Abstract
Sport-related concussion (SRC) and physical pain are both associated with poor mental health, impaired cognition, and reduced quality of life. Despite SRC and physical pain often co-occurring, there is little research that investigates these two factors together, and therefore it is difficult to conclude which of these contributes to the negative outcomes associated with them. Therefore, the present study aimed to investigate the effect of SRC and physical pain on mental health, cognitive ability, and quality of life. Depression was measured using the Center for Epidemiological Studies Depression Scale, anxiety was assessed using the State-Trait Anxiety Inventory while the SF-12 recorded health-related quality of life. A trail making task (TMT) assessed cognitive flexibility of participants. Analysis of 83 participants (43 concussed) revealed that SRC led to reduced accuracy on TMT(A) and (B), whereas physical pain was responsible for poorer mental health and reduced quality of life. This study highlights the influence that SRC has on cognitive ability and the impact that physical pain has on mental health and quality of life. With this information, we are better placed to predict the negative consequences of SRC and physical pain and therefore tailor support accordingly.
Introduction
Sport-related concussion (SRC) has become a widely investigated area in recent years, with many sport-related activities involving high energy events that can expose athletes to direct and indirect traumas and increase their risk of injury.1,2 Consequences of SRC have been identified, with poorer mental health,3,4 impaired cognition,5,6 and reduced quality of life,7,8 among the most prevalent outcomes. Although physical pain often accompanies SRC,9,10 surprisingly few studies incorporate this factor into SRC research. Therefore, the relationship between SRC and physical pain and these three broad outcomes warrants investigation. By better understanding how SRC and physical pain relate to mental health, cognitive ability, and quality of life, we are better able to support athletes that have sustained SRC, experiencing physical pain, or both.
Depression is one of the most researched mental health disorders, likely due to its high prevalence, with 3.8% of the general population suffering from depression. 11 However, higher rates are reported in athletes that have12,13 and have not sustained SRC.14,15 These elevated depressive symptoms are also found in student athletes who report higher levels of physical pain.14,16 Given the great comorbidity between depression and anxiety, it is predictable that elevated scores of anxiety are also often found in those that have sustained SRC 17 and experiencing physical pain.18–20 Therefore, as SRC and physical pain are likely to co-occur9,10 and both are found to negatively impact depression and anxiety, it is important to understand which contributes more to these outcomes.
Cognitive flexibility involves the ability to adjust to change in task demands or priorities 21 and is therefore important for athletes with evidence that cognitive flexibility levels of team athletes are higher than those of individual athletes. 22 Aslan 22 suggests this could be due to individual sports requiring less cognitively than team sports. Team sports tend to be contact sports such as rugby, football, and hockey whereby SRC is likely, 23 and as SRC negatively impacts cognitive flexibility,24,25 this threatens optimal performance 22 as well as exacerbating other negative consequences of SRC. Therefore, it is necessary to protect athletes from sustaining SRC and the impact this can have on cognitive flexibility. The role of physical pain on cognitive flexibility is still unclear with many studies examining chronic pain in humans26,27 and animals. 28 Despite the literature unclear on the role that physical pain has on cognitive flexibility, there are studies linking physical pain with impairments to other areas of cognition.5,6 As these studies did not account for SRC, it may be that impaired cognition was misattributed to physical pain, and therefore assessing both simultaneously is warranted.
Considering there is evidence that SRC and physical pain are associated poorer mental health12,13,17 and cognitive impairment,24,25 it is unsurprising that these factors are also associated with reduced quality of life.29,30 It is possible that the two broad outcomes could negatively impact quality of life. For example, impaired cognition leading to individuals struggling to complete daily tasks could negatively impact quality of life. Likewise, not being able to compete at a sporting level that one once could, can lead to poorer mental health and quality of life. However, even if these examples did explain reduced quality of life in athletes, it is still unclear whether this is due to SRC or physical pain, with evidence that both negatively impact quality of life,31–34 and therefore this warrants further exploration.
