Abstract
Background
Past research on paediatric concussion awareness, management, impact and outcome priorities has focused on health care professionals and sports organizations, yet little is known about patient, parent and educator perspectives.
Methods
To address this knowledge gap, we conducted a qualitative descriptive study using semi-structured interviews with three participant groups: patient-participants including children with acute or chronic concussion; parent-participants including caregivers of children at risk for or with history of concussion; and educator-participants including teachers and athletic coaches from three Ontario secondary schools. We designed our interview guide to elicit participants’ perspectives across four domains: concussion awareness, concussion experience, support and resources, and outcome priorities. We analyzed our resultant data using a qualitative content analysis approach.
Results
Nine paediatric patient-participants, 17 parent-participants, and 14 educator-participants completed the study. Participants described concussion as a serious health concern and attributed greater concussion awareness to increased media attention and concussion protocol implementation within schools/sports. While most educator-participants regarded concussion protocols positively, some feared student manipulation. Parent- and educator-participants desired consistent information and resources from reliable sources. The impact of concussion ranged from a few days to prolonged absences (from school, sports, and socializing) and necessitated accommodations in both academic and sport settings. Short-term problems (e.g., decreased peer-contact) primarily troubled patient-participants, whereas long-term problems (e.g., impaired academics, psychological stress) concerned parent and educator groups.
Conclusion
Patients, parents and educators worry about the consequences of paediatric concussion. Initial concussion recovery in youth should focus on a timely return to academics and on minimizing social isolation by ensuring peer-contact during recovery.
Introduction
Paediatric concussion has been recognized as an increasing health problem, 1 with emergency department (ED) and physician office visits for paediatric concussion quadrupling over the last decade.2–4 Further, up to one-third of children with concussion experience post-concussive symptoms beyond one month. 5 These prolonged symptoms negatively impact quality of life, 6 reduce peer-contact and social activities,7,8 and can lead to prolonged absenteeism from school. 9
Evaluations of concussion awareness, management, and outcome priorities following paediatric concussion have thus far focused largely on the perspectives of front-line physicians and other health care professionals and sports organizations.10,11 Existing studies are skewed towards youth athletes rather than the general paediatric population,1,2 focus primarily on concussion guideline implementation,1,2 or target small samples of children with acute concussion rather than prolonged concussion symptoms. 3 In contrast, there is a paucity of research focused on patient, parent and educator perspectives on paediatric concussion, resulting in a knowledge gap in how concussion impacts patients’ activities of daily living at home and school, how activities should be prioritized during recovery, and how paediatric concussion guidelines are received by end users. As paediatric concussion guidelines and return-to-learn and return-to-play protocols differ depending on the targeted end-user, it is important to consider the perspectives of children and adolescents, their parents, and academic as well as athletic educators. As such, this qualitative study sought to describe the perspectives of children/adolescents with either acute or chronic concussion symptoms and their parents, as well as educators and coaches, relevant to paediatric concussion awareness, impact, management and outcome priorities.
Methods
We selected a qualitative approach known as qualitative description12–14 to present a comprehensive summary of the perspectives of paediatric concussion patients and those most closely involved in their daily care: parents and educators. Interviews focused on paediatric concussion awareness, the influence of concussion on daily activities and outcome priorities during recovery. The choice of domains of management and outcome priorities was two-fold: 1. to evaluate the first comprehensive paediatric concussion guidelines and inform the updated version, and 2. to provide insight into the most important patient-priority outcomes in concussion management to inform future clinical trials in paediatric concussion.
Participant groups
To capture a variety of perspectives within and across participant groups, we employed a maximum variation purposeful sampling method. 15 Paediatric patient-participants were selected to include children and adolescents aged 8 through 18 years with an acute (<24 hours of sustaining injury) concussion diagnosis 1 or chronic concussion (persistent symptoms beyond 4 weeks of injury) 5 and were recruited from the Children’s Hospital of Eastern Ontario Emergency Department (CHEO ED) (Ottawa, ON) and the CanChild Centre for Childhood Disability Research at McMaster University (Hamilton, ON) respectively. To increase heterogeneity, parent-participants consisted of the parents/caregivers of eligible patient-participants, as well as parents/caregivers of children and adolescents presenting to CHEO ED for a traumatic injury other than concussion (but with a past history of concussion). Eligible educator-participants were all academic and/or athletic teaching staff employed at one of three secondary schools (grades 9–12) in the Thames Valley District School Board within Ontario, Canada. These schools were selected by a study collaborator (LW; see acknowledgements) familiar with the district to represent a variety of settings including urban, suburban, and rural communities (collectively, these schools serve approximately 2500 students).
