Abstract
Introduction
The retrospective study evaluated the clinical and radiological outcomes of conservative treatment for type II odontoid C2 fractures in octogenerians. The study aimed to assess the clinical outcomes and quality of survival of patients treated using conservative methods. Additionally, the study sought to define radiological outcomes, fracture healing success and the development of complications in correlation with clinical outcomes.
Materials and Methods
Patients aged ≥80 with dens C2 fracture were fixed with a hard cervical collar for 6 weeks, followed by early mobilization. Patients showing delayed fracture healing on computed tomography (CT) scan were subsequently immobilized in a soft neck collar for additional 6 weeks. The follow-up CT scan was then performed with consequential rehabilitation. Patients with nonunion of the C2 on the follow-up CT scan and clinical symptoms were contraindicated for physical rehabilitation for cervical spine till next CT scan after another 12 weeks. Clinical and radiographic evaluations were performed during follow-up visits, with a median follow-up was 109 days, with the range extending from 1 day to 1 year.
Results
In total, 33 patients were included in the study and were followed for 1 year. The 30-day mortality rate was 21.2%, and between 30 days and one year post-treatment, it was 18.2%. Mortality was higher during the study period in displaced fractures (>2 mm; 9 out of 16 patients died) compared to non-displaced fractures (≤2 mm; 4 out of 17 patients died). The Japanese Orthopaedic Association (JOA) score remained unchanged between admission (mean 16.9; SD ± 0.5) and the end of follow-up (mean 16.9; SD ± 0.5; P > 0.05), the Visual Analogue Scale (VAS) score showed improvement from values measured upon admission to the hospital (mean 7.97; SD ± 1.33) to values measured at the end of follow-up (mean 1.58; SD ± 1.62; P < 0.001) and the Neck Disability Index (NDI) showed a statistically significant difference between admission (mean 41.3; SD ± 14.92) and the end of follow-up (mean 14.29; SD ± 4.65; P < 0.001). The standard measurement of Posterior Atlantodental Interval (PADI) had an average value of 18.6 (range 16-22 mm) and primary bony union of odontoid fractures occurred in eleven cases (33.3%), while six patients (18.2%) had fibrous union with minimal clinical difficulties.
Conclusion
This study demonstrates the safety and efficacy of conservative treatment for odontoid fractures in octogenerians and underscores the critical role of conservative management in a polymorbid elderly population.
Introduction
Fractures of the axis (C2) are the most common isolated fractures of the cervical spine 1 in patients older than 65 years, comprising approximately 5-20% of all cervical spine fractures.2-5 In patients over 80, C2 fractures represent the majority of all cervical spine fractures, with an incidence of up to 60%,6,7 often combined with atlas (C1) injuries.8,9 The most typical fracture of C2 is the type II odontoid fracture according to the Anderson and D'Alonzo classification,2,10-12 with an increasing incidence due to demographic changes. 13 Injuries in the geriatric population typically result from low-energy extension mechanisms in the setting of advanced degeneration of the upper cervical spine and low bone quality in the area of the odontoid base.2,14-18 Delayed diagnosis or failure of conservative therapy can lead to gross dislocation with instability and neurological complications. 19 Prior studies suggest similar mortality rates for both operated and non-operated patients, yet surgical intervention often involves higher morbidity. 19 Treatment options for type II fractures include both conservative and surgical approaches, however, patient age, comorbidities, bone quality, and segmental degeneration contribute to the ongoing debate over optimal management, especially in older patients who may have increased surgical risks. Clear indications for choosing between conservative or surgical treatment are not yet established. 2
This retrospective study aimed to evaluate the clinical and radiological outcomes of conservative treatment of type II odontoid fractures according to Anderson and D'Alonzo classification in the geriatric population over 80 years at our institution. The study aimed to accomplish the following: firstly, to evaluate the clinical outcomes including mortality and quality of life of surviving patients (using VAS, JOA and NDI scores) treated by conservative methods, and secondly, to define radiological outcomes, fracture healing success, and the development of complications in relation to clinical outcomes.
Materials and Methods
This single center retrospective study assessing the effectiveness of conservative treatment of dens fractures in octogenarians, was conducted from January 2016 to June 2021 in University hospital (tertiary center). Patients were identified by reviewing hospital admissions for odontoid fractures in octogenarians within this period. All patients provided written informed consent upon admission, and the data were retrospectively collected from medical records. The study was performed with the approval of the institutional ethics committee of the hospital.