Although there is evidence that SRC negatively impacts mental health such as depression12,13 and anxiety, 17 areas of cognition such as cognitive flexibility,24,25 and quality of life,29,31,34 the role that physical pain has on these outcomes is still ambiguous. This is due to evidence that physical pain can also lead to poorer mental health,14,16 impaired cognition,26,27 and reduced quality of life.32,33 Although SRC and pain are often experienced simultaneously,9,10 and athletes are among the most at-risk of sustaining both, the two contributing factors are rarely examined in conjunction in the literature. Therefore, the present study aims to address this gap in the literature, as learning which factor affects each outcome will allow better support for athletes that have sustained SRC, are experiencing physical pain, or both.
Method
Participants
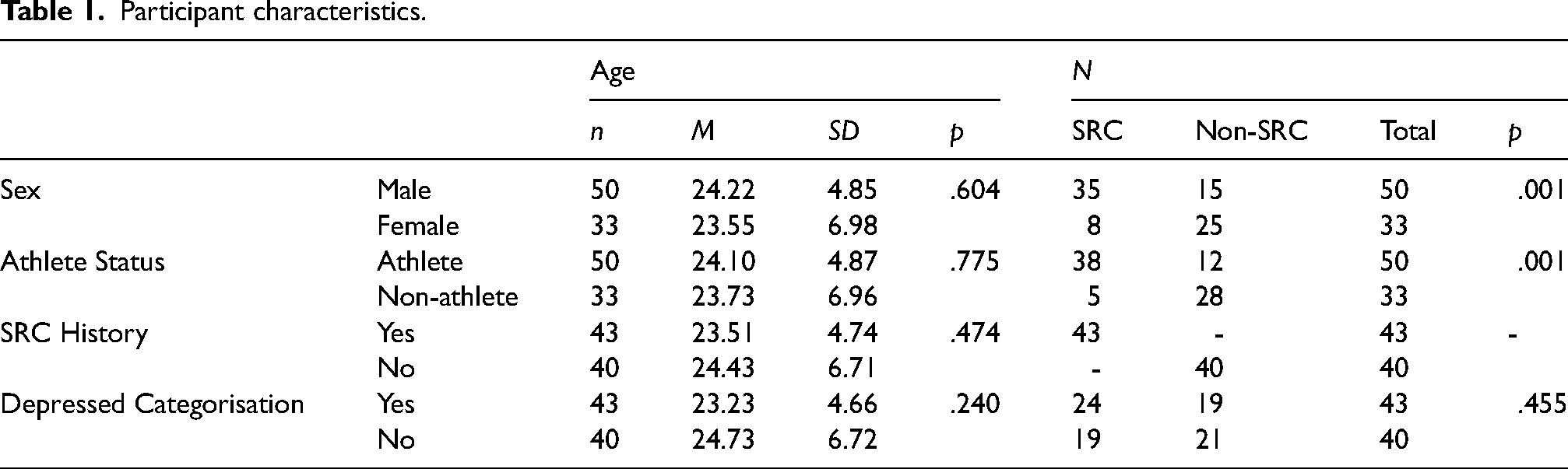
Forty-three post-concussed participants were compared with 40 non-concussed participants. The total sample completed questionnaires measuring depression and anxiety symptoms as well as quality of life, and a trail making task (TMT) designed to measure cognitive flexibility. Participants were recruited via the online departmental recruitment system within the university, advertisements on social media platforms LinkedIn and Twitter as well as word of mouth. Men and women over 18 years of age were welcomed to take part in the study. For those that had sustained concussion, a minimum of 28 days must have passed before taking part in this study to avoid exacerbating post-concussion symptoms due to the surveys being displayed on a computer screen. Those that had sustained concussion < 28 days were ineligible to take part until this period had elapsed. Post-concussed participants had sustained SRC between 1 and 48 months (M = 21.38, SD = 14.92) prior to participation with incidences ranging between 1 and 12 (M = 3.88, SD = 3.01). Further information of participants is presented in Table 1.
Participant characteristics.
Sample size calculations
Sample size was calculated using G*Power 3.1.9.7. A priori calculations indicated that 84 participants were required (across the two groups) to achieve adequate power (β = 0.95) to detect an effect size of f = 0.4 (large effect size) at α = 0.05. Therefore, the sample in this study falls one short to achieve this level of power. Post-hoc calculations were conducted to compute the actual power achieved with the sample obtained (β = 0.949) which highlighted the sample was not underpowered. A large effect size was used in calculations due to the time difference between variables (SRC history being 28 + days ago compared with physical pain in the past week).
