Abstract
Objective
Absent adequate randomized control trials to inform appropriate treatment for concussion in pediatric patients, guidelines have been developed based on expert opinion and observational data that may not apply to all groups. This study examines differences in the previous clinical care between concussed patients who present in pediatric practice and specialty clinics. Differences found might influence treatment recommendations for each setting.
Study design
Prospective data collected from a pediatric practice in 2011 to 2013 were compared to chart review data from two specialty clinics between 2015 and 2017. In all three groups patients 11–19 years of age with an ICD9 billing code for concussion were included if they met the 4th International Consensus definition of concussion. Patients were excluded if hospitalized or had abnormal CNS imaging.
Results
The time between injury and presentation was substantially longer in specialty clinic patients versus those seen in the primary pediatric care office. (median 10 vs. 2 days-p < 0.001) Primary care patients presenting had higher rates of immediate rest after injury, 61.4% vs 27.9% (p < 0.001). More specialty clinic patients had been seen in the emergency departments prior to presentation (47.5% vs. 18.8% p < 0.001) regardless of rest status at presentation to the office.
Conclusion
Several differences in previous clinical care between the groups were found. These included the time of presentation from injury, rates of cognitive rest both immediate and non-immediate, and emergency department visits. These differences may have implications for management recommendations. Accordingly, the appropriate treatment for patients seen by the primary pediatric care physicians may be different from those referred to specialty care. Given these findings randomized controlled trails should be conducted independently in both groups of patients.
Introduction
The published estimates of the annual number of pediatric concussions in the United States vary depending on the definition1–3 of concussion with estimates as high as 1.1 to 1.9 million annual occurrences 1 in children under 18 years of age. Of these, only a minority (approximately 10%) are seen in emergency rooms. 3 Primary pediatric care physicians see the majority of patients <18 years of age who seek care for concussion.4–8
Despite the large number of patients affected, there is little data from randomized control trials on how best to treat these patients and there remains a significant controversy about the role of cognitive rest. To date there have been only four randomized control studies, evaluating cognitive rest including pediatric patients, each of which had less than 100 patients and a limited follow-up period of 10 days or less.9–12 A number of observational studies (see Table 1) examining the benefit of cognitive rest have been conducted but are all subject to confounding by indication, such that patients with different levels of symptoms receive different treatments and recover at different rates. In addition, there is a wide variability seen in concussion etiologies, symptoms and signs, and post-concussive recovery. Therefore, recent guidelines and reviews which provide guidance on the use of cognitive rest in the management of concussion are based on incomplete data and may not be applicable to the general population of pediatric concussion patients. 13
