Abstract
Introduction
Chronic disease is placing an overwhelming burden on the American health care system with almost 1 out of every 2 adults having at least 1 chronic illness. 1 These conditions shorten lives, reduce quality of life, and create considerable burden for caregivers. Patients with chronic conditions improve their outcomes when they follow recommended treatment regimens, obtain relevant tests for monitoring of their disease(s), perform self-management activities, and follow a healthy lifestyle.2-6 Since the overwhelming majority of patients receive care for their chronic conditions from primary care practices,7,8 this is an important venue to assist patients in taking these steps.
An increasing role in the primary care practice to assist patients with chronic disease management is the role of care manager. Care management typically encompasses chronic disease management, care coordination, and self-management support. It is provided by nurses, social workers, dietitians, pharmacists, or others. Care management services can be delivered via telephone or other means, although face-to-face in-practice interaction is almost often included.
Results of research-supported care management studies have generally been positive in influencing patient outcomes although not always improving costs, but mixed when conducted outside of primary care or in real practice implementation.9-16 What is lost in the translation of controlled interventions to the real world of care delivery? In the current study, we evaluated the implementation of care management in a nonresearch primary care setting. We sought to understand how individual practices and their associated administrative medical group structure would implement care management, what the successful elements of the implementation were, and the effects that implementation had on patients with diabetes or those at risk of diabetes due to obesity. In this paper, we describe changes in patients’ clinical outcomes as a result of implementation, whereas other study results are reported elsewhere.17,18
Methods
Study Design
The study was a pair-matched cluster randomized controlled trial.19,20 The participating practices were part of a physician-owned medical group in southeast Michigan. Ten total primary care practices were categorized according to size (large being 5 or more providers or small being 4 or less providers), discipline (family or internal medicine) and rural or suburban location and placed in pairs. One practice from each pair was randomly selected using a random number generator for intervention.
Participants
Given the pragmatic nature of this study, eligibility criteria for patients were broad to include as representative a sample as possible. The inclusion criteria were (1) active patient at one of the study practices during the study period (at least 1 visit in the prior 24 months), (2) age 18 years or older, and (3) as noted in the medical record, a diagnosis of type 2 diabetes (ICD-9 code 250.xx) or obesity (body mass index [BMI] of ≥30 kg/m2). In these practices, prediabetes was not reliably recorded. Patients were excluded if they (1) had less than 12-month life expectancy as noted in the medical record, (2) were non-English speaking, (3) lived in a nursing or group home, (4) had serious substance abuse, psychiatric illness, or cognitive impairment, or (5) had diabetes or impaired glucose tolerance secondary to chronic glucocorticoid use, polycystic ovary syndrome, pituitary lesion, or pancreatectomy.
Intervention
The focus of the care management intervention was on improving diabetes- and obesity-related outcomes. The key components of the care management intervention included (1) staffing improvements, including training for existing staff plus the addition of new care managers and (2) the addition of new care management software and modifications to the existing electronic medical record (EMR). Intervention practices each received an embedded care manager (part- or full-time depending on practice size), which was a new role in the practice. Care managers were extensively trained over a 2-month time period, including didactic instruction on the target conditions, behavioral change strategies using motivational interviewing, handling behavioral health issues, use of the EMR and care management enhancements, conducting patient assessments, creation of a community resource and referral guide, and ongoing planning sessions with their assigned practice to identify a practice plan for implementation. Providers and all staff were trained over approximately a 2-hour time period by care managers and the director of clinical quality improvement in identification of eligible patients, use of the EMR data elements, referral to and utilization of the care manager, and data recording and tracking. Selected practice staff and providers worked with their care manager to develop the practice plan for implementation.
Care management enhancements to the practice’s EMR were made and focused on identifying eligible patients for care manager visits, notifying providers of patients’ eligibility for care management, and flagging gaps in chronic care for patients with diabetes (such as not having a visit in the previous 6 months or an A1c more than 8%). Other changes included templates for management of diabetes and obesity by clinical practice guidelines, reporting tools for tracking individual patient progress and overall panel status, ability to review patient health assessment results, and individual goal tracking and planning associated with care manager planned care visits.
