Abstract
Conventional embryo selection by morphological evaluation is still related to relatively low implantation and live birth rates. To resolutely take up this challenge, noninvasive and invasive methods of embryo selection are still debated regarding their improvement on in vitro fertilization (IVF) success rates. Within the past few years, combining morphology with kinetics has inspired a new field named “morphokinetics,” which enabled a new way of evaluating and selecting embryos by continuous surveillance. Many studies have tried to connect more or less conclusively embryo development, timing of the mitotic divisions, embryo viability, and implantation. The aim of this review is to summarize the current understanding of time-lapse monitoring in the IVF laboratory and to discuss the evidence regarding morphokinetics as a predictive method for blastocyst formation, aneuploidy detection, and implantation potential.
Introduction
Historically, morphological evaluation of embryos has been the method of choice to assess and select embryos (Pinborg, 2005; Stromberg et al., 2002). As the embryo quality is still the most predictive factor of the in vitro fertilization (IVF) treatment’s outcome (Sazonova et al., 2013; Shaulov et al., 2015; Walker et al., 2004), scoring embryos remains the fundamental IVF of laboratories, but still remains open to intra- and interpersonal variability, despite recent efforts made to find more objective means (ALPHA-ESHRE, 2011a, 2011b). Also, to decrease the risk of multiple pregnancies, a figure that in 2011 reached an alarming threshold of 19.2%, a better selection of embryos to be transferred is essential (Kupka et al., 2014).
The development of incubators with built-in time-lapse technology (EmbryoScope™, Miri®, Geri™) or of specialized cameras that function within a conventional incubator (PrimoVision™; Eeva™) has enabled the routine study of morphokinetics of the preimplantation human embryo within a clinical IVF setting.
Continuous monitoring of embryo development from fertilization to blastocyst stage by automated time-lapse imaging has offered the possibility to appraise the timing of embryonic cell division (Kirkegaard et al., 2012a; Lemmen et al., 2008; Pribensky et al., 2010; Wong et al. 2010). In the classical morphological evaluation, the embryos have to be removed for few minutes from the incubator daily to allow a static and single observation under the microscope; whereas in time-lapse systems, embryos can be continuously monitored from images taken 4–6 times per hour without being removed from the incubator. In addition, time-lapse allows observing exact time points of cell divisions, compaction and blastocyst formation, generation and absorption of fragments, and multinucleation. Thus, blastocyst evaluation in conventional incubation systems is based on morphologic criteria only, for example, blastocoel formation and expansion, inner cell mass quality, and trophectoderm quality, whereas in time-lapse instruments, kinetic parameters can be evaluated besides pretransfer final morphology (Gardner et al., 1998; Meseguer et al., 2011; Wong et al., 2010).
Safety studies
The imaging system in the EmbryoScope™ uses low-intensity red light (635 nm) and is thus devoid of low-wavelength light (<550 nm), which has been shown to be inhibitory to embryo development (Oh et al., 2007; Takenaka et al., 2007) and comprises ∼15% of the light encountered in a normal IVF microscope (Meseguer et al., 2011). Effects of repeated, short, low-intensity light exposure used for time-lapse imaging were compared with the longer, less frequent exposure to higher intensity light used for routine microscopic embryo morphology observations in two studies. Safety of embryo culture in time-lapse versus conventional incubation was thus shown in embryos from fresh oocytes derived from donors or infertile patients, respectively (Cruz et al., 2011; Kirkegaard et al., 2012b).
Predicting blastocyst formation
Culturing embryos until day 5 to select the best morphology blastocyst ensures higher implantation and decreased miscarriage rates either after fresh transfer or following vitrification (Gardner et al., 1998; Kuwayama et al., 2005; Liebermann, 2009; Milki et al., 2000).