Measures
General Information Questionnaire (GIQ): included data on sex, age, athlete status, concussion history, and level of physical pain experienced in the past week.
Numeric Rating Scale-11 (NRS-11 35 ): The NRS-11 measured self-reported physical pain in the past week providing a score ranging 0–10. Downie et al. 35 suggests that a score of ‘0’ indicates no pain, ‘1–3’ mild pain, ‘4–6’ moderate pain, and ‘7–10’ severe pain. Therefore, data from NRS-11 can be used as continuous or categorical.
Center for Epidemiological Studies Depression Scale (CESD 36 ): The CESD is a 20-item questionnaire that measures the depressive symptoms that participants have experienced in the past week. A four-point scale was used to rank the responses; 0 to 3. Zero indicated that participants had experienced that symptom ‘rarely or none of the time’ (less than once a week), 1 ‘some or a little of the time’ (1–2 days a week), 2 ‘occasionally or a moderate amount of time’ (3–4 days a week) and 3 ‘most or all of the time’ (5–7 days a week). Four items were reverse coded due to the nature of the question. A total score ≥16 of 60 highlights an individual may be experiencing some form of depression. 37 A higher total score reflected more severe depressive symptoms.
State-Trait Anxiety Inventory (STAI 38 ): The STAI was used to assess state and trait-anxiety in participants. The 40-item questionnaire was presented as two surveys; Y-1 and Y-2, which measured state-anxiety and trait-anxiety, respectively. The Y-1 form evaluated how participants felt at present whereas the Y-2 form recorded how participants feel generally. The four responses for both forms were ranked 1 to 4. For the Y-1 form, 1 suggested ‘not at all’, 2 indicated ‘somewhat’, 3 indicated ‘moderately so’ and 4 indicated ‘very much so’. For the Y-2 form, 1 suggested ‘almost never’, 2 indicated ‘sometimes’, 3 indicated ‘often’ and 4 indicated ‘almost always.’ This resulted in a scoring range of 20–80 for both State-Anxiety and Trait-Anxiety with greater scores indicating higher anxiety levels.
Health Related Quality of Life: SF-12 (SF-12 39 ): The SF-12 contained 12 items which had a two, three, five and six-point Likert scale depending on the nature of the question. The sum of scores was calculated between 0 and 36, with greater scores indicating better quality of life.
TMT: The Trail Making Task (TMT 40 ): a computerised version of TMT (Pavlovia 41 ) was used. TMT is a popular switching task that can assess cognitive flexibility and consists of two parts (A & B) in which the participant connects 25 circles as quickly as possible while maintaining accuracy. 42 The first part of the task, TMT-A, the circles are numbered 1–25, and the person should connect the numbers in ascending order. In part B, the circles include both number (1–13) and letters (A-L). Connecting dots 1–25 provides a baseline score whereas the second part, TMT-B, acts as the switching task. Accuracy scores and reaction times were recorded for both TMT (A) and TMT (B).
Reliability statistics
Reliability statistics was calculated by conducting a Cronbach's Alpha. Analyses revealed internal consistency scores of α = .91 for CESD, α = .95 for STAI (state), α = .94 for STAI (trait) which are all considered excellent. 43 The SF-12 bore an internal consistency score of α = .81 which Sharma 43 describes as a good score.
Procedure
Participants completed the questionnaires on the online survey platform Qualtrics 44 (Qualtrics, Provo, UT) and were fully informed about the study with their consent obtained prior to participation. This was followed by the participants completing the study questionnaires (GIQ, CESD, STAI, SF-12). After completing the last questionnaire, participants were directed to the TMT on Pavlovia.
Ethics
British Psychological Society (BPS) ethical guidelines were adhered to with data collection commencing after ethical approval was obtained from the University's Departmental Research Ethics Committee (DREC). A participant information sheet informed participants of the nature of the study and their rights as a participant including details on the withdrawal of data if they wished to do so. Tick box options were provided with the consent form with validation options set disallowing participants to continue if they did not provide consent. A debrief form was displayed at the end of the study.
