Abstract
Midregional pro-adrenomedullin (MR-proADM), midkine, and stromelysin2 (ST2) are novel cardiac biomarkers associated with heart failure and atherosclerotic diseases like stable ischemic disease and acute coronary syndrome. The potential association between these three biomarkers and peripheral artery disease (PAD) remains unclear. The aim of this study was to assess the correlation between these three biomarkers and their association with PAD in the Chinese Han population. This study included 224 patients suspected of having coronary artery disease (CAD). All subjects underwent coronary angiography and carotid and subclavian ultrasound assessment for detection of coronary and peripheral atherosclerosis and were divided into two groups according to whether they had PAD or not. Pearson’s correlation coefficient
Introduction
Peripheral artery disease (PAD) has become a global public health problem. Patients with PAD have a higher risk of adverse cardiovascular and cerebrovascular events, such as heart attack, stroke, and death; however, the public does not fully understand the definition of PAD, its risk factors, and related knowledge. 1 Moreover, available study results further reveal that PAD patients have a lower level of education that may negatively affect the therapy of this complex disease. 2
Recently, great progress has been made regarding the utilization of novel biomarkers in the early diagnosis, risk evaluation, and stratification of coronary artery disease, 3 acute coronary syndrome,4,5 and heart failure.6,7 Moreover, in both basic and translational medical research, the novel, widely used cardiac biomarkers have attracted our attention, among which midregional pro-adrenomedullin (MR-proADM), 8 midkine,9,10 and stromelysin2 (ST2)11,12 have been proven to be associated with PAD or useful for risk evaluation and diagnosis.
Nonetheless, discrepancies still exist for different populations regarding the use of these novel biomarkers for earlier diagnosis and risk assessment of PAD 13 and some of these results might provide possible explanations. 14 Taking these inconsistent findings into consideration, we found that a study of the three biomarkers, MR-proADM, midkine, ST2, and their association with PAD in a Chinese population is still lacking even there is lack of data regarding the effect of race on the development or progression of PAD. We, therefore, designed this study to assess the inner association of these three biomarkers, their gender differences, and their association with PAD in the Chinese Han population, by incorporating these complex pathophysiological processes present in PAD to facilitate a more accurate evaluation of PAD.
Material and methods
Study subjects
Between December 2017 and December 2018, 224 patients were consecutively enrolled from the Department of Cardiology, Affiliated Sixth People’s Hospital East to Shanghai Jiao Tong University. The study participants were all hospitalized for suspicion of CAD, were willing to participate in the study, and all subjects underwent coronary angiography and carotid ultrasound assessment for detection of coronary and peripheral atherosclerosis; 81 of these patients had stable CAD. CAD was defined as at least one stenosis (⩾70%) in one of the three main coronary arteries or their major branches assessed by coronary angiography (CAG). Stable CAD was defined according to Chinese guidelines. 15 PAD was defined as having ⩾50% stenosis in ⩾1 carotid or subclavian artery; 133 patients had PAD and the other 91 participants without PAD served as non-PAD controls. The exclusion criteria included acute coronary syndrome (ACS, including ST-segment elevation and non-ST-segment elevation myocardial infarction, unstable angina), congenital heart disease, severe kidney or liver disease, acute or chronic inflammation by clinical manifestation and history, or rheumatic immune diseases, and a contraindication for the use of contrast. The Medical Ethics Committee of Shanghai Jiao Tong University Affiliated Sixth People’s Hospital East approved the current study (NO. 2016-006). Each participant gave written informed consent before the study began. The main authors had access to the information which could identify individual participants during and after data collection.
Coronary angiography, carotid ultrasound assessment, and stenosis determination
All patients underwent elective coronary angiography (CAG) during hospitalization and carotid ultrasound assessment for the diagnosis of CAD and PAD. Two cardiologists evaluated the results and determined the final diagnosis, with their consensus as the final result.
Clinical parameters and risk factors
Clinical data, including sex, age, type 2 diabetes mellitus (T2DM), hypertension, and smoking, were collected. Meanwhile, fasting blood sugar (FBS), main lipid parameters, including total cholesterol (TC), low-density lipoprotein cholesterol (LDL-C), triglycerides (TG), high-density lipoprotein cholesterol (HDL-C), white blood cell (WBC) and red blood cell (RBC) counts, hemoglobin, hematocrit, and creatinine were determined from fasting plasma samples by using an automatic chemistry analyzer (Synchron Clinical System LX20, Beckman Coulter, CA, USA). The definition of hypertension, T2DM, and smoking have been previously described. 16
Detection of the concentration of MR-proADM, midkine, and ST2
Venous blood samples were collected during hospitalization, and plasma concentrations of MR-proADM, midkine, and ST2 were determined in January 2019 using commercial ELISA kits (MyBioSource Inc. California, USA and Shanghai Jimian Shiye Co., Ltd. P.R. China), according to the manufacturer’s instructions.