During the study period, a total of 34 patients (21 women, 13 men) aged 80 years and older with a mean age of 86 years (range 80-99 years) were treated for injuries. Of these, 33 conservatively treated patients were included in the study, as 1 patient underwent surgery. Inclusion criteria were defined as follows: age 80 years and older, Anderson and D'Alonzo type II odontoid fracture, normal neurological findings, ASA (The American Society of Anesthesiologists) risk IV, V, dislocation assessed by posterior atlanto-dental interval (PADI) over 15 mm. Conversely, exclusion criteria for the study were defined as: pathological fracture, manifested neurological deficit, ASA risk I, II, III, PADI dislocation less than 15 mm. Patients with ASA risk levels I, II and III, neurological deficit or PADI dislocation less than 15 mm were indicated for surgery. The simultaneous presence of other types of cervical fractures was not an exclusion criterion. In our cohort, we proceeded conservatively even in the presence of primary gross displacement (PADI under 15 mm) without further progression, if the patient was contraindicated for surgical intervention based on ASA classification or absence of neurological deficit.
Patients were admitted to our department through the acute trauma admission of the hospital for the acute phase treatment. All patients underwent standard CT examination to assess the type and size of fracture dislocation, as well as neurological and internal examination with ASA risk determination. Patients were then immobilized with a hard cervical collar, and if there were no contraindications present (hemodynamical instability, fever, anemia requiring blood transfusion therapy, decompensated internal comorbidities), early mobilization was initiated on the second day after admission under the supervision of certified physiotherapist. The early mobilization encompassed verticalization, sitting and respiratory exercises. The cervical spine remained immobilized during physical rehabilitation. Follow-up anteroposterior (AP), lateral and open-mouth X-ray projection examinations were conducted during hospitalization, 2-3 days after verticalization. In case of worsening findings, CT scan was also performed. If the patient developed a neurological deficit, experienced pain significantly limiting verticalization, or gross dislocation with PADI under 15 mm during follow-ups, surgical treatment was chosen. Subsequent follow-up appointments of conservatively treated patients were scheduled at 3, 6 weeks, 3 months, 6 months, and 1 year post-injury. Post-discharge check-ups at 3 weeks included AP, lateral and open-mouth radiographs. At 6 weeks after discharge, all living patients underwent CT examination and dynamic cervical spine X-ray. If patients showed delayed fracture healing on CT at 6 weeks, a follow up CT was indicated after the next 6 weeks (i.e. 3 months after discharge). The subsequent follow-ups at 3, 6 and 12 months respectively consisted either of CT scan if the fracture showed non-union features on the previous CT scan or X-ray if the fracture was healed on previous radiographs. Bony union was diagnosed if trabecular bone spanned the fracture on CT. Otherwise, patients were classified as having nonunion using evaluation through CT and dynamic X-rays, which showed no pathological motion between the fracture fragments, based on these findings, this was considered fibrous union. The stability of the fractures was assessed based on the CT scans as well as dynamic X rays. The hard collar was worn by the patient for at least of 6 weeks (no longer than necessary because of prevention of ulcers development) and if the fracture was assessed as stable on dynamic X rays the hard collar was switched for soft collar with subsequent mobilization including verticalization, physiotherapy of all extremities, however the cervical spine remained immobilized. When patients showed healed fracture on CT the soft collar was removed.
Fractures were classified using the Anderson and D'Alonzo, 10 Roy-Camille, 20 and White and Panjabi 21 schemes. Clinical outcome assessment used the JOA (Modified Japanese Orthopaedic Association) score 22 and VAS (Visual Analog Scale for Pain) interval measured upon admission to the hospital and at the time of fracture healing, defined by radiograph, with some patients’ scores assessed at the final clinical follow-up. The pain severity VAS used in this study was measured on a 10-cm scale ranging from “no pain” (0 cm) to “worst pain” (10 cm), no patient had cognitive deficit impairing their judgment. The ASA score was determined by an internist to assess the risk of surgical treatment for the patient. Functional ability assessment of the patient was evaluated using the NDI (Neck Disability Index) questionnaire completed by patient upon admission and at the time of fracture healing. 23 Fracture healing was monitored using X-ray and CT scans 24 at intervals during hospitalization, of 3, 6 weeks, 3 months, 6 months and 1 year. Nominal values are expressed as mean and standard deviation. Two-tailed paired t test was used for statistical evaluation of clinical outcomes of JOA, VAS and NDI with significance level P value <0.05. For NDI, only data collected from surviving patients were included for the statistical analysis.