Data analysis
Correlations were run between SRC history, mental health, quality of life, cognitive flexibility, and physical pain, isolated and when controlling for physical pain. A MANOVA and MANCOVA investigated the difference in cognitive flexibility, depression, anxiety, and quality of life between those that have and have not sustained SRC; one with and one without controlling the effect of physical pain. It was predicted that those that have sustained SRC would produce lower accuracy scores and higher reaction times scores on the cognitive flexibility task, elevated depressive and anxiety symptoms and lower scores of quality of life, as well as physical pain covarying significantly.
Results
Correlations
Correlation analysis was run on multiple variables; SRC history, depression, anxiety, cognitive flexibility, quality of life and physical pain, with and without physical pain as a covariate. Results are described in Table 2.
Correlations between SRC history and mental health, cognitive flexibility, and quality of life with and without controlling for physical pain.
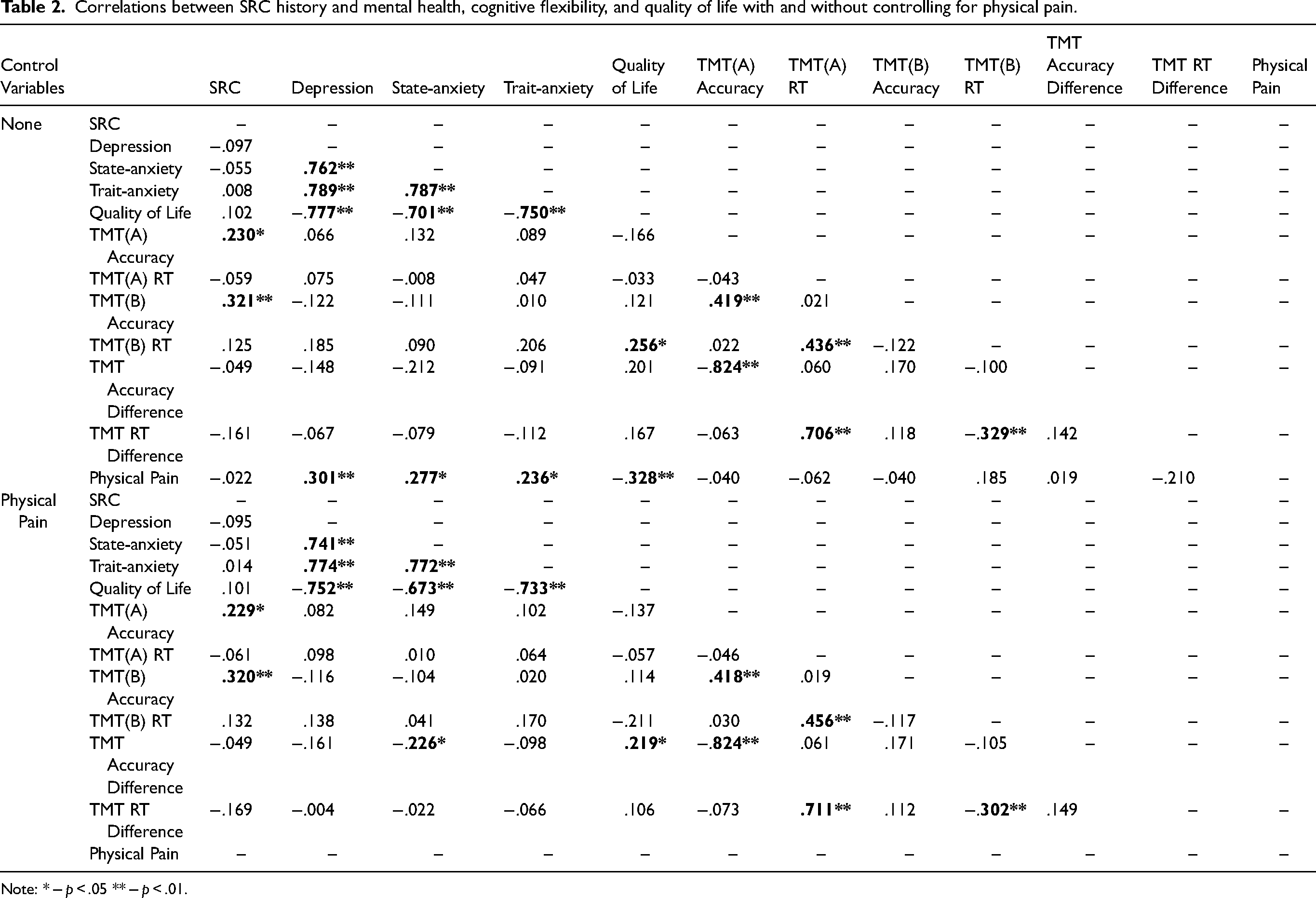
Note: * − p < .05 ** − p < .01.
