Abstract
Background:
Aortic dissection requires operation for some reasons.
Methods:
We experienced a case for infected thrombus caused by Escherichia coli in the false lumen of the descending aorta 3 years after ascending aortic replacement for acute aortic dissection.
Results:
A deep sternal wound infection caused by Staphylococcus species after the initial surgery had been successfully treated with both administration of antibiotics for 8 weeks and omental transfer. Replacement of the descending aorta resulted in successful outcomes.
Conclusion:
A thrombosed false lumen with a low blood flow may be vulnerable to bacteremia.
Introduction
Type A acute aortic dissection is treated with ascending aorta replacement with or without aortic arch replacement. An additional operation is required in some patients because of various reasons, such as a dilated false lumen and progressive aortic regurgitation. We experienced an operation case with an infected thrombus in the false lumen 3 years after ascending aortic repair for acute aortic dissection. We got an informed consent from the patient to describing him.
Case
A 61-year-old man presented with fever of unknown origin. He underwent ascending aorta replacement for type A acute aortic dissection 3 years ago. After the operation, he developed infectious mediastinitis caused by Staphylococcus species and was successfully treated with both administration of antibiotics for approximately 8 weeks associated with omental transfer to the mediastinum. He was discharged after the operation and was followed up by his family physician. He had been doing well before this febrile episode.
He visited his family physician, and workup surveys for origin of the fever were scheduled. The first blood culture showed Escherichia coli, and a second blood culture 4 days later was negative for bacteria. Chest computed tomography (CT) after 10-day antibiotic treatment showed an enlargement of the descending aorta without any interval changes around the replaced prosthetic vessel of the ascending aorta (Figure 1(a) and (b)). He was then transferred to our hospital for treatment of the dilated aorta.
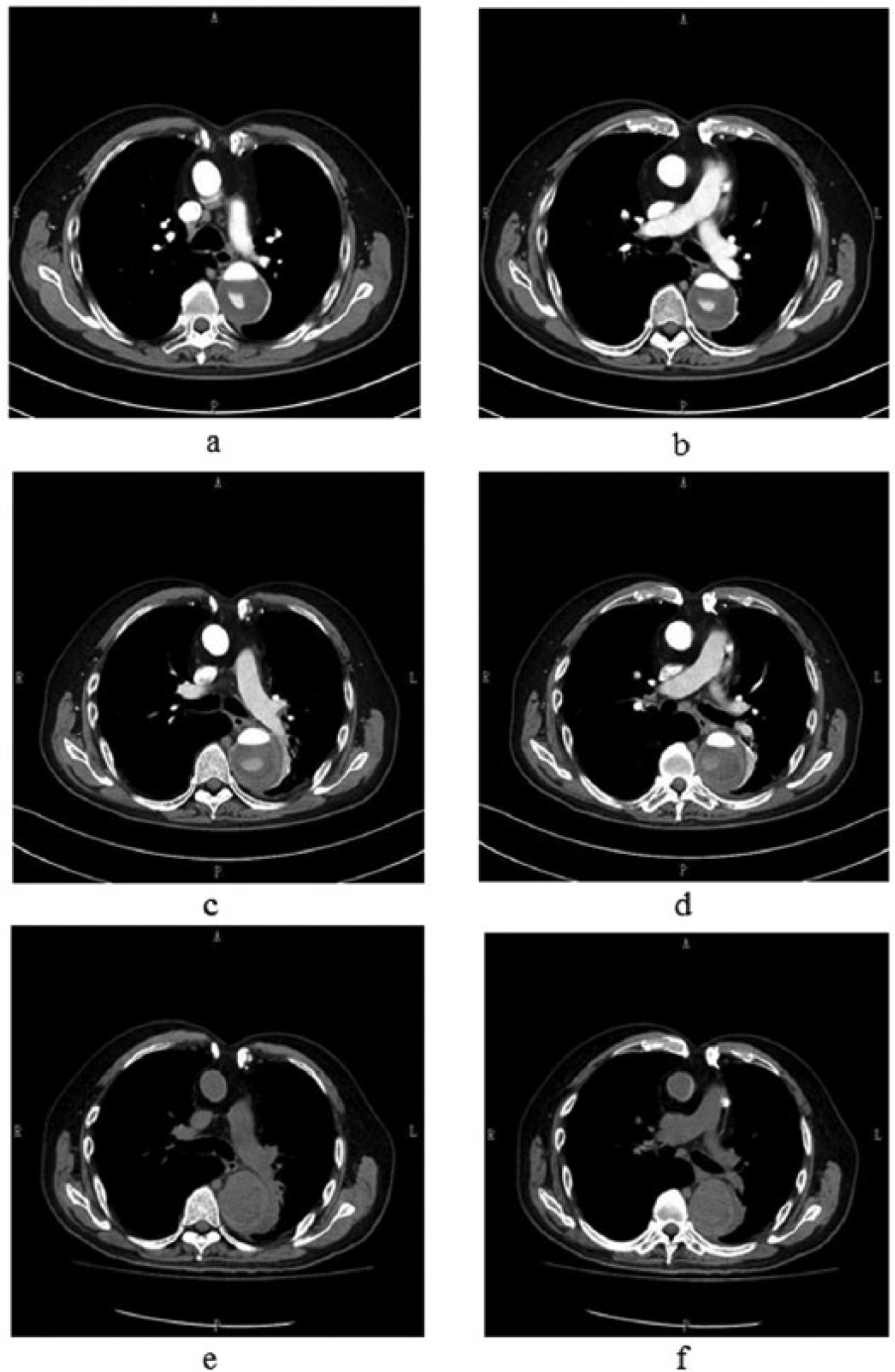
Serial preoperative chest CT findings: (a) and (b) initial CT after a febrile episode. Enlargement of the distal aortic arch compared with CT findings after the initial operation can be seen; (c) and (d) CT 10 days after the antibiotic treatment. A further enlarged false lumen with thrombus and periaortic soft tissue mass swelling with a small amount of left pleural effusion can be seen; (e) and (f) CT 12 days after the antibiotic treatment. The false lumen of the descending aorta becomes more enlarged, and a change in shape associated with increased periaortic soft tissue mass swelling is observed.