Results
Comorbidities Prevalence Among Patients. Data are Expressed as Absolute Values.

One patient in this study was chosen for posterior fixation by the Goel-Harms, thus this patient was not included among the 33 conservatively treated patients. The patient was indicated for surgery due to unstable fracture of C2, Anderson D’Alonzo II, Roy-Camille type II, displacement size 4 mm, two side C1-C2 subluxation, PADI 17 mm, ASA III, without neurological deficit.
The average follow-up time was 109 days (range 1 day to 1 year; SD ± 106.65 days), in which eight patients had a follow-up duration of approximately three months. During the study period, 13 patients died. Within 30 days since trauma admission, seven patients died (including four during hospitalization, three due to cardiac arrest and 1 due to respiratory failure), representing a mortality rate of 21.2%. Between 30 days and 1 year, six patients died, corresponding to 18.2% mortality rate. (Figure 1). All deceased patients succumbed to internal medical conditions. In patients with displaced fractures greater than 2 mm, 9 out of 16 patients died during the study period. In patients with non-displaced fractures under 2 mm, 4 out of 17 patients died during the study period. Mortality during follow-up expressed in absolute counts and percentages in two intervals: during the first month and from 30 days to 1 year.
The clinical status of patients assessed using the JOA score remained unchanged for all 33 patients (mean 16.9; SD ± 0.5) from admission and at the end of follow-up (mean 16.9; SD ± 0.5; P > 0.05) (Figure 2). Pain assessment using the VAS score showed improvement in 33 patients from admission (mean 7.97; SD ± 1.33) to the end of follow-up (mean 1.58; SD ± 1.62; P < 0.001 (Figure 3). NDI was initially evaluated in 33 conservatively treated patients. Upon admission, three patients had severe scores (25-34 points), and 30 patients had complete scores (over 34 points). The final NDI value was assessed at the time of fracture healing in 17 patients. At the end of follow-up, nine patients scored in the mild range (5-14 points), and eight in the moderate range (15-24 points). There was a statistically significant difference between admission (mean 41.3; SD ± 14.92) and at the end of follow-up NDI values (mean 14.29; SD ± 4.65; P < 0.001) (Figure 4). The statistical significance was assessed only in the 17 patients for whom both the initial and final values were known. Clinical assessment before and after treatment using Japanese Orthopaedic Association score (JOA). Data are expressed as mean ± SD. We did not observe a statistically significant difference before (dark blue) and after (light blue) treatment in terms of clinical status. Visual analog scale (VAS) for pain quantification before (dark blue) and after (light blue) follow up. Data are expressed as mean + − SD. Statistical significance is indicated as follows: ***P < 0.001. Clinical assessment evaluation using neck disability index (NDI) before (dark blue) and after treatment (light blue). Data are expressed as mean + − SD. Statistical significance as follows: ***P < 0.001.


Fracture Type Assessment is Conducted Using Anderson D´Alonzo, Roy-Camille, White – Panjabi Classifications. Data are Expressed as Absolute Numbers.
