Abstract
Introduction
Venous leg ulcers are the most common cause of leg ulcers. The aim of this study is to assess the effect of Combined Ultrasound and Electric Field Stimulation therapies (CUSEFS) on wound surface area and pain level in patients with venous leg ulcers, utilizing a novel device (BRH-A2 from BRH Medical, Ltd).
Methods
This prospective case series study, conducted by the Department of Plastic Surgery at the Yitzhak Shamir Medical Center, Israel, collected data for subjects treated with CUSEFS with the BRH-A2 device, between April 2018 and September 2019. Measurements of wound area and assessment of pain intensity using a 10-point visual analog score were recorded. At the end of the four-week period, average wound area and pain scores were included for analysis.
Results
Ten consecutive patients met the inclusion criteria. During the study period, all patients exhibited a reduction in the wound surface area. The final average wound surface area was reduced by 53.52% following the combined treatment. Eight out of the ten patients (80%) reported a reduction in pain, with an average pain level reduction of 64% throughout eight consecutive treatments.
Conclusion
CUSEFS therapies with BRH-A2 technology is a promising treatment for venous leg ulcers. In accordance with our preliminary results, this treatment modality can aid in the reduction of wound surface area as well as reducing the pain suffered by patients from these chronic wounds. Larger multicenter studies are needed to further quantify and qualify the beneficial effect of CUSEFS in venous leg ulcers and other chronic wounds.
Lay Summary
Venous leg ulcers (VLUs) are painful wounds occurring between the knee and ankle joint, that fail to heal for a period of at least two weeks and occur in the presence of venous disease. VLUs, are the most common cause of leg ulcers, affecting approximately 5% of the general population over the age of 65. Numerous non-invasive treatment modalities have been attempted for healing chronic wounds and ulceration, however, in some instances surgery, although invasive, is the preferred option. For many years, ultrasound (US) has been used therapeutically to treat chronic ulcers. US produces biophysical effects that are significantly beneficial to the wound healing process. Electrical stimulation therapy is another treatment option which contributes to wound healing by influencing the electrochemical wound process.
Combined Modulated Ultrasound and Electric Field Stimulation (CUSEFS) have been shown to improve the healing of chronic wounds. However, research has focused predominantly on objective measures of healing, while less consideration has been given to researching the subjective discomfort and the negative impact that ulceration places on the patient. The aim of this study was to assess objective and subjective factors by measuring the short-term effect of CUSEFS on the surface area of wound and on pain levels in patients with venous leg ulcers (VLUs). Our study findings demonstrate that the combined treatment was effective in initiating wound healing and reducing levels of pain in chronic, stagnant, recalcitrant venous leg ulcers.
Keywords
Introduction
A venous leg ulcer (VLU) is defined as the loss of skin between the knee and ankle joint that remains unhealed for at least two weeks and occurs in the presence of venous disease. 1 In the United States, chronic wounds affect roughly 6.5 million patients and a total of 25 billion USD is spent annually on treatments. 2 VLUs account for 60–80% of all leg ulcers, and are therefore the most common cause. 3 These ulcers are often chronic in nature and 33–60% of them persist for more than six weeks, 4 furthermore the three month recurrence rate is as high as 70% following wound closure.5,6
Numerous non-invasive treatment modalities have been studied and utilized for healing chronic wounds and ulceration. 7 For many years, ultrasound (US) has been used therapeutically to treat chronic ulcers, given its biophysical effects that significantly impact wound healing. 8 These wound healing effects include changes in cellular protein synthesis, reduction of edema, increased blood flow into the wound bed, angiogenesis, leukocyte adhesion to endothelial cells and stimulation of fibroblast proliferation. 9 Electrical stimulation therapy, another treatment modality for ulcers, contributes to wound healing by affecting the electrochemical wound process. Intact skin has a transepithelial potential difference of 10–60 mV, with the skin surface having a negative charge from chloride ions and the dermis maintaining a positive charge via sodium ions. 10 Ulceration leads to an imbalance in the electrical currents, thus disrupting the wound healing processes. Electrical stimulation therapy is able to realign the currents and thereby assists with the healing process. 9
In a few studies,11,12 Combined Modulated Ultrasound and Electric Field Stimulation (CUSEFS) have been shown to improve healing of chronic wounds. Research indicates that wound management has been mostly focused on ‘objective’ parts of the healing process and subsequently the patient's subjective discomfort and the impact that ulceration poses on the patient, has received comparatively less consideration. 13