Data Collection
The intervention recruitment period was 16 months, and all patients were followed for 1-year postrecruitment. As patients presented for care, clinical data and laboratory test results were recorded as part of standard practice and these data were later extracted for the evaluation. The primary outcomes included A1c, weight, blood pressure, low-density lipoprotein (LDL) cholesterol, BMI, and microalbumin. We also extracted data on prescriptions for metformin, long-acting insulin, short-acting insulin, glitazones, DPP-4 agents, sulfonylureas, beta-blockers, angiotensin-converting enzyme (ACE) inhibitors, angiotensin II receptor blockers (ARB-II), calcium channel blockers, centrally acting antihypertensives (eg, clonidine), statins, orlistat, and appetite suppressants. Patients were considered to have had their medications intensified if they (1) switched from oral medications to insulin, (2) had an increase in the number of oral medications, (3) added oral agents to insulin or insulin to oral medications, or (4) increased oral and insulin combination. Intensification of hypertension medications was defined as either (1) from no medication to initiation of pharmacotherapy or (2) increasing number of unique prescriptions. Medication dosage was not captured. Files were generated by the medical group information technology staff quarterly and transferred to the study team’s secure server via a secure file transfer protocol.
Statistical Analysis
We analyzed the primary outcomes first as continuous outcomes and then as binary outcomes based on clinically meaningful cutoffs: A1c <7%, systolic blood pressure (SBP) <140 mm Hg, LDL <100 mg/dL (diabetic patients), LDL <130 mg/dL (nondiabetic patients), and weight loss ≥5% of baseline weight. For each intervention patient, a control patient from the paired practice, who had the same baseline risk score (defined on an 8-point scale from 0 = no risk factors to 7 = diabetes and LDL >100 mg/dL and SBP >140 mm Hg), disease status (diabetes vs obesity without diabetes), and whose first available clinic datum was within ±3 months of the enrollment time of the intervention patient, was randomly selected to be a matched comparison patient.
Even after selecting comparison patients by the above criteria, there was still some imbalance (eg, baseline BMI and statin use) within each pair of clinics using paired t test and for categorical variables, we used McNemar’s chi-square test 21 or Stuart-Maxwell symmetry test. 22 (detailed results are available on request). To control for these, we used a 2-step procedure that allows adjustment of baseline patient-level differences between groups.23-25 After the patient-level differences are adjusted, the inference is made at the practice level. For continuous outcomes, in the first step, we estimated a linear mixed effects model (generalized linear mixed model for binary outcomes) with a random intercept for the patient-pairs controlling for imbalanced baseline covariates and calculated the average residuals within each practice-pair for each of the time interval, baseline, 3-, 6-, 9-, and 12-month follow-ups. If the intervention had no effect, then the residuals in the intervention and comparison practices should be similar on average. Thus, in the second step, we used a linear regression of the average residuals on indicators for the intervention, time intervals and their interactions. The coefficients on the interaction terms represent difference in the changes (also called different-in-differences) in outcomes between the intervention and comparison practices from baseline to follow-ups.
Results
The practice participants included 10 primary care practices within one physician-owned practice organization in southeast Michigan. Intervention practices were pair-wise matched with similar comparison practices on practice discipline, size, and geographic location. There were 2 internal medicine (1 large urban and 1 small urban) and 3 family medicine (1 large urban, 1 large rural, and 1 small rural) in each pair. Figure 1 depicts the flow of practices and patients in the study. The total number of active patients in the 5 paired control practices who met the inclusion criteria (assessed through their EMR system) were 56 048. A total of 707 patients enrolled with a care manager in the 5 intervention clinics over the 16-month recruitment window, among whom 444 had diabetes at baseline and 263 were obese, but did not have diabetes. Out of the 707 intervention patients, 696 were matched, leading to 443 pairs of patients with diabetes and 253 pairs of patients without diabetes. The 11 intervention patients who did not have a valid match were excluded from the analysis.