Data collection
After Research Ethics Board approval was granted by participating institutions [CHEO: Protocol Number 15/43X; McMaster University], participant recruitment began in May 2015 and continued until February 2016. Patient- and parent-participants were screened for eligibility by trained research volunteers (CHEO) or trained research assistants (CanChild Centre) using the same criteria as our team’s previous concussion collaboration. 5 Educator-participants received study information through their schools’ principal via email, which included a link to a secure Research Electronic Data Capture (REDCap) tool hosted at the CHEO Research Institute 16 to collect participant demographics and contact information. Interested participants were contacted within 7 days by telephone or email (for a maximum of five attempts) to schedule a telephone interview date.
Consent/assent was obtained from all participants (including the parents of all patient-participants) at the start of each interview. Interviews with children/adolescents preceded the interview with parents in the situation that both child and parent participated in the interviews, to prevent children from repeating their parents’ answers or opinions.
Data collection instrument
Data was generated using semi-structured interviews conducted via telephone for participant convenience. The interview guide (Table 1) was developed by the research team using the Dillman Tailored Design Method 17 and consisted of basic demographic questions and open-ended questions (including relevant prompts) to elicit participants’ perspectives across four domains. The selection of these domains was informed by existing literature and team members’ subject matter expertise, and included concussion awareness, experience with concussion, support and resources, and outcome priorities. Interviews were conducted by three trained researchers (study author [AG]; a paediatric nurse with qualitative research experience; and a MSc student with paediatric research experience). All interviews were audio-recorded and transcribed verbatim.
Individual telephone interview guides for children, parents and educators.

Data analysis
The team employed a deductive approach to qualitative content analysis 18 whereby transcripts were coded using preexisting codes relevant to the study domains. Modifications to codes were made throughout the analysis to better reflect the data. 19 The data analysis was informed by the team’s decision to use deductive coding based on the four a-priori defined domains. The team was open to revisiting these domains, had the data required it. Study domains and pre-existing codes originated from the literature review and the team’s subject matter expertise and was refined through ongoing research team consensus meetings. As the interview guides were tailored to each participant group, the resultant data were analyzed separately and then compared. We used NVivo 11 (QSR International), a qualitative data analysis software, to house the transcripts and facilitate the coding. One study author (AG) conducted the analysis with regular input from the team obtained through weekly peer debriefings.
Results
In total, 40 participants completed the study: 9 patients, 17 parents (13 with a concussed child and 4 with a non-concussed child), and 14 educators (Table 2). The interviews lasted approximately 30 minutes and the coded data was ultimately arranged into our four a priori defined domains. No new domains emerged from the data set during analysis.
Participant demographics.