MANOVA/MANCOVA
Results from the MANOVA (without controlling for physical pain) and the MANCOVA where physical pain was added as a covariate are displayed in Table 3. Descriptive statistics are presented below in Table 4 to aid the interpretation of the findings from Table 3.
MANCOVA depicting the influence of SRC history on cognitive flexibility, depression, anxiety, and quality of life with pain as a covariate.
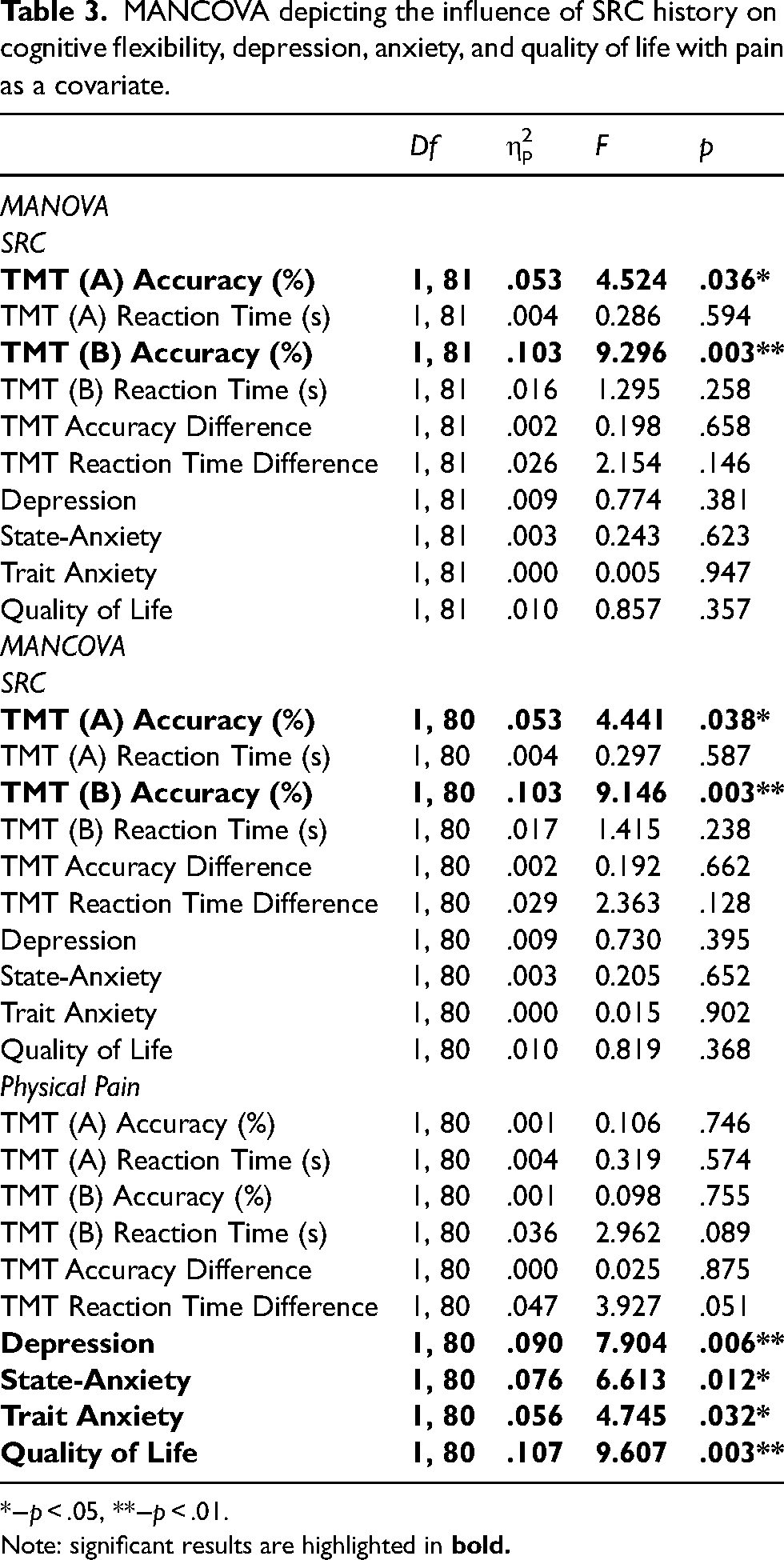
*−p < .05, **−p < .01.