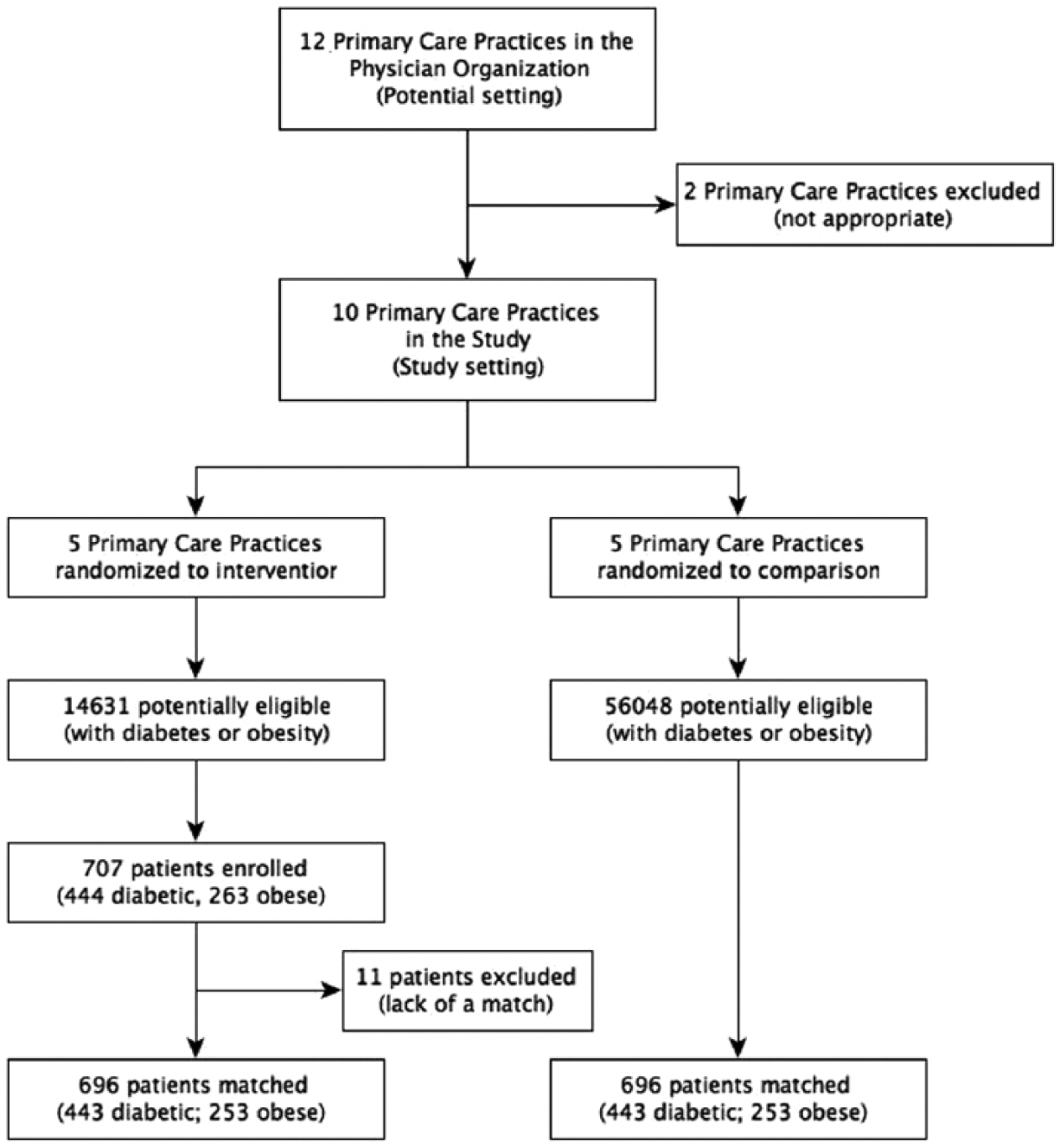
Practice and patient participation flow diagram.
Table 1 presents the demographic and baseline clinical characteristics of the intervention and matched comparison patients in the study. Patients in the intervention group at baseline were overall significantly different on several characteristics as compared with matched comparison patients. These differences were controlled statistically in outcome analyses, as described above.
Baseline Characteristics of Intervention and Matched Comparison Patients.
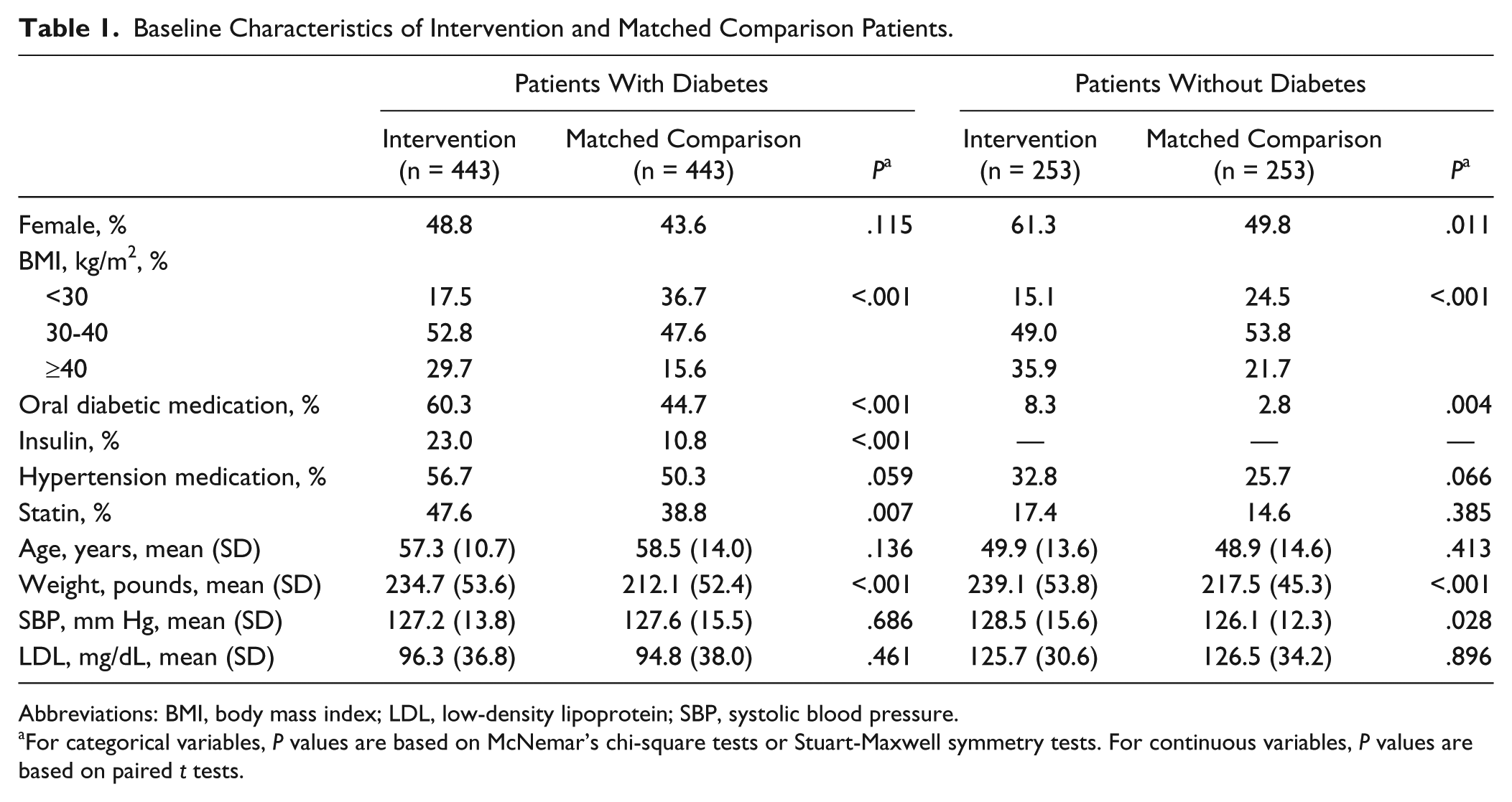
Abbreviations: BMI, body mass index; LDL, low-density lipoprotein; SBP, systolic blood pressure.
For categorical variables, P values are based on McNemar’s chi-square tests or Stuart-Maxwell symmetry tests. For continuous variables, P values are based on paired t tests.
Table 2 presents the unadjusted and adjusted estimates of differences in changes in the primary outcomes for patients with diabetes. Improvements for the intervention as compared with comparison patients were found in A1c levels (−0.5, 95% CI, −1.0 to −0.04) and the proportion of diabetes patients whose A1c was under control (12% higher increase than the comparison group, 95% CI, 3%-20%).
Adjusted and Unadjusted Difference-in-Differences Estimates of the Effects of the Intervention for Diabetic Patients.

