Abstract
Background
Adverse childhood experiences are demonstrated risk factors for depression, a common co-morbidity of multiple sclerosis, but are understudied among people with multiple sclerosis.
Objective
Estimate the association between adverse childhood experiences and depression among 1,990 adults with multiple sclerosis.
Methods
Participants were members of Kaiser Permanente Northern California from two studies between 2006 and 2021 and were diagnosed with multiple sclerosis by a neurologist. Adverse childhood experiences were assessed using two instruments, including the Behavioral Risk Factor Surveillance System. Participants self-reported ever experiencing a major depressive episode. Meta-analysis random effects models and logistic regression were used to estimate odds ratios (ORs) and 95% confidence intervals (CIs) to assess the relationship between adverse childhood experiences and a history of depression across study samples. Adverse childhood experiences were expressed as any/none, individual events, and counts. Models adjusted for sex, birth year, race, and ethnicity.
Results
Exposure to any adverse childhood experiences increased the odds of depression in people with multiple sclerosis (OR: 1.71, 95% CI: 1.21–2.42). Several individual adverse childhood experiences were also strongly associated with depression, including “significant abuse or neglect” (OR: 2.79, 95% CI: 2.11–3.68).
Conclusion
Findings suggest that adverse childhood experiences are associated with depression among people with multiple sclerosis. Screening for depression should be done regularly, especially among people with multiple sclerosis with a history of adverse childhood experiences.
Keywords
Introduction
Depression is one of the strongest predictors of quality of life and worse disability among people with multiple sclerosis (PwMS).1,2 It is associated with multiple sclerosis (MS) outcomes such as greater accumulation of physical disability, cognitive dysfunction, worse self-care, and fatigue.1–3 Additionally, PwMS and depression are likely to require more hospital services, rehabilitation, and informal care from supporting family members than those without depression. 3 The lifetime prevalence of depression among PwMS is estimated to be 37%–54%, which is higher than the general population's (∼ 18%).3–5 Diagnosing depression among PwMS is challenging given the overlap in disease characteristics, such as changes in sleep, appetite, memory, and fatigue.1,6 Importantly, evidence suggests that depression is underdiagnosed and undertreated in PwMS.1,4,6,7
Childhood trauma, defined as notable distress or maltreatment, can increase the risk of developing a lifetime diagnosis of depression.8–10 Childhood maltreatment is common among PwMS; 24%–64% of PwMS self-report at least one form of childhood trauma in recent observational studies.11–13 However, there is limited research on the impact of childhood trauma on depression among PwMS. Childhood trauma can be assessed by adverse childhood experiences (ACEs), potentially traumatic events occurring before the age of 18 years including abuse, neglect, and household dysfunction.8,14 Studies in the general population have identified individual ACEs associated with an increased risk of depression, such as abuse (emotional, sexual, and physical), neglect, and domestic violence. A dose–response relationship was also identified between cumulative ACEs and the risk of depression.9,15–17
To date, investigations of the relationship between ACEs and depression in PwMS have been inconsistent. A cross-sectional study including 232 Canadian PwMS found that emotional abuse was the only ACE associated with psychiatric comorbidity. 11 In contrast, a study with 192 Canadians with MS reported that sexual abuse was associated with depression. 18 Similarly conflicting results exist for ACE scores. The aforementioned cross-sectional study identified a graded relationship between ACE scores and depression, but a study with 31 PwMS reported insignificant associations between depression and 0–3 ACEs.11,19 Inconsistencies may be attributed to the limitations of small sample sizes and non-standard collection of ACE data. Understanding these relationships could improve diagnostic screening and treatment outcomes for depression in PwMS.
This study's objective was to estimate the magnitude of association, if any, between ACEs and a history of depression among 1,990 adults with MS by testing the effect of individual and cumulative ACEs on depression. We hypothesized that, among PwMS, ACEs would be associated with increased odds of having a history of depression.