Statistical analyses
SPSS 21.0 software (SPSS, Chicago, IL, USA) was used for statistical analysis. Normally distributed data are presented as means ± standard deviation, and comparisons between groups were performed using the Student
Results
Comparison of baseline characteristics between PAD patients and non-PAD controls
A total of 224 subjects meeting the inclusion criteria were selected, including 133 with PAD and 91 non-PAD controls. Table 1 presents the basic characteristics of the study subjects. Compared with controls without PAD (non-PAD controls), patients with PAD had higher values of TC, LDL-C, FBS, and lower values of MR-proADM and midkine (all
The baseline characteristics of patients with and without peripheral artery disease.

CAD: coronary artery disease; FBS: fasting blood sugar; HDL-C: high-density lipoprotein cholesterol; LDL-C: low-density lipoprotein cholesterol; MR-proADM: midregional pro-adrenomedullin; RBC: red blood cells; ST2: stromelysin2; T2DM: type 2 diabetes mellitus; TC: total cholesterol; TG: triglyceride; WBC: white blood cells.
Data are expressed as the number of individuals (percentage in parentheses) or the mean ± SD, as appropriate.
Correlation analysis of midkine, ST2, MR-proADM, and plasma parameters
Pearson’s correlation coefficient r was calculated to test the associations among midkine, ST2, MR-proADM, and other continuous parameters. Results showed that midkine was positively correlated with MR-proADM and negatively correlated with ST2 (all
Correlation analysis of midkine, ST2, MR-proADM, and main plasma parameters.
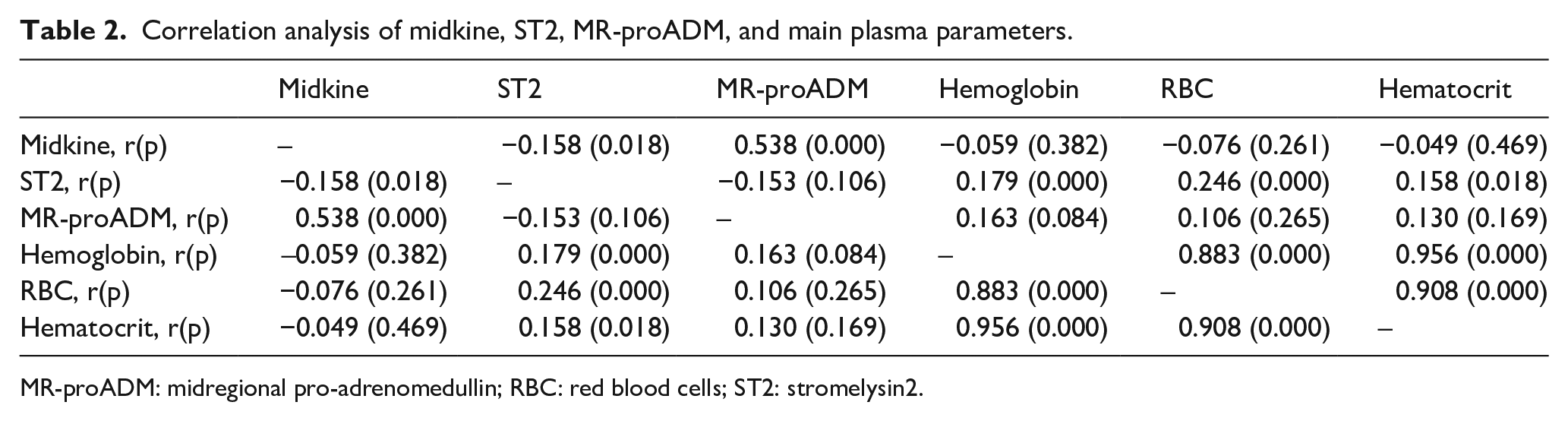
MR-proADM: midregional pro-adrenomedullin; RBC: red blood cells; ST2: stromelysin2.
Impact of sex on baseline characteristics and 3 biomarkers
We conducted further analyses to evaluate the impact of sex on baseline characteristics and the three biomarkers. Compared with females, male patients had a higher ratio of smoking, higher values of WBC, RBC, hematocrit, hemoglobin, and MR-proADM (all
Comparison of main baseline characteristics between male and female subjects.

CAD: coronary artery disease; FBS: fasting blood sugar; HDL-C: high-density lipoprotein cholesterol; LDL-C: low-density lipoprotein cholesterol; MR-proADM: midregional pro-adrenomedullin; RBC: red blood cells; ST2: stromelysin2; T2DM: type 2 diabetes mellitus; TC: total cholesterol; TG: triglyceride; WBC: white blood cells.
Multivariable regression analysis of predictors of PAD
After adjusting for sex, CAD, hypertension, smoking, and other continuous parameters, two factors were identified as predictors of PAD. These two factors were risk factor FBS (OR: 1.163, 95% CI: 1.108–1.401,
Multivariable regression analysis of predictors of peripheral atherosclerosis.

MR-proADM: midregional pro-adrenomedullin; ST2: stromelysin2; FBS: fasting blood sugar.