Overview of clinical trials performed in pediatric concussion patients.
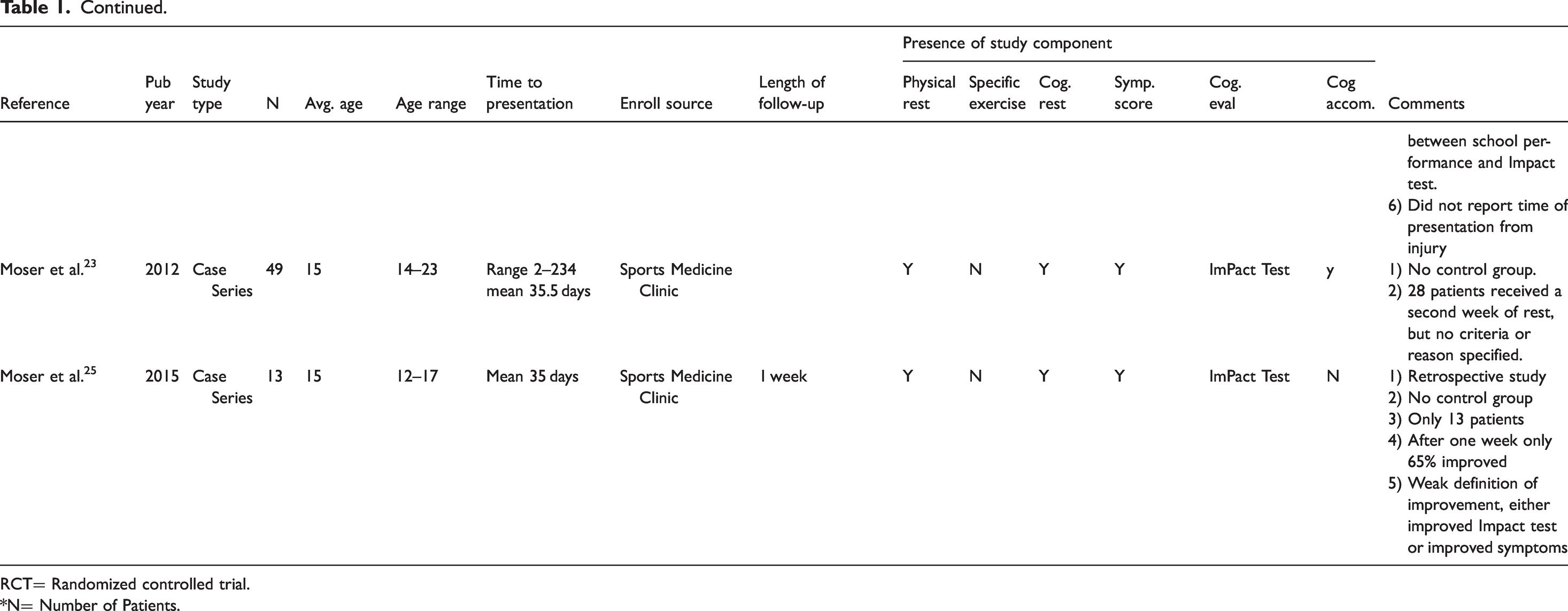
RCT= Randomized controlled trial.
*N= Number of Patients.
Also, as a consequence of the lack of evidence-based data, the guidelines for management of concussion are based on clinical experience and written primarily by specialists treating the concussed patient.14–18 If there is a difference in the population of patients seen by specialists and the primary care pediatric practice, it is possible that the guidelines may not properly reflect the appropriate care for the majority of concussed patients. To our knowledge there are no studies in the literature comparing the clinical characteristics of care at presentation of concussed patients seen in the primary care setting versus the specialty clinic. This study was undertaken to better understand the differences in previous clinical care at presentation between the population of concussed pediatric patients treated in a primary care pediatric office and those seen in a specialty clinic. We examined demographics, time interval between injury and presentation, presence and absence of cognitive rest, and previous ER visits before presentation. We were particularly interested in cognitive rest as its use in the management of concussion has consistently been mentioned in the guidelines but remains controversial.19–21 In addition there is one study which demonstrates the lack of immediate cognitive rest prolongs recovery 22 and three studies claiming to show limited benefit of cognitive rest but which were not properly designed.23–25 Choices made about future care will be related to the population of patients seen and should be understood in that light.
Methods
This study was approved by the Institutional Review Board of Cooper University Health System.
One of the authors of this study (BT) has a long-standing interest in the treatment of concussion and had prospectively collected data on patients presenting with a concussion to the primary care pediatric practice in Cherry Hill, New Jersey, and who were enrolled from 12/2011 to 4/2013. Information on the specifics of the data collection and analysis has been previously published.22,28 For comparison, two specialty clinics involved with concussion care in the Cooper University Health System, Camden, New Jersey were approached and agreed to participate in this study: 1) the Sports Medicine Clinic, designed to care for sports-related concussions, and 2) the Pediatric Concussion Clinic, designed to see patients with concussions sustained from non-sports activities or non-traditional sports. These specialty clinics were selected because they serve patients from seven locations in southern New Jersey, with a catchment similar to the primary care pediatric practice. All the clinic offices used the same electronic medical record system. Although there was 4 years difference between the two data collection, no changes in patient presentation or therapy had been implemented over that time.
