Abstract
Background
Myelomeningocele is a severe and complex congenital malformation of the central nervous system. Failure of neural tube closure at around four weeks of gestation results in an open communication between the neural placode and the external environment with varied functional impairment. Surgery is usually required.
Objectives
The primary goals of surgical management are to preserve neural function and minimise infection. Reconstruction is dependent upon the site and size of the defect as well as the quality of the surrounding soft tissues. Surgeons may employ a range of reconstructive techniques in order to achieve closure. Skin substitutes, also known as dermal regeneration templates, have also been utilised.
Discussion
In our unit, we use NovoSorb Biodegradable Temporising Matrix to reconstruct full-thickness skin and soft tissue defects. It is a synthetic, biodegradable, dermal regeneration template, composed of polyurethane foam bonded to a transparent sealing membrane and typically requires a two stage reconstruction. Integration and vascularisation take approximately three weeks. After this time, the recipient wound bed is suitable for split thickness skin grafting. A further benefit of dermal regeneration templates is the possibility of ‘stacking’ layers, which serves to increase the thickness of the final construct and to minimise overall contour defects. The authors present the case of a one-day-old full-term neonate with a large lumbosacral myelomeningocele that was successfully managed with staged, stacked NovoSorb Biodegradable Temporising Matrix and split thickness skin grafting. The authors believe this is the first case in which a ‘stacked’ dermal regeneration templates has been used to achieve healing of a primary myelomeningocele defect.
Lay Summary
Keywords
Background
Myelomeningocele is a severe and complex congenital malformation of the central nervous system and forms the group of anomalies commonly referred to as neural tube defects (NTDs). Part of the spina bifida spectrum, it occurs due to failure of neural tube closure at around four weeks of gestation and results in an open communication between the neural placode and the external environment. 1 The degree of functional impairment varies and this is dependent on the vertebral level affected as well as the extent of the lesion but usually results in: lower limb paralysis; sensory loss; bladder dysfunction; bowel dysfunction; and cognitive dysfunction. 2 The prevalence of NTDs varies globally. Different rates have been documented based on ethnic and geographical characteristics, as well as being influenced by the availability of prenatal detection. An average of 1 in 1000 live births are affected worldwide. 3 The aetiology and pathogenesis of spina bifida is multi-factorial with genetics, nutrition and environmental factors all playing a role. 4
The main objectives of surgical management are to preserve neural function and to minimise risk of infection. Reconstruction is varied and is dependent upon the site and size of the defect as well as the quality of the surrounding soft tissues. 5 Robust dural coverage of neural elements within the spinal canal and stable soft tissue coverage is integral in preventing cerebrospinal fluid (CSF) leakage and wound dehiscence and should be undertaken as early as possible following birth. 6 Numerous methods of reconstruction have been described ranging from direct closure (with or without skin undermining and relaxing incisions); skin grafting; local fasciocutaneous flaps (random or perforator-based); myofascial turnover flaps (with or without paraspinous muscle flaps) as well as regional muscle-based flaps, e.g., Latissimus dorsi, Gluteus maximus.5–16
Skin substitutes, also known as dermal regeneration templates (DRT), have been employed in combination with flaps both in utero and postnatally with good effect.8,17,18 The authors have used NovoSorb Biodegradable Temporising Matrix (BTM; PolyNovo Ltd, Port Melbourne, Victoria, Australia) to reconstruct complex wounds. This has been utilised in full-thickness skin and soft tissue defects resulting from burn injury, trauma, infection or surgery.19–23 It is a 2-millimetre thick, synthetic, biodegradable DRT and is composed of polyurethane foam bonded to a transparent (non-biodegradable) sealing membrane and typically requires a two-stage reconstruction. Integration and vascularisation lead to the formation of a ‘neo-dermis’ and this is usually apparent from approximately three weeks. At this time, the sealing membrane starts to delaminate by separating from the underlying integrated foam to reveal a vascularised wound bed. This is demonstrated by a colour change from white to a pinkish red with blanching observed on palpation. A second stage procedure can then be performed, with removal of the outer sealing membrane and split thickness skin grafting of the ‘neo-dermis’ layer.
Empirical evidence suggests that NovoSorb BTM may confer relative resistance to infection and to skin contracture and improve post-operative skin pliability.19,24,25 A further benefit of DRTs is the possibility of ‘stacking’, with an additional layer added, once vascularisation of the outermost DRT layer is complete. This serves to increase the thickness of the final construct and to minimise overall contour defects.
The authors present the case of a one-day-old full-term neonate with a large lumbosacral myelomeningocele that was successfully managed with staged, stacked NovoSorb BTM and split thickness skin grafting to achieve a robust and durable reconstruction. The authors believe this is the first case in which a ‘stacked’ DRT has been used to achieve healing of a primary meningomyelocele defect. In addition, this case describes the youngest patient to be reconstructed using multiple layers of a DRT.
Case study
A male newborn was delivered under the combined care of obstetricians and neurosurgeons, following elective Caesarean section, at 38 weeks gestation. Antenatal diagnosis of spina bifida had been made on anomaly ultrasound scan performed at 21 weeks (Figure 1(a)) and confirmed by fetal MRI scan (Figure 1(b)). This showed a large mid-thoracic myelomeningocele as well as kyphoscoliosis, ventriculomegaly and Chiari malformation (Type II). Following delivery and combined clinical assessment, a surgical plan for repair and reconstruction was made by plastic surgeons and neurosurgeons.