Methods
Study population
Adults with MS were identified among members of Kaiser Permanente Northern California (KPNC) through electronic health records (EHR) as any person aged 18–69 years with at least one outpatient diagnosis of MS (ICD9 code 340.x) by a neurologist at the time of recruitment. KPNC members account for 25% of the service area's population and are generally representative of the region's population. 20 Participants from two different research studies under the KPNC MS Research Program (MSRP) were included in this analysis, which we refer to as “Study 1” and “Study 2.” Study 1 recruited PwMS between 2006 and 2014 for a large genome-wide and environment case-control study. To achieve sufficient statistical power for those original genetic analyses, the sample was mostly limited to the largest single racial group within KPNC, non-Hispanic Whites. Full recruitment details are available elsewhere. 21 Study 2 recruited PwMS between 2019 and 2021 to investigate MS outcomes across a racially and ethnically diverse sample. Recruitment procedures were the same as in KPNC MSRP Study 1, except without limitations on race or ethnicity. Participants from both KPNC MSRP studies were included in the analysis if MS onset occurred after the age of 10 years. This criterion was set to exclude individuals with onset of MS before or during exposure to early life ACEs as defined in this study. Age at MS diagnosis was determined using comprehensive interview data.
The study protocol was approved by the Institutional Review Boards of UC Berkeley and the Kaiser Permanente Division of Research. Informed consent was obtained for all study participants.
Exposure: Early life ACEs
Study participants from both studies were administered a comprehensive computer-assisted telephone interview (CATI) by trained staff at study entry. The CATI consisted of self-reported demographic, clinical, environmental, and lifestyle questions. Details are described elsewhere. 21 The CATI ACE survey included nine ACE events (yes/no) during ages 0–10 years which were adapted from Coddington's Life Event Record. 22 These items were parent or sibling death, parental divorce/separation, parental remarriage, foster care placement (or late adoption), lived with extended family, the life-threatening illness of parent or sibling (including psychiatric illness or substance abuse), significant verbal or physical abuse or neglect, the family lost home or had to move, and violent crime victim. We refer to these as “CATI ACEs.”
Several questions and assessments were updated in the CATI before the start of Study 2. Consequently, participants in Study 2 were administered the Behavioral Risk Factor Surveillance System (BRFSS) ACE survey in addition to the original CATI ACE survey. 23 The BRFSS ACE items include physical abuse, sexual abuse, emotional abuse, mental illness in the household, substance abuse in the household, intimate partner violence in the household, parental divorce/separation, and incarcerated household member(s). For this analysis, items were treated as yes/no during ages 0–18 years. We refer to these as “BRFSS ACEs.”
Outcome: History of depression (ever/never)
The CATI included questions on symptoms of depression. 24 For analysis, symptoms were organized into DSM-5 diagnostic criteria categories: depressed mood (or irritability), anhedonia, appetite or weight changes, sleep difficulties, psychomotor changes, fatigue, diminished concentration, feelings of worthlessness/guilt, and suicidality. 25 History of depression was classified as “ever” if the participant indicated experiencing at least two weeks characterized by a depressed mood or anhedonia and at least four other depressive symptoms during that period. Participants were also classified as “ever” having depression if they indicated feeling bothered/irritable or anxious and at least five other depressive symptoms for a period of at least 2 weeks.
Covariates
Participants’ sex, birth year, race, and Hispanic ethnicity were included as covariates in this analysis. Race was categorized as White or non-White in Study 1, where 97% of the non-White group identified as African American/Black. In Study 2, race was categorized as African American/Black, American Indian/Alaskan Native, Asian/Pacific Islander, or White. Race and Hispanic ethnicity were controlled to account for the different selection criteria in the KPNC MSRP studies.
Statistical analysis
Logistic regression was used to estimate odds ratios (ORs) with 95% confidence intervals (CIs) for a history of depression according to exposure to CATI ACEs. In separate models, CATI ACEs were expressed as (a) any/none; (b) individual events (yes/no); (c) scores 0, 1, 2, 3, or 4 +; or d) continuous count. The associations between individual ACEs and a history of depression were not estimated for rare ACEs (< 3% prevalence in the sample). Due to sample differences, ORs were estimated separately for Study 1 and Study 2. Models for Study 1 adjusted for race as a binary variable while models for Study 2 adjusted for race as a four-level categorical variable plus a covariate for Hispanic ethnicity. All models adjusted for sex and birth year. Results were averaged across studies using meta-analysis random effects statistical models. 26 The random-effects model accounts for effect heterogeneity between studies by applying random-effect weights to each estimate when pooling results. This is necessary to account for the differences in study populations which may create a variance in effect sizes that cannot be attributed to sampling error alone. False discovery rate (FDR) was used to correct for multiple testing across all meta-analysis random effects models. 27 After adjustments, FDR q values < 0.05 were considered statistically significant.