The medical records for all patients seen in these two clinics with an ICD9 billing code for concussion with or without loss of consciousness (850,850.0,850.5,850.11) between August 2015 and May 2017 were reviewed. Patients from the primary care pediatric practice and both specialty clinics were included if they were 11 –19 years old, not in college, and had sustained injuries which resulted in concussion meeting the definition of the 4th International Consensus Statement on Concussion. 20 The minority of patients who had previously been admitted to the hospital or who had abnormalities on CNS imaging were excluded. We were concerned that these few patients would differ significantly from patients treated only as out patients or had normal CNS imaging.
Concussed patients seen in the primary care pediatric practice were enrolled prospectively. Data was collected and recorded at the time of presentation. The data from the concussed patients seen in the specialty clinic also had been collected prospectively as part of their routine care and was obtained by chart review. The data collected included: age, gender, grade in school, time from injury to presentation, school attendance at time of presentation, whether there had been an ER visit before presentation, and whether or not the patient had undergone any immediate cognitive rest following the injury. Information such as memory loss, LOC, previous concussion, ADD and mood disorders was based on the history taken at the time of presentation. Because of the differences between the two groups in the data collected, the criteria for considering a patient to have undergone a period of cognitive rest differed. In the specialty clinic, to be considered at cognitive rest a patient had to have been at home not participating in sports and not attending school for one or more days. In the primary care pediatric office to be consider at cognitive rest a patient also had to have been not doing homework and not using a computer. Immediate rest was defined as having at least 24 hours of rest immediately following the injury.
Statistics
The primary analysis was a comparison of the demographic features between the two clinical populations. Differences in the demographics were assessed using an ANOVA. Patient characteristics were assessed using simple linear regression, Poisson regression, and median tests as appropriate. Given the descriptive nature of this study, the majority of the results are presented with 95% confidence intervals to provide an estimate of precision in lieu of p-values. STATA SE 15.1 was used for the statistical analysis.
Results
Approximately 100 patients were seen in each of the three practices: the primary care pediatric practice (n = 101), Pediatric Concussion Clinic (n = 105) and Sports Medicine (n = 99). Consistent with their specific focus, 92% of the patients seen at the Sports Medicine clinic and 52% of the patients in the Pediatric Concussion Clinic reported suffering a sports-related concussion for a combined specialty clinic average of 71.6% compared to 65.3% in the primary care office Since there were only small additional demographic differences among the two specialty settings (Supplement 1), the two specialty groups were combined to be compared to the patients seen by the primary care pediatric physician. Sex and age distributions were similar, but rates of loss of consciousness, attention deficit disorder, and mood disorders were all higher in the specialty clinics (Table 2). The referral source for the combined specialty clinics and the primary care pediatric practice is shown in Table 3.
Patient and concussion incident demographic data – primary care versus combined specialty clinic.
