Abstract
Introduction
Scrotal burns resulting from wound care are a rare but preventable injury compared to the wide spectrum of post-circumcisions related complications documented. We report an inadvertent cetrimide-chlorhexidine antiseptic scrotal burns due to post-circumcision dressing and review the literature on genital chemical burns.
Case Presentation
A 6-week-old baby presented with a 3-days history of worsening scrotal burns following smearing of undiluted cetrimide-chlorhexidine as dressing post-circumcision. Examination revealed a healthy baby with non-tender non-specific multiple ulcers and pan-erythematous scrotum. Wound swab isolated Klebsiella and Pseudomonas spp.
Discussions
Although there was no clinical complication during procedure, the wrongful post-operative care resulted in scrotal burns. The isolated uropathogens did not result in sepsis or Fournier’s gangrene, we believe this preventable burn was eventually reported due to the worsening progression over the period, albeit with minor adverse effects.
Conclusion
Post-circumcision instruction for cetrimide-chlorhexidine use by caregiver must be understood to avoid scrotal burns.
Lay Summary
Scrotal skin burns from chemical agent: Isolated scrotal skin burns are not common and even rarer when they are caused by prescribed medical solution. A neonate was brought in by the parents with complain of developing watery containing swellings on the scrotum that later bust and leads to peeling of the scrotal skin. The mother noticed this after applying dressing solution as part of the measures to prevent circumcision wound infection. Even though the child looked well, the large scrotal surface without skin cover could become a common point for bacteria entry into the body and its consequences. Even though our test isolated 2 different types of disease-causing bacteria from the scrotal wound, this child was managed well and the wounds healed without any further problem. The lessons: 1. circumcision is the commonest surgical procedure performed. 2. This incidence may only be the tip of the iceberg. 3. The parents brought him because it was getting worse. 4. It is a preventable injury by just using the agent in accordance with recommendations.
Keywords
Introduction
Scrotal burns resulting from antiseptic use are rare with most attributed to diaper reaction or unhygienic perineal care in children. Scrotal burns resulting from cetrimide-chlorhexidine smear may be the rarest of post-circumcision complications. Cetrimide-chlorhexidine is frequently used as a household bathing agent and surgical antiseptic and as such it has long been viewed as a safe antiseptic.1,2 Such burns following circumcision, the most common surgical procedure in our setting, may not be an isolated injury and poses significant concern to caregivers. This case report seeks to create awareness about the potential effect of undiluted cetrimide-chlorhexidine scrotal smear and our management outcome following the burn injury.
Case presentation
A 6-week-old male infant was brought to the urology unit with a 3-day history of progressive ulceration of the scrotal skin. Three days prior to appearance of the lesions, he underwent a religious circumcision (Khattan) using open plastibell insertion method at a primary healthcare center as a day case. The mother started to smear undiluted cetrimide- chlorhexidine on the external genitalia twice daily 24-hour after surgery as part of the post-circumcision instruction for good hygiene. Three days later, the mother noticed a few blisters on the scrotum as the prepuce expectantly became necrotic. The blisters progressively became worse, peeled off with resultant ulcers (Figure 1). There were no other significant symptoms. She had not applied a diaper after circumcision nor any form of medication or cream except the undiluted cetrimide-chlorhexidine. There is no known allergic disease in the family. Examination revealed a healthy neonate. The scrotum was observed to be erythematous throughout, with gangrenous preputial skin on the dorsal glans penis and non-tender antero-inferior ulcers (Figure 1). There was no discernible scrotal discharge, and the testes were palpable and normal. Table 1 shows the blood cell indices and an elevated C-reactive protein levels. Wound swab for culture isolated Klebsiella spp and Pseudomonas spp, demonstrating sensitivity to only Amikacin and Gentamicin. Clinical management comprised twice daily oral cefuroxime administration which was started on arrival, wound cleaning with 0.9% normal saline and shea butter moisturisation. The redundant gangrenous preputial skin spontaneously detached within 2 days, with complete scrotal ulcers resolution achieved in 6 days (Figure 2), resulting in successful patient discharge and parental satisfaction.

Erythematous scrotum with ulcers and gangrenous redundant prepuce.
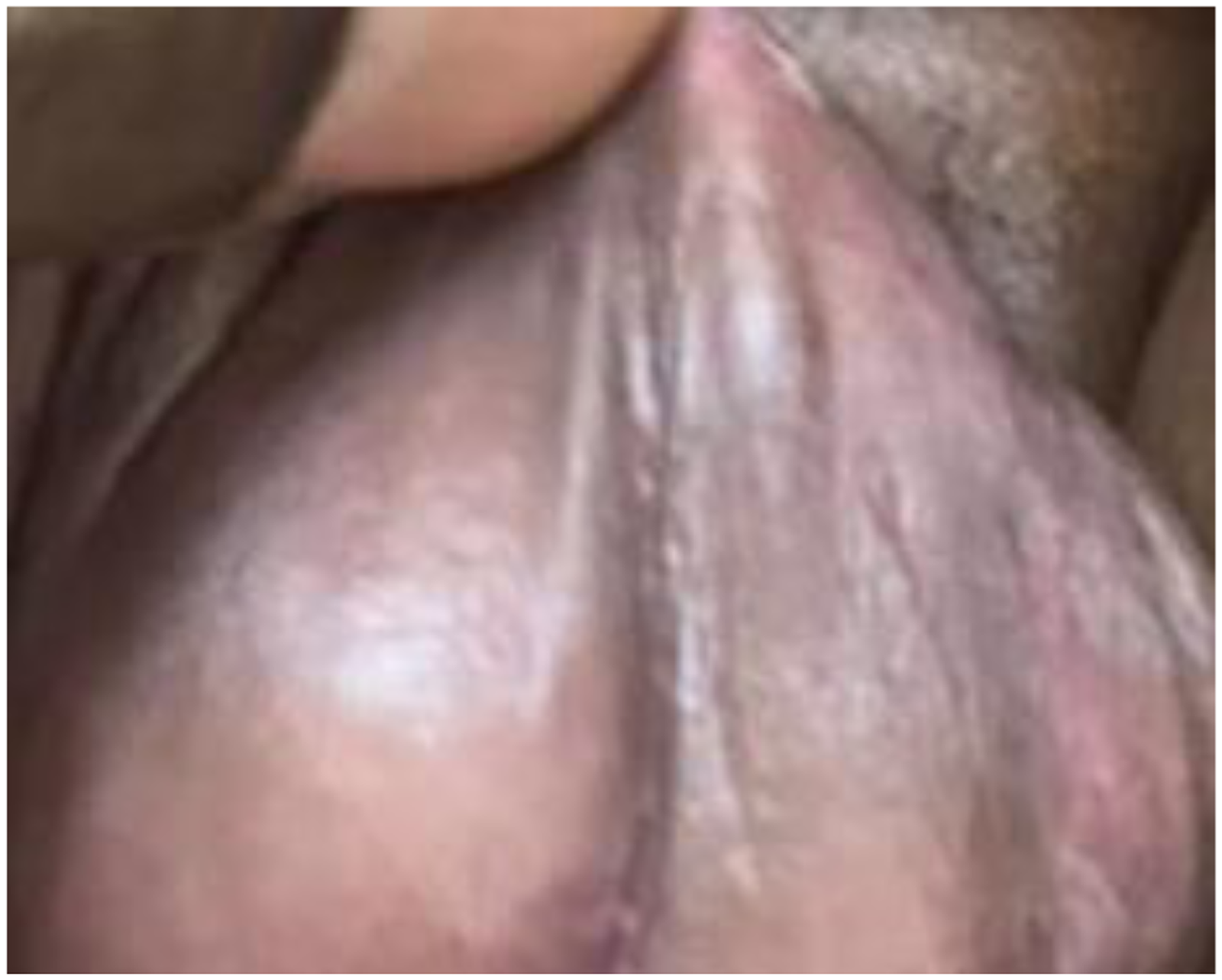
Spontaneous resolution after 6 days of treatment.
Blood investigations at presentation.