The examination of the development of 242 slow frozen and thawed two-pronucleate stage embryos showed that blastocyst development can be predicted at early stages, before embryonic genome activation (Wong et al., 2010). Blastulation (tSB)was predicted in this study by measuring three dynamic, noninvasive imaging parameters by day 2 after fertilization, namely, the timing of the first, second, and third mitoses (Wong et al., 2010).
In a subsequent retrospective cohort study, 834 embryos from 165 oocyte donation couples were analyzed using a time-lapse monitoring system. Previously published Meseguer’s hierarchical model was used in an effort to correlate kinetics of early embryo development with blastocyst formation and quality (Cruz et al., 2012). This study showed that a larger fraction of the embryos that underwent cleavage within the proposed optimal time interval for implantation reached the blastocyst stage or a better blastocyst morphology, particularly for t3, t5, s2, and cc2 (Cruz et al., 2012). The authors concluded that embryos with a t5 of 48.8–56.6 h have not only a higher implantation potential but also a higher probability of developing into a good morphology blastocyst (Cruz et al., 2012).
Dal Canto et al. (2012) have also investigated the morphokinetics regarding the development of embryos to blastocyst and implantation. Cleavage times to seven- and eight-cell stages and relative intervals from four- to eight-cell stage but also from five- to eight-cell stage have been found to be statistically different for embryos arresting after the eight-cell stage and for embryos developing to blastocyst. Blastocysts’ ability to expand correlates with all cleavage times from the three-cell stage onward. Moreover, implanted embryos achieve the eight-cell stage earlier than those that did not implant. Therefore, the study showed that cleavage from two- to eight-cell stage occurs progressively earlier in embryos with the ability to develop to blastocyst, expand but also implant (Dal Canto et al., 2012). These observations also infer that using cleavage times until the five-cell stage may not be enough in a different IVF laboratory setting to predict blastocyst formation potential and implantation, as delays in cleavage times accumulate and hence are more prominent from the five- to the eight-cell stage. However, a prospective study reported that only the duration of the first cytokinesis, the duration of the three-cell stage, and direct cleavage to three cells predict development to high-quality blastocyst with an area under curve (AUC) of 0.69, but no difference was found in timing between implanted and nonimplanted embryos (Kirkegaard et al., 2013b).
Furthermore, a model based on some cleavage time intervals up to the four-cell stage (t3−t2: time between cytokineses 1 and 2; t4−t3: time between cytokineses 2 and 3) inferred that when used with traditional day 3 morphology, it may help embryologists to predict usable blastocyst outcomes and reduce the variability among embryologists (Conaghan et al., 2013; Diamond et al., 2015). Nevertheless, when the model was applied retrospectively in an independent set of morphokinetic data, a large fraction of the transferred embryos that would have been classified as nonusable were found to have actually resulted in ongoing pregnancies. There are probably two reasons for this: First, the model has a high specificity (84.7%) but a relatively low sensitivity (38%); second, the time intervals for t3−t2 and t4−t3 are too narrow, deselecting erroneously viable embryos (Kirkegaard et al., 2014).
Therefore, our group aimed to build a model predicting good quality blastocyst formation of a day 3 embryo using our own morphokinetic data. The ultimate objective of the analysis was to adapt this kinetic blastocyst prediction model as an alternative to conventional morphologic grading. Thus, we translated the rhythm of the preimplantation embryo development into equations to reflect with higher accuracy the cleavage synchronicity (CS) observed throughout the first 3 days (Çetinkaya et al., 2015). The first formula used, the CS from two to eight cells, describes the synchronicity of cleavage cycles and is based on the fact that a human embryo synchronously divides into two cells, stays shortly at the three-cell stage and divides again, to stay longer at the four-cell stage. The five-, six-, seven-cell stages are very rapid compared to the duration of the four-cell stage. Thus, the equation CS2-8 = ((t3 − t2) + (t5 − t4))/(t8 − t2) gives the total duration ratio of cell evenness until the eight-cell stage (Çetinkaya et al., 2015). Similarly, the CS from four to eight cells, CS4–8, expresses the duration of the five-, six-, seven-cell stages when compared to the interval from four to eight cells (Çetinkaya et al., 2015).