Compared with a chest CT 1 year after the initial operation, a chest CT on admission showed an enlarged descending aorta with thrombus in the false lumen and periaortic soft tissue mass swelling with a small amount of left pleural effusion (Figure 1(c) and (d)). A chest CT, 2 days after admission showed that the false lumen of the descending aorta was enlarged, and the change in shape was associated with increased periaortic soft tissue mass swelling (Figure 1(e) and (f)). No abnormal findings around the prosthesis of the ascending aorta were also observed. We speculated that elevated aminotransferase levels were caused by antibiotic administration, and we changed the type of antibiotic while observing the liver function. An infected false lumen was strongly suspected. He gave informed consent for repair of the dilated aorta.
The descending aorta was successfully replaced with a prosthetic vessel via the standard left postero-lateral thoracotomy and under cardiopulmonary bypass. The left femoral artery and vein were cannulated for the establishment of partial cardiopulmonary bypass. A proximal cross-clamp was placed between the left common carotid and subclavian arteries. The segmental cross-clamp method was used for grafting of the descending aorta, and the distal end anastomosis was completed by a double-barrel procedure. The descending aorta including the false lumen was resected as long as possible, and a rifampicin-soaked prosthetic vessel was implanted. A small amount of dark yellow liquid was observed in the false lumen with thrombus.
Specimens acquired during operation were microbiologically negative. The patient’s postoperative course was uneventful. Postoperative 6-week intravenous administration of antibiotics was followed by oral intake of antibiotics for life.
Discussion
Ascending aorta replacement is widely chosen as an initial operation for acute type A aortic dissection. Reoperation after the initial operation for the aortic dissection is required mainly for enlargement of the distal aorta, progressive aortic valve regurgitation, pseudoaneurysm at the aortic graft anastomosis, and graft infection.1,2 Risk factors for the reoperation after the initial repairs include the use of gelatin–resorcinol–formaldehyde glue, nonreplacement of the aortic root, a patent false lumen, and an unresected intimal tear. 2
Infected thrombus in the false lumen requiring an operation has rarely been reported. Matsubayashi and colleagues 3 reported a 68-year-old man with chronic DeBakey type II aortic dissection with infected thrombus in the false lumen. Yih Lim and colleagues 4 also reported similar cases of chronic type A aortic dissection.
The serial changes in chest CT findings led to the diagnosis of infected aortitis of the dissected descending aorta. Microbiological evidence is desirable, but it is not essential for the diagnosis of infective aortitis. Huang and colleagues 5 described in detail about CT imaging of vascular infection as follows. Generally, a saccular-shaped change in the aortic wall with associated periaortic soft tissue mass, inflammation/edema, or abscess is an important CT finding of an infected aorta. An equally important CT feature of mycotic aortic change is a rapid change in size or shape of the aorta on follow-up CT studies. Periaortic gas is also a helpful indication for an infected aneurysm. Rapid enlargement of the false lumen with periaortic mass swelling was important in our patient for the diagnosis of infected aortitis.
In our case, Staphylococcus species was proven as the cause of the mediastinitis after the first operation. Serial CT finding thereafter denied infection of the replaced ascending aorta. Preoperative blood culture showed initially Escherichia coli for the febrile episode, but thrombus cultures were negative for bacteria. Different organisms were detected in our case. Thus, it is not unclear whether the preceding mediastinitis caused the thrombus infection or not. A thrombosed false lumen with a low blood flow may be vulnerable to bacteremia.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