(a) Ultrasound scan performed at 21 weeks gestation. Defect demonstrated by marker. (b) Fetal MRI scan confirming myelomeningocele defect.
At day one post-partum, dural repair of the myelomeningocele was performed. The defect was measured at 8 × 7 cm (Figure 2). The neural placode was circumferentially dissected and any non-functioning neural filaments were removed. The placode was subsequently inverted and closed using 4/0 polypropylene sutures to reconstruct a neural tube (Figure 3). With no apparent dural plane evident, the adjacent paraspinous muscular fascia was incised laterally, elevated and brought medially to envelop the neural tube and closed with further 4/0 polypropylene sutures. Due to tethering of the surrounding skin and the size of the defect, safe reconstruction using local soft tissue options was not deemed possible. As a result, a DRT (NovoSorb BTM) was selected. A single sheet (10 × 10 cm) of NovoSorb BTM was cut to the size and shape of the defect, ARTISS (Baxter Healthcare, Newbury, UK) fibrin sealant spray was applied to the wound bed prior to application to aid adherence and the DRT was affixed using 4/0 polypropylene sutures (Figure 4). A non-adherent silicone interface dressing (NA Ultra, Systagenix, Gargrave, UK) was applied over the NovoSorb BTM and the whole wound was sealed within a negative pressure wound therapy (NPWT) dressing (V.A.C., 3M, St Paul, Minnesota, USA). This was set at a continuous pressure of −25mmHg to provide splintage of the DRT and to minimise any loss of CSF. The NWPT attachment to its non-collapsible tubing was sited on the anterior abdomen, in order to avoid compression effect upon the skin of the back.

Primary lumbosacral myelomeningocele at 1-day post-partum. Defect measured 8 × 7 cm.

Tubularised dural repair.

