Abstract
Background:
Descending necrotizing mediastinitis has been known to be a life-threatening condition. It is most likely to be lethal without a prompt diagnosis and aggressive surgical management. In the surgical management of this subset of mediastinitis, a debate remains as to whether a transthoracic incision should be mandatory in addition to cervical approach.
Methods:
This is a single-center retrospective study performed at Cipto Mangunkusumo Hospital from January 2012 to June 2014. Patients with descending necrotizing mediastinitis were treated with broad-spectrum antibiotics and with cervical and transthoracic approach (via sternotomy) surgical debridement.
Results:
There were 16 consecutive cases of descending necrotizing mediastinitis. One patient did not undergo sternotomy and was ruled out from the study. The mean intensive care unit stay was 26.4 days, with a mean hospital stay of 46.7 days. There were three mortality cases reported and a total of three cases that needed reoperation. There was neither post-operative sternal dehiscence nor osteomyelitis found.
Conclusion:
Considering there are no post-operative sternal-related infection reported in this study, sternotomy should be considered as an access in descending necrotizing mediastinitis management. In the three mortality cases reported, two patients came with preoperative sepsis and one had iatrogenic subclavian artery injury.
Introduction
Acute mediastinitis is a serious infection affecting connective tissue of the interpleural mediastinal space and surroundings of the median thoracic organs.1–4 Among the many forms of mediastinitis, descending necrotizing mediastinitis (DNM) has been known to be one of the most severe types. During the early 1920s, data suggest that even after the utilization of broad-spectrum antibiotics, mortality is approximately 40%. 5 Furthermore, without a prompt diagnosis and aggressive surgical management, the mortality rate could be as high as 60%. 6
DNM is caused by downward spread of deep neck infections and commonly arises as a complication of odontogenic, peritonsillar, or other pharyngeal infections. 7 After the initial infection occurs, the presence of mixed aerobic–anaerobic bacteria and the inadequacy of immune-competent cells in the cervical mediastinum result in the spreading, descending, and necrotizing process through the fascial planes of the neck.3,7
As recent literature suggests, the attributes of successful DNM management comprises three main principles: (1) early diagnosis (by the use of current imaging modalities), (2) aggressive surgical management with adequate cervical and transthoracic drainage, and (3) perioperative use of appropriate antibiotics. 7
In the surgical management of DNM, a debate remains as to whether a transthoracic approach (i.e. thoracotomy or sternotomy), in addition to cervical approach, should be compulsory.8,9 A number of authors have recommended a selective use of transthoracic exploration of chest in DNM patients,5,10 while others, considering the rapid caudal spread of this disease, recommend mandatory transthoracic mediastinal exploration regardless of the level of anatomical involvement.7,11–13
Methods
This is a single-center retrospective study which aims to evaluate the current surgical management of DNM, in particular, the outcome of mandatory sternotomy in DNM cases.
The study was conducted at Rumah Sakit Cipto Mangunkusumo Hospital (RSCM), Jakarta, Indonesia, from January 2012 to June 2014. Patients presented with DNM at our emergency department were followed until hospital discharge using our database.
Inclusion criteria for the study population were those previously defined by Estrera et al.: 5 (1) clinical manifestations of a severe cervical infection, (2) establishment of a relationship between an oropharyngeal or cervical infection and subsequent mediastinitis, (3) demonstration of radiographic features characteristic of DNM, and (4) documentation of a necrotizing mediastinal infection at the time of operative debridement or necropsy.
Missing information was obtained from medical record review. Our management currently involves both cervicotomy and thoracic approach via median sternotomy for all cases of DNM. Debridement is performed from the cervical region up to the mediastinum with complete excision of necrotic tissues. Primary sternal closure was performed in all of our patients.
Thoracic drains were subsequently inserted to the neck and mediastinopleural region involved with infection for continuous irrigation. Cervical wounds were left open for secondary intention healing.
Wound care was performed daily with honey. Perioperatively, meropenem and metronidazole were administered prior to conversion to definitive antibiotics after isolate from blood culture can be confirmed. Post-operative serial plain chest radiography was conducted for control.
Re-operation criteria include (1) a new accumulation of pus found in chest X-ray, (2) inadequate drainage production, and (3) clinical and laboratory signs of sepsis and visible progression of necrotic tissue.
Results
There are 16 consecutive cases of DNM in RSCM from January 2012 to June 2014. The inclusion criteria were met in 15 out of 16 patients. A patient did not undergo sternotomy and was excluded from the study as the intraoperative findings showed no direct involvement of the disease into the thoracic cavity. Delay between the onset of primary infection to hospitalization was 3–30 days (mean: 9.4 days).
