Abstract
Keloid scars are notoriously difficult to treat with very high recurrence rates despite a range of treatment options. We present a case report of a 43-year-old man with a resistant keloid scar on his left ear from a piercing. After 15 years of multimodal treatments including surgery, steroid and 5-fluorourcil injections, the keloid persisted. It has responded very well to a single treatment of intralesional cryotherapy (trademark: CryoShape, Etgar Group International Ltd). The authors would now consider intralesional cryotherapy as a useful tool in their armamentarium for prominent, resistant or recurrent keloids. Future experience will guide its clinical applications.
Lay Summary
There is limited evidence of efficacy, more research is required.
Background: Keloid scars grow outside of the initial wound margins. They can be itchy and very unsightly. They are difficult to treat. Whether treated by surgical removal, injections, or radiotherapy, there is a high recurrence rate.
Question: Can a new technique be used to successfully treat resistant keloid scars?
How the work was conducted: A technique of freezing the scar to cause frostbite and auto-amputation of the scar has been developed. This report describes 15 years of multi-modality treatment for a patient who had a large keloid scar on his ear. It recurred after all conventional treatments and had started growing very aggressively despite treatments. A new technique of intralesional cryotherapy was used to freeze the keloid scar. This has had excellent initial results and although the follow-up time is relatively short at six months, there has been no aggressive regrowth yet which is very promising.
What have we learnt: The procedure went smoothly and was very well-tolerated by the patient. The scar resolved with no early evidence of recurrence. We do not yet know whether this scar will recur in the future and if so how quickly. The scar was however very troublesome to the patient before the treatment and his symptoms have now resolved with no sign of regrowth to date. We need a larger case series with long term follow up before any firm conclusions can be drawn from this.
Introduction
A keloid scar is excessive scarring which clinically differs from hypertrophic scarring by extending beyond the original wound boundaries, by not regressing spontaneously and by having the ability to develop months to years after the injury. Histologically, they are composed of large, thick collagen fibres, made from many tightly packed fibrils.1,2 They are more common in patients with darker skin with an estimated incidence of 4.5–16% in people with black skin and Hispanics. 3 People can have a genetic predisposition and younger patients are more prone to developing them. As well as the psychological distress due to the appearance, patients can experience symptoms such as pain and itching. 4
Treatment options have included pressure garments, silicone dressings or ointments, steroid injections, 5-fluorouracil (5-FU) injections, surgery, radiotherapy and combination therapy with variable success and a high recurrence rate. In 2002, Mustoe 5 published international clinical recommendations for scar management, advising intralesional steroid injections for keloid scars, followed by or in conjunction with topical silicone gel sheeting, pressure therapy and surgery further down the list with a high recurrence rate, quoted as 45–100%. Adjuvant radiotherapy reduces the risk of recurrence, but treating a benign condition with radiotherapy remains a source of anxiety. The exact incidence of radiation induced cancer is very hard to quantify. Studies are limited and difficult to standardise due to the different doses, 6 evolving equipment, 6 confounding variables 7 and the need for a long follow-up period. A risk assessment from current literature would suggest that the risk to adults is very low, 6 but younger adults and children are more radiosensitive 8 and therefore should be treated with caution.
Several authors have reported encouraging results from different injectable drugs, including 5-FU, interferon, bleomycin, mitomycin C, retinoic acid and colchicine. The authors of this case report have had positive personal experience with steroid and 5-FU in combination to control and flatten keloid scars 9 and adjuvant laser therapy to treat residual prominent vessels.
Cryotherapy was first reported as a treatment for keloid scars by Shepherd and Dawber in 1982. 10 Intralesional cryotherapy was developed later by Weshahy 11 and tailored for the treatment of keloids by Zoubulis, and Gupta and Kumar.12,13 Har-Shai further developed the needle equipment that was used in this case report. 14 After local infiltration to block the scar being treated, the sharp-cutting, double-lumen, uninsulated needle (Trademark: CryoShape; Etgar Group International Ltd.) is used to pierce the scar tissue. Liquid nitrogen is then passed through the needle which is designed to allow even cooling along its length. The endpoint is an ice ball with 5 mm extension of the freezing onto surrounding tissue. This is then left to desiccate and separate without any further intervention. Disrupting the separation process at this point could cause further trauma and recurrence of the keloid. The idea was developed from the observation that keloid scars did not form after frostbite. The aim is to freeze and destroy all pathological scar tissue leaving a less bulky scar without keloid characteristics.
Case report
We present a case report of a 43-year-old man who developed a keloid scar on his left ear from a piercing. This resisted multiple multimodal treatments over 15 years and responded very well to intralesional cryotherapy.
This patient was originally referred to the plastic surgery department with a keloid scar on his left ear from a piercing at the age of 28 years. Initially, this was managed with surgery and adjunctive steroid injections due to the size of the keloid, followed by six laser treatments with KTP (532 nm) to improve the appearance further. There was no sign of recurrence when he was reviewed 11 months and 17 months following his surgery, but recurrence was noted at 23 months. Three consecutive steroid injections (triamcinolone 10 mg/mL) had no visible effect. A combination of triamcinolone 10 mg/mL and 5-FU was then used. Following this, the scar reduced in size and appeared inactive, pale, soft and non-itchy.
Three years later, he was re-referred with recurrence of the keloid. It was excised for a second time with simultaneous intralesional 5-FU and steroid, followed by four more injections. No further follow-up was arranged due to patient reasons but he was referred again with a recurring keloid 1 year later. Due to the associated discomfort of the injections, he was initially reluctant to have further treatment, but proceeded with seven further 5-FU and steroid injections, and was fitted with a pressure clip. Despite this, the keloid enlarged. Surgical debulking was repeated, followed by six further injections, but the keloid continued to enlarge. Figures 1 and 2 demonstrate the keloid appearance before treatment and after many treatments.