Abbreviations: ALB, microalbumin; LDL, low-density lipoprotein; SBP, systolic blood pressure.
Confidence intervals are based on cluster robust standard errors. The adjustments vary across outcomes (last 2 columns). Weight (percent change of weight compared with baseline)—adjusted for baseline weight, age, sex, and whether with insulin injection. A1c (A1c <7%)—adjusted for baseline weight, age, sex, baseline A1c, intensification of diabetes, and number of medications at last quarter. SBP (SBP <140 mm Hg)—adjusted for baseline weight, age, sex, baseline SBP, intensification of hypertension, and number of medications at last quarter. LDL (LDL <130 mg/dL; LDL <100 mg/dL)—adjusted for baseline weight, age, sex, baseline LDL, and whether takes statin. ALB—adjusted for baseline weight, age, sex, and baseline ALB.
Table 3 shows the results for patients without diabetes. Adjusted average weight loss was 8.1 kg (95% CI, −13.2 to −3.0) more in the intervention compared with the comparison patients and 15% more intervention patients lost more than 5% of their weight in 1 year (95% CI, 2% to 28%). Significant improvements were not observed in blood pressure control. However, most patients already had an SBP <140 mm Hg at baseline (86% and 71% in intervention and comparison patients, respectively).
Adjusted and Unadjusted Difference-in-Differences Estimates of the Effects of the Intervention for Nondiabetic Patients.