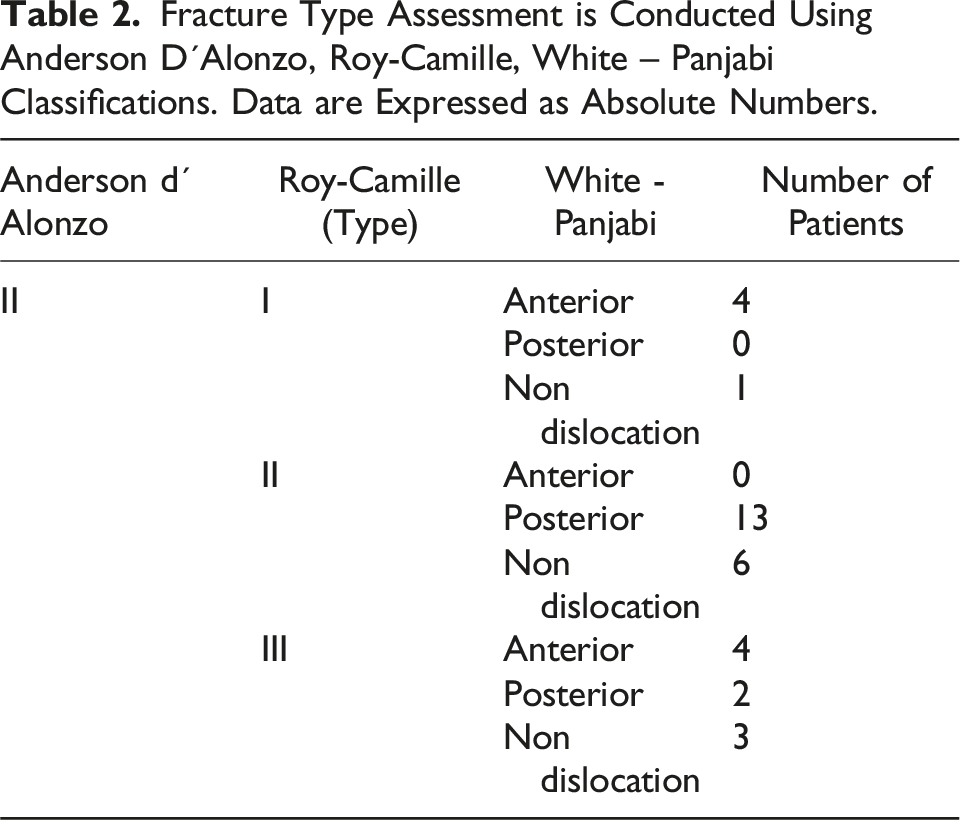
Characterization of Fracture Dislocation Using Anderson D´Alonzo and White-Panjabi Classifications. Fractures With Dislocation Equal to or Greater Than 2 mm Were Considered Dislocated. Data are Expressed as Absolute Counts as Well as Mean ± SD.

Discussion
Odontoid C2 fractures represent a significant medical problem, especially in the frail elderly population over 80 years old. The incidence of odontoid fractures is increasing with demographic changes. Treatment decisions for fractures in the geriatric population are highly individualized due to numerous severe comorbidities, reduced patient cooperation, decreased bone quality, and other local anatomical complications.11,26,27 In our study, we retrospectively evaluated the effect of conservative therapy in octogenarians. The average age of patients in our sample was 86 years, with a predominance of women.
The mortality rate showed that 21.2% died within 30 days, which aligns with other authors reporting a 30-day mortality of 14-15%.14,28 Interestingly, we observed lower mortality between 30 days and 1 year (18.2%), while global sources report a higher mortality (37.5%). 14 This difference was likely due to the size of the sample and the causes of injury, as our sample did not include injuries from high-energy mechanisms. 14 According to meta-analysis 5 that included twelve studies with a total of 730 patients, eleven studies reported mortality. The overall reported mortalities ranged from 20% to 50%, which well corresponds to the overall mortality in our cohort, where a total of 39.4% individuals died during the 1-year follow-up period. However, these meta-analyses typically include younger patients and those receiving surgical treatments, unlike our study.5,29
In our cohort, we observed that 17 patients (51.5%) had minimal (<2 mm) or no displacement. Among patients with displacement under 2 mm, seven (21.2%) died. This included two patients (6.1%) with no displacement and five patients (15.2%) with displacement under 2 mm. These data are fully consistent with published literature, where observed mortality was significantly higher in displaced fractures (>2 mm) at 40% compared to patients without displacement (<2 mm) at 11%. 29 None of the patients in our cohort died from the primary diagnosis, but rather from comorbidity complications. During hospitalization, four patients died (12.1%). This hospitalization mortality aligns with recently published data,28,30 which reported hospitalization mortality rates of 15%, i.e, 6.9% in cohorts of similarly aged patients over 80 years old. The difference in mortality may be attributed to the geoethnic specifics of the studied population and the size of the sample. Comparing surgical and conservative treatments, meta-analyses show no significant difference in overall mortality.5,31 However, these studies include younger age groups, as well as octogenerians only, 28 and do not show a significant difference between conservative and surgical solutions. Furthermore, there is no significant difference in 1- and 5-year mortality between patients treated conservatively or surgically. 32 According to Honda et al, 30 overall hospitalization mortality was similarly low in both conservative treatment and surgical approach (anterior, posterior, and combined) groups, though surgical technique specifics were not provided.