As shown in Table 1, the mean intensive care unit (ICU) stay is 26.4 days, with a longest stay of 51 days. Mean hospital stay for our patients is 46.7 days, the shortest being 30 days and the longest being 74 days.
Summary of 15 DNM patients.
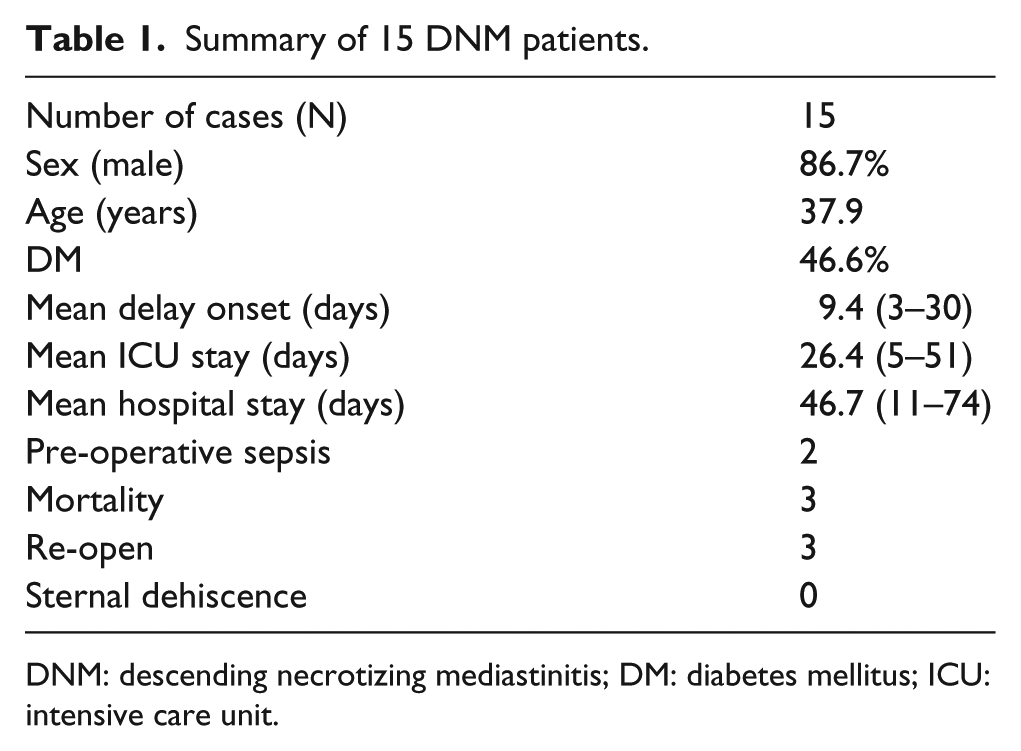
DNM: descending necrotizing mediastinitis; DM: diabetes mellitus; ICU: intensive care unit.
In this study population, the bacterial isolates found include Pseudomonas aeruginosa (four patients), Enterobacter aerogenes (three patients), Acinetobacter baumannii (three patients), Streptococcus viridans (two patients), Staphylococcus epidermidis (two patients), and Enterobacter cloacae (one patient) (Table 2).
The main bacterial isolate that was found from intraoperative tissue culture.

Post-operative wound care with honey and continuous irrigation along with appropriate perioperative antibiotics were shown to be adequate in this study as there are no wound dehiscence reported (Figure 1). Additionally, none of the patients suffered from sternal dehiscence or sternal osteomyelitis.