First DRT layer at primary procedure, prior to application of NWPT dressing.
Over the next 12 days the patient returned to theatre twice for change of NPWT dressing and inspection of the NovoSorb BTM. By day 19, the outer sealing membrane of the NovoSorb BTM had delaminated and the underlying foam was completely vascularised (Figures 5 and 6). A further sheet of NovoSorb BTM was applied at this point and the above process was repeated (Figure 7). On day 23, an ultrasound-guided right parietal ventriculoperitoneal shunt (VPS) was placed, to relieve hydrocephalus. A further change of NWPT dressing was performed on day 26 and split skin grafting of the second DRT layer was carried out on day 40 (Figures 8 and 9). A hand-fenestrated 8/1000-inch-thick skin graft was harvested from the outer aspect of the right thigh and affixed with absorbable 4/0 sutures (Vicryl Rapide, Ethicon, Cincinnati, USA) (Figure 10). NWPT was used again to protect and splint the graft. A graft review seven days later demonstrated full take. No wound complications were encountered thereafter.
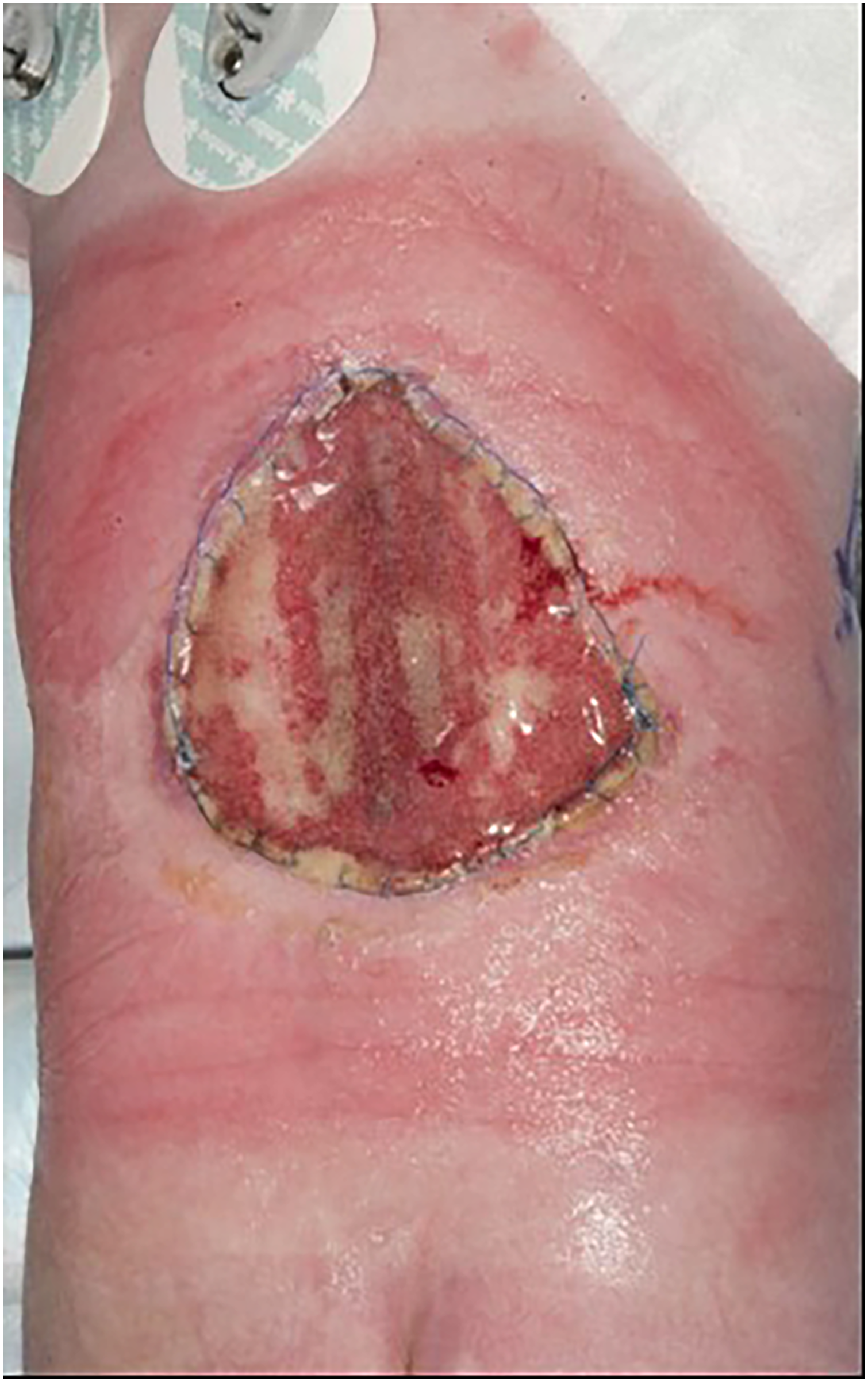
Three weeks post-partum. DRT is integrated, with complete vascularisation (red colour) and delamination of bonded polyurethane top layer (pale areas).

Removal of polyurethane top layer, revealing vascularised ‘neo-dermis’.