In a secondary analysis, we sought to identify consistencies in findings from CATI ACEs and BRFSS ACEs. Logistic regression models estimated ORs with 95% CIs for history of depression given exposure to BRFSS ACEs in Study 2 (not available for Study 1). In separate models, BRFSS ACEs were expressed as (a) any/none; (b) individual events (yes/no); (c) scores 0, 1, 2, 3, or 4 +; or (d) continuous count. These models adjusted for sex, birth year, race, and Hispanic ethnicity. We estimated the correlation between CATI ACE counts and BRFSS ACE counts using the Pearson correlation coefficient. All analyses were performed using R Version 4.0.2. 28
Results
Demographic characteristics are shown in Table 1. Overall, the mean age of participants was 47.5 years (SD 9.9) at the time of the interview. The sample was 77.4% female. More than three-fourths of the participants identified as White (83.4%), with African American/Black being the second largest racial subgroup (9.4%). There were clear differences between the two studies regarding age, birth year, race, ethnicity, and age at MS onset. Notably, Study 2 had higher proportions of American Indian/Alaska Native, Asian/Pacific Islander, and Hispanic participants. On average, participants in Study 2 were nearly nine years younger and born two decades later than those in Study 1. Overall, 38.8% of participants reported a history of depression. Depression was more prevalent among participants in Study 2 compared to Study 1 (56.1% and 32.8%, respectively), as well as in American Indian/Alaskan Natives (58.7%) and Asian/Pacific Islanders (51.1%) (Supplemental Table 1). More than half of the Hispanic PwMS reported a history of depression (52.6%).
Baseline characteristics of people with MS (n = 1990) in the Kaiser Permanente Northern California MS Research Program (2006–2021), stratified by study.
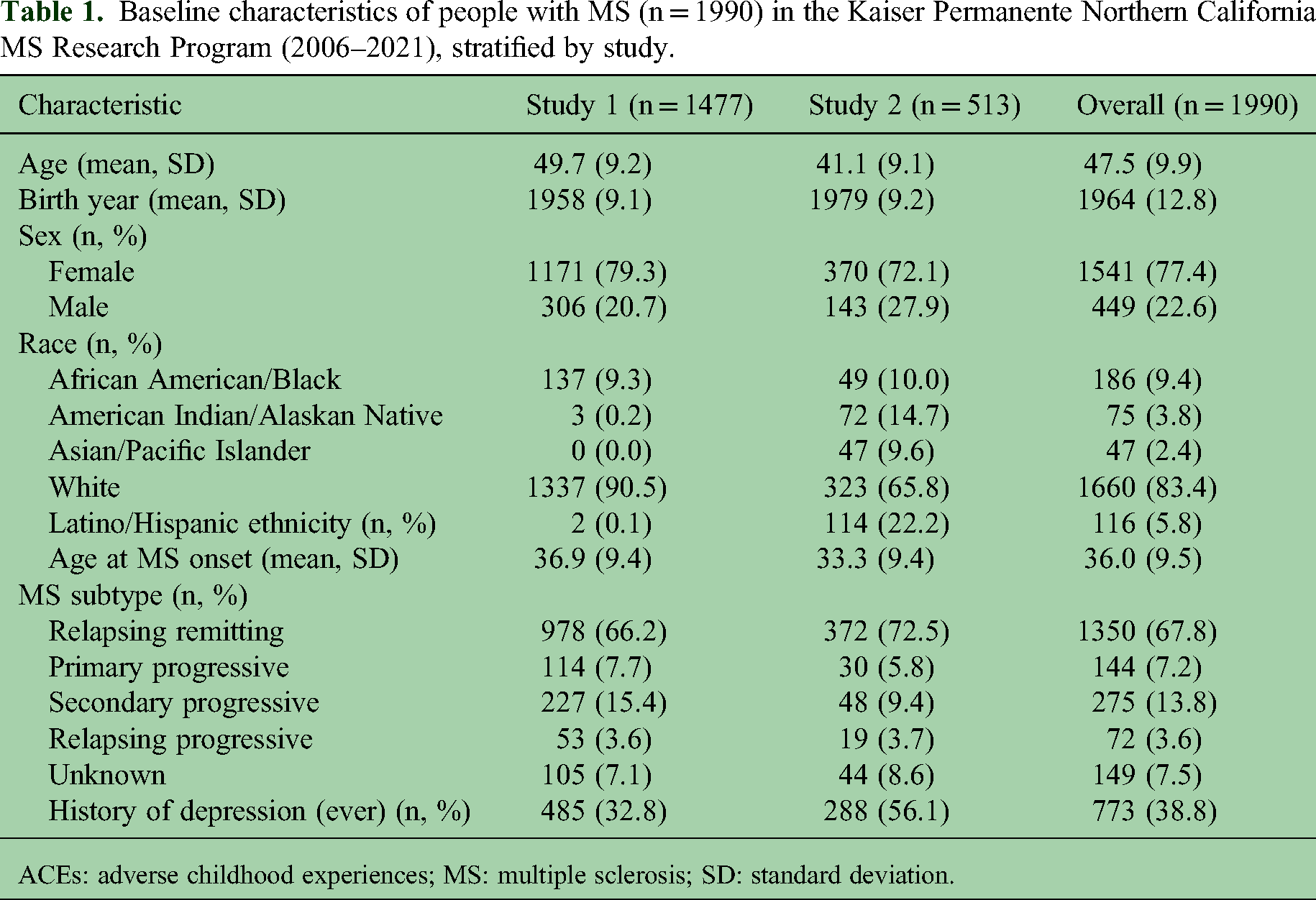
ACEs: adverse childhood experiences; MS: multiple sclerosis; SD: standard deviation.