Abbreviations: LDL, low-density lipoprotein; SBP, systolic blood pressure.
Confidence intervals are based on cluster robust standard errors. The adjustments vary across outcomes (last 2 columns). Weight (percent change of weight compared to baseline)—adjusted for baseline weight, age, and sex. SBP—adjusted for baseline weight, age, sex, baseline SBP, and the intensification of hypertension. LDL (LDL <130 mg/dL; LDL <100 mg/dL)—adjusted for baseline weight, age, sex, baseline LDL, and whether takes statin.
Discussion
Our findings are consistent with the literature demonstrating that in practice care management usually results in favorable impacts on clinical outcomes related to diabetes and obesity.3,26,27 The positive results in this trial add to the evidence for the effectiveness of care management in nonresearch community practices and demonstrate that the positive results found in research settings can be replicated in community primary care delivery settings. A recent review found that care management is increasingly being utilized in managing diabetes in US primary care settings. Physicians are trained to deliver evidence-based care and incorporate office staff such as care managers to deliver diabetes self-management education. 3
One of the most clinically significant findings in this study was the substantial increase in the proportion of patients with diabetes who met the clinical target of A1c <7% in the intervention group—an increase from 25% before the intervention to 45% after intervention implementation. Also 26% of patients without diabetes in intervention practices lost 5% or more of their body weight during the intervention as compared to 10% of comparison patients. Weight loss of 5% or more is considered clinically significant for reducing risk for diabetes.28,29
The intervention did not result in significant improvements in weight loss, blood pressure, and LDL control among diabetes patients. This in part reflects the fact that diabetes patients in this study were selected based on needed improvements in A1c rather than blood pressure or LDL. Additionally, though behavioral changes are recommended for addressing blood pressure and LDL, 30 these values are also readily addressed by medication adjustments and thus are likely to improve over time with or without care management.
The challenge in this translational work is in learning what it takes to achieve clinically meaningful results through practice change in community care settings. 31 Although this study was research funded, the funding was largely provided for the evaluation, not the implementation of the intervention. Study staff did not control the implementation as practice staff identified their own mechanisms for use of the care management.
We noted that variability in patient health care participation was a source of missing data. Clearly, all patients did not visit the clinics every quarter and missing data may be more common among patients with poorer health status. Two features of our analysis reduce concern about missing data or loss to follow-up. First, the random effects model we used allowed data to be missing at random, that is, the groups had missing patterns predictable based on observed data; and these data were controlled for in the analysis. From our analysis, we can see initially the intervention group had higher proportions of patients with follow-up, most likely due to enhanced care management; and it is reassuring that at 12-month the proportions of patients with available data were similar between groups for each outcome. Second, the study is a cluster randomized controlled trial and therefore the appropriate level of inference is at the clinic level. In the second step of our analysis we used the clinic-time average residuals and the correct degrees of freedom for inference. This is consistent with the intent-to-treat principle at the clinic level.
This study has several limitations. Only 10 practices participated in southeast Michigan, of which 5 received the intervention. There was also variability in the baseline risks factors of intervention versus comparison patients, especially BMI and A1c for diabetic patients. Despite statistical control, these baseline differences may have contributed to variability in average change scores between intervention practices and comparison practices, especially if important differences were not captured by observed variables. Additionally, there were many regional and national initiatives and changes happening in primary care during the time period of this study. However, we have no reason to believe that such macro-changes differentially effected the implementation sites. Our extensive qualitative assessment alerted us to any implementation issues and their resulting implications. From this assessment, while the core components of care management were assessed and determined to be present in each of the intervention practices, implementation was variable in terms of the intensity and staffing for these services. Site-specific variation is how “real-life” implementation occurs, and it is encouraging that overall effects were observed despite those differences. We explored these implementation issues extensively in a separate qualitative study. 18 In brief, we found that practices that utilized effective macrocognitive processes were much more effective in achieving implementation outcomes.
In summary, these results support previous research demonstrating that the implementation of care management in a typical community care delivery setting does deliver improved clinical results for patients with diabetes and obesity. Continuing research should explore the factors necessary for all practices to implement care management to achieve these improved results.
Footnotes
Authors’ Note
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of Diabetes and Digestive and Kidney Diseases or the National Institutes of Health. John Piette is a VA Senior Research Career Scientist.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The project described was supported by Award Number 1 R18 DK082377-01A2 from the National Institute of Diabetes and Digestive and Kidney Diseases. Additional support was provided by Grant No. P30DK092926 from the National Institute of Diabetes and Digestive, and Kidney Disease. John Piette is a US Department of Veterans Affairs Research Career Scientist.