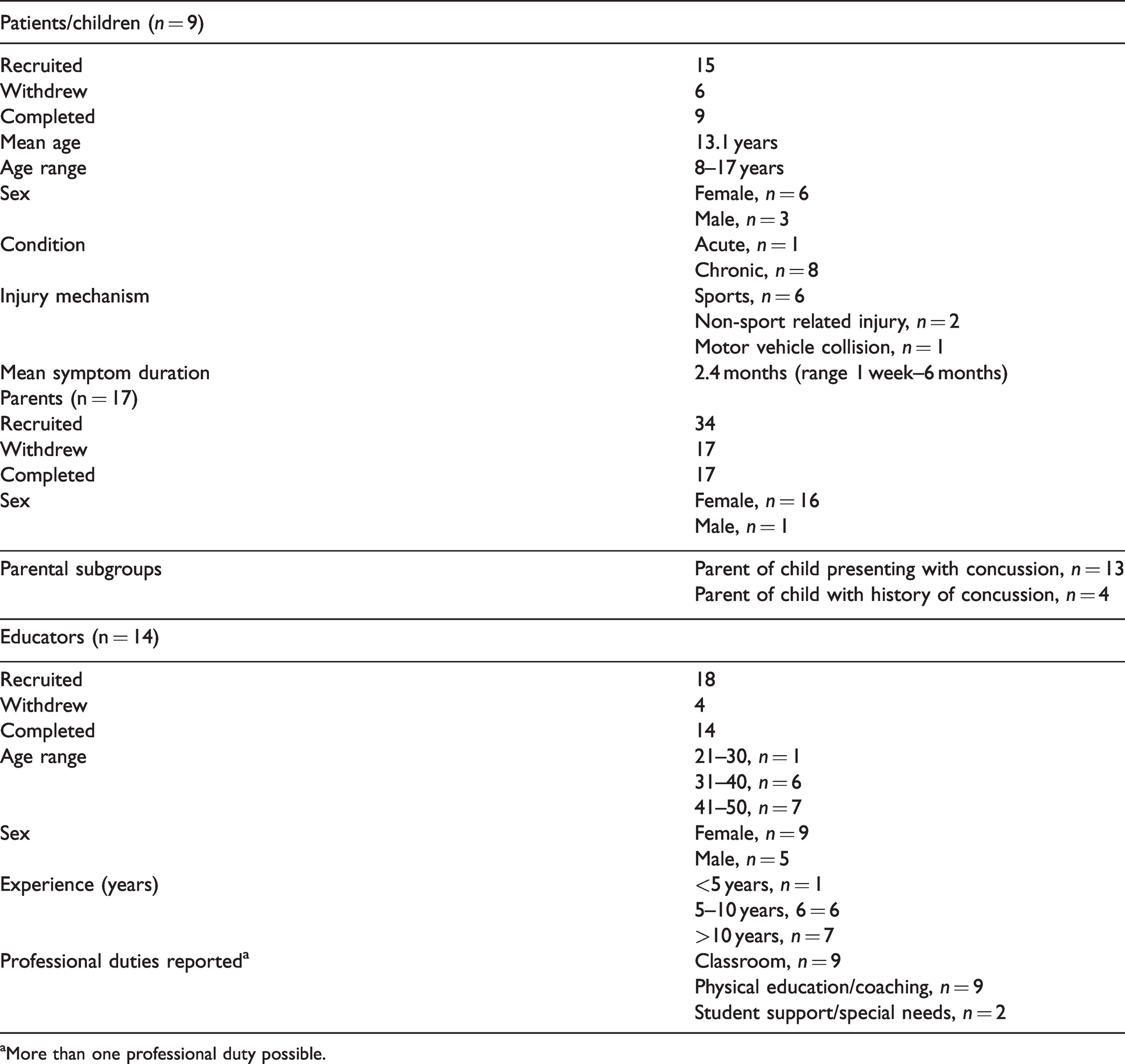
aMore than one professional duty possible.
Concussion awareness
All participants identified concussion as a priority health issue for school-aged youth. Increased media attention as well as the implementation of concussion protocols in school and youth sports were noted as important factors for a change in personal and public perception of the seriousness of concussion over the past ten years. One parent-participant [P1] commented: “I just find in general, people talk about it more or worry about it more.” According to an educator-participant [P2], concussions are handled differently now as compared to the past: “I can see that there have been concussion related injuries throughout the past that we haven’t really recognized […] Now we realize that those injuries were actually brain related injuries.” Another educator-participant [P3] added: “I think it’s probably been underreported for a lot of years, and kids have not been as successful as they could have been because of it.”
Parent-participants and educator-participants expressed that concussion has received more attention within schools in recent years. According to an educator-participant [P4]: “In the past few years I’ve seen much more attention around it in the school systems and we’re attempting to do due diligence around it, but it’s a process in the making because the information was not all available or we didn’t know where to look.” Some educator-participants discussed potential drawbacks of increased concussion awareness and the implementation of protocols at school [P5]: “My only concern is that it seems that there’s been a lot of diagnosis now. So, you know, from a teacher perspective we’re seeing a lot of students missing a lot of school because of their concussions, and even parents that are trying to diagnose them without any medical expertise.” Another educator-participant [P6] adds that: “There’s so much fear about concussions now because of the media regime; it’s not necessarily a bad thing but we’re also seeing that what has happened now is that teenagers are manipulating the system [to get out of exams].”
