Abstract
Background
Over the past 10 years, the nation has witnessed a significant increase in the number of physician assistant (PA) education programs. Primary care shortages throughout the United States have reached a staggering deficiency. The purpose of this project was to expand the primary care workforce in the Commonwealth of Virginia by increasing exposure to primary care setting early in the academic didactic year of physician assistant schooling.
Methods
This innovative research project originated in 2017 and was inclusive of PA students ranging from 20 to 44 years of age, across multiple demographics, conducted during the first year of didactic studies. This cross-sections study examined a total size of 115 students over from three different cohort years that participated in the free medical clinic completed a pre/post exposure survey.
Results
This study highlighted that an increased exposure to primary care in the early didactic phase of physician assistant graduate studies yielded a moderate increase in the interest to pursue a career in primary care upon graduation. Throughout the 2016 to 2017, 2017 to 2018, and 2018 to 2019 academic cohorts, 19% more from baseline indicated at the end of their primary care experience that they were more likely to practice in the field of primary care following the free medical clinic experience.
Conclusions
This study demonstrates a positive influence of early exposure to primary care for Physician Assistant students with the increased affinity to practice in the field upon graduation and has set a foundation for continuation of data collection in future PA cohorts.
Introduction
Over the past 10 years, the nation has witnessed a significant increase in the number of physician assistant (PA) education programs. Currently there are 218 accredited PA programs and the number is expected to increase by 52 by the end of 2020. 1 These increases in programs are a direct response to the current and anticipated need for more health care providers, driven in part by increased access to health care through the Affordable Care Act, increased demand for health care services related to the graying of the baby boomer generation, and anticipated retirement of practicing physicians. 2 Primary care shortages throughout the United States have reached a staggering deficiency. The Association of American Medical Colleges (AAMC) estimates a deficit of 14,900 to 35,600 primary care physicians by 2025. 3
A promising solution to meet this deficiency, and increase interest in primary care, requires a multi-pronged targeted approach. Previous research has demonstrated that exposure to vulnerable populations has a positive impact on student attitudes about vulnerable populations and generally increases the likelihood that they will volunteer to work in settings that provide care to the underserved.4,5 The purpose of this project was to expand the primary care workforce in the Commonwealth of Virginia by increasing exposure to primary care setting early in the academic didactic year of physician assistant schooling.
The aim of this early exposure experience was to elicit a genuine interest and continued commitment to the field of medicine, and in particular to primary care. This goal was examined through student exposure and experience to primary care early on in the didactic phase of study. This experience took place in an underserved community, as an interprofessional service learning opportunity, and at a local free medical clinic located in rural western Virginia.
Background
In order to introduce primary care to first year PA students early in their didactic education an evening interprofessional clinic was established. This clinic provided a primary care experience in a rural setting available to students from the areas of occupational therapy, physical therapy, pharmacy, physician assistant, and nursing. The Physician Assistant program is 1 professional program that was an active participant in the interprofessional free medical evening clinic experience. This PA program awards a Master’s of Science in Physician Assistant Studies upon completion of 86 graduate credits completed over 8 consecutive semesters during a 30-month time frame.
The free medical clinic currently has a patient base of 1,800 and limited capacity to provide additional care without expanding hours. In 2016, the Free Medical Clinic provided over 6,400 visits and nearly 2,000 specialist referrals at no cost to the patients. The most common problems patients were seen for include hypertension, elevated lipids, chronic pain, mental health issues, and diabetes. The average Free Medical Clinic patient’s age was 48 years-old and 60.3% were female. Over 62% were <100% of the federal poverty level (FPL), 24% 101-150 FPL, and 14% 151-200% FPL. Sixty-four percent of the patients were Caucasian, 21% Hispanic, and 11% African-American.
The free medical clinic, allowing for this experience, is currently funded through a five-year Health Resources and Service Administration (HRSA) grant. This clinical setting is an interprofessional clinic inclusive of graduate health professions students from the programs of physician assistant, physical therapy, pharmacy, occupational therapy, and nursing.