Note: significant results are highlighted in
Descriptive statistics of cognitive flexibility, depression, anxiety, and quality of life by SRC history.
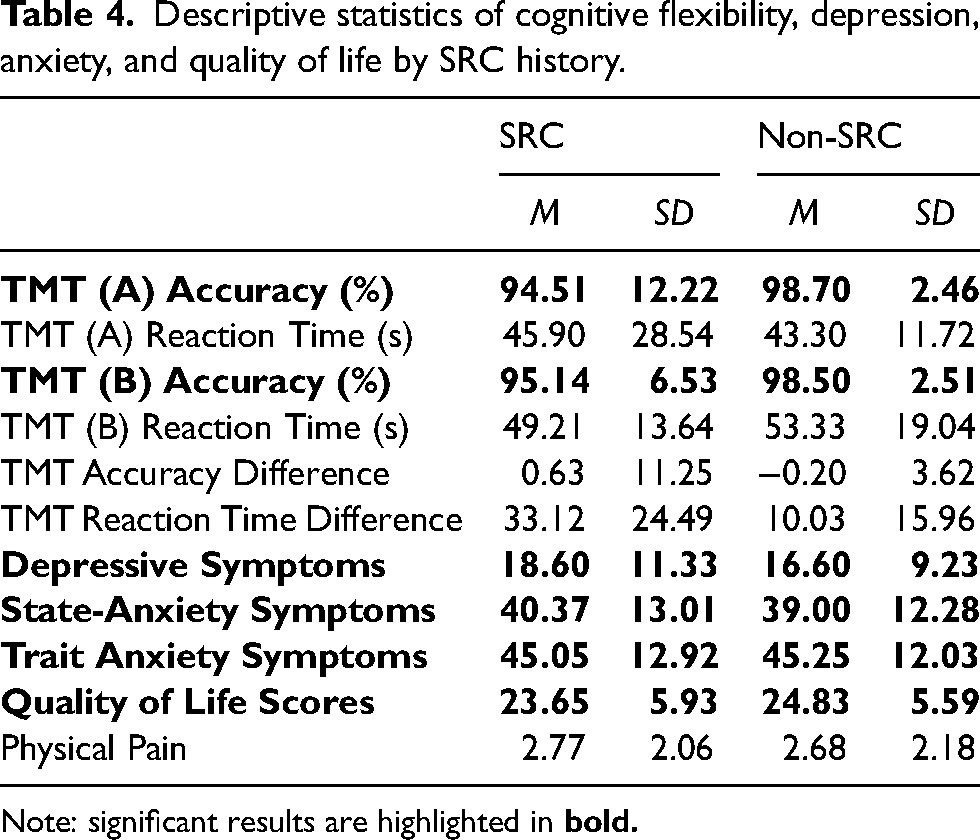
Note: significant results are highlighted in
Post-Hoc tests
Following this, the assumption of homogeneity of regression slopes was tested, as this is vital when using MANCOVA analysis. The interaction term between SRC history and physical pain had a significant effect on TMT(B) accuracy (p = .032) violating the assumption of homogeneity of regression slopes and therefore results for this variable should be inferred with caution. However, this assumption has been adhered to for all other variables (p > .05), indicating that we can accept what has been found in the main analysis for these factors.