Experience with concussion
Participants reported varying degrees of the impact of concussion on daily activities, ranging from taking a few days off to prolonged absenteeism after which schedule and classroom adaptations were necessary to facilitate a gradual return to academic and athletic activities. Parent-participants and educator-participants expressed concern about prolonged absence from school, not only because of the negative impact on the child’s academic success, but also on the potential for psychological stress and mood disturbances due to limited peer contact. Paediatric patient-participants were most concerned about social withdrawal as a result of absence from school, sports and social activities. One patient-participant [P7] mentioned: “Avoiding music class and gym class I found actually caused more anxiety and depression. [Avoiding the things that you like doing] was probably one of the things that I really struggled with, because I’m one of those people that always needs to be doing something or making progress - so when you’re not allowed to do that it’s very hard.” Several patient-participants mentioned self-perceived pressure to return to academic and sports activities too quickly. [P8] “If you’re not practicing, you’re not working hard enough…It’s basically ‘it’s on you to make this progress’. When you’re not making progress, you feel like it’s on you even though you know there’s nothing you can do about it.” Only one patient-participant perceived pressure at school to perform at a ‘normal’ level during his recovery.
Several educator-participants experienced difficulty linking the severity of the injury to the estimated impact on the child’s activities. [P6] “I’ve seen both sides of the spectrum. I’ve seen 15 year-olds in their first year of senior high school football, and they never return. And […] it blows you away that the contact was so minimum. And then you see the other ones that you know it looks like they got hit by a freight train and they’re back in two weeks and they are okay.”
Support and resources
Approximately half of the parent- and educator-participants were familiar with existing concussion protocols or guidelines prior to participating in this study. Those parent-participants who had previously sought online resources described difficulties processing the volume and variation of concussion management recommendations available. Most parent-participants preferred receiving detailed information from health professionals. One parent-participant [P9] noted: “You can get really bombarded on the internet. I did really appreciate the handout that they gave at the hospital. I found that extremely helpful as a guideline, and it’s better when the information is provided by a health professional because then the rest of the family is more likely to take it.” Some parent-participants suggested supplementing the patient education materials supplied by hospitals with links to online resources for more in-depth and up-to-date information on concussion and its management.
Patient-participants indicated that support at school ranged from no assistance to increased breaks and gradual build-up of hours using half-day increments. Only one patient-participant received structured support in the form of an individual lesson plan. Several patients-participants stressed the need for better support at gradually building academic tasks on an individual level. As for sports, patient-participants felt that they received sufficient support from their coaches to gradually build their activities according to their symptom levels.
For teacher-participants, resource needs and availability varied across schools and by educator roles. While protocols for the recognition and management of concussion were implemented in all participating schools as a result of changes in Ontario legislation, it appears that only physical education staff (not all teaching staff) received formal concussion training. Similarly, our data suggests that physical education staff had better knowledge of protocol recommendations than strictly classroom-based teachers. In addition, temporary or substitute teachers were often unaware of the existence or specifics of concussion protocols, as information and training were offered only at the beginning of the academic year or during staff meetings. Resources for classroom adaptations or alternative learning environments were only available in one school.
All participants alike strongly supported the implementation of a standardized protocol for recognizing and managing concussion in all youth sports (school-based and non-school-based). All but one parent-participant felt that it is important to not only educate players, but also parents and coaches on concussion safety. Participants uniformly felt that it is important to educate children/adolescents about the importance of disclosing injuries sustained by themselves or teammates, to ensure that coaches and parents are informed once an injury occurs.
With regard to concussion protocol recommendations, most participants found return-to-learn protocols generally easy to follow. Most patient-participants noted that while it was ‘boring’, initial mental rest was perceived as an important step to recovery. Overall, patient-participants experienced most difficulties refraining from television and multimedia devices, as this increased their feelings of isolation from their peers and furthermore because many academic exercises are nowadays using online materials. Some patient-participants experienced difficulties with the return-to-learn schedule [P7]: “Actually the one [guideline] I have in front of me says to avoid music class altogether. When I tried that, it was very frustrating and it actually created anxiety and depression on top of the rest of my symptoms.” Another noted [P10]: “I felt like it was very hard to differentiate where you were because it felt like in some areas I felt like I was still in stage two, or I was in stage three, but in other parts I was kind of in stage 4. It was very hard to pinpoint what I actually should be doing to get better.” [P7] “It was really hard to find what I was supposed to do in the guidelines, because I couldn’t avoid music class and sound didn’t bother me at all, it was more light that bothered me.” For return-to-play protocols, participants groups uniformly preferred an early resumption of light aerobic activity to currently recommended complete physical rest following concussion until symptom-free.