Overall, 40.8% of participants reported experiencing any CATI ACEs between the ages of 0–10 years (Table 2). The most common CATI ACEs were “serious illness of a parent or sibling” (14.8%) and “significant verbal or physical abuse or neglect” (13.7%). Participants in Study 2 consistently reported a higher prevalence of CATI ACEs than those in Study 1 for all ACEs, except for “death of a parent or sibling.” Across both studies and surveys, participants with a history of depression generally reported ACEs more frequently than those without (CATI, BRFSS). Notably, CATI ACE “significant verbal or physical abuse, or neglect” was reported more than twice as often among those with a history of depression. Over three times as many participants reported experiencing 4 + ACEs on the BRFSS survey compared to the CATI survey (23.0% vs. 7.4%, respectively) in Study 2.
Distribution of ACEs from the CATI and BRFSS surveys among people with MS, stratified by study and history of depression.

ACEs: adverse childhood experiences; BRFSS: Behavioral Risk Factor Surveillance System; CATI: computer-assisted telephone interview; MS: multiple sclerosis; SD: standard deviation.
Results of random-effects meta-analysis showed that participants who reported any CATI ACEs between ages 0–10 years had increased odds of having a history of depression compared to those who experienced no ACEs (OR: 1.71, 95% CI: 1.21–2.42) (Table 3). Several CATI ACEs were significantly associated with a history of depression: “significant verbal/physical abuse or neglect” (OR: 2.79, 95% CI: 2.11–3.68), “victim of a violent crime” (OR: 2.08, 95% CI: 1.22–3.56), “family lost their home or had to move” (OR: 2.02, 95% CI: 1.47–2.76), and “serious (life-threatening) illness of parent or sibling (including psychiatric illness or substance abuse problem)” (OR:1.56, 95% CI: 1.20–2.04). CATI ACE scores of 2, 3, or 4 + (vs. 0) were all statistically significant after FDR adjustment and demonstrated a dose–response trend (p < 0.001). When expressed continuously, each additional CATI ACE count was associated with increased odds of depression (OR: 1.28, 95% CI: 1.17–1.39).
Associations between CATI ACEs and history of depression among people with MS, stratified by study.

All models adjusted for birth year and sex. Study 1 adjusted for race as a binary variable. Study 2 adjusted for race as a 4-level categorical variable and included a covariate to account for Hispanic ethnicity. ORs for individual events that were rare (< 3%) were not included in individual ACE analysis.
ACEs: adverse childhood experiences; CI: confidence interval; FDR: false discovery rate; MS: multiple sclerosis; OR: odds ratio; CATI: computer-assisted telephone interview.
“death of a parent or sibling” and “foster care or late adoption” were excluded from individual ACE analysis due to the rarity of the event (< 3% prevalence).
Several BRFSS ACEs were strongly associated with depression: “mental illness in the household” (OR: 3.25, 95% CI: 2.14–5.01), “incarcerated household member” (OR: 2.86, 95% CI: 1.43–6.28), “emotional abuse” (OR: 2.85, 95% CI: 1.94–4.22), “physical abuse” (OR: 2.20, 95% CI: 1.37–3.61), and “sexual abuse” (OR: 1.86, 95% CI: 1.13–3.14) (Table 4). Continuous BRFSS ACE counts and ACE scores were also associated with increased odds of depression. ACE counts from the CATI and BRFSS survey responses in Study 2 were moderately correlated (Pearson correlation coefficient = 0.52, p-value <0.001) (Supplemental Figure 1).