To the best of our knowledge, CUSEFS has not previously been studied as a treatment modality for VLU-related pain. This is the first study using Combined Ultrasound and Electric Field Stimulation therapies with BRH-A2 device (from BRH Medical, Ltd) to assess the short-term effect on reduction of pain and wound surface area in patients with VLUs.
Materials and methods
This prospective study was conducted in the Department of Plastic Surgery at the Yitzhak Shamir Medical Center, Israel. Approval was received from Ethics Committee/Institutional Review Board. Informed consent agreement for inclusion in this study, including information regarding BRH-A2 device and its management, publication of this paper, and the accompanying images, was obtained from all patients. Between April 2018 to September 2019, data was collected for subjects treated with the wound management system (combined ultrasound and electric field stimulation (CUSEFS), BRH A2 device (from BRH Medical, Ltd).
Inclusion criteria
The study population included patients between the ages of 18 to 90 years. Criteria for inclusion included: (1) Wounds that had been present for at least one month and involved only the skin or deep dermal tissues; (2) Stable wounds that had not improved (as measured by a 30% reduction in surface area) in the 30 days prior to treatment. The etiology of the wounds was determined based on compromise in venous blood flow, as documented by Doppler ultrasound and the exclusion of other etiologies mentioned below.
Exclusion criteria
Exclusion criteria included patients with a history of recent trauma to the affected area or any suspected foreign body in the wound bed and patients with a permanent implant in the treated area (such as metal plates). Patients were also excluded if they had abnormal liver or renal function, high HbA1c levels, morbid obesity, history of immunosuppression / deficiency disorders, history of coagulopathy/thromboembolic condition and patients with abnormal arterial flow, measured by Doppler ultrasound. Patients that received other treatment that may have affected wound healing within 30 days prior to CUSEFS treatment, were also excluded from the study. These treatments included macrophage or partial blood injections, skin grafts or application of dermal equivalents. Furthermore, we excluded oncology patients who had undergone any form of treatment for active cancer, month prior to initiation of CUSEFS treatment, as well as patients with a history of skin cancer (including malignant or pre-malignant pigmented lesions) or any other cancer, in the area needing treatment. Any patients who were excluded from the study were provided with the appropriate standard of care management and treatment of their wounds.
BRH-A2 technology
The BRH-A2 wound management system is a US Food and Drug Administration approved non-invasive portable device, developed by BRH medical Ltd, Jerusalem, Israel. The device utilizes the combination of modulated ultrasound energy and electric field stimulation therapy to heal chronic wounds, such as diabetic foot ulcers (DFUs), venous leg ulcers (VLUs), ischemic ulcers and pressure ulcers. The technology adjusts its ultrasound and electrotherapy waves’ frequency and intensity in real time, as needed, in order to generate corresponding tissue resonance. The resonance achieves improved microcirculation in, and around, the wound bed.
Treatment protocol
All dressings, ointments and creams were removed, and the wound was cleansed using sterile, normal saline. After appropriate debridement, the wound was clinically measured by the digital BRH-A2 CUSEFS system and then photographed. Wound measurements were recorded for the initial visit, as well as at visit 8, which was scheduled four weeks from the beginning of the study. CUSEFS was applied for 15 minutes at every visit (overall eight treatments). The wound was then covered by a saline gauze dressing and a secondary dressing. The dressing was held in place with a gauze net, and a compression bandage that was applied from the metatarsophalangeal joints to the tibial tuberosity. The regular local treatment that the patient received prior to enrollment in the study, was continued throughout the study period, and CUSEFS treatment administered twice weekly, was added onto the regular treatment regimen.
Pain level assessment was carried out and recorded before the study and after each CUSEFS treatment.
Assessment tools
Pain intensity was assessed using a 10-point visual analog score (VAS). The VAS scale ranges from 0 to 10, with 0 indicating the absence of pain and 10 indicating unbearable pain. Participants were asked to rate their pain intensity before the study and after each CUSEFS treatment. At the end of the four-week period, the wound area and pain scores documented over the course of the study were recorded and an average was calculated for the purpose of analysis.
Results
Between April 2018 to September 2019 CUSEFS therapy was applied to ten consecutive patients.
Nine patients suffered from VLUs and one patient from DFU. The average age of the patients was 66.9 years (range: 40–83 years). The initial wound surface area was an average of 13.14 cm2 (range: 0.67–36.12 cm2). In one patient, an initial surface area of the wound was not measurable. Initial wound age was an average 18.02 months (range: 1.25–49 months) (Table 1, Figures 1–6).