Discussion
The present study aimed to identify the role that SRC and physical pain have in conjuncture on mental health, cognitive ability, and quality of life. Initially, our analysis revealed that SRC negatively impacted cognitive flexibility performance, with lesser accuracy recorded on both aspects of a TMT. When accounting for physical pain, we found the same results regarding SRC and cognitive flexibility, but also that physical pain was associated with depression, state-trait anxiety, and quality of life. Therefore, despite literature that links both SRC and physical pain with poor mental health,3,4,14,16 cognitive impairment,5,6 and reduced quality of life,7,8,32,33 a more nuanced explanation would be that SRC is responsible for cognitive impairment and physical pain contributes to poor mental health and reduced quality of life.
SRC and impaired cognitive flexibility have been linked before,24,25 however, the role that physical pain has on cognitive flexibility is unclear. This is because studies assessing chronic pain in humans26,27 and animals 28 are commonplace. Many athletes and non-athletes 45 live daily with acute physical pain, however, the effect of this on cognitive flexibility, to our knowledge, has not yet been examined. This study addresses this shortfall and provides evidence that acute physical pain has no detrimental impact to cognitive flexibility, which has positive practical implications given the many negative impacts of physical pain. From a sporting perspective, Vestberg et al. 46 have shown that professional and semi-professional football players had significantly better performances in switching tasks like TMT. Similar findings have been reported in rugby, 47 basketball 48 and tennis. 49 This signifies the importance of task switching ability and cognitive flexibility for optimal sporting performance. Therefore, it is reassuring that physical pain is not associated with impairment to cognitive flexibility but concerning that SRC history is.
Although it is thought cognitive impairment subsides shortly after concussion, 50 and some studies suggest cognitive impairments resolve within a week,51,52 this study indicates that the effects can last up to four years following concussion. Our sample consisted of athletes that had sustained concussion between 1 and 48 months prior to their participation with a large variance as highlighted by the standard deviation. Therefore, cognitive flexibility may be impaired following a concussion that never returns to baseline (however, pre-morbid assessments were not conducted in this study). Cognitive flexibility is important for various reasons within 53 and outside of sport,21,54 and therefore this study highlights the importance of avoiding SRC.
Moreover the prevention of physical pain is paramount. Where SRC history is associated with poorer cognitive flexibility, physical pain appears to contribute to poorer mental health (depression and anxiety) and reduced quality of life. These findings support previous literature that have found physical pain to be associated with poor mental health14,16 and reduced quality of life.29,30 However, this study brings into question studies that conclude concussion is responsible for negative changes to mental health and quality of life, that do not account for physical pain.3,4,7,8 As concussion and physical pain often co-exist,9,10 it could be that previous studies have misattributed these negative consequences to concussion, where in fact physical pain may be the responsible factor. Therefore, from the present study, it appears that SRC is associated with cognitive impairment and physical pain is responsible for poor mental health and reduced quality of life.
Knowledge application
This main findings from this study are that SRC is linked with poorer cognitive flexibility, even long after the event, and acute physical pain has a negative impact on mental health and quality of life. These findings are concerning given prior evidence that physical activity appears to promote cognitive flexibility performance.55,56 From this study, it seems physical activity is not enough to offset the effects that SRC has on cognitive ability. Given that age between concussion groups were not significantly different, it is unlikely that age was a confound in this sample whereby changes in cognitive flexibility could be attributed. Additionally, as both groups are young, it is alarming that concussion has had a negative long-lasting influence on cognitive ability. Based on these findings, sports coaches, especially in contact sports where concussion is prevalent, 57 should incorporate cognitive flexibility tasks within training sessions to combat cognitive flexibility changes. There is evidence that cognitive training can slow down cognitive decline, 58 and as there are benefits to efficient cognitive flexibility within 53 and outside of sport,21,54 this is highly beneficial for athletes and sports teams.