The study included 3354 embryos, with annotations up to t8, and cultured until day 5 from 626 infertile patients. A total of 17 kinetic expressions, either absolute cleavage timings and time intervals or time ratios, were tested retrospectively for the prediction of blastocyst formation and quality. Relative timings (t8 − t5, the CS from four to eight cells and from two to eight cells) were found to be better indicators of blastocyst formation and quality when compared to absolute time points (Figure 1). Especially, the CS from two to eight cells (CS2-8) = ((t3−t2) + (t5−t4))/(t8–t2)) was found to be the best predictor available on day 3 for blastocyst formation and quality (AUC: 0.786; sensitivity: 83.43; specificity: 62.46). Thus, we concluded that time intervals and relative ratios based on selected cleavage cycles defining synchronicity allowed a specific analysis providing high predictivity of blastocyst formation and quality.
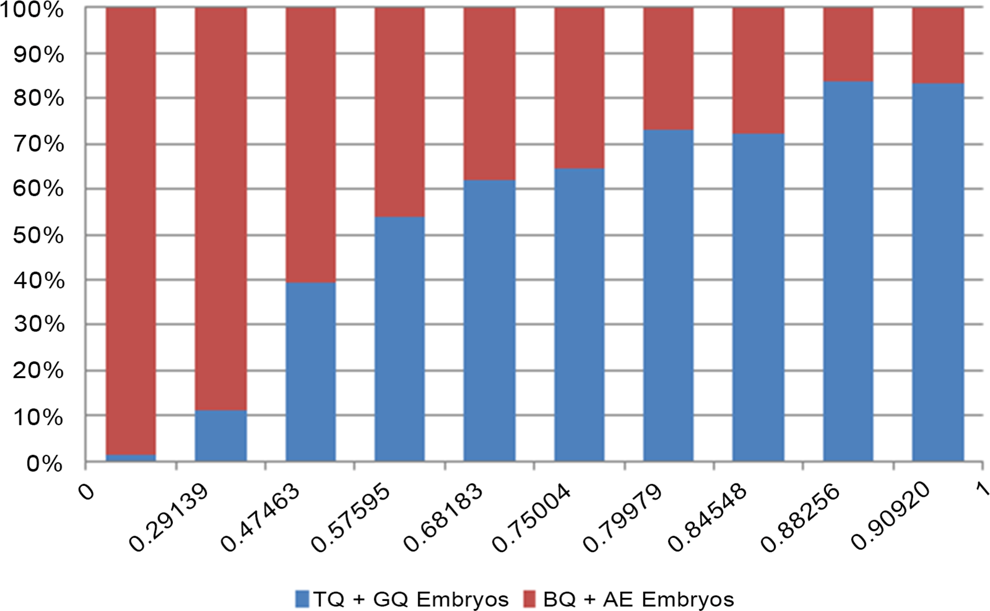
Histogram representing the 10% distribution of our initial study group (n = 788) for the cleavage synchronicity from two- to eight-cell stage: cleavage synchronicity CS)2–8 = ((t3−t2) + (t5−t4))/(t8−t2). TQ + GQ top and good quality embryos (TQ + GQ) are represented in blue and bad quality and arrested embryos (BQ + AE) in red.
The latest model reported to date was built retrospectively in 832 transferred blastocysts and the time to achieve a morula (81.28 h < tM < 96 h) was established as the first step of a hierarchical model; t8 − t5 was also found to be critical and was implemented as a second criterion with a threshold of 8.78 h (Motato et al., 2016). Although blastocyst formation was predicted with a receiver–operating characteristic curve (ROC) value of 0.849 (95% confidence interval [CI], 0.835–0.854), the same parameters were found to be less predictive of implantation, with an ROC value of 0.546 (95% CI, 0.507–0.585), which is, as recognized by the authors, poor (Motato et al., 2016). Indeed, such embryo-based systems, although certainly giving a reliable idea on the quality of the embryo, which can be extrapolated to the quality of both gametes, can certainly not reflect the receptivity status of the endometrium on the embryo transfer day. Therefore, linking implantation to embryo development, especially on day 5, cannot be straightforward and should include endometrial receptivity data to be considered as another criterion (Garrido-Gómez et al., 2013; Salamonsen et al., 2013.