Methods
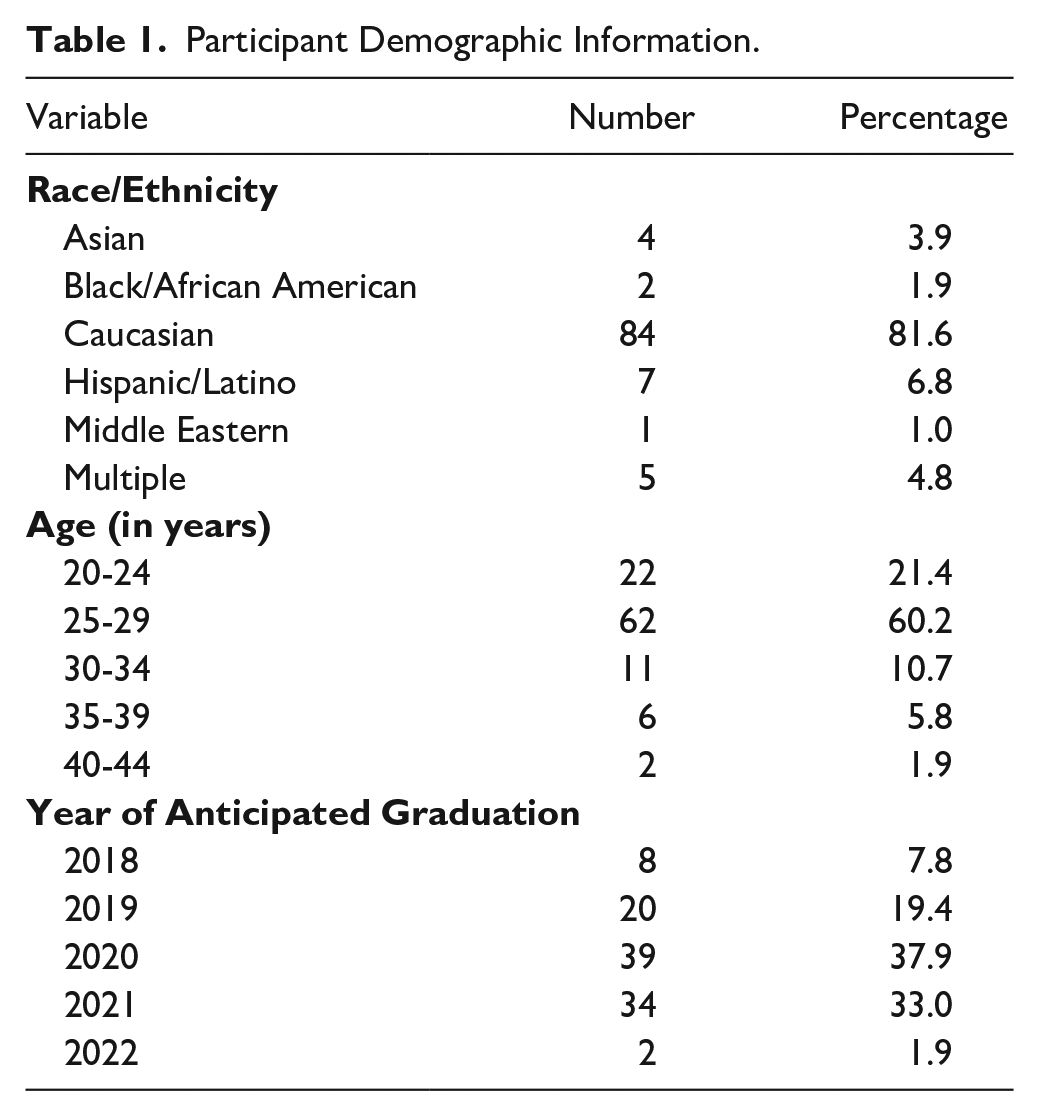
This study was approved by the Shenandoah University IRB. This research project originated in 2017 and was inclusive of PA students ranging from 20 to 44 years of age, across multiple demographics, conducted during the first year of didactic studies (Table 1). The sampling was purposive and convenience sampling, and students volunteered to participate. The design was quantitative and cross-sectional, examining a total sample size of 115 students from 3 different cohorts of students over a 3 year period. In years 2016 to 2017 50 students were eligible to participate, in years 2017 to 2018 58 students were eligible to participate, and in years 2018 to 2019 60 students were eligible to participate. In total, 115 students volunteered to participate from the available 3 cohorts of students. A total of 27 (out of 50 eligible) first year PA students were part of a single rotation through the free medical clinic in the academic year 2016 to 2017, 32 (out of 58 eligible) first year PA students rotated through in the academic year 2017 to 2018, and 56 (out of 60 eligible) first year PA students rotated through in the academic year 2018 to 2019. A total of 115 students that participated in the free medical clinic experience and all students completed the study pre/post survey.
Participant Demographic Information.
The pre and post-survey was administered at the same time to students at the end of their didactic experience. The survey intended to assess each student’s interest in primary care before and after exposure to the free medical clinic. The survey asked participants to reflect on, and assess, their initial interest in primary care prior to the primary care clinic exposure in comparison to the likelihood of entering into primary care after graduation. Each students’ 5 hr clinical experience allowed for the opportunity to provide direct patient care in an interprofessional setting throughout a rural community. The following question was used to assess the self-reported likelihood of practicing in primary care prior to the clinical experience: “Prior to your experience at the clinic, how likely were you to practice in a primary care setting after graduation?” A subsequent question, “Following your experience at the clinic, how likely is it that will practice in a primary care setting after graduation?” was used to assess the self-reported likelihood of practicing in primary care after the clinical experience. Additional questions were asked of students regarding their knowledge and experience with other areas such as social determinants of health and vulnerable populations.