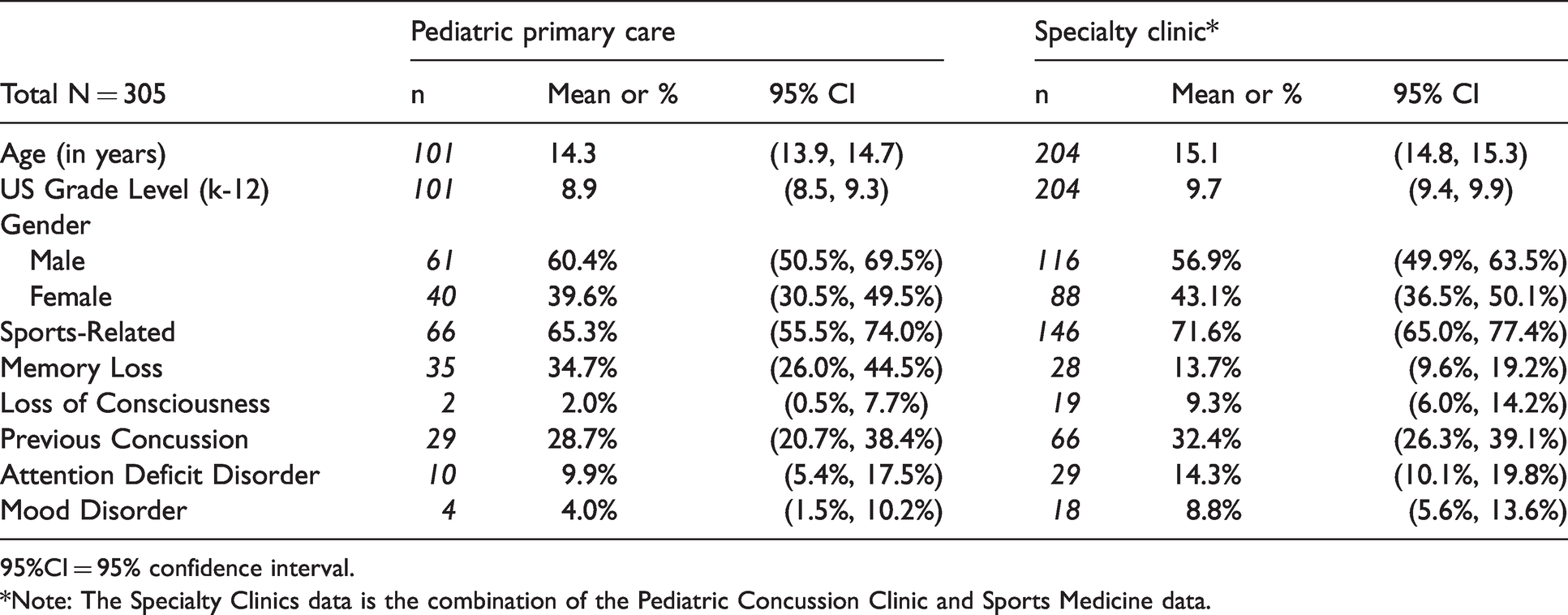
95%CI = 95% confidence interval.
*Note: The Specialty Clinics data is the combination of the Pediatric Concussion Clinic and Sports Medicine data.
Referral source by speciality clinic*.
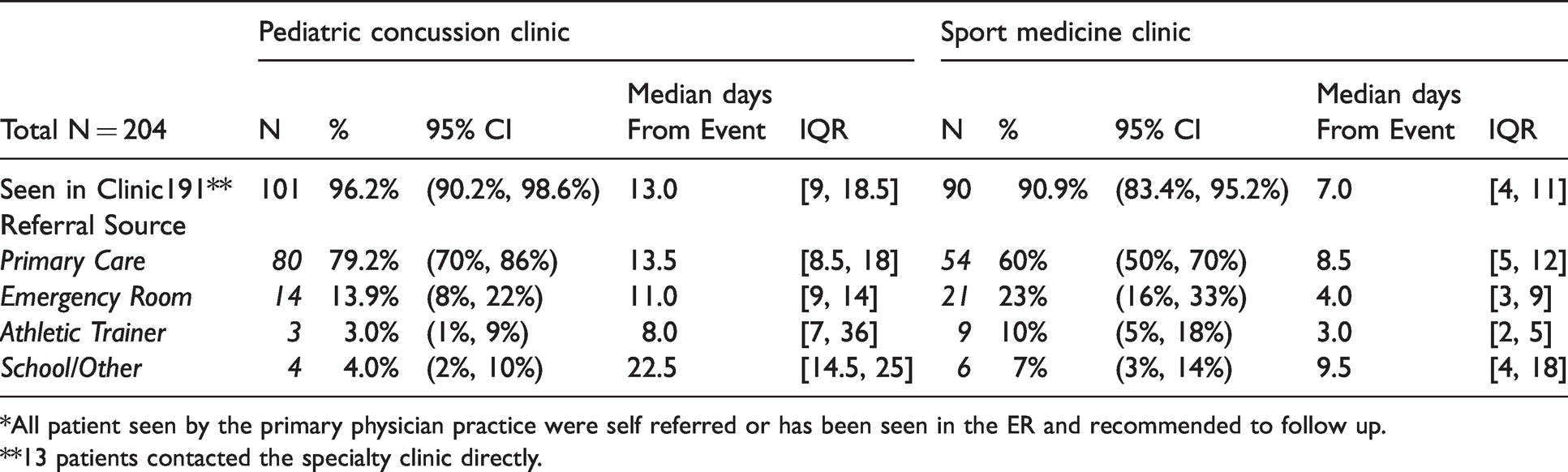
*All patient seen by the primary physician practice were self referred or has been seen in the ER and recommended to follow up.