Implantation prediction
Deselection models
Prediction models can also be used to deselect embryos with a reduced implantation potential. The CS algorithm allows for the prediction on day 3 of embryos that have obviously a decreased chance of becoming a blastocyst, thus a much lower probability of generating a clinical pregnancy (Çetinkaya et al., 2015).
Moreover, as time-lapse monitoring allows precise identification of each cell cycle, abnormal cleavage events such as direct cleavage can be easily observed. The implantation rate of embryos dividing from two to three cells in less than 5 h was observed as being considerably lower than those with a normal cleavage pattern (1.2% vs. 20.2%, respectively), implying that those embryos should not be transferred unless no other possibilities exist (Rubio et al., 2012).
The frequency of embryo multinucleation detected by time-lapse system and its impact on pregnancy outcome was studied in 159 embryos and was detected in 145 intracytoplasmic sperm injection (ICSI) cycles. In cycles with multinucleated embryo transfers compared with cycles with no multinucleated embryos, clinical pregnancy rates (respectively, 23.4 vs. 44) and implantation rates (respectively, 23.3 vs. 43.6) were found to be significantly lower (Ergin et al., 2014).
Also, blastomere fusion, also termed reverse cleavage, was recently described as significantly compromising embryo development, culminating in poor implantation potential. Interestingly, the assessment of the spatial arrangement of the four blastomeres or the theoretically resulting number of intercellular contact points (ICCPs) showed that embryos with fewer than six ICCPs at the end of the four-cell stage show compromised subsequent development and reduced implantation potential (Liu et al., 2015).
Selection models
Besides deselection models, positive prediction models were suggested. The first algorithm for implantation prediction was proposed by Meseguer et al. (2011) and used early cleavage divisions. This retrospective analysis of morphokinetic data from 247 embryos generated from IVF and donation cycles, incubated in time-lapse, and transferred on day 3 allowed the establishment of a concept by which a hierarchical model relying on morphokinetics can predict embryo implantation (Meseguer et al., 2011). In this study, the most predictive parameters are as follows: first, the time of division to five cells (t5), second, the time between division to three cells and subsequent division to four cells (s2 = t4−t3), and finally, the time between division to two cells and division to three cells (cc2 = t3−t2). In this hierarchical classification tree model, implantation rates of the different embryo categories varied from 8% to 52%, in the worse group E and best group A, respectively (Meseguer et al., 2011).
The same group has also presented a retrospective cohort study including again a mixture of donation and autologous ICSI cycles collected from 10 IVF clinics sharing the same protocols with some technical differences, cultured in time-lapse (n = 1390) or in a standard incubator (n = 5915) (Meseguer et al., 2012). The report indicated that by culturing and selecting embryos only using the time-lapse system, the improvement on the clinical pregnancy rate will be of 9%, or in other words, the relative increase would be of 20.1% (Meseguer et al., 2012).
Algorithms that have been proposed brought a great enthusiasm into the field as they showed how to implement this new technology into a clinical setting and revealed that indeed timings did matter to predict that an embryo would implant (Meseguer et al., 2011; Wong et al., 2010). Most importantly, the study by Meseguer et al. (2011) showed that using quartiles to approach this huge data generated by all time points coming from the numerous annotations was a sound solution. Thus, implantation was clearly shown not to always fall in white or black zones but that gray zones exist in relation with the cleavage timings’ quartiles. However, the proposed model could not be widely reproduced and become a starting point for laboratories that look for ways of predicting blastocyst formation and implantation in their own setting (Best et al., 2013).
