Abstract
Purpose
Fracture Liaison Services (FLS) have been developed as a coordinated, multidisciplinary programs designed to improve the identification and management of patients with fragility fractures, including hip fractures. This study aims to evaluate the impact of coordinator based FLS on medical treatment compliance and mortality in patients following hip fracture. Specifically, it seeks to evaluate the impact of routine follow-up post discharge on these outcomes.
Methods
Comparative retrospective cohort of following hip fracture patients for one year after surgery. First group with the complete FLS treatment and protocol and second group with partial FLS protocol without the routine clinical follow-up after discharge. Main clinical outcomes were osteoporosis medication compliance and morality rates.
Results
347 participants, 182 (52.4%) without a coordinator follow-up and 165 (47.6%) with a coordinator follow-up. Patients with coordinator follow-up had better medication compliance 1 year following hip fracture (77% vs 39%). First year mortality rate was 11% and 13% accordingly without statistical significance.
Conclusion
This study found that patients in an FLS with coordinator follow-up had better clinical outcomes, receiving more timely medication recommendations and showing higher treatment adherence, highlighting the value of coordinated follow-up in long-term care.
Keywords
Introduction
Hip fractures are a significant public health concern, particularly in the elderly population, due to their high morbidity, mortality, and impact on quality of life. The incidence of hip fractures increases with age, and given the global trend of an aging population, the burden of these injuries is expected to rise dramatically in the coming decades. Approximately 1.6 million hip fractures occur worldwide each year, and this figure is projected to double by 2050 due to demographic shifts and increased longevity. 1 The mortality rate following a hip fracture is alarmingly high, with estimates suggesting that 20-24% of patients die within one year of the injury. 2 Despite the availability of effective pharmacologic treatments to prevent subsequent fractures, the medical treatment rate for osteoporosis following hip fracture is low. 3 To address these challenges, Fracture Liaison Service (FLS) has been developed as a coordinated, multidisciplinary program designed to improve the identification and management of patients with fragility fractures, including hip fractures. FLS programs aim to close the gap in care by ensuring that patients receive appropriate osteoporosis screening and treatment, thereby reducing the risk of future fractures. Importantly, FLS has been shown to improve treatment compliance and reduce mortality among fracture patients.4,5 Several models of FLS have been suggested with coordinator based as the most common. Routine Follow-up following discharge by the coordinator adds costs and time. Our FLS model is coordinator based with two main steps. The first is an in-house evaluation and recommendation provided to the patients during their initial hospital stay (including a treatment recommendation for osteoporosis medication) and the second is routine follow-ups 6-12 weeks following discharge to evaluate treatment initiation; when required the follow-up is up to one year. During hospitalization (first stage) all patients are screened for metabolic and hormonal imbalance (blood tests), dietician consultation and recommendation, daily physical therapy, fall prevention education and screened and educated for osteoporosis by a clinical pharmacist. This study aims to evaluate the impact of coordinator-based FLS on medical treatment compliance and mortality in patients following a hip fracture. We hypothesize that the involvement of a coordinator enhances adherence to osteoporosis treatment and contributes to reduced mortality rates.
Patients and Methods
We conducted a comparative retrospective analysis among patients recovering from a hip fracture following local IRB approval. All patients were treated at a single medical center. The patients were treated in the orthopedic department and were managed by the FLS. Eligible participants were patients aged 50 years and older who sustained a low-energy hip fracture. Patients were excluded if they were younger than 50 years, if the fracture resulted from high-energy trauma, if the fracture was pathological (ie, not attributable to osteoporosis, such as in the context of malignancy), or if they had severe dementia that precluded a reliable assessment of adherence to osteoporosis treatment. Patients were divided into two groups: one that was not followed by the coordinator after discharge as part of the FLS (second stage), and another that was managed under the full FLS protocol (historical), including both in-hospital evaluation and routine follow-ups. Part of the latter’s data had been published before. 6 In Israel, Osteoporosis medical treatment is given by the general practitioner. First group was comprised of all osteoporotic hip fracture patients admitted to the orthopedic department in our medical center between 1.1.2021 to 31.12.2021. During these dates the FLS was completing only the first step and not conducting routine follow-up of the patients (second step). These patients were contacted during 2023 and were inquired about the first year of recovery. Patients were contacted by telephone and inquired about parameters such as post-surgical complications, osteoporosis treatment adherence, supplements regimen and recurrence of fractures. Treatment adherence was defined as positive if the patient reported administration of at least one dose of the prescribed medication within 12 months following surgery. Optional prescribed drugs were Teriparatide (RxNorm 1 435 115), Romosozumab (RxNorm 2123190), Denosumab (RxNorm 993452) and Zoledronic acid (RxNorm 77655)). Data surveyed was compared to historical group of patients following a hip fracture during June 2018 to June 2019 who were managed by the FLS including both stages with routine follow-up following discharge. Collected variables were demographic, surgical and post-surgical and metabolic blood tests. Morbidity (complication, fractures) and mortality were noted and osteoporosis treatment evaluated for comparison. Primary outcome was the impact of FLS service on medicational regimen adherence, and the secondary outcome was mortality rates.