Outcome priorities
Paediatric patient-participants were most worried about the short-term problems associated with concussion, including absenteeism from school, sports and social encounters. One patient-participant also noted the importance of preventing re-injury. Parent- and educator-participants shared this concern but added that long-term complications were of a growing concern. According to one educator-participant [P11]: “The long term is what we’re seeing in the news, but the short term - a lot of people don’t see that [a concussion] does impact their day-to-day living, especially school: they can’t concentrate, they’re not going to do the learning progression that they normally would do […] and I see it firsthand because I coach football, basketball, soccer, hockey, and I’m also a high school teacher.” Another educator-participant [P12] added: “So I think as adults and as coaches and educators it’s important that we remind them that this isn’t about today and next week and next month, it’s about forever [….] and I think we just can’t be too careful when it comes to your brain.”
Both parent- and educator-participants perceived a timely return to school as a primary focus during concussion recovery, followed by resumption of physical activity (including sports) and social activities.
Discussion
Our study found that paediatric concussion is a serious health concern to patients, parents and educators. Social withdrawal, removal from sports and falling behind on academic achievements were of biggest concern to patient-participants. The majority of parent-and educator participants expressed that their primary concern had shifted from short-term to potential long-term complications following paediatric concussion, including psychological stress, cognitive problems and potential for decreased academic achievement. Timely return to school was therefore described as the fundamental goal during concussion recovery. Increased media attention and greater awareness of concussion protocols were mentioned as important contributors to the evolving personal and public opinion on the perceived importance of paediatric concussion. Some educator-participants however felt that children and adolescents might not be as aware of these potential long-term complications, which might account for the difference in outcome priorities between children and their support network. Our study was focused on an exploratory examination of participant perspectives on pediatric concussion awareness, experience, support/resources, and outcome priorities; future research should consider explanatory analyses as to better understand the why and how of stakeholders’ perspectives in pediatric concussion.
Emerging evidence on potential short-term and long-term complications,7,20,21 recent concussion guideline recommendations advocating stricter follow-up and medical clearance of concussed athletes, 22 and changes in Ontario legislation23–26 might have led to increased identification and reporting of concussion in school-aged youth.
A recent, large prospective cohort study across 9 Canadian paediatric EDs demonstrated that up to 30% of concussed youth suffer from prolonged post-concussive symptoms one-month following an acute concussion. 5 All efforts should be made to improve paediatric concussion recognition and management to optimize concussion recovery, not only by health care providers but by everyone involved in the care for concussed youth, including parents and educators. Efforts should be made to incorporate a single standardized protocol for the diagnosis and management of concussion in school-aged youth for general use in schools and sports facilities. In addition, there is room for improvement in how this information is disseminated. Ideally, this information would be shared by schools and sports organizations at the beginning of the year or season, as well as by health professionals involved in the care of a children presenting with a head injury.
In addition to the use of concussion protocol guidelines, concussion legislation is another avenue to standardize the approach to paediatric concussion management. Following recent advances to better protect young athletes and educate coaches about the potential dangers of head injuries, Rowan’s Law (Bill 193) was passed in Ontario in 2018 27 as Canada’s first concussion safety legislation. 28 The law establishes removal-from-sport and return-to-physical activity protocols for players suspected of having a concussion. As concussion legislation has been demonstrated to have a positive effect on health care utilization, 23 this is an important step in optimizing concussion awareness and management in youth. In our study, educator-participants mentioned a wide variation in concussion education and knowledge not only between institutions, but also within organizations between athletic and academic staff. For any legislation to succeed, standardized protocols and training opportunities are necessary to ensure that teachers and coaches have the skills to accurately recognize and manage concussive symptoms. Including youth and their families in concussion education was positively received by patient- and parent-participants in our study. Although beyond the scope of our study, educating patients and their families on paediatric concussion diagnosis and management might further optimize paediatric concussion recovery through improved adherence to protocol recommendations. 29
While parents mentioned utilizing online resources to better recognize and manage symptoms during concussion recovery, many struggled with the volume and variation in recommendations available. Further, parents uniformly preferred health care professionals to online resources as the primary source of concussion information. These findings are largely in line with those described in another study exploring caregivers of youth athletes in the United States. 30 That study, as well as our own, suggests that more uniform and detailed patient education material (e.g., hand-outs) provided at the time of health care visits is the preferred channel for patients and their families to receive information to recognize and manage concussion and post-concussive symptoms. According to our parent-participants, handouts should include more detailed examples of cognitive and physical activities that are safe as well as those that should be avoided during recovery.