**13 patients contacted the specialty clinic directly.
Differences were seen in previous ER visits, timing of visits to the clinic, and the presence or absence of rest before presentation (Table 4). A greater number of the specialty clinic patients had initially presented to an emergency room (47.5% versus 18.8% P < 0.001). The time between injury and presentation was substantially longer in the specialty clinic patients compared to the primary care pediatric physician (median 10 days [IQR 1–3 days] versus 2 days [IQR 5–16 days] – p < 0.001, respectively -Table 4). Even in patients first seen in the emergency room, the time to presentation to the specialist compared to the primary care pediatric practice did not change (median 10 days [IQR 1–3 days] versus 2 days [IQR 5–16 days] – p < 0.001) (Table 4). Another difference was that more patients seen in the primary care pediatric practice had undergone immediate rest following the injury and prior to their visit, compared with those seen in the specialty clinics, 61.4% versus 27.9% respectively (P < 0.001) (Table 4).
Initial emergency room visit, time from injury to visit, exposure to types of cognitive rest.
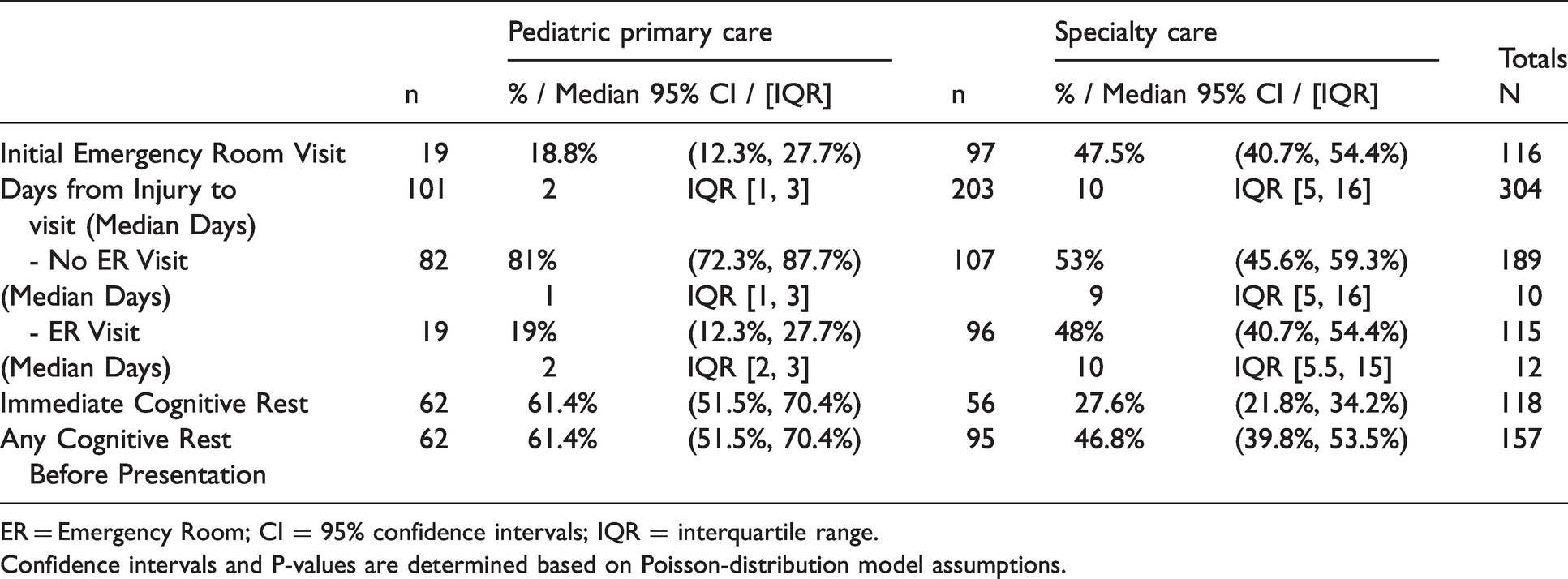
ER = Emergency Room; CI = 95% confidence intervals; IQR = interquartile range.