Although treatment selection criteria for C2 dens fractures remain somewhat unclear, surgical intervention is generally indicated in cases of neurological deficit, atlantoaxial instability, unstable dens fractures (PADI <15 mm), and compromised circulatory stability defined by ASA criteria. 14 These criteria were strictly evaluated in relation to each individual patient. Among our patients, a total of 21 cases met at least 1 criterion for dens fracture surgical fixation but were contraindicated for surgery due to internal comorbidities, however none of the 21 patients further progressed in dislocation nor developed neurological symptomatology.
Clinically significant complications of C2 dens fractures include the risks of developing cervical myelopathy, odontoid nonunion, and fracture displacement progression.1,19,29 Recent studies33 identified advanced age, conservative therapy, and type II fracture as major risk factors for odontoid nonunion, while direct anterior screw fixation did not lead to a higher incidence of pseudoarthrosis compared to conservative therapy. Overall, dens fractures primarily fully consolidated in eleven cases (33.3%), while nonunion occurred in six patients (18.2%), during the follow-up period. This is likely comparable to other studies, which report union rates from 29% to 37.3%13,34 and stable nonunion at 37.5%. 38 Among these patients, four subjectively did not experience painful symptoms, while two patients reported localized pain. 35 All six patients exhibited no neurological deficit manifestation with normal daily activities considering their age and comorbidities, and furthermore, none of our patients experienced secondary fracture displacement. Consistent with literature, a high rate of pseudoarthrosis occurrence is most commonly described in dislocated type II C2 fractures,33,36 confirming our findings.
The primary goal of treating dens fractures in the geriatric population is to preserve their independence and quality of life. 37 Surgical fixation is associated with a faster fusion rate, but its utility in older patients with comorbidities and poor bone quality is debatable.34,38 According to Jung et al, 39 there is no significant difference in trabecular bone healing between the conservative and surgical groups.
In our octogenarian cohort, conservative treatment led to a significant reduction in pain, as indicated by VAS scores, which showed improvement from admission to the end of the follow-up period after fracture healing. Most patients (n = 27) were either pain-free or experienced only mild pain (VAS less than 3) that did not require analgesic administration upon follow-up. One patient maintained a VAS score of 7 but unfortunately passed away from cardiac causes the day after hospital admission, preventing us from assessing the effectiveness of conservative therapy in this instance. Importantly, there were no new neurological deficits reported, all patients had a median JOA score of 17 at discharge, indicating stable neurological function throughout their treatment. This strongly supports the effectiveness of conservative therapy. On the other hand, in the meta-analysis by Huybregts et al, 31 no clinically relevant differences were identified between surgically and conservatively treated patients in terms of Neck Disability Index score and VAS pain. All surviving patients showed favorable improvement in activities of daily living as assessed by NDI score, although none of the observed patients were completely without limitations. Our data are consistent with previous reports including a study by Rizvi et al 27 In this study, unlike our data, 53% of patients were without disability. Additionally, 19.7% of patients presented with mild disability, and 17.9% exhibited moderate disability. In contrast, our cohort showed mild disability in 27.3% and moderate disability in 24.24% of patients. Furthermore, the median patient age was 72 years, indicating that these patients were younger than those in our cohort, which included individuals with type III fractures.
Our study was limited by its retrospective design, absence of a control group, and was restricted to a single orthopedic center. However, it represents 1 of the largest studies of its kind in our population, primarily demonstrating the safety of a conservative approach in managing type II C2 odontoid fractures in the geriatric population over 80 years old. Still, further multicenter prospective studies are needed to confirm its role in the treatment algorithm for odontoid fractures.
Conclusion
The presented study confirms the seriousness of C2 injuries in octogenarians, associated with high morbidity and mortality in the subsequent period. The results of conservative treatment of odontoid fractures with early mobilization of patients demonstrated the safety and effectiveness of treatment in a group of polymorbid patients with a high risk of complications from surgical therapy. At the same time, it is possible to achieve satisfactory results in patients with significant displacement of odontoid fractures with a PADI of less than 15 mm or with delayed healing and manifested fibrous union (nonunion). The study confirms the severity of injuries to the upper cervical spine in the geriatric population and demonstrates the efficacy of conservative treatment even in borderline indications of significantly displaced fractures.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this study was supported by the Ministry of Health of the Czech Republic, grant no. NU23-10-00413.