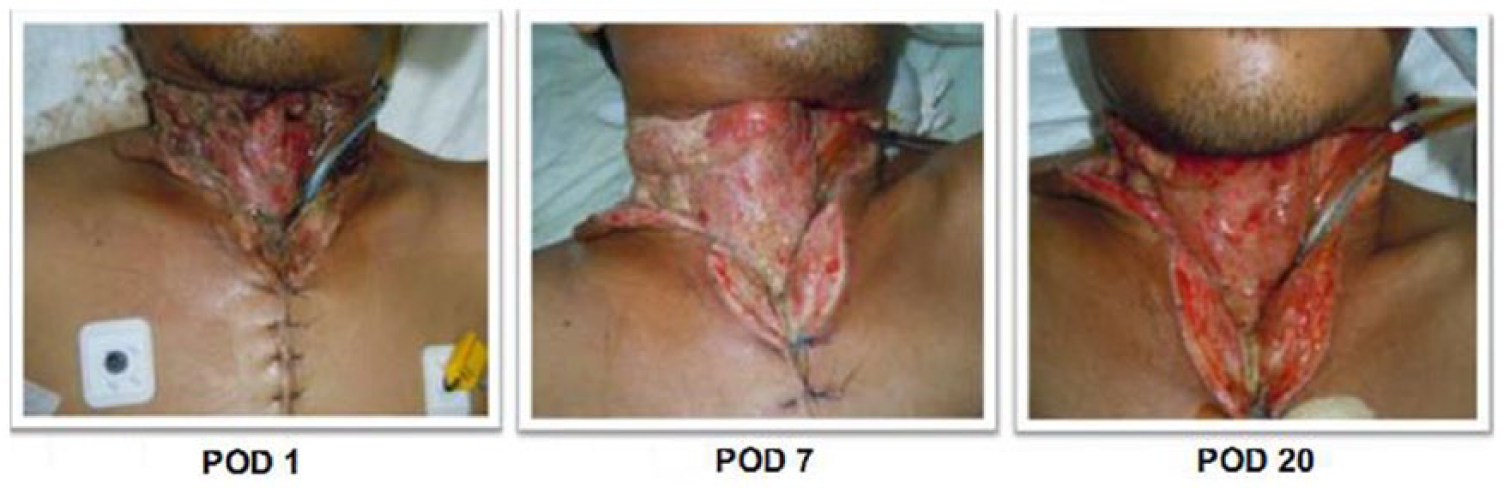
Post-operative wound care by secondary intention. This figure shows the gradual progress of a patient from post-operative date (POD) 1, 7, and 20.
A total of three cases needed to undergo reoperation due to the re-accumulation of pus. Mortality was found in three of our patients (20%). Two of these patients came with a late presentation and severe preoperative sepsis, and the other was reported having intraoperative rupture of the subclavian artery.
Discussion
DNM resulted from the downward spreading of deep cervical infection. To understand the pathways of propagation, symptoms, and thoracic complication of cervical infections, it is essential for a clinician to have a detailed knowledge of the cervical fascial planes.
There are three layers of deep cervical fascia: the superficial layer (pretracheal), visceral layer, and prevertebral layer, all of which partition the deep cervical region into three main spaces: pretracheal, perivascular, and retrovisceral or prevertebral space. Each of these spaces communicates with the mediastinum (Figure 2).
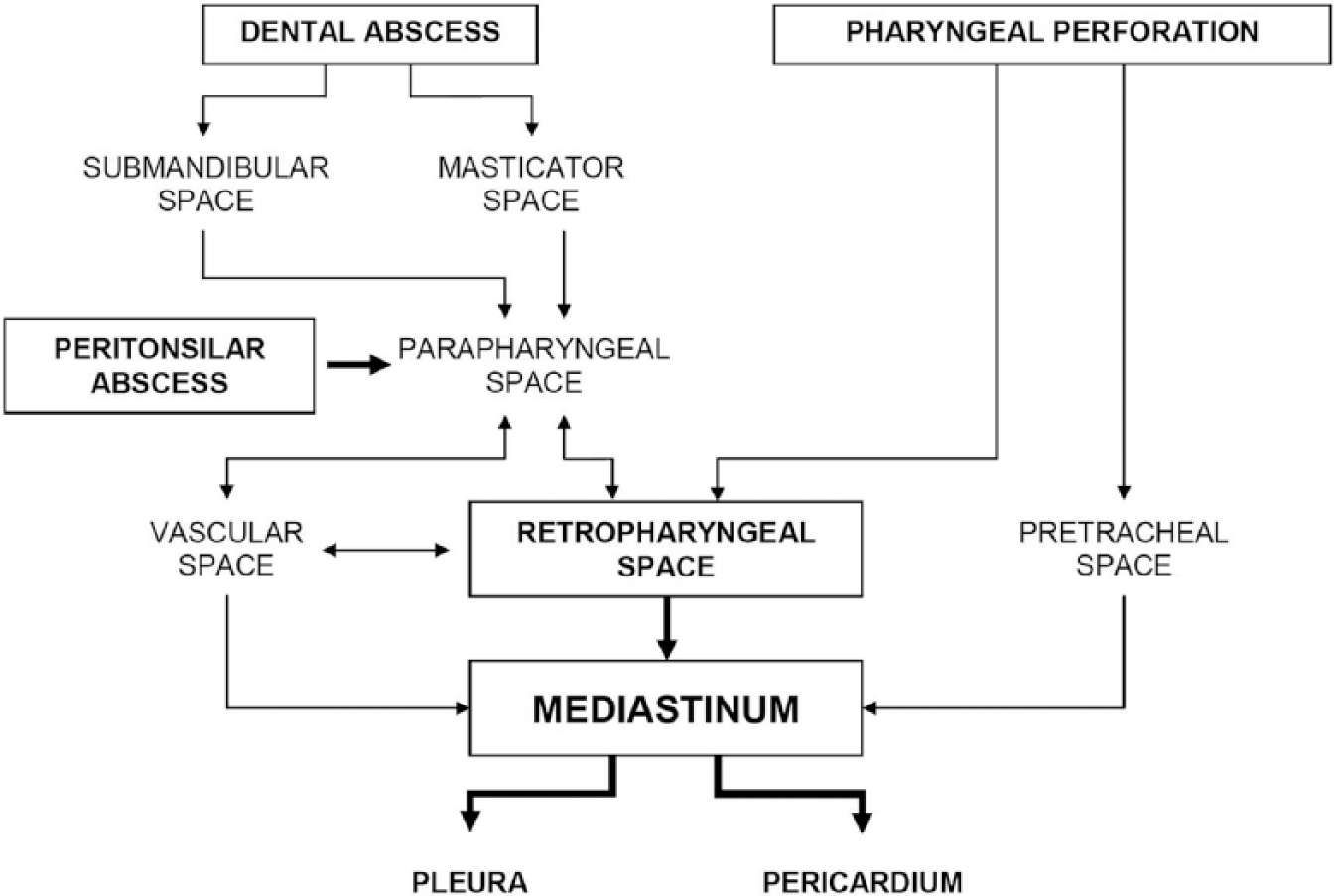
Communication pathways of oropharyngeal infections into the mediastinum. 11
This subset of mediastinitis frequently has a rapid course. Patients who suffer from DNM can suddenly progress to sepsis and death. The rapid caudal spread of cervical infection in DNM is facilitated by gravity, respiration, and the negative intrathoracic pressure. 11 Approximately, 8% of mediastinitis originated from the deep neck infection spread through the pretracheal space; more than 70% of spread occurs via the retrovisceral space, while the remainder cases occurs through the perivascular space. The absence of barriers in the fascial planes, microbial gas formations, and tissue necrosis further speed up the spreading of the deep neck infection.2,14
Soft-tissue infection in DNM is primarily caused by β-hemolytic group A Streptococcus strains. These strains produced a trypsin-like protease which might interfere with immune response at the site of infection. Majority of cases are frequently mixed polymicrobial aerobic and anaerobic bacteria. In the beginning of the process, aerobic bacteria are prominent. Gaining access to soft tissues of the neck changes the tissue redox potential creating an environment suitable for anaerobic bacteria to flourish. 