Confidence intervals and P-values are determined based on Poisson-distribution model assumptions.
Discussion
To our knowledge this is the first study to compare the pre-presentation care of pediatric concussed patient who present to a primary care office versus a specialty clinic. We compared previous clinical care characteristics at presentation between the two populations and noted a substantially longer period from time of injury to presentation, higher rates of previous ER visits, and lower rates of any cognitive rest in the specialty clinic population. Of primary importance in considering the appropriate care of patients seen is the length of the delay from injury to being seen with a median of 2 days (primary care pediatric practice) versus approximately 10 days for the specialty clinics. This was true even though the policy at both specialty clinics was to see patients referred from the Emergency Department within 2 days if requested by the patient or caregiver. Nearly all the specialty clinic patients were referred by an emergency room physician or a primary pediatric care physician. The reason for the delay is unknown. Difficulty in obtaining insurance approval for the referral is one possible explanation. Another is that parents waited to see if the symptoms would resolve and if the symptoms continued, followed through with the referral. One possible explanation for continued symptoms in the specialty clinic group is that there were more patients with ADHD and mood disorders in that group (Table 2). Both have been associated with prolonged recovery.26,29
Another important difference was the frequency of reported rest immediately after injury. In the primary care pediatric practice setting, 61.4% of patients reported immediate rest before being seen versus 27.9% in the specialty clinic. In addition, only 39.6% of the patients in the primary care pediatric practice had gone back to school with symptoms before being seen versus 53.7% in the specialty clinic. Although there may be several possible explanations for fewer patients with immediate cognitive rest being seen in the specialty clinic, one possibility is that patients who had rested immediately had recovered faster and did not need to follow through with visits to the specialty clinics.
The goal of the management of pediatric concussions should be to eliminate symptoms and return patients to their pre-concussed academic cognitive level as quickly and safely as possible. One controversial tool in the management of concussion is cognitive rest. The first published guidelines for the management of concussion developed in 2001 by the Concussion in Sport Group international conference recommended cognitive and physical rest until symptom free. 19 Again in 2008 and 2012 the guidelines state “The cornerstone of concussion management is physical and cognitive rest until symptom free.20,27 However, most recently in 2016, the recommendations were modified to say that after a brief period of rest (24 to 48 hrs.) patients could be encouraged to increase cognitive and physical active so long as such activity did not bring on worsening of any ongoing symptoms. 21 This change was reportedly based on clinical trial data; however, in the literature there are only four relatively small RCTs which provide only limited information on which to base this change in guidelines (see Table 1). Of these RCTs, three enrolled patients from an emergency room and one from athletic trainers.9–12 Each of these studies was small and did not follow patients beyond 10 days, and none of these studies addressed the question of cognitive rest as it relates to symptoms while in school and academic performance. Thomas et al., is a study of 88 patients seen in the emergency room who were assigned to either two days or five days of cognitive and physical rest, is the most referenced study in support of the lack of benefit of cognitive rest. 11 Patients in both groups returned to school with symptoms and patients were only followed ten days or less. Over the 10 day follow-up period 67% in the 5 day group and 63% of the 2 day group experienced symptom resolution which is of unclear significance given the small sample size (N = 88). Another study in 2017 by Sufrinko et al. included 93 patients, aged 11–18 years, randomized after having been seen in the ER 12 with a larger group (23 patients) who had suffered loss of consciousness. Again, the maximum time of restricted school, extracurricular work and physical exertion was five days. In addition, the control group allowed the emergency department physicians to freely recommend activity restriction based on their individual standard of care without reporting their recommendation for rest making it impossible to know if a difference exists between the therapeutic groups. In addition to these four randomized trials, there are a few observational studies that examine the effect of cognitive rest on recovery. Two were case studies; one was a retrospective cohort study and two were prospective cohort studies.23–25,30,31
As previously reported by Taubman et. al., the patients in that study’s primary pediatric practice group became asymptomatic on average of 11 days.22,28 The concerns raised specialist about the negative effects of school absence may well apply to patients beyond 10–14 days but it is unclear if these concerns apply to the earlier group. 32 Guidelines that are primarily based on expert opinion of how to treat patients beyond 10 days may not apply earlier in the process in the primary care setting earlier in the process. A randomized control trial with appropriate timing of assessment is needed for a definitive answer.