Statistical Analysis
Sample size estimation was based on the expected difference in adherence to osteoporosis treatment between the study groups. Assuming that the intervention group included at least 160 participants with an adherence rate of 73%, 6 with a one-sided significance level of 5% and a statistical power of 80%, and further assuming that approximately 130 patients would be included in the non-intervention group, a statistically significant difference between groups would be detected if adherence in the non-intervention group were 60% or lower. According to the literature, adherence rates are around 40%, and therefore the study was expected to achieve higher power than originally calculated.
Chi-Square test was used to compare categorical variables, such as gender distribution, mortality rates and Medication adherences. Continuous variables like age and biochemical levels, were calculated using T-test to compare group means. The Fisher-Freeman-Halton test was applied to compare the distribution of surgical procedures, which involved multiple categories. P value <0.05 was applied for all statistical analysis.
When analyzing mortality, patients who could not be contacted and whose status remained unknown were excluded from the analysis. Furthermore, patients confirmed as deceased but without an exact date of death were classified as having died more than one year after surgery.
The manuscript was prepared according to the STROBE guidelines.
Results
Demographic and Surgical Data
Demographics of Patients With Hip Fracture

Abbreviations: TSH thyroid stimulating hormone, PTH para-thyroid hormone, CRE creatinine, CA calcium, P phosphate.
Reference ranges: Hemoglobin (Male 13.5-175, Female 12-15.5), CA (2.1-2.65), Vitamin D (>20), CRE (Male 60-110, Female 45-90), TSH (0.4 – 4), PTH (1.6-6.9), P (0.8-1.5).
aIndependence status according to the American Society of Anesthesiologists.
Osteoporosis Medical Treatment