Wound of patient 3 (69 yr-old men) before treatment with CUSEFS; Wound size 1.71 cm2; Pain level 5.

Wound of patient 3 following four weeks of treatment with CUSEFS; Wound size 0.96 cm2; Pain level 2.

Wound of patient 10 (65 yr-old men) before treatment with CUSEFS; Wound size 36.12 cm2; Pain level 3.
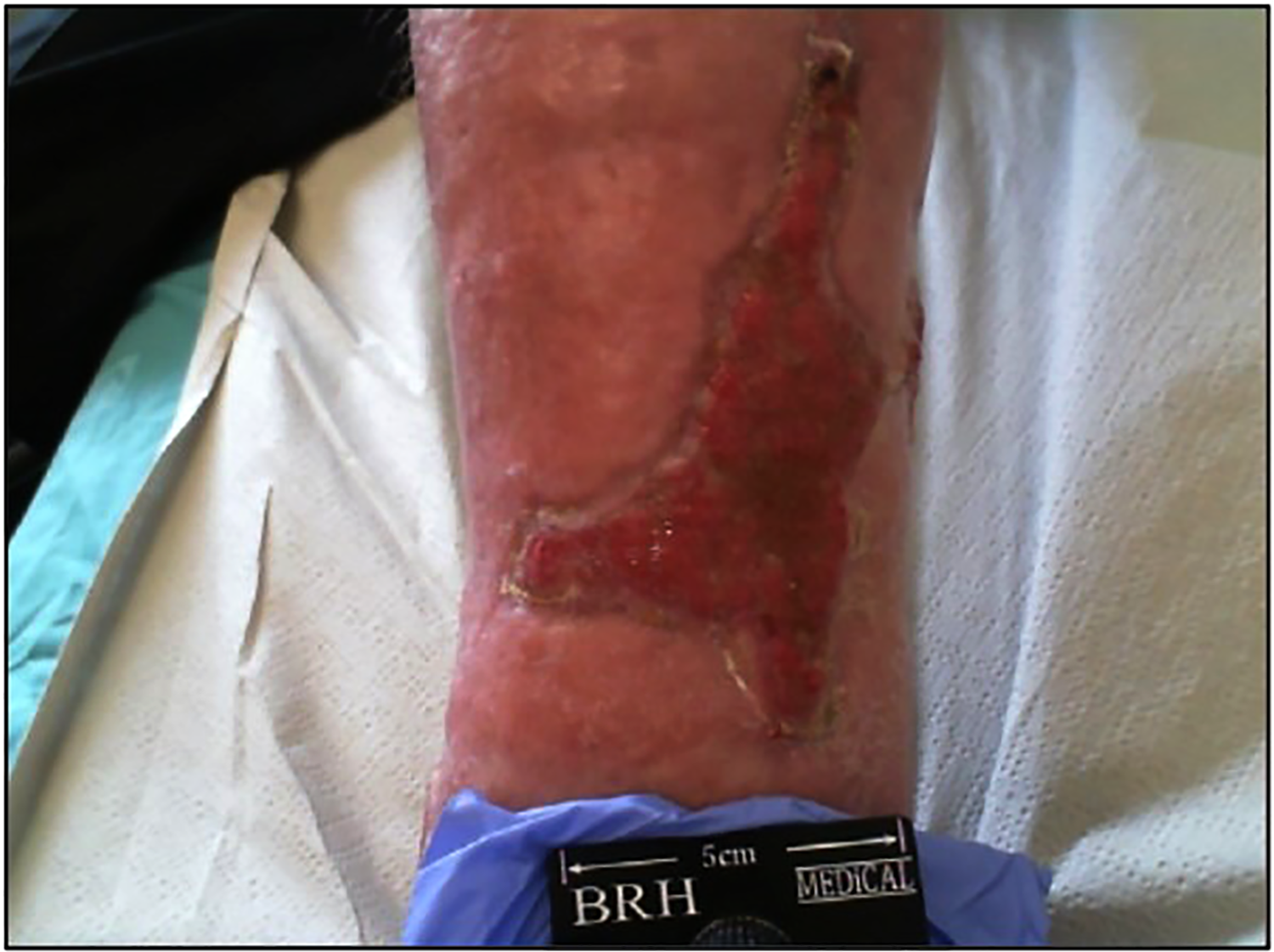
Wound of patient 10 following four weeks of treatment with CUSEFS; Wound size 19.93 cm2; Pain level 0.

Wound of patient 2 (69 yr-old men) before treatment with CUSEFS; Wound size 11.93 cm2; Pain level 2.