15 This combination is lethal. Anaerobes possess a high affinity to the lipid parts of cellular membranes, causing the muscle cells, erythrocytes, and platelets to be hydrolyzed. Even with a rapid intravenous administration of broad-spectrum antimicrobial agents, death is likely without immediate and comprehensive surgical treatment. Therefore, in many of the cases, adequate surgical drainage of the cervical and mediastinal collections, complete debridement, and excision of necrotic tissue are compulsory.
Other factors contributing to the poor outcome of DNM are diagnostic delays and inadequate initial incision and drainage.5,12 The cervical involvement of DNM is relatively easy to be recognized from the obvious clinical features such as edema, erythema, and tenderness around the neck region. Along with these signs, patients often suffer from neck pain and dysphagia. Unfortunately, a prompt recognition of the mediastinal involvement and DNM can be challenging for the unclear symptoms and signs. In many of the cases, infection is clinically silent and symptoms may be masked by the use of analgesics. The deprived recognition and a tardy diagnosis are the main culprits for suboptimal surgical management of DNM, causing the disease to rapidly progress into fatal systemic sepsis. 11
The anatomical involvement and the onset of medical and surgical treatment of mediastinitis greatly affect the prognosis of this disease. From the three attributes of good DNM management, this study focuses on how aggressive surgical approach should be performed in order to obtain an adequate transthoracic control and the use of sternotomy for transthoracic access in draining the mediastinal compartments.
Surgical approach
As discussed earlier, a number of authors recommend a selective approach of transthoracic incision in surgical drainage of the chest.5,10 These authors advocate the use of transthoracic approach only when there is a necrotizing process below the carina anteriorly and the fourth thoracic vertebra posteriorly as mediastinitis caudal to these levels has been associated with more complication such as increased incidence of pleural empyema. In the absence of the aforementioned findings, these authors opt transcervical drainage of the mediastinum.9,16 Transcervical drainage may be successful in treating patients with DNM if performed without delay. This approach, however, provided only minimal access to the mediastinum; hence, a complete excision of the tissue necrosis will be difficult.