Prior to completing the primary care exposure at the evening at the clinic, the students selected for this experience had successfully completed didactic course work in anatomy, physiology, dermatology, ears nose and throat, head face and neck, and pulmonology. A Physical Assessment and Medical Interviewing course that instructs students on the appropriate techniques of physical examination was conducted concurrently with each topic. This allowed students the ability to confidently perform medical examinations on patients presenting with complaints in the origin of dermatology, upper respiratory, or pulmonology. An example of the patient cases observed during this clinical experience? include, but are not limited to, the chronic management of diabetes, hypertension, and hyperlipidemia, along with the acute complaints associated with primary care. Each evening students experienced cases that also include preventative health management during annual health exams and well-women visits.
Data Analysis & Results
The data collected from the surveys were first entered into excel and cleaned. The data were then imported into Statistical Product and Service Solutions (SPSS) software version 24 and descriptive statistics were run. The descriptive statistics results indicated that students who participated in this early exposure to primary care reported a greater interest in entering into primary care after graduation compared to what they indicated as their level of interest prior to this primary care experience (Table 2). This table highlights if students were “likely” or “unlikely” to agree to the questions posed pre/post exposure to the primary care clinic. Additionally, the absolute differences between the pre/post exposure are highlighted in the last column of Table 2 with a “+” indicating an increase in the likelihood of answering “likely” in the post survey versus the pre-exposure survey. Whereas the “–” indicates that there was a decrease in participants reporting that they were “unlikely” to respond post-survey to the question than they did pre-exposure.
Pre/Post Questions to Participants Prior and After Exposure to Primary Care Setting.

Overall, this study highlighted that an increased exposure to primary care in the early didactic phase of physician assistant graduate studies yielded a moderate increase in their expressed interest to pursue a career in primary care upon graduation. Throughout the 2016-2017, 2017 to 2018, and 2018 to 2019 academic cohorts, 19% more from baseline indicated at the end of their primary care experience that they were more likely to practice in the field of primary care following their experience at the free medical clinic. The rural primary care experience also yielded a 9% increase in PA students agreeing that they would not be more sensitive to the needs of vulnerable populations post-exposure compared to pre-exposure. Lastly, the comfort level of working within an interprofessional team increased by 8% from pre-exposure to post-exposure.
Discussion
This study demonstrates that exposure to primary care early in the PA curriculum can positively influence decisions to enter into this area of practice upon graduation. Given the need to fill more gaps in primary care nation-wide, and in rural areas in particular, this is a promising approach to influence the uptake of those wanting to practice in this area post-graduation. This study also demonstrates that exposure to a rural healthcare setting can positively alter perceptions of working with vulnerable populations and within interprofessional teams. While this study shows promising effects of exposure to a primary care setting related to later interest in practicing in a primary care setting, this study does have several limitations.
One limitation to this study is related to the timing of the pre/post surveys. This data was originally collected as part of the reporting requirements for a grant and a research study was not part of the original design. After the grant activities were underway a study was designed, and an IRB was obtained. However, the exposure to the primary care setting had already taken place by the time the IRB was approved. As a result, the pre/posttest surveys were administered at the same time point and not prior to the primary care exposure, and instead were both administered post the primary care exposure asking students to answer questions about pre/post exposure effects. Therefore, the results of this study must be understood and interpreted within these design constraints. Additionally, the study does not utilize a validated survey instrument; therefore, the survey questions are limited in the conclusions that can be drawn here. Further, the study included a small sample size per cohort and no ability to conduct statistical analyses due to the nature of how the data was collected. Further, it must also be recognized that participants may have responded more positively than they felt about a particular question due to the social desirability of wanting to appear more likely to go into a particular field of healthcare and this may not actually translate into this occurring for a variety of reasons not measured here. Lastly, the conclusions drawn from this study are based on only 1 exposure to primary care for the participants.
Despite these limitations, this study marks 1 of the few studies, to our knowledge, that has attempted to impact and study PA students’ exposure to primary care early in the didactic career to influence job seeking behavior post-graduation. It has highlighted the role that creative curriculum approaches can play in securing a more robust primary care workforce and closing the gap in this area of care that PAs can play. This study further highlights the need to conduct studies with a more rigorous study design utilizing a valid survey instrument.
Conclusion
This study demonstrates a positive influence of early exposure to primary care for Physician Assistant students with the increased affinity to practice in the field upon graduation. It is anticipated that as this project continues to progress, the exposure of an additional 62 PA students each year to primary care during the didactic phase of a curriculum, has the potential to influence interest to practice in primary care upon graduation and ultimately continue to fill the void of healthcare practitioners in rural communities. Additional data collection from the 2019 to 2020 cohort continues to strengthen this relationship, along with the most recent study published in Medical Education Online 6 referencing the integration of early clinical exposure to increased interest in primary care. This study has set a foundation for continuation of data collection in future PA cohorts as well as for future studies of a similar nature.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