Second ‘stacked’ DRT layer, prior to application of NPWT dressing.
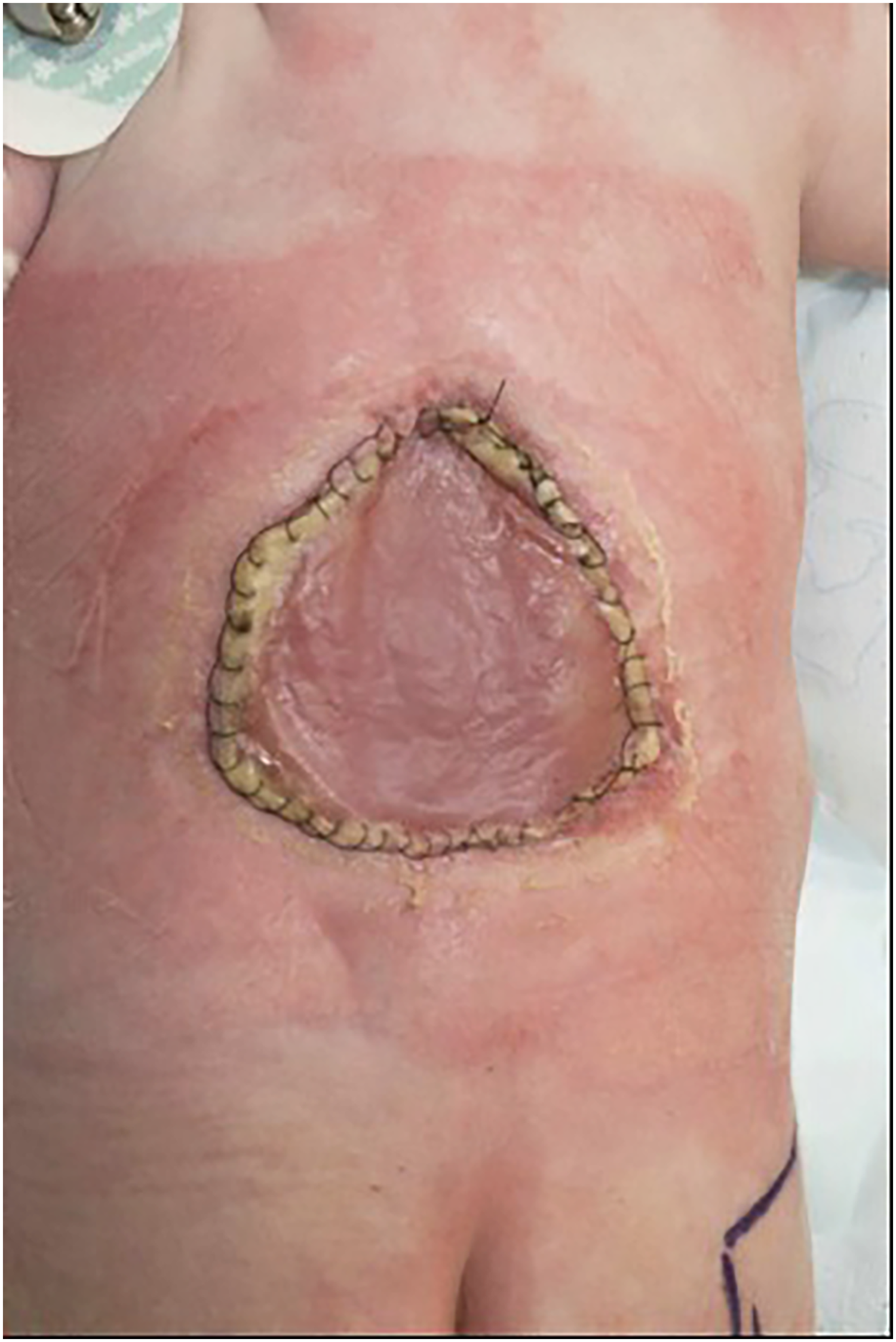
Full integration and vascularisation of second DRT layer.

Second layer of DRT demonstrating a vascularised wound bed with punctate bleeding.