In most of the cases, a prompt recognition of DNM is difficult. Furthermore, DNM is rapidly spreading. In these cases, without an aggressive surgical approach, patients with DNM can suddenly progress to sepsis and death. It is not surprising that many of the other authors recommend mandatory transthoracic mediastinal exploration regardless of the level disease involvement.7,11,12 The proponents of mandatory transthoracic incision also argue that narrow access to the mediastinum while being able to drain does not give complete excision of tissue necrosis. 11 Their claim is further supported by a subsequent meta-analysis by Corsten et al. 8 which concluded that mandatory transthoracic mediastinal exploration resulted in a statistically better prognosis with 81% survival rate compared to 53% with selective approach (p < 0.05). They concluded that the mediastinal collection cannot be adequately drained through a limited subxiphoid or anterior mediastinotomy approach and that early thoracotomy for the best control of mediastinal sepsis is necessary.
Current literature describes several approaches for optimal transthoracic drainage and debridement for DNM patients. Various approaches from clam-shell, subxiphoid, posterolateral thoracotomy, median sternotomy, and thoracoscopic have all been reported with each author citing potential advantages and disadvantages each technique has to offer.9,12,17–19
In this study, median sternotomy approach is used in all our cases. Sternotomy gives a more optimal area for assessment, dilution, and drainage of the mediastinal compartment and both pleura using a single incision. Unfortunately, the possibility of sternal dehiscence and sternal osteomyelitis shuns many surgeons away from using this approach.9,20 This study, however, showed no case of sternal dehiscence and sternal osteomyelitis up until the point of patients’ discharge.
Computed tomography scan
Since the invention of contrast cervicothoracic computed tomography (CT), a number of authors have claimed that the modality leads to improved outcome in DNM cases. This contrast CT helps surgeons to acquire a faster definite diagnosis and more accurately estimate the needs of surgical approach.11,14,21 Contrast-enhanced cervicothoracic CT imaging has been considered as the diagnostic method of choice for patients in whom DNM is suspected. The frequent use of CT imaging for surveillance allows prompt, directed operative drainage, often before the occurrence of clinical signs of deterioration.
Unlike cervical infections, there are no obvious clinical features of mediastinitis or DNM. It is practically harder for physicians to clinically recognize DNM. Furthermore, plain chest X-ray is often non-diagnostic until the patients progress to sepsis. 11
Despite the increased use of CT scan, the mortality reported in DNM cases remained essentially the same. 12 Early comprehensive reviews that recommend CT scan in all DNM patients mostly still have a major question surrounding the adequacy of transcervical mediastinal drainage in this rapidly progressive condition.5,12
The population of DNM patients in our center in general came late compared to normal literature. The delay between onset of primary infection to hospitalization is normally 5–15 days (mean: 8 days),11,21 while in ours it is 3–30 days (mean: 9.4 days).
Therefore, in our center, CT scan is only performed in selective cases. The main reasons are (1) late presentation of cases gives a clearer sign of mediastinal involvement, (2) the speed disease progression in DNM requires emergency debridement, and (3) in our center a clinical triage adapted from Estrera’s classification are enough to predict the involvement of mediastinitis in our group of DNM patients with delay hospital presentation.
Conclusion
Current controversies surrounding the need for sternotomy in DNM management becomes the center focus of this study. We support the use of mandatory transthoracic incision in addition to cervicotomy for a better prognosis and safety profiles.
Our study reported three post-operative mortality cases (20%). Two patients came with preoperative sepsis and was a main risk factor in this series for mortality. One patient had iatrogenic subclavian artery injury. This rate is lower than the previous data by Estrera et al. 5 as well as Freeman 9 which reported a mortality rate of 40% and 29%, respectively. A more selective population of DNM patients that was treated with an aggressive transthoracic incision recorded a mortality rate of around 17%. 11
There is neither sternal dehiscence nor osteomyelitis reported in this study. In our series, the length of hospital discharge in average was 46.7 days compared with other studies that does not use sternotomy in majority of patients.9,11 Our method of post-operative wound care using Indonesian honey is already extensively reviewed in other literatures. 22
We recommend sternotomy to be considered as an approach for surgical debridement in DNM cases. Further study should be done in order to improve the management for DNM patients with late presentation and sepsis. Additionally, mid-term and long-term results of post-sternotomy complication needs to be reported.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