Overall, the compliance rate across both groups was 60% in the first year of follow-up, improving to 68% in the second year. In the first year after fracture, adherence differed significantly between groups (P < 0.001): 124 patients in the coordinator group (77%) were adherent compared to 49 patients in the non-coordinator group (39%) (Figure 1). In the coordinator group, 122 (74%) patients initiated treatment within 1 year, with a mean time to initiation of 80 days (SD 32). In contrast, among 62 patients in the non-coordinator group treated by general practitioners, 6 (9.7%) began treatment preoperatively, 43 (69.4%) within 1 year, and 13 (21%) after more than 1 year, yielding a mean initiation time of 314 days (SD 156) (Figure 1). The difference between groups was statistically significant (two-sided P < 0.001). This was partly explained by differences in medical recommendations (P < 0.001), as 41 patients in the non-coordinator group (22.5%) did not receive any medication recommendation, compared to only 5 patients (3%) in the coordinator group. Percentage of patients receiving OP medication and timing for starting Tx
When focusing on the reason for non-adherence to medical treatment we found differences between the groups: In the coordinator follow-up group, all 31 patients who responded to inquiries about medication non-adherence declined the prescribed regimen. In contrast, among 53 patients in the non-coordinator follow-up group who provided explanations for non-adherence, 13 (24.5%) declined the regimen, while 40 (75.5%) did not receive any clarification regarding medication necessity (Figure 2). Vitamin D and calcium supplements continuous intake was noted in 71% of participants in the non-coordinator follow-up group. We do not have information of the other group for comparison. Overall, 41 (12%) patients had a prior fracture preceding the femoral neck fracture examined in this study, with 80% of them presented in the earlier study group. Number of patients not receiving OP medications and reason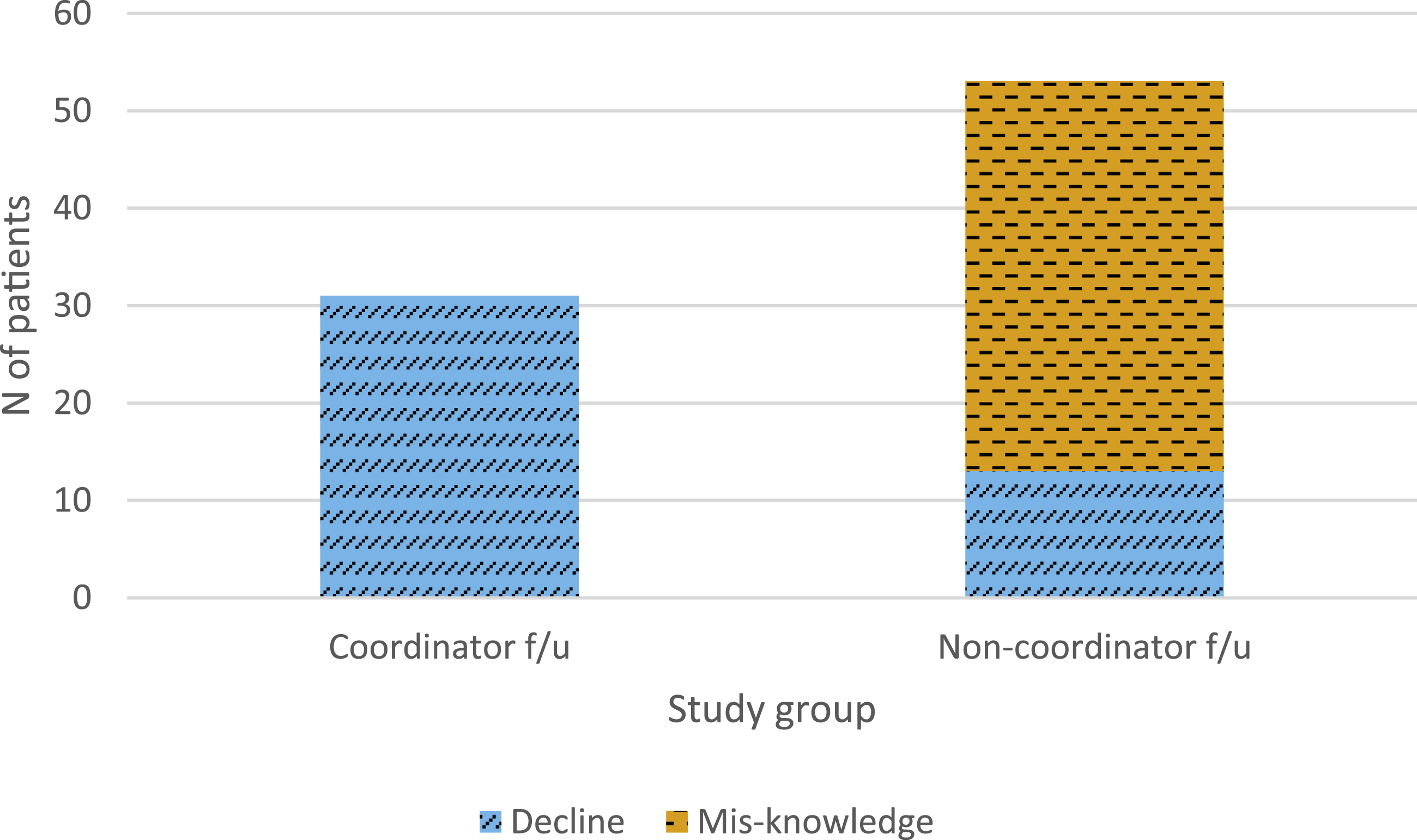
Adverse Outcomes
20 patients with unknown status were removed from the cohort. For the remaining 326 patients, a 1-year mortality analysis was performed. A crude comparison of 1-year mortality between the groups did not reveal a statistically significant difference (P = 0.646). In the coordinator follow-up group, 19 patients (11%) died within one year of surgery, while in the non-coordinator follow-up group, 22 patients (13%) died during the same period.