Keloid at presentation before any treatment.

Keloid 15 years later after three operations, 24 injections of steroid or steroid and 5FU in combination, pressure clips and laser therapy.
After counselling the patient regarding intralesional cryotherapy and potential complications, including infection, bleeding, persistent pain, failure of the treatment and recurrence of the keloid scarring, he consented to the treatment.
This was performed in an outpatient treatment clinic. The area was cleansed with an alcohol wipe and anaesthetised with 0.5% levobupivicaine and 1% lignocaine with adrenaline (1:200,000). The cryotherapy needle was inserted through the scar in two areas and liquid nitrogen was passed through the needle for a total of 52 min until freezing of the scar tissue and a border of normal tissue was achieved. In this case, due to the shape of the scar, two passes of the needle were used with cooling of each section. The length of time required to cool the scar was guided by the appearance and feel of the scar and surrounding tissue. A paraffin-based ointment with polymyxin B sulphate and bacitracin zinc was applied and a simple non-adhesive paraffin tulle dressing and gauze were used. The patient described rapid progression of necrosis over the following week with final separation of the necrotic scar leaving a healed wound by day 24 post treatment. At the 3-month and 6-month follow-up appointments, the residual scar was small and asymptomatic. Figures 3–8 demonstrate the stages of the treatment.

Needle inserted through the keloid and freezing with liquid nitrogen commenced.

Lower portion of the keloid frozen with the ice ball appearance.
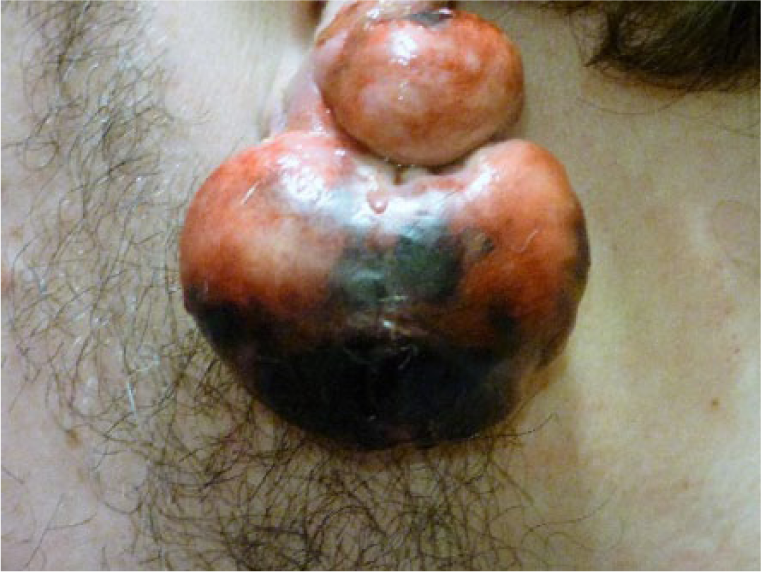
Day 8 post treatment showing necrotic tissue.
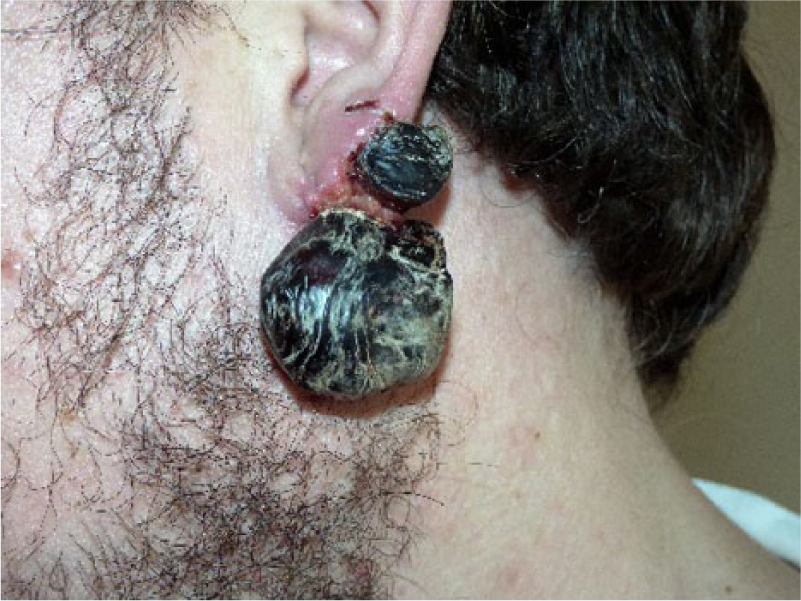
Day 18 showing dry necrosis of keloid scar.

Day 21 showing the patient demonstrating that the necrotic keloid is separating.

Day 30 showing a fully healed small scar.
Discussion
Preliminary studies have shown promising results with significant debulking of keloid scars in the majority of cases. 14 This case demonstrated complete initial resolution of an aggressive keloid scar with no sign of recurrence noted in the first 6 months post treatment. Prior to using cryotherapy, the keloid was growing rapidly and was not responding to the standard therapy provided by the unit. It responded well to the cryotherapy, but the main limitation of this report is the relatively short follow-up time. Due to this limitation and the knowledge that keloid scars can occur months to years after the initial insult, we cannot conclude that the keloid will not recur. We can, however, be confident that since there are no signs of recurrence to date, this keloid is definitely not behaving in such an aggressive way as it was before the treatment. The authors plan to follow this patient up indefinitely with regular 6 monthly reviews.
The patient is aware of the possibility of a future recurrence and the novelty of this procedure within the unit. He will therefore continue self-examination between these appointments and contact the unit if he has any concerns. He found the regular injections prior to the cryotherapy difficult to tolerate and the one-off cryotherapy treatment much more manageable. To date, the patient is very pleased with the treatment process. He has not had any adverse effects such as persistent pain. He is keen to share his images in order to help patients with similar troublesome keloid scarring. The procedure has since been performed on eight patients in this department.
The authors would now consider intralesional cryotherapy as a useful tool in their armamentarium for prominent resistant or recurrent keloid. Future experience with other refractory keloids will guide its clinical applications further.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