Wound of patient 2 following four weeks of treatment with CUSEFS; Wound size 0 cm2; Pain level 0.
Patient's characteristics and wound surface area.

Table 2 summarizes the average improvement of pain and wound surface area throughout the study period. All patients exhibited a reduction in the wound surface area. 40% of wounds showed a ≥ 50% reduction of wound surface area, and 30% of wounds were completely healed. The final average wound surface area was 6.17 cm2, accounting for a wound surface area reduction of 53.52% (Table 2).
Attenuation in wound surface area and pain level reduction during the study period.

With regard to pain assessment, at initial evaluation all patients except one (VAS = 0) complained of pain related to their chronic wounds. Eight out of the ten patients reported reduction in pain. The average pain level reduction following eight CUSEF treatments was 64%. After four weeks of treatment, 40% (four) of the patients were pain free, and 89% of patients with pain experienced ≥50% reduction in the level of pain. The average pain score before and after treatment was 2.5 and 0.9, respectively (Figure 7 and 8).

Change in pain intensity (using a 10-point VAS) and change in wound area (%) after each treatment with CUSEFS in patient 3. After 8 treatments with CUSEFS, the percentage difference in wound size was 43.86% smaller; After 4 treatments with CUSEFS, the patient's pain level decreased to VAS 1 and ended at VAS 2 after the last treatment with CUSEFS.