A Kaplan–Meier survival analysis performed on 323 patients did not indicate a higher risk in either group; however, the difference was not statistically significant (hazard ratio = 1.00, log-rank P = 0.989). Three patients who were confirmed dead lacked an exact date of death and were therefore excluded from the analysis. The results are shown in Figure 3. Kaplan Meier survival analysis of one year mortality of both groups
In the non-coordinator follow-up group, 32 patients (17.5%) experienced an additional fracture during the first postoperative year, while 5 patients (3%) only in the coordinator follow group. However, Comparison of the incidence of subsequent fractures within one year after the initial surgery between the two groups could not be done due to study limitations. Among 99 patients with available data on treatment adherence within the first postoperative year, 1-year refracture rates did not differ significantly between those who adhered to a medication regimen (15.5%) and those who did not (13%) (P = 0.712).
The analysis revealed some unexpected protective factors associated with lower mortality. Examining the data using an univariable analysis, patients with preoperative anemia had a lower mortality rate (6.8%) compared to those with normal hemoglobin levels (15.7%). Notably, younger age was associated with increased postoperative complications, with patients who experienced complications having an average age of 72 compared to 78 for those without complications. A multivariable logistic regression impaired the statistical significance of anemia, leaving age as the main factor impacting mortality (P = 0.001). The average age of patients who died within 1 year was 84, higher than those who survived beyond that time (average age 77). Gender and the occurrence of an additional fracture within 1 year did not significantly impact mortality.
Complications Rates
Complications
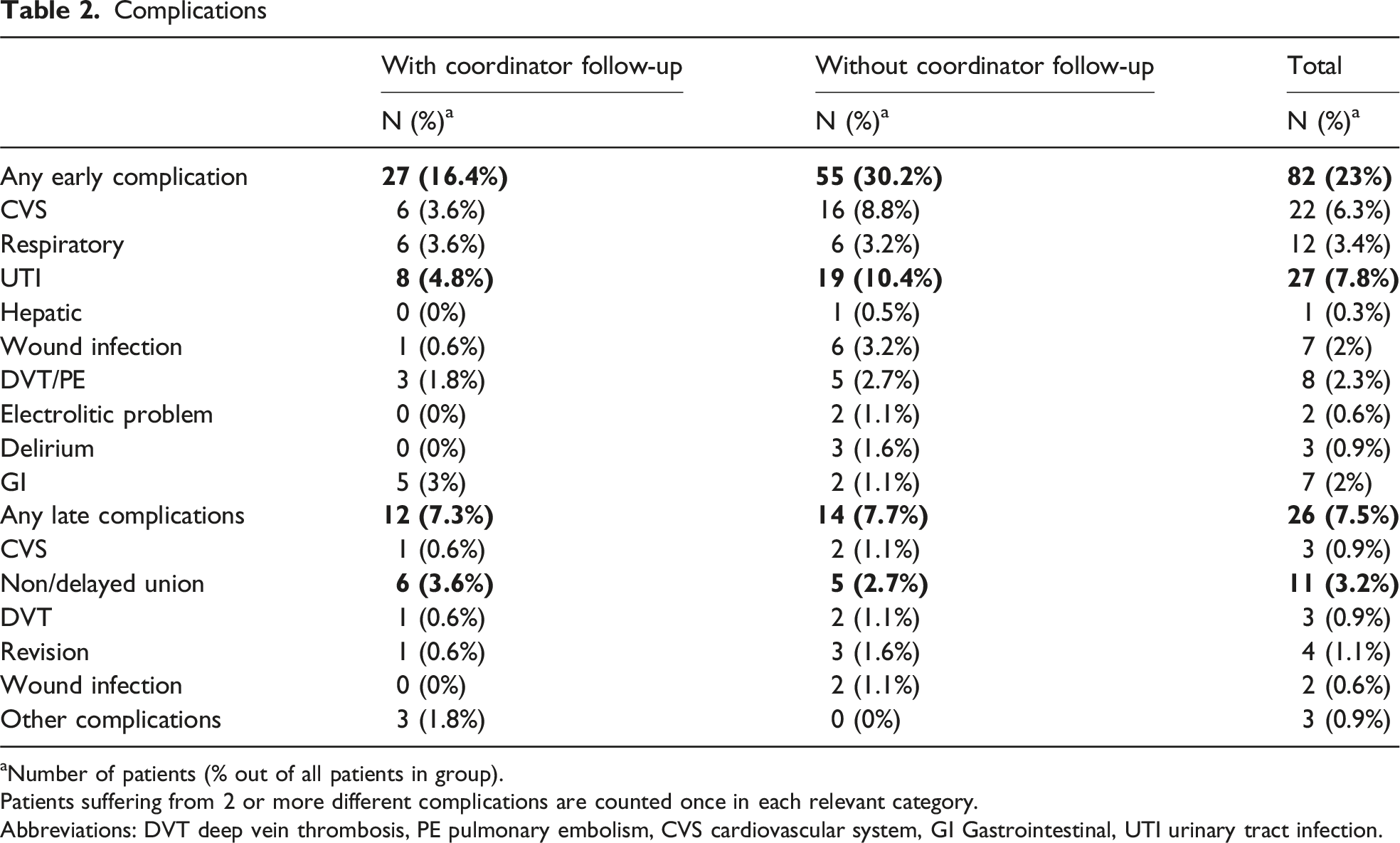
aNumber of patients (% out of all patients in group).
