Abstract
Introduction:
EpiProtect® is a biosynthetic cellulose dressing indicated for the treatment of superficial burns and the dressing of deep burns. Prior to this study the youngest reported patient treated with EpiProtect® was aged 13 years.
Method:
Data were collected prospectively for patients aged < 5 years, presenting to the Children’s Burns Unit with ⩾ 2% total body surface area (TBSA) burns sustained by any mechanism.
Results:
Thirty children were treated (median age = 17 months, age range = 1–61 months). Thirty-six burn depths were documented: superficial partial thickness (SPT) in 53% (n=19); mid-partial thickness (MPT) in 33% (n=12); deep partial thickness (DPT) in 11% (n=4); and full thickness (FT) in 3% (n=1). Median burn size was 4.5% TBSA (range = 2%–12%). EpiProtect® was applied under general anaesthesia in all cases. The median length of stay (LOS) was two days (range = 0–6 days). EpiProtect® was tolerated well and provided effective analgesia for subsequent dressing changes. Median healing time was 13 days (SPT burns), 14 days (MPT) and 24 days (DPT burns). Three patients required split skin grafting. Hypertrophic scarring arose in one patient.
Discussion:
This case series represents the youngest published patient group to have been treated with EpiProtect®. Authors conclude that EpiProtect® provides a safe, reliable and well-tolerated dressing option for all burn depths in young children. Importantly, EpiProtect® is culturally neutral and may be used in situations which, for cultural reasons, may preclude the use of animal-derived products. Further studies are warranted to evaluate pain scores, burn depth, size and LOS correlation, and comparative analysis between dressing types.
Lay Summary
Burn injuries in the paediatric population are common and often require multiple dressing changes. Dressing changes can be painful and distressing to both children and their care givers. This article describes the experience of using a synthetically derived burns dressing, called EpiProtect®, in children aged ⩽ 5 years. Thirty patients were recruited with varying depths of scald burns and all underwent application of EpiProtect® dressing. The results suggested that EpiProtect® was a user-friendly dressing that can be used to treat partial-thickness burns and to dress full-thickness (FT) burns. It was well-tolerated and provided effective analgesia at the time of dressing changes. There was no incidence of increased burn wound infection rates and all wounds healed. In addition, as EpiProtect® is a synthetic product, it has the benefit of being culturally neutral, which is advantageous in a culturally diverse population. Further studies are warranted to evaluate the effectiveness of this dressing and to compare it to similar dressings that are available.
Keywords
Introduction
Approximately 25,000 children attend emergency departments in England and Wales per year due to burns, with 3800 requiring admission to hospital. 1 Children account for almost half of all burn injuries 2 and 72% of children’s burns occur in children aged < 5 years. Scalding is the most common burn injury mechanism (58%, n=709/1215). 1
Burns dressings may be simple or specialised. Specialised dressings include Biobrane® (Smith & Nephew, Watford, UK) and Suprathel® (PolyMedics Innovations GmbH, Denkendorf, Germany). The main benefit of these dressings is their adherence to the wound bed, providing temporary closure of the wound.3–5 This minimises the need for further interference with the wound bed, greatly reducing pain at dressing changes.3–7 In addition, specialised dressings may allow drainage of excess exudate and prevent wound desiccation. 8 However, existing specialised burns dressings may have several disadvantages. Biobrane® is pork-derived which, for cultural or religious reasons, may preclude its use in some patients or their families. 9 In addition, it is indicated only for superficial partial thickness (SPT) wounds and has been associated with episodes of infection and toxic shock syndrome. 8 Suprathel® is a reliable synthetic epidermal substitute which can be used for the treatment of partial thickness, mid-partial thickness (MPT) and deep partial thickness (DPT) dermal burns,3,10 but is expensive. 5
The aim of the present study was to evaluate the authors’ experience of the use of EpiProtect® microbial cellulose dressings in the treatment of burn injuries in a series of patients aged < 5 years.
Methods
Data were collected prospectively for patients aged < 5 years presenting to the Children’s Burns Unit with ⩾ 2% total body surface area (TBSA) burns sustained by any mechanism. Information regarding EpiProtect® and its management was given to parents, and informed written consent was obtained.
Burn depth was assessed and recorded both on hospital admission and again at the time of burn debridement. EpiProtect® was applied within 48 h of injury. Under general anaesthesia, wound swabs were taken and patients underwent superficial burn debridement. This involved scrubbing using gauze in the case of clearly SPT injuries, < 24 h old. In burn wounds > 24 h old, or if areas were non-blanching to digital pressure, debridement was carried out using Versajet® hydrosurgery (Smith & Nephew, Watford, UK) on setting 1.
After superficial debridement, EpiProtect® was applied to the wound (Figures 1–3). Initially, EpiProtect® was fixed in place using tissue glue (n = 7). However, due to skin irritation in glued areas, no fixation was used in subsequent applications (n = 23). Secondary dressings were applied over the EpiProtect® and consisted of a non-adherent, knitted viscose rayon sheet with a silicone coating (NA Ultra®, KCI Medical Limited, Gatwick, UK), gauze and tape. In most cases patients were discharged on the same day. Patients with higher percentage TBSA burns, facial burns or concerns regarding their social circumstances had a longer length of hospital stay.