Limitations
As in all observational studies, our study has a number of limitations that must be considered.
Of primary importance is that we are only able to demonstrate association, not causation, given the nature of observational studies. However, our study does show that the patients seen in specialty clinics are clearly different from those seen in a pediatric private practice. Whatever the cause of the delay in presentation to the specialty clinics, the percentage of patients undergoing some degrees of cognitive rest was substantially lower in the patients with continued symptoms at an average of 10 days. While causality cannot be proven, this association warrants a more careful consideration than the small and underpowered randomized trials conducted thus far. Another issue is that our study included only one pediatric primary care practice and two specialty clinics. It is possible that the populations reported do not represent the general population. However, the primary care pediatric practice in this study is part of a group of 60 primary pediatric care centers with a diverse urban/suburban patient base and with the same catchment area as the two specialty clinics. Another limitation is that the data from the primary care pediatric practice were collected prospectively, whereas the data from the specialty clinics were obtained from chart review. The information in the specialty clinics was documented at the time of presentation and it is standard to record the type and timing of injury, and the immediate post-concussion treatments as an integral part of patient care. While recall bias is a potential problem, given the significance attributed to a concussion it is unlikely that both the child and the parents would not remember the details of the events and treatments over the past 10 days (on average).
The chart review of the specialty clinic patients only allowed us to determine the state of cognitive rest in terms of whether the patients were in school or sports. It is possible that those not in school were on their computers or doing homework. This may result in an over estimation of the number of patients who had a period of cognitive rest in the specialty clinics. This would only increase the differences in cognitive rests between the two groups.
Another limitation to be considered is that specialty clinic data were collected for a period of four years after the pediatric primary care clinic. While it is possible that the treatment of concussion and the distribution of patients who went to an ER versus the primary care pediatric practice may have changed, it is unlikely that the pre-presentation conditions would have changed. If there were changes it should have been an increased awareness of the existence of the specialty group and earlier visits. While it is possible that a change in initial treatment over time may have affected the results, we have previously noted the change in recommendation for limited cognitive rest was only published in 2016 and it is unlikely that such a recommendation would not have been widely accepted before the end of the second data collection. Any increased public awareness about the importance of concussion injuries would only serve to decrease the time from injury to presentation. Although it is still possible that the change in timing may explain a portion of the difference in cognitive rest observed between the two practices, we do not believe it is the only factor and it does not diminish the need for additional studies to examine these issues.
Conclusion
In the absence of data from adequate randomized controlled trials, the differences this study found between the concussed patient presenting to the primary care pediatric physician versus the specialist raises the issue of the need for guidelines to address different approaches in the two patient populations. Guidelines written for patients seen in specialty clinics after an average of 10 days post-concussion may not apply to the care that should be provided by the primary pediatric care physicians seeing patients at an average of 2 days after concussion. These differences reflect the fact that concussed patients do not present as a monolithic group and suggests that perhaps treatment recommendations should not be monolithic either.