Additionally, this study links physical pain with reduced quality of life, with the reasons for improving quality of life obvious. Providing athletes with pain questionnaires to complete regularly may benefit athletes and their teams. Physical pain has been associated with depression, 14 and depression has in-turn been linked with lower quality of life. 59 Therefore, pain questionnaires may indicate those at risk of reduced quality of life. There is also evidence that female athletes will experience depression at lower levels of physical pain than male athletes, 16 and therefore coaches should consider this. Therefore, regular anonymous pain questionnaires would aid the identification of struggling athletes and in-turn supporting those that require it.
Limitations
Although the present study has a relatively low sample size it was not underpowered as highlighted by the sample size calculations. Therefore, the risk of type II error was low. There is, however, a risk of self-selection bias due to the voluntary nature of our recruitment. As the study was advertised as exploring the impact that SRC has on mental health, cognitive ability, and quality of life, post-concussed athletes that have noticed deterioration of these three factors may be over-represented in this sample. This could explain the high prevalence of depression in the sample regardless of concussion history, as well as impaired cognition and lower quality of life in the post-concussed sample. Additionally, data collection commenced largely during COVID-19 restrictions, and as these restrictions were found to be detrimental to mental health, 60 this could have influenced results regarding mental health and quality of life. However, this is unlikely to have any impact regarding SRC history, as all would have been subjected to these restrictions. Although this confound was unavoidable, future research should continue to investigate the impact that SRC has on mental health and quality of life.
Another issue was the difference in timeframe between SRC history and physical pain. SRC history was recorded as anyone that had previously sustained SRC in the past four years. By contrast, physical pain scores were recorded as to the level of pain experienced in the week preceding the study. Therefore, this disparity in timeframe may be reflected in the present findings and could explain why physical pain is associated with mental health and quality of life. However, while research tends to suggest cognitive impairment lasts for around a week,51,52 this study suggests that these effects persist over a longer period, and future studies should investigate the mid to long-term effects of SRC on cognitive ability.
Importantly, it must be noted that participants completed questionnaires and the cognitive task just once and were then separated into concussion groups based on their reporting of their SRC history. Due to this, we cannot know the cognitive abilities of the concussed group prior to their concussion. It is possible that this group would have always performed less accurately on the cognitive flexibility task, regardless of their concussion, and that we are falsely attributing this to the concussive event. However, our approach is typical within concussion literature due to practical issues associated with pre-morbid assessments. Therefore, the results still hold value, despite this limitation.
That said, the usual approach within concussion literature is to match participants for potential confounds so that the impact of SRC is evident. However, in this study, there was a significant difference between the biological sex of participants and their status as an athlete. As there are significant differences between these variables, they could both act as confounds when assessing the negative impacts of SRC. In this study, there were more males than females that had sustained SRC, and therefore the results here are perhaps more applicable to males. Moreover, athlete status is unlikely to effect the outcomes we were interested in as SRC, by nature, is only possible in athletes. In fact, some athletes could withdraw from sport due to sustaining SRC and experiencing its’ negative consequences (i.e., there were 5 participants that were non-athletes that has sustained SRC) and would therefore be classed as a non-athlete in this study. Therefore, although this limitation should be considered when inferring the results, it is perhaps better to evade this misclassification of athlete status in the analysis.
Conclusion & future directions
The present study attempted to investigate the impact of SRC and physical pain on mental health, cognitive ability, and quality of life. Despite what is often reported,51,52 SRC appears to have a long-lasting negative impact on cognitive ability. The SRC group performed significantly worse on TMT (A) and (B) than the non-SRC group with and without controlling for physical pain, indicating that SRC is responsible for this reduced accuracy. It is noteworthy that this effect was twice as strong for TMT(B) than (A). Additionally, physical pain was significantly associated with poor mental health and reduced quality of life, supporting previous literature that deems this to be the case.29,30 The effect on quality of life was stronger than any effect on mental health measures, and just under twice as strong as the effect on trait-anxiety. Given what we know about the link between physical pain and depression,14,16 and depression and quality of life, 59 it is sensible to treat them similarly. Sports teams could utilise pain questionnaires to identify vulnerable athletes that may require emotional support.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