EpiProtect® biosynthetic cellulose dressing.
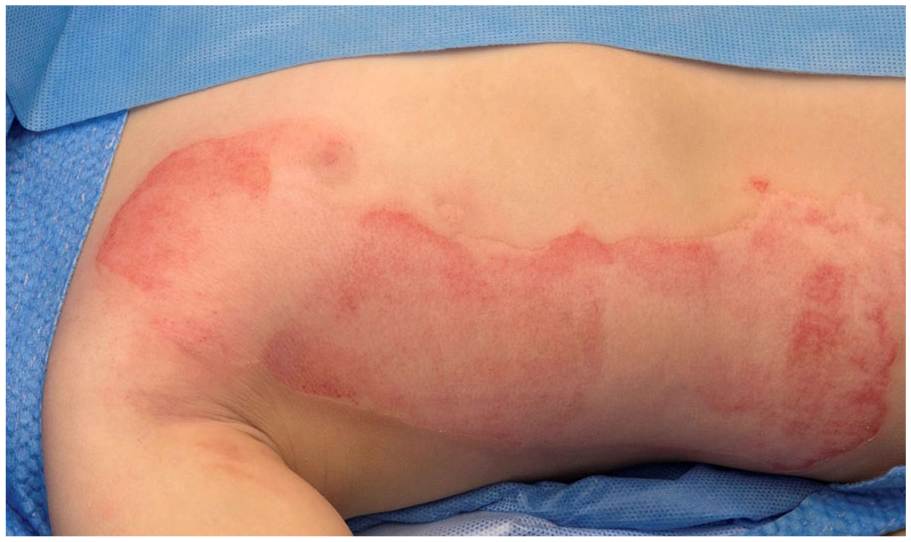
EpiProtect® applied to burn without additional fixation.

Mixed superficial partial thickness and mid-partial thickness burn immediately after superficial debridement in operating theatre.
A wound check was performed in clinic 24–48 h after application (Figure 4). The EpiProtect® remained in situ until spontaneous re-epithelialisation and loss of adherence occurred, allowing trimming of non-adherent EpiProtect® without disturbing unhealed areas. Patients were monitored through the burns dressing clinic until wounds had fully healed, unless their care was repatriated to other units. Simple analgesia (paracetamol and ibuprofen) was used for all dressing changes. Patients were reviewed in a consultant-led follow-up clinic 3–4 months after injury (Figure 5).
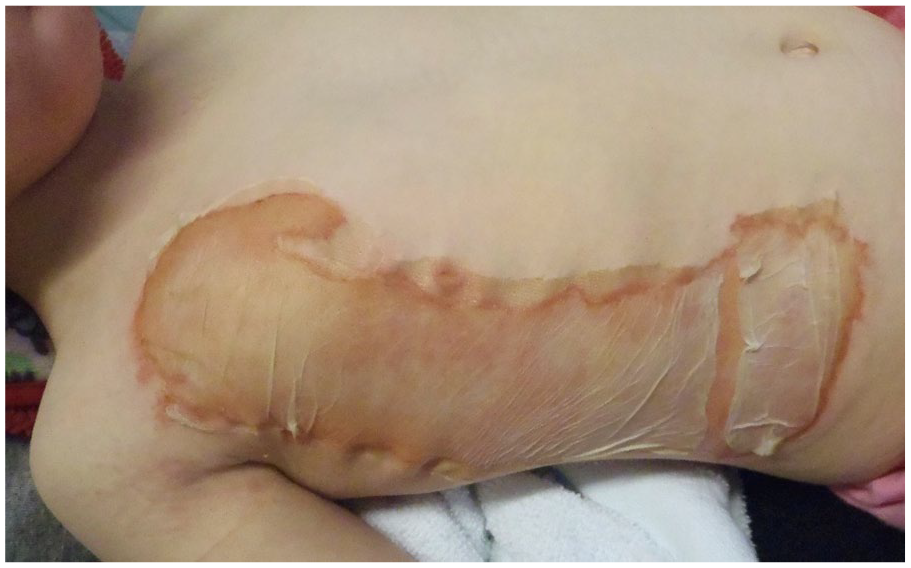
EpiProtect® in situ at 48-h dressing change.

Healed burn, three months after injury.
Cases were evaluated for: demographics; burn characteristics; ease of EpiProtect® application; intraoperative complications; pain; post-application complications; patient and family satisfaction; and healing time. In cases of mixed-depth burns, in which some parts were SPT and others were MPT, DPT or FT, then those areas of SPT, MPT, DPT and FT injury were evaluated separately in the data field.