Associations between BRFSS ACEs and history of depression among people with MS in Study 2 (n = 513) of the KPNC MS Research Program (2019–2021).

All models adjusted for birth year, sex, race as a 4-level categorical variable, and Hispanic ethnicity.
ACEs: adverse childhood experiences; BRFSS: Behavioral Risk Factor Surveillance System; CI: confidence interval; KPNC: Kaiser Permanente Northern California; MS: multiple sclerosis; OR: odds ratio.
Discussion
The goal of this study was to examine the association between ACEs and a history of depression among PwMS using multiple measures of ACEs. Our results showed that ACEs were strongly associated with increased odds of depression among PwMS. Several individual ACEs more than doubled the odds of depression among PwMS, including abuse or neglect, family losing home/moving, and being a victim of a violent crime. Moreover, our results demonstrated a strong dose–response relationship between an increasing number of ACEs and the odds of depression. We found that a history of depression was high among PwMS (39% of the total sample), as was the prevalence of ACEs (1 + CATI ACE: 41% of the total sample; 1 + BRFSS ACE: 69% of Study 2). Consequently, depression should be regularly screened for in PwMS, especially among those with a history of ACEs.
Individual CATI ACEs during ages 0–10 years demonstrated varying strengths of association with a history of depression. Primary results suggest that exposure to emotional or physical abuse or neglect had the strongest effect on the prevalence of depression. This agrees with the results from studies in the MS and general populations which found that emotional abuse had the strongest association with depression.11,15,29 Being a victim of a violent crime or losing a home more than doubled the odds of depression in our study. This aligns with previous studies in the general population that identified income hardships and proximal violence as depression risk factors.15,18 Our null finding for “parental divorce or separation” differed from others which found it increased the risk of depression. 16
Recognizing the burden of experiencing several types of childhood trauma is important. Our findings suggest that PwMS are commonly exposed to multiple ACEs, with nearly 20% of the total sample reporting two or more CATI ACEs, and 50% of Study 2 reporting two or more BRFSS ACEs. Results from both ACE surveys (CATI and BRFSS) demonstrated a dose–response relationship between increasing ACEs and odds of depression among PwMS. This relationship is most obvious in the BRFSS ACE scores where four or more ACEs quadrupled the odds of depression compared to fewer ACEs. These findings agree with several previous studies that show accumulating exposure to ACEs is associated with higher depression prevalence.8,10,11,16 These findings are striking given their consistency across KPNC MSRP studies, even when considering different ACE assessments, exposure windows, and possible cultural norms surrounding experiencing ACEs and reporting of depression.
Critically, we observed that the burden of ACEs and depression varied across race and ethnicity. A BRFSS study with 214,157 respondents found that exposure to ACEs was highest among multiracial, Hispanic, and African American/Black individuals (respective mean ACE counts: 2.52, 1.80, and 1.69). 30 The CDC similarly reports varying prevalences of depression across demographics, with men and non-Hispanic Asians reporting significantly lower frequencies than other groups. 31 These findings suggest that women and certain racial groups may be disproportionately burdened with exposure to ACEs, depression, and MS. Our analysis lacked sufficient statistical power to assess the association between ACEs and depression among different racial and ethnic groups of PwMS, which is a limitation of this article. Future studies should aim to explore this relationship across demographics to understand the effects of cumulative adversity on PwMS through culturally sensitive perspectives of trauma.
To date, the relationship between ACEs and the onset of MS is unclear. A Norwegian prospective study including 77,997 women found that the risk of MS was increased if women were exposed to abuse as a child. 12 Interestingly, a previous study using MS cases and controls from Study 1 did not find an association between ACEs (individual or cumulative) and the risk of MS. 32 This suggests that the effect of ACEs on depression among PwMS in this analysis is not simply because of confounding between MS, ACEs, and depression, as is possible in case-only studies. Our results indicate there may be an independent effect of ACEs on depression within PwMS. The biological and psychosocial pathways contributing to this mechanism should be investigated further.
This study had several strengths. Since participants in Study 2 received both ACE surveys (CATI and BRFSS), we compared the CATI ACE survey results with those from a standardized instrument. Although the CATI and BRFSS ACE surveys notably differ, we did not observe contradicting results when both surveys were administered to the same sample. This improves our confidence in the CATI