Patients suffering from 2 or more different complications are counted once in each relevant category.
Abbreviations: DVT deep vein thrombosis, PE pulmonary embolism, CVS cardiovascular system, GI Gastrointestinal, UTI urinary tract infection.
Discussion
This study, involving 347 participants diagnosed with hip fracture which participated in FLS treatment and follow-up, found that coordinated follow-ups significantly improved osteoporosis management and outcomes. Patients’ mean age is consistent with local epidemiology of femoral hip fractures. 7
As we assumed, FLS coordinator did prove to positively affect various aspects of patients’ post operation period: patients with coordinator follow-ups had better medication adherence (77% vs 39%) compared to those without coordinator. Additionally, those in the coordinator group-initiated osteoporosis treatment more promptly (mean 80 days vs 314 days). Overall, the data suggests that a structured follow-up system improves treatment adherence and reduces fracture-related complications. These outcomes align with previous literature investigating FLS benefits: several studies have demonstrated the effectiveness of FLS in enhancing compliance with osteoporosis treatment among hip fracture patients. Our former study found that 73% of patients received osteoporosis medication within three months post-surgery following FLS intervention, significantly improving compliance rates. 6 Similarly, González-Quevedo D et al reported that anti-osteoporotic drugs were more frequently prescribed after FLS implementation (79.3% vs 12.5%), with a notable increase in adherence to treatment (51.7% vs 30.2%). 8 A systematic review and meta-analysis performed by Yan C et al confirmed that FLS significantly improves medication adherence in patients with hip fractures. 9 Additionally, a study by Naranjo A et al highlighted that long-term persistence with anti-osteoporosis medication was optimal in patients managed through FLS, with a proportion of days covered (PDC) > 80% in 55.7% of patients. 10 These findings collectively underscore the positive impact of FLS on improving compliance and adherence to osteoporosis treatment in hip fracture patients, thereby supporting the integration of FLS into routine clinical practice for better management of osteoporosis. In this study we emphasized the importance of routine follow-up following discharge to improve patient compliance to medication. The patients who declined medication in the non-coordinator follow-up group were not all educated on the importance of medical treatment. Although both groups were evaluated and educated on osteoporosis during hospitalization for surgery, a difference in understanding the importance of the medical treatment was found during the follow up. The routine follow-up has left more time for re-education and improve compliance for medical treatment.
In the current study, we could not compare fracture rate between the two groups due to study limitations. However we found that medical adherence on its own did not significantly affect re-fracture rates. This may stem from the limited information we were able to gather about adherence and fractures incidence, or from the fact that follow-up visits-with their emphasis on patient education and close monitoring-helped patients identify and address problematic aspects of their daily routines.
Studies indicate that within one year, approximately 8.4% of patients sustain a subsequent fracture, which increases to 32.5% after five years. 11 The implementation of an FLS has been shown to significantly reduce the re-fracture rate. A systematic review and meta-analysis by Wu CH et al found that patients managed under an FLS had an unweighted average re-fracture rate of 6.4%, compared to 13.4% in those receiving usual care. 12 Another study by Nakayama A et al demonstrated that FLS implementation was associated with a 30% reduction in any re-fractures and a 40% reduction in major re-fractures over three years. 13 Additionally, a cohort study in Sweden reported an 18% lower risk of recurrent fractures in hospitals with FLS compared to those without. 14
The complication rate following an osteoporotic hip fracture is a significant issue as well, as the World Hip Trauma Evaluation (WHiTE) study reported complications within the first 120 days post-hip fracture, including wound infection (3.1%), chest infection (6.3%), urinary tract infection (5.0%), and VTE (venous thromboembolism) (1.8%). 15 We found higher early complications rate in the non-coordinator follow-up group, despite no significant difference in care of those patients during hospitalization. It is important to note that complications were obtained from electronic medical records for both groups and questionnaires filled by the patients of the non-coordinator group only, which may result in a collection bias.
