission with the necessity to provide care. In this article, we demonstrate a testing strategy to limit COVID-19 transmission in outpatient clinics.
Authorship Contributions
Disclosures
Footnotes
This article was presented at the AAO-HNSF 2021 Annual Meeting & OTO Experience; October 3-6, 2021; Los Angeles, California.