Change in pain intensity (using a 10-point VAS) and change in wound area (%) after each treatment with CUSEFS in patient 10. After 8 treatments with CUSEFS, the percentage difference in wound size was 47.59% smaller; After only a single treatment with CUSEFS, the patient's pain level decreased from VAS 3. to VAS 0 and remained at 0 for the remainder of the study.
Discussion
Our study demonstrated the benefit of non-invasive combined ultrasound and electric field therapy in patients with non-healing venous leg ulcers. At the end of the trial period, CUSEFS treatment was shown to effectively initiate wound healing, measured by the reduction in wound surface area and also reduce the level of pain, measured on the VAS scale, in chronic, stagnant, recalcitrant venous leg ulcers.
The average age in patients with VLUs in our study was 66.9 years, which is consistent with the accepted literature indicating that venous leg ulcers tend to be more common in older patients. The prevalence of VLUs among the general population is between 0.18% and 1% 14 and over the age of 65, the prevalence increases to 4%. 15
It should be noted that due to the consecutive nature of the study design, there is variation in the patients who entered the study relating to their characteristics, such as the size of the wound and the duration of its presence. For the same reason, we also included one patient with DFU in the overall analysis, although the rest of the patients suffered from VLU. The inclusion of a diabetic ulcer in this case diverges from the focus of the study which is venous ulcers, considering this type of wound has a different aetiology altogether including the presence of peripheral neuropathy (potentially affecting pain scores). However, including the diabetic ulcer demonstrates the potential for CUSEFS to be used for the treatment of diabetic ulcers as well. With regard to patient 6, although the initial surface area of the wound was not measurable, we included this patient in our final analysis, as the treatment area of the affected skin was shown to be much healthier, with less drainage. In addition, this patient experienced a reduction in the level of pain (an additional relevant parameter that we tested) at the end of the study.
Our study findings show that most patients showed decrease in wound size after eight treatments with CUSEFS. In 30% of the patients, the wound healed completely, and the overall average decrease of wound size was approximately 50%. Rosenblum and Papamichael 16 evaluate the efficacy of CUSEFS therapy with BRH-A2 as a treatment for pressure ulcer (PU). Their study protocol was similar to ours, with their patients treated with CUSEFS BRH-A2 device twice weekly and followed up for four, eight and 20 weeks. At four weeks, 40.4% of the overall PU wounds closed by 50% of their surface area but none of them had completely healed. The authors hypothesize that the difference in total closure rate at four weeks stems from the different etiologies and mechanisms for each of the wound types. Venous ulcers have a predominantly vascular component in contrast to PUs which are primarily metabolic in nature. 17 Therefore, utilizing modalities that improve microcirculation in and around the wound bed, such as the BRH-A2 device, might explain the more rapid healing process in venous leg ulcers as a function of the increased vascularity of the wound bed versus the pressure ulcer wound bed.
As seen in many international guidelines, the management of pain associated with VLUs remains largely unaddressed, although some clinical research is trying to encourage wound care practitioners to address chronic ulcer pain and its impact on patients’ well-being and the health care system at large. 13 Wound pain is a serious clinical problem for older people with chronic leg ulcers as it can substantially reduce quality of life. 18 Over the past decade, wound care management consistently demonstrates that healing cannot be effectively managed if a patient's experience of pain is not sufficiently addressed and improved. 19 Hofman et al. 20 found that approximately 64% of patients with VLUs reported severe intermittent or continuous pain. Persoon et al. 21 and Green et al. 13 reported that pain was the leading focus of clinical attention in patients with VLUs, being described as the worst symptom, and the cause of significant suffering. VLU-related pain may have far reaching consequences including a negative impact on patients’ mental wellbeing, delayed healing, reduced mobility, loss of independence and increased hospital visits.22,23
Our research found that nearly all patients with VLUs treated with CUSEFS therapy had a reduction in pain level and almost 50% of them were free of pain after four weeks of treatments. Avrahami et al. 12 conducted the first retrospective multicenter study on the Combined Modulated Ultrasound and Electric Field Stimulation (CUSEFS) when studied as a single modality over a variety of wounds, which included DFUs as well as VLUs. Their results showed that of 38 VLUs treated, 71.7% (27) achieved 50% closure within four weeks. However, unlike our study, they did not measure the patient-reported outcome of a reduction in pain. Previous publications have also demonstrated the benefits of each modality on its own in the conservative management of VLUs, however the focus appears to be weighted to wound healing parameters and not on the reduction in ulcer-related pain.24,25 Jünger et al., 26 on the other hand, conducted a double-blind randomized study on 39 patients and demonstrated the benefit of electrical stimulation in the treatment of chronic VLUs. The reduction in pain was measured on a 5-point scale and showed a significant reduction in pain after four weeks which was maintained until the study end at four months. The authors concur with other publications, as well as our publication, in highlighting that the reduction in pain is a central factor for improved quality of life in patients with VLUs, however this study did not study the effect of a combination of US and EFS on pain or wound healing parameters.
Gehling and Samies 27 showed reduction in pain among 80% of their patients after chronic wound therapy with noncontact kilohertz ultrasound. Furthermore, it has been reported that electrical stimulation aids in wound healing as well as reduction of ulcer related pain. 28 It is hypothesized that the effects of the therapeutic US component are intensified by the addition of electric field stimulation during treatment. The micro-movement generated by CUSEFS, with the two distinct wave types, causes an immediate effect, Hence, it is not surprising that the novel CUSEFS device, which integrates these two therapeutic modalities, could be an effective non-invasive adjunctive tool to relieve pain within short timeframe, in these patients.
To our knowledge, this is the first study to investigate the combined modulated CUSEFS when studied as a single modality in VLUs from the perspective of both the patient reduction in pain as well as the objective wound healing process. Previous studies have either studied each modality on its own or have studied CUSEFS only from the perspective of wound healing. This preliminary study therefore adds to the body of knowledge regarding the benefits of CUSEFS in VLUs.
Limitations of our research stem from this relatively small case series study, conducted in a single center. Larger multicenter studies are needed to evaluate pain scores and to compare the outcomes of this study with other types of non-invasive treatment modalities, and with other protocols for the treatment of chronic wounds. The main limitation of our study stems from the consecutive recruitment of patients that resulted in variation between the patients who entered the study, in relation to the size of the wound, and the duration of its presence. We showed a similar trend regarding improvement in pain and reduction in wound size in patients with different characteristics. Although we believe that this trend may actually strengthen our research hypotheses regarding the benefit of CUSEFS in patients with VLUs, we still think that the variability factor should be taken into account when analyzing our results and deciding on the ideal patient for CUSEFS treatment in the real-world setting. This is a preliminary, non-comparative study that will form the basis for further follow-up studies that we plan to conduct in our department. As part of these follow-up studies, we will consider comparing between different sub-groups in our analysis (for example comparing between different time periods that the wound has been present 1–3 months, vs. 3–6 months, vs. 6–12 months) to better determine which patients would ideally suit this type of treatment.
Conclusion
Combined Ultrasound and Electric Field Stimulation therapies with BRH-A2 technology is a promising treatment for VLUs. In accordance with our preliminary results this treatment modality can aid in the reduction of wound surface area as well as reducing the pain suffered by patients from these chronic wounds. Larger multicenter studies are needed to further quantify and qualify the beneficial effect of CUSEFS in VLUs and other chronic wounds.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
How to cite this article
Shapira E, Govrin-Yehudain Y, Heller L. The efficacy of combined ultrasound and electric field stimulation therapy in the treatment of venous leg ulcers. Scars, Burns & Healing, Volume 6, 2023. DOI: 10.1177/20595131231174225.