Overall, 12% of patients had preoperative fractures, with the majority observed in the early research group, reflecting the increasing awareness of osteoporosis. This trend is further highlighted by the observation that a higher percentage of patients in the later research group had normal vitamin D levels, with 49% in the earlier group compared to 65% in the latter group.
The mortality rate following a hip fracture is notably high. Published literature describes 1-year mortality rates that range from 20% to 30%, with variations depending on patient demographics and comorbidities. For example, a study in the UK reported a 1-year mortality rate of 20.5%, while another study in Ireland found a similar rate of 20.8%.16-18
The implementation of a Fracture Liaison Service has been shown to significantly reduce mortality rates in patients with hip fractures. According to a systematic review and meta-analysis by Li N et al, FLS programs are associated with a reduction in mortality, with an odds ratio of 0.65 for mortality (95% CI: 0.44-0.95, P = 0.03) in studies comparing outcomes before and after FLS implementation. 19 Another study demonstrated that the introduction of an FLS was associated with a 16% reduction in 1-year mortality (hazard ratio of 0.84, 95% CI: 0.77-0.93).20,21 Our study supports the implementation of FLS to reduce mortality (11% vs 13%), however the difference was not statistically significant, possibly due to data gaps. Older age did seem to be a risk factor.
Limitations
The main limitations of this research involve data collection and its reliability. First, comparative parameters were not identical between the control and historical groups. As the historical group’s data was collected two years ago without consideration of a future comparative study, some information available for the control group was missing from the historical group and therefore could not be used for statistical analysis. Second, as data was collected only from patients who could be contacted, a potential selection bias exists. For the historical group, it is possible that the more severe patients, for whom the coordinator would not have made a difference, were unable to respond and thus were not included in the statistical analysis. For the control group, patients who recovered successfully without the coordinator service may have been uncontactable. Third, because the data relied on the recollections of patients or caregivers, often regarding events that had occurred more than a year earlier, there is a risk of recall bias, with information potentially being incomplete or imprecise. Finally, exact dates of subsequent fractures were unavailable for the majority of patients, which prevented us from conducting a time-to-event analysis using Kaplan–Meier curves; therefore, we were limited to reporting crude second fracture rates only.
Conclusion
This study highlights important differences in clinical outcomes between patients managed through a FLS with coordinator follow-up and those without the continuous follow-up. Significant difference in medication recommendations and adherence between the groups underscores the potential role of coordinator follow-up in optimizing long-term care, as more patients in the coordinator follow-up group received timely medication recommendations and adhered to treatment.
Footnotes
Author Note
Dr. Tamar Fisher Negev is an equal contributor with the first author Nitzan Israeli Eilon.
Ethical Considerations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
The study was approved by the Hadassah Hebrew University medical centers ethical committee. HMO-0363-22.
Consent to Participate
Informed consent was required for the telephone interview only.Conflicts of interest: Nitzan Israeli Eilon, Tamar Fisher Negev, Elad Eilon, Manal Alami, Rivka Israel and Noam Olshinka declare that they have no conflict of interest. Omer Or received a support grant for the FLS project by the Israel foundation of osteoporosis and bone disease (IFOB).
Author Contributions
This work was performed as a part of an MD thesis of the student Nitzan Israeli Eilon, The Faculty of Medicine, The Hebrew University in Jerusalem, Israel. Nitzan Israeli Eilon contributed to the study Conception and design, data curation, formal analysis, investigation, methodology, validation, visualization and drafting and revising the manuscript. Dr Tanar Fisher Negev contributed to the study Conception and design, data curation, investigation, methodology and drafting and revising the manuscript. Elad Eilon contributed to the study data curation, formal analysis, investigation, validation and visualization. Manal Alami contributed to the study Conception and design, data curation, investigation. Rivka Israel contributed to the study Conception and design, data curation, investigation. Dr Noam Olshinka contributed to the study Conception and design, investigation, methodology and revising the manuscript. Dr Omer Or contributed to the study Conception and design, data curation, formal analysis, investigation, methodology, validation, visualization and drafting and revising the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