Rest has long been considered the “cornerstone of concussion management”. 21 An initial period of full mental and physical rest until symptom resolution, as recommended by paediatric concussion guidelines at the time of study data collection,21,31 was for many patient-participants and their families challenging to achieve. All three participant groups described difficulties adhering to strict rest recommendations following concussion, particularly physical rest. Participants were uniformly in favor of a more active approach to return-to-physical activity, as long as deemed safe by medical professionals. A recent large comparative effectiveness study demonstrated that persistent post-concussive symptoms at one-month were significantly less prevalent in children who engaged in early physical activity compared to those who reported complete physical rest at one-week, and irrespective of symptoms, approximately 70% of youth participate in physical activities within one-week following an acute concussion. 32 Similarly, recent recommendations from an international consensus statement on concussion in sport suggest that after a brief period of rest (48 hours) patients can be encouraged to gradually become more active (while staying below cognitive and physical symptom-exacerbation thresholds). 1 While our findings suggest that this recommendation would be acceptable to youth as the desire to participate in physical activity was expressed by our patient-participants, the optimal timing, type, intensity and duration of this activity requires further research. 33
Limitations
There are limitations to consider when interpreting the findings of this study. First, our team members are clinical and published experts in the field of paediatric concussion. It is possible that team members’ preconceptions of concussion and its effects on patients and families may have influenced our choice of study design, data collection and analysis. Second, as deductive coding was used to analyze four a-priori selected domains, it is possible that a different coding scheme or inductive coding might have revealed different, although likely not incompatible, results. Third, data was collected for an a-priori set time period. Post-analysis, the team concluded that additional interviews would likely not enhance our understanding of the findings. Fourth, we did not stratify enrolment based on sex or gender. Since female gender is an important predictor of prolonged post-concussive symptoms, 5 this likely explains the 2:1 female to male ratio in our patient-participant sample. However, a more balanced sample would likely not have led to different results. As a qualitative study based in one Canadian province, our findings are not necessarily representative of other regions. We attempted to increase transferability of our findings by recruiting various participant groups from multiple sites within Ontario; future studies using larger sample sizes drawn from geographically dispersed sites would also provide greater representation of the paediatric concussion population and the transferability of those study’s findings.
Conclusion
Patients, parents and educators identify concussion as a serious health concern with reduced peer-contact, potential for decreased academic achievement, and psychological stress as principal concerns. Differences exist in the perceived outcome priorities post-concussion; short-term problems were of biggest concern to patient-participants, whereas the primary concerns for parents and educators are potential long-term complications. Timely return to school was identified as the priority during concussion recovery, in order to enable peer contact and resume academic activities. Educational materials should be tailored to ensure instructions resonate with all intended end-users and optimize concussion recovery at home, school and sports.
Footnotes
Acknowledgements
The authors would like to thank Corinne Kagan, Ruth Wilcock, Linda Weir, Janice Gray and Kristina Rohde for their review of the study design, interview guides and analysis. The authors thank Kaylee Eady for critical appraisal of the early manuscript draft. The authors thank Dale Dalgleish and Justin Piche for their roles in conducting the telephone interviews. The authors also thank the student volunteers and research assistants involved with participant recruitment, and the student volunteers for their help with transcribing interviews for analysis: Brandy Dunfield, Megan Singh, Emma Gibbons, Thomas Bogdanowicz, Bilal Kabir, Nooh Kabir and Nell Farion.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and publication of this article: This study was supported by a demonstration grant from the Ontario Child Health SPOR Support Unit and funding by the Ontario Neurotrauma Foundation.