Discussion
This analysis explored the internal correlation among three novel biomarkers, MR-proADM, midkine, and ST2, and PAD at a single center treating a Chinese Han population, and their association with gender differences. The main findings of our study were that the biomarkers MR-proADM, midkine, and ST2 are internally related and have sex-specific differences. Furthermore, FBS and MR-proADM were found to be risk and protective predictors of peripheral atherosclerosis, respectively, in the Chinese Han population studied.
As a global health problem, PAD confers higher risk of cardio- and cerebrovascular events but receives less attention.1,2 New emerging methods with noninvasive imaging and novel biomarkers have helped us in early risk stratification and decision-making in our daily practice.8–12,17 It is reasonable to observe the elevations of these biomarkers in the early stage of ACS,4,5 and as a relatively unstable condition, we excluded those patients diagnosed with ACS in the current study. In our study, besides the fact that PAD patients had higher values of TC, LDL-C, and FBS, and a higher ratio of hypertension, they had lower values of MR-proADM and midkine, and similar levels of ST2. Our results are different from results found by Kollerits et al., 8 in which the level of MR-proADM was significantly associated with intermittent claudication in a male cohort of patients and the study by Jirak et al., 12 in which PAD patients have significantly higher levels of ST2. Elevated plasma concentrations of ST2 independently predicted short- and long-term risk of fatal CVD events and total mortality in stable CAD patients. 18
However, more recently, emerging data from a study with a large sample again provide us inconsistent or contrary results;
13
in a prospective longitudinal cohort study of middle-aged individuals from the cardiovascular cohort of the Malmö Diet and Cancer Study (MDCS) (
In the current study, we calculated Pearson’s correlation coefficient r to test the associations among midkine, ST2, MR-proADM, and other continuous parameters. The results showed that midkine was positively correlated with MR-proADM and negatively with ST2. Furthermore, ST2 was positively correlated with RBC, hemoglobin, and hematocrit. However, no correlations were found between ST2 and MR-proADM. These correlation results have not been reported before. More interestingly, in a recent study, 19 the authors found that though PAD patients have higher levels of WBC, neutrophil-to-lymphocyte ratio values and C-reactive protein, only mean platelet volume was a statistically significant predictor of PAD. Even so, the real relationship between midkine, ST2, MR-proADM or between ST2, RBC, hemoglobin, and hematocrit, and the exact mechanism warrants further research.
Concerning the risk evaluation, resource utilization, therapy, and outcome in PAD patients, the disease burden obviously is large 17 and gender differences do exist. 20 Doshi et al. 20 more recently reported that women hospitalized for peripheral vascular intervention had a greater risk-profile and resource utilization as expressed by the longer length of hospital stay and higher cost compared with percutaneous coronary intervention. In our study, after assessing the gender-specific effect on these three cardiac biomarkers and PAD, we found that, compared with females, male patients had higher ratios of smoking, higher values for WBC, RBC, hematocrit, hemoglobin, and MR-proADM. Our results support the findings by Eggers et al. 21 and Krintus et al., 22 who found that MR-proADM levels were independently related to current smoking or a history of smoking and low-grade inflammation.
In the current study, compared with females, male subjects had higher values of average MR-proADM. These results partially support the findings by Neumann et al.
23
in which MR-proADM had a male gender-specific association with echocardiographic measures of hypertension. To identify potential independent predictors of PAD, we conducted a multivariate logistic regression analysis to adjust sex, CAD, hypertension, smoking, and other continuous parameters, and found that only FBS and MR-proADM were identified as independent predictors of PAD, with FBS as a risk factor and MR-proADM a protective factor (all
Our study has strengths and limitations. First, the relatively small study sample from one setting (a university hospital) might limit the power of the study; secondly, because all participants are Chinese and came from one tertiary hospital, the study population may not represent the general population or other ethnicities and population groups. The strength of our study is that all participants underwent elective CAG, sensitive carotid and subclavian ultrasound assessment, and thus received a definite and accurate diagnosis, enhancing the quality of the study design. We excluded ACS patients, and those with inflammation or rheumatic immune diseases to ensure all participants had a relatively stable condition. Finally, we did not assess the relation between these three cardiac biomarkers and LVEF values, and our study lacked causal evidence and follow-up data, which restrict the interpretation of the study results.
Conclusion
Three novel biomarkers, MR-proADM, midkine, and ST2, are internally related, and MR-proADM is a protective factor of peripheral artery disease in the Chinese Han population studied. These findings thus provide novel evidence linking PAD and novel cardiac biomarkers and would add additional value to our daily practice.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was supported by Science and Technology Development Fund of Shanghai Pudong New Area (PKJ2018-Y53) awarded in 2019 and the 2017 program of Shanghai Hospital Development Center Research Project (SHDC12017X24). The manuscript was written without the role from funders concerning study design, data collection, preparation of the manuscript or publishment.
Ethics approval
Ethical approval for this study was obtained from The Medical Ethics Committee of Shanghai Jiao Tong University Affiliated Sixth People’s Hospital East (no. 2016-006).
Informed consent
Written informed consent was obtained from all subjects before the study.
Trial registration
Clinical Trial: ChiCTR-DDD-17013908.