Time points indicating precise embryo cleavages were shown to be affected by ovarian stimulation protocols, culture media (sequential or single step), fertilization method (IVF or ICSI), culture conditions (e.g. reduced oxygen) but also by the patients themselves as illustrated by reports investigating the relation between the body mass index, polycystic ovary syndrome, and morphokinetics (Bellver et al., 2013; Ciray et al., 2012; Cruz et al., 2013; Kirkegaard et al., 2013a; Muñoz et al., 2013; Wissing et al., 2014). Therefore, in a blastocyst and implantation prediction model that seeks to be commonly used, these precise time values cannot be used alone or in other words cannot be standardized in order to be strong enough to be extensively accepted. Also, simulating embryo development with precise time points or with quartiles defined by sharp limits may not be correct and may not reflect the plasticity of embryos (Çetinkaya et al., 2015). Moreover, if the time intervals of optimal division are defined too narrow, a small displacement in timing may result in viable embryos being deemed unviable (Kirkegaard et al., 2014; Kirkegaard et al., 2015).
The first prospective, randomized, double-blinded controlled study aiming to determine whether incubation in time-lapse and selection supported by the use of a multivariable morphokinetic model improve reproductive outcomes in comparison with incubation in a standard incubator embryo culture and selection based exclusively on morphology was published by Rubio et al. (2014) and involved 843 patients who underwent ICSI. When analyzed per treated cycle, the ongoing pregnancy rate was found to be statistically significantly increased by 10% in favor of time-lapse (51.4 vs. 41.7%). Early pregnancy loss was also calculated as being statistically significantly decreased for the time-lapse group with 16.6% versus 25.8% (Rubio et al., 2014). However, the patient population was mixed, including oocyte donation cycles. The day of transfer (3 or 5) diverged also, adding therefore supplemental variability in the study. The randomization was flawed since some patients to be randomized requested time-lapse incubation. Most importantly, as the embryo selection method differs for each group (morphology alone for standard incubation and a morphokinetic model for time-lapse incubation), the better outcomes obtained with the use of a morphokinetic model in time-lapse cannot be reliably attributed to the model itself, since undisturbed culture may well be the reason for the improvement observed. Indeed, Kahraman et al. (2013) observed that in a selected good prognosis elective single embryo transfer (eSET) population, similar rates of good and top quality blastocysts and comparable implantation and pregnancy rates were achieved in conventional or time-lapse incubators and that the stable culture conditions provided by time-lapse incubators and the use of morphokinetic parameters may allow the selection of the best available embryos with high developmental capacity, especially in poor prognosis patients.
A recent retrospective multicentric study of 1664 cycles (799 of which were used to develop an algorithm and 865 to test its predictive power) questioned whether morphokinetic markers can be used to select the embryos most likely to implant and whether the results are likely to be consistent across different clinics (Basile et al., 2015). Three variables were identified as being most closely related to implantation (t3, followed by cc2 and t5). An algorithm classifying embryos from A to D according to implantation was proposed and implantation rates observed were as follows: A: 32%, B: 28%, C: 26%, D: 20%, and E: 17%. Thus, the authors claimed that this new strategy represents the best option to improve clinical outcomes based on embryo selection.
Aneuploidy prediction
With advancements in technologies for assessing embryo ploidy, for example, array comparative genomic hybridization (aCGH), single-nucleotide polymorphism microarray, and next-generation sequencing, combining morphokinetic and genetic evaluations has been a new opportunity in ART. Furthermore, an interesting publication highlighted the imprecision of conventional morphology in selecting euploid embryos, as a 44.9% aneuploidy rate was observed for blastocysts belonging to patients with good prognosis (Yang et al., 2012).