Discussion
Circumcision represents the most prevalent surgical intervention performed at peripheral health-facilities in Ghana, predominantly motivated by religious and cosmetic considerations. 3 While generally perceived as a low-risk procedure, potential complications including intraoperative erectile tissue damage, hemorrhage, postoperative pain, urinary retention, and meatal stenosis have been reported. 4 The surgical procedure undertaken on a 6-week-old infant aligns with typical religious circumcision practices. 5 In this specific case, a scrotal burn was associated with postoperative wound management following an otherwise uneventful surgical intervention. Circumcision sides exposed to microbial contamination can potentially precipitate severe complications such as Fournier's gangrene and sepsis.6,7 Consequently, infection preventive protocols are imperative, including thorough cleansing of the scrotum and perineum to mitigate faecal contamination risks. 8 Antiseptic agents, including guided concentrations of cetrimide-chlorhexidine, are typically employed by caregivers to maintain external genital hygiene. However, in this instance, the application of undiluted cetrimide-chlorhexidine suggested a potential misunderstanding of product instructions or clinical guidance. Savlon's active constituents comprise Cetrimide 0.5% w/w and Chlorhexidine Digluconate 0.1% w/w. 9 The quaternary ammonium compound cetrimide, a mixture of tetradonium bromide, cetrimonium bromide, and laurtrimonium bromide, serves as an antiseptic agent typically utilized at 1–3% concentration for wound cleansing. Potential adverse effects include cutaneous manifestations such as rash, irritation, and dermal desiccation.10–12 Chlorhexidine (molecular formula C22H30Cl2N10) functions as a broad-spectrum antiseptic and disinfectant, commonly employed in surgical prophylaxis, wound management, and instrument sterilization.2,3 Minor dermal irritation represents its primary side effect. Although Savlon is a ubiquitous domestic and medical antiseptic, minor scrotal burns are likely underreported. The microbiological isolation of Pseudomonas and Klebsiella species suggests potential for severe infectious complications. Notably, this case was successfully managed through appropriate clinical intervention.
Literature review
Scrotal burns following post-circumcision dressing with cetrimide-chlorhexidine (Savlon) can occur due to chemical irritation and improper application of antiseptics. Chlorhexidine, while generally safe, can contribute to chemical burns when pooled beneath patients, particularly in sensitive areas like the scrotum, where immature skin is more susceptible to injury. 13 Cetrimide, a common antiseptic component, has been associated with irritant contact dermatitis, leading to painful rashes and potential burns, especially when used improperly or in high concentrations. 11 In cases of accidental exposure, such as ingestion of diluted antiseptic solutions, severe caustic burns have been reported, highlighting the risks associated with these agents. 14 Effective management of such injuries requires careful monitoring and appropriate dressing techniques to prevent complications. 15
Epidemiology of chemical burns
The epidemiology of chemical burns associated with cetrimide-chlorhexidine (Savlon) dressing reveals significant concerns, particularly in vulnerable populations such as children and those with compromised skin integrity. Chemical burns from antiseptics like cetrimide and chlorhexidine have been documented, with irritant contact dermatitis reported in various cases, often manifesting as painful rashes after prolonged exposure. 11 In a study of chemical burns in Shiraz, the prevalence was noted to be 1%, with a majority occurring at home, highlighting the need for awareness regarding the safe use of antiseptics. 16 Additionally, perioperative incidents involving chlorhexidine-alcohol solutions have led to burns due to pooling beneath patients, particularly affecting immature skin.13,17 These findings underscore the importance of proper application techniques and monitoring to prevent chemical injuries during medical procedures.
Management of chemical burns
Management of scrotal burns resulting from post-circumcision cetrimide-chlorhexidine (Savlon) dressing necessitates careful consideration of the irritant properties of these antiseptics. Cetrimide has been associated with irritant contact dermatitis, particularly in sensitive areas such as the genitalia, leading to symptoms like pruritus and burning after prolonged exposure. 11 In cases of chemical burns, as seen with chlorhexidine-alcohol solutions, the pooling of antiseptics can exacerbate skin damage, especially in vulnerable populations like children. 13 Effective management typically involves conservative measures such as irrigation and regular dressing changes, which have shown success in healing superficial burns. 18 Additionally, recognizing the potential for chemical injury and ensuring proper application techniques can mitigate risks associated with these antiseptics. 19 Overall, a combination of vigilant monitoring and appropriate wound care is essential for optimal recovery.
Conclusion
Circumcision performed on newborns delivered in healthcare facilities in low or middle-income countries are at an increased risk of dressing associated Savlon scrotal rashes or burns and bacteria isolation. The management of such lesions must be culture-directed. Education on dilution of cleaning agents must be well understood or practiced by caregiver before discharge.
Footnotes
Acknowledgements
We acknowledge UHAS-ECL Research centre for the use of the conference room
Ethical considerations
This report was guided by the Helsinki declaration on medical research.
Consent for publication
Verbal and written informed consent were given by the mother for educational demonstration and publication.
Author contributions
M.A.A. and M.A.O. were responsible for the conception of the study design of this work. M.A.A. and W.R.N. wrote the draft manuscript. All authors critically reviewed the manuscript, data analysis, and interpretation. All authors have read and agreed to the final version of this manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The analyzed data is wholly contained in the manuscript. The raw data is currently with the corresponding author and can be obtained on reasonable request. The study was conducted in accordance with the Declaration of Helsinki on medical research.