Our data analysis showed a substantial difference in time from injury to presentation between primary care and specialty clinics and the difference in cognitive rest between the two groups. We hope this paper will encourage high quality randomized studies incorporating the spectrum of injury classification, timing of the presentation, and status of the patient at the time of presentation in deciding on the management of concussed patient. Given our findings and the limited evidence to guide us, we would like to propose that the care of concussed pediatric patients be considered for future study in four phases: 1) immediate post-injury (0–24 hrs.); 2) acute post-injury follow-up (1–7 days); 3) an intermediate phase (8–30 days); and 4) chronic care greater than 30 days (which was not collected in this study – see Figure 1). In the immediate post-injury phase, the patient is seen in the emergency room or in their primary care pediatric practice. This is followed by the acute post-injury care, which is generally overseen by the primary pediatric care physician or the patient’s parents. Patients who continue to have symptoms into the intermediate phase, (i.e. longer than 7 days) are those likely to follow up on a referral to the specialists for ongoing care. The treatment of patients should take into account the level of injury, time to presentation, and amount of cognitive rest before presentation.
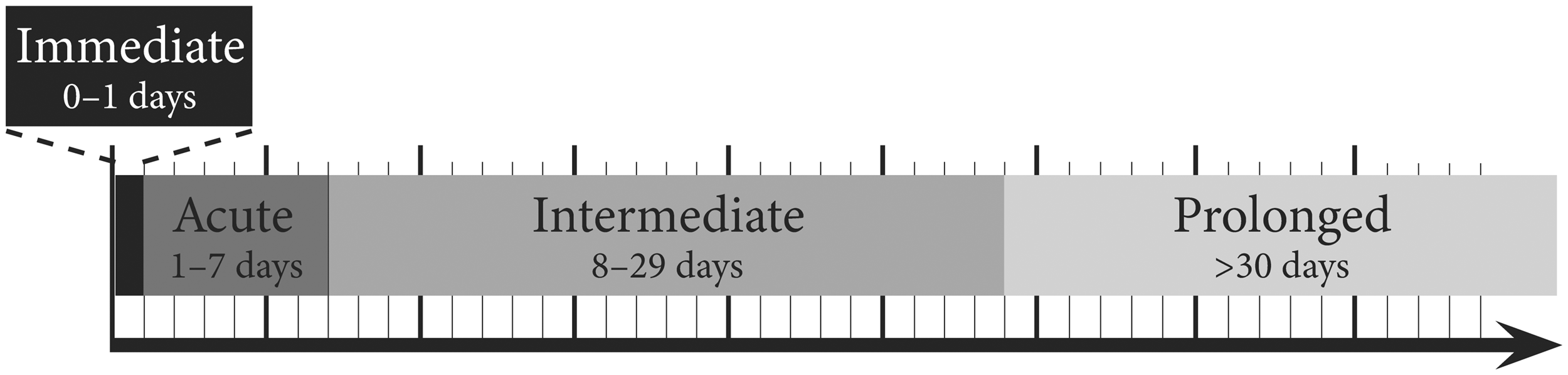
Phases of Concussion Care.
Until such studies are conducted, we cannot know the effect of the timing of returning to school with the primary outcome being symptom free and functioning at their pre-concussion academic level.
Supplemental Material
sj-pdf-1-ccn-10.1177_2059700221998921 - Supplemental material for The care of the concussed pediatric patient prior to presentation to primary care pediatrician versus concussion specialists: Implications for management
Supplemental material, sj-pdf-1-ccn-10.1177_2059700221998921 for The care of the concussed pediatric patient prior to presentation to primary care pediatrician versus concussion specialists: Implications for management by Bruce Taubman, A Michael Luciani, David B Gealt, Thomas P Drake, Philip Cochetti and John T Farrar in Journal of Concussion
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