The aneuploidy status of embryos according to the start of tSB and the formation of a full blastocyst (tB) was analyzed, and a risk classification of aneuploidy was constructed with three categories defined as low, medium, and high with an aneuploidy rate of 36%, 69%, and 100%, respectively (Campbell et al., 2013a). This risk classification analysis also proved beneficial for correlating with implantation and fetal heart beat when applied in a retrospective study on nonbiopsied embryos (Campbell et al., 2013b). In the logistic regression model applied, for each year, the patient age increases, the odds of having an aneuploid embryo increases by 18%, and for each hour, the value of tSB increasing the odds of getting an aneuploid embryo increases by 5% (Campbell et al., 2014).
Chavez et al. (2012) have combined additional technologies to time-lapse in order to generate a ploidy prediction model on the basis of embryo kinetics. They observed that at the four-cell stage of development, dynamic assessment of cell cycle parameters in conjunction with fragmentation analysis and blastomere asymmetry assists in the differentiation between the type of error (meiotic versus mitotic), detects chromosomal duplications (trisomies) and deletions (monosomies), and provides a reliable readout of the degree of mitotic mosaicism (high vs. low) in human embryos (Chavez et al., 2012).
As we observed in our own practice that early blastulating embryos were mostly diagnosed as being euploid, we applied that model in our own data with some modifications and found that CS (CS2-8, CS4-8) thresholds derived from aneuploid embryos predict embryo implantation and live birth in an infertile cohort without Preimplantation Genetic Screening (PGS) (Pirkevi et al., 2014). A total of 359 embryos biopsied on day 5 and diagnosed using array CGH were used to derive the ploidy model, which was further retrospectively applied to 997 embryos with known implantation data (KID). Live birth was available for 669 KID embryos belonging to 387 patients. Four categories were defined in the non-PGS group using cutoff values obtained from biopsied embryos. Cutoff values were calculated as 0.8315 