Results
Between July 2018 and June 2019, EpiProtect® was applied to 30 paediatric patients, aged ⩽ 5 years. Sixteen patients were boys and 14 were girls. Demographic characteristics for this patient group are shown in Table 1. The median patient age was 17 months (age range = 1–61 months). All burn injuries were sustained from scalds, with a median burn size of 4.5% TBSA (range = 2%–12%). Six patients (20%) had mixed-depth burns. These areas of differing burn depth were evaluated separately. This resulted in 36 depths of burns being documented. Most burn injuries (53%, n=19) were SPT in burn depth; 33% (n=12) were MPT; 11% (n=4) were DPT; and there was 1 (3%) FT burn.
Basic characteristics of patients and burns treated with EpiProtect®.

A, Asian; AC, Afro-Caribbean; C, Caucasian; FT, full thickness; DPT, deep partial thickness; MPT, mid-partial thickness; SPT, superficial partial thickness; TBSA, total body surface area.
All burns other than burns to the head and neck region were treated with EpiProtect®. All patients underwent surgery within 48 h of injury. The median inpatient stay was two days (range = 0–6 days), with over one-third of cases staying < 24 h and over two-thirds of patients staying < 48 h. The largest burn treated as a day case was 4.5% TBSA. In two cases, 8% TBSA burns were treated with a single overnight stay, which was due to surgery being carried out late in the day.
Healing times were unknown for four patients as follow-up took place with distant care providers. For patients on whom data were available (n = 26), median healing times were: 13 days for SPT burns (range = 8–21 days); 14 days for MPT burns (range = 9–26 days); and 24 days for DPT burns (range = 21–26 days). Of the six patients with mixed-depth burns, three patients underwent a second operation for split thickness skin grafting. The median healing time for these patients was 28 days (range = 21–48 days). The median number of visits to the Paediatric Dressings Clinic for dressing changes was four visits (range = 2–4 visits).
Dressing changes were uniformly well-tolerated and were completed rapidly. Although formal pain scores were not recorded, all patients required simple analgesia only. At dressing changes it was noted that the translucent nature of EpiProtect® allowed clinical wound monitoring through the cellulose sheet.
Complications were seen in three patients. Rolling of the edge of the EpiProtect® dressing occurred in one patient. Two patients presented to the Emergency Department 48 h after dressing application with symptoms suggestive of sepsis. Both patients were returned to theatre for removal of EpiProtect®, cleansing and inspection of the burn wound, to rule out toxic shock syndrome. Both patients were found to have other causes for malaise: hand-foot-and-mouth disease in one case and viral pharyngitis in the other. Following these complications, if a child became unwell after application of EpiProtect®, a clinic- or a ward-based dressing change was performed, obviating the need for additional anaesthesia.
Twenty-two patients (73%) returned for a consultant-delivered review in clinic at three months after EpiProtect® application. Four patients had their follow-up care in other units; another four patients had not had their three-month follow-up appointment at the time of submission. Of the 22 who returned, one patient had a mildly hypertrophic scar. This patient had 8% MPT and DPT burns, most of which healed conservatively with EpiProtect®, but 1%TBSA required split thickness skin grafting. This patient is currently receiving topical scar therapy as an outpatient.
Discussion
To the authors’ knowledge, the use of EpiProtect® in patients aged < 13 years has not been documented. This report represents the youngest patient group and the largest paediatric case series involving EpiProtect®.
The authors found EpiProtect® to be safe, versatile and highly effective in young children and had minimal associated complications. Of particular benefit, no increased pain associated with dressing change was observed and there was minimal distress from patients and parents. In addition, senior nursing staff noted the benefit of a flexible, adherent layer dressing in reducing the time required for each dressing change. No additional visits for dressing changes were required and after application of EpiProtect® in theatre, subsequent dressing changes were straightforward, requiring only simple analgesia.
During the first 12 months of use, this procedure was typically carried out as a day case, or involved an overnight stay in hospital if performed in the evening or at night. In this series, the number of cases was too small to allow valid correlation between burn size and depth and length of inpatient stay.
The authors believe that their rate of skin grafting for paediatric scald injuries has decreased since commencing the use of EpiProtect® (3/30 patients). Some wounds diagnosed as deep dermal spontaneously healed under EpiProtect® dressings.
The authors had previously experienced refusal by some parents to the use of porcine-derived wound dressings on their child. EpiProtect® is made from cellulose, is completely free from animal and human tissue, and is therefore culturally neutral. No patients or families refused the use of EpiProtect® for cultural or religious reasons.
With respect to financial costs, at the time of writing, EpiProtect’s® UK price was 36 pence/cm2 for a single sheet of 17 × 21 cm. By comparison, Biobrane’s® price was 24 pence/cm2 for five sheets of 13 × 13 cm and Suprathel’s® price was 46 pence/cm2 for five sheets of 18 × 10 cm, before delivery charges.
The authors recognise that this is a relatively small case series, based in a single centre. More robust studies are warranted to evaluate pain scores, correlation between burn depths and size and LOS, and provide comparative outcome analysis between types of dressing and duration of dressing changes.
Conclusion
EpiProtect® is a user-friendly and well-tolerated synthetic skin substitute for the treatment of partial thickness burns, and for use as a temporary dressing for FT burns before debridement. The use of EpiProtect® was not refused by patients or their families on religious or cultural grounds.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