Third reconstructive procedure: split thickness skin graft secured over second DRT layer.
A review at one year post-operatively, demonstrated the patient to be in good health with no skin or soft tissue problems experienced at the reconstruction or skin graft donor site. The skin over the reconstruction was soft, pliable and maintained a good contour with the surrounding tissues (Figure 11). The scar around the periphery of the reconstructed area was slightly hypertrophic and was treated with a scar therapy program and continues to be under regular review. At the time of writing, no further reconstruction was required.

Appearance 1-year post-partum. Stable, robust soft tissue coverage. Peripheral scar is slightly hypertrophic.
Discussion
The rationale for early surgical intervention for myelomeningocele is to preserve neural function and reduce the risk of infection. If at all possible, this should be performed within the first few days of life. Early closure has been shown to be a significant determinant in enhancing neurosurgical outcome. 26 The principles of reconstruction are dependent upon the size and site of the defect as well as the state of the surrounding tissues. It is important to minimise tension across the line of closure and to provide stable soft tissue coverage of the dural repair and prevent CSF leak. Numerous techniques for myelomeningocele closure have been described. Collectively, these illustrate the spectrum of soft tissue reconstruction, the variety of surgical experience and degree of local resource availability, which fall outside the remit of this article.
Most lumbosacral myelomeningocele defects can be closed directly.6,9 Larger defects will pose reconstructive challenges. Local fasciocutaneous flaps are still advocated and have a role in the moderate to large myelomeningocele defects.5,9–12 However, owing to the potential need for extensive skin undermining to achieve primary closure, concerns still remain with regards to progressive skin necrosis and flap failure following surgery. Large musculocutaneous flaps may provide durable soft tissue coverage by reinforcing the dural repair, reduce dead space and provide a robust barrier between the spinal cord and skin. However, donor site morbidity can be high.14,16 Harvesting of muscle flaps comprising Latissimus dorsi or Gluteus maximus, in an already neurologically compromised child, has the potential to limit future functionality and worsen postural development. 13 In addition, operative scars on the posterior trunk may complicate planning for any subsequent reconstruction.
A number of factors influenced the decision to select NovoSorb BTM as the primary reconstruction in the case presented. Firstly, a procedure involving DRT placement is relatively low risk, with minimal morbidity (e.g., blood loss) and preserves the full complement of flap based reconstructive options for a later stage if required. This in effect ‘buys time and tissue’, allows for growth and expansion of the soft tissues, which could then permit future instrumentation and reconstruction. The skin over the DRT repair was of good quality and pliability one year following surgery, with the area being treated as ‘normal skin’ with no additional safety precautions required. Secondly, NovoSorb BTM conferred a robust seal over the dural repair. This was evident with no demonstrable CSF leak or any sub-DRT fluid collection during the hospital admission. Thirdly, the ability to add layers (‘stack’) of NovoSorb BTM in stages, once integration and vascularisation of the previous layer is complete, allows reconstruction of deeper contour defects with a further 2 millimetres being added with each layer. The authors acknowledge that in order to reach completion, reconstruction requires several procedures under general anaesthetic, which in turn may not be feasible or practicable for all centres providing reconstruction of myelomeningocele defects.
The use of a NWPT dressing in this case was discussed prior to surgery with the neurosurgical team. Negative pressure would have potential to worsen the effects on any CSF leak. However, at operation, the dural repair along with its fascial envelope was confirmed to be complete and sufficiently ‘water-tight’ to allow the placement of a NWPT device. In addition, the DRT provides an interposed layer, protecting the dura from any direct effects of negative pressure. The benefits of a NWPT dressing for DRT care include: splinting; drainage; wound hygiene; and vascularisation. 27
The development of fetal spina bifida surgery, presents the possibility of improved neurological outcomes compared to postnatal surgery, when performed before 26 weeks gestation. 28 Currently in the United Kingdom, this technique is subject to specific inclusion criteria and is limited to a small number of specialist institutions. In most centres, postnatal repair of myelomeningocele remains the only option.
The authors describe successful use of the NovoSorb BTM as a DRT to achieve closure of a large lumbosacral myelomeningocele without complication and with longstanding stability. We believe this technique provides reconstructive teams with an alternative option that is effective, safe, reproducible and which spares local tissues for future elective reconstructive procedures, should they be required.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: PolyNovo Limited have funded part of the publication fee.