for CS2–8 and as 0.2734 for CS4–8 in PGS embryos. The mean female age was 33.18 and 32.35 in the PGS and non-PGS groups, respectively. The KID rate increased from 22.48% to 42.86% (twofold increase, χ2 p < 0.0001) and the live birth rate was multiplied by three in the high euploidy category when compared to the high aneuploidy category (from 14.44% to 42.10%, χ2 p < 0.0001) (Figure 2).
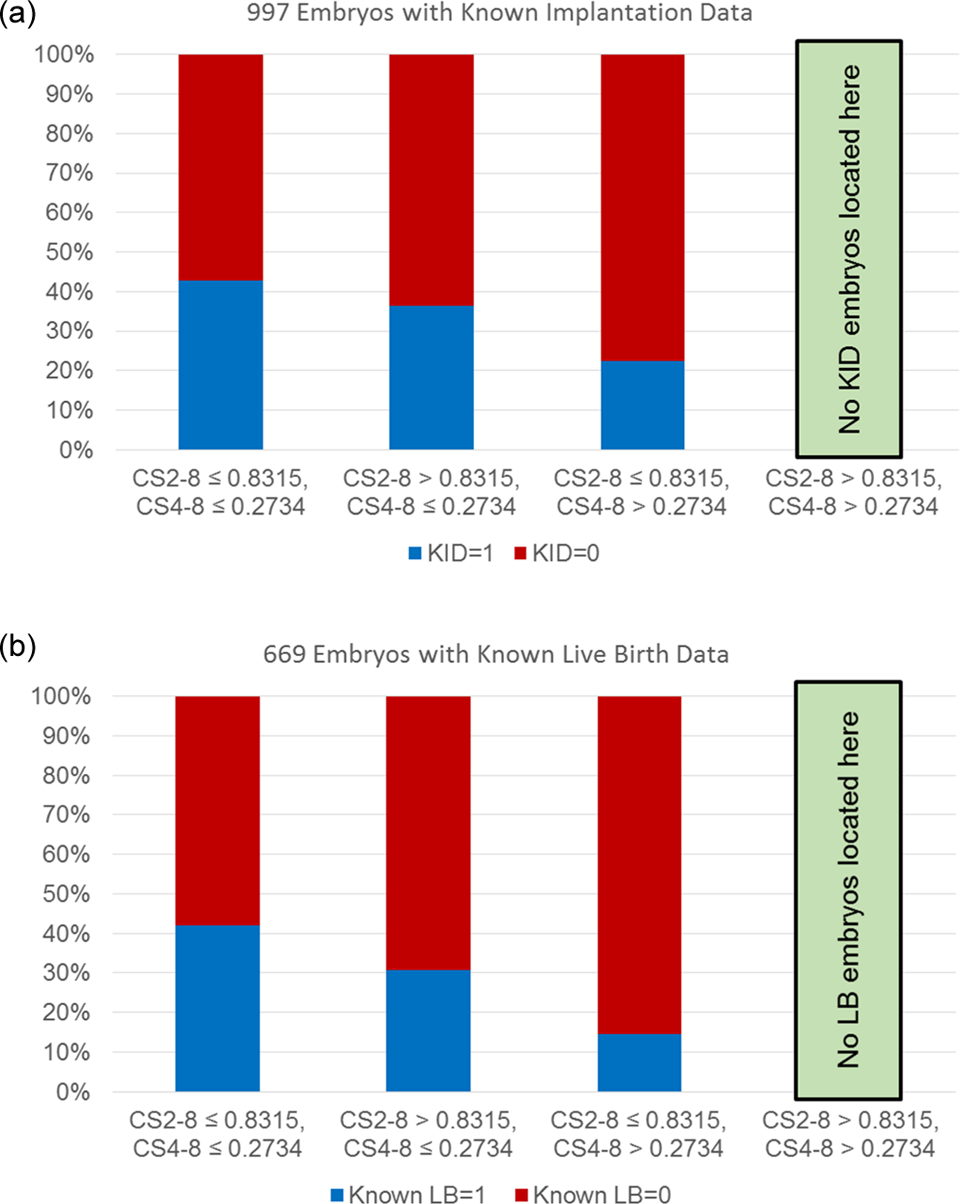
(a) The known implantation data (KID) rate increased from 22.48% to 42.86% (twofold increase, χ2 p < 0.0001). (b) The live birth rate was multiplied by three in the high euploidy category when compared to the high aneuploidy category (from 14.44% to 42.10%, χ2 p < 0.0001).
Differences in the cleavage time between chromosomally normal and abnormal embryos were also analyzed, and an algorithm to increase the probability of noninvasively selecting chromosomally normal embryos was elaborated (Basile et al., 2014). The study analyzed the chromosomal content by aCGH at cleavage stage, where mosaicism is known to be highly prevalent. Observations in 504 embryos resulted in an algorithm composed of two variables: t5−t2 < 20.5 h and 11 h < cc3 = t5−t3 < 18 h as increasing the probability of selecting chromosomally normal embryos in the absence of PGS (Basile et al., 2014).
The same thresholds were applied in a different IVF laboratory, which claimed that no evidence of association between blastocyst aneuploidy and morphokinetic assessment was found in a selected population of poor-prognosis patients composed of advanced maternal age and repeated implantation failure cases (Rienzi et al., 2015). As outlined earlier, morphokinetic parameters are influenced by culture media (Global for Basile and Sage for Rienzi) and culture conditions (20% O2 for Basile and 5% O2 for Rienzi) but also by stimulation protocols (antagonist for Basile and agonist or antagonist for Rienzi) (Kirkegaard et al., 2015). Therefore, discrepancies in morphokinetics are expected in laboratory practice where embryo culture is not aligned, and the model should have been first retrospectively applied and fine-tuned in order to be effective in a different clinical setting.
Time-lapse can never replace array CGH but can provide additional valuable data in order to choose the most suitable embryo(s) for a cost-effective trophectoderm biopsy strategy and for single embryo transfer. In other words, the use of these algorithms does not necessarily replace blastocyst culture as well; it is the combination of blastocyst culture and selection based on morphology plus kinetics markers that seems to be the best approach for improving clinical outcomes (Basile et al., 2015).
Conclusion
Until now embryos could only be evaluated with morphological grading systems, which are clearly subjective and prone to intra- and interpersonal variations. Attempts to better score embryos according to their metabolism with glucose uptake measurements or to their respiration with oxygen consumption rates are very promising but unfortunately not currently available in clinical practice (Gardner et al., 2012; Tejera et al., 2012). Other attempts to find complementary metabolic methods for morphological assessment revealed not to be effective and reliable in a clinical setting, time-consuming, or very expensive, thus difficult to put in the daily practice (Scott et al., 2008a, 2008b; Seli et al., 2007, 2010).
Therefore, the time-lapse technology has become a new option to consider in a routine embryology laboratory. High-resolution pictures of embryos obtained from fertilization up to the blastocyst stage have offered insightful details of mitotic divisions that could not be monitored before. Watching and annotating the embryos grow until the day they will be replaced have undeniably changed the way to select embryos to be transferred.
Selecting day 3 embryos with a high probability of becoming top and good quality blastocysts without the need to culture two more days fragile embryos outside the body may allow more cleavage-stage embryo transfers. Indeed, controversial reports exist on preterm deliveries, postnatal effects, and epigenetic modifications as long-term risks of blastocyst culture (Kalra et al., 2012; Katari et al., 2009). A recent review suggests that although blastocyst stage embryo transfers ensure an increased live birth rate per fresh embryo transfer, it ultimately results in lower cumulative live birth rates per couple, higher risk of preterm birth, large for gestational age, monozygotic twins, and congenital anomalies compared with embryo transfer at cleavage stage (Maheshwari et al., 2016). As extended conventional embryo culture in laboratory conditions still allows for a selection among other embryos looking alike on day 3 regarding morphology, kinetic selection of day 3 embryos will certainly increase the outcomes of cleavage-stage embryo transfer, which is nowadays inferior to blastocyst transfer (Glujovsky et al., 2012 Cochrane review).
Moreover, aneuploidy algorithms reviewed herein may also allow the development of biopsy strategies for PGS and PGD cases by predicting top and good quality blastocysts that will be available for trophectoderm biopsy. Also, applying an aneuploidy risk model after having adapted the equations in-house may allow a subselection or a prioritization of blastocysts for an eSET (Campbell et al., 2013a, 2013b). However, morphokinetics is a way of assessing embryos and will therefore never replace a genetic test per se.
Also, we advise a cautious approach when considering transferring such morphokinetic embryo selection models between centers without prior validation. Kinetic parameters are very much affected by culture conditions, culture media, stimulation type, and female age and are therefore not universal. Some embryo development concepts may hold true for different IVF settings (e.g. tSB, tB, and tEB for aneuploidy prediction) but the thresholds found in one study cannot be copied and pasted to be implemented in a different laboratory. This is especially true for implantation models. Since each IVF laboratory may not have the same transfer policy and the clinical etiology of patients may differ in day 3 versus day 5 transfers, although outcomes of day 3 transfers can be modeled by blastocyst formation models, predicting implantation in day 5 transfers remains a very challenging task.
To conclude, and as recently reviewed by Kaser and Racowsky (2014), morphokinetics has the potential to revolutionize clinical embryology; however, robust prospective studies reporting clinical outcomes as end points and specifically live birth rates are urgently needed. Although time-lapse incubation systems are valuable in building algorithms predicting blastocyst formation, quality, and aneuploidy in IVF laboratories, well-designed randomized controlled trials are still needed to evaluate the efficacy of morphokinetic models in order to clinically establish that time-lapse systems are essential in improving implantation in IVF treatments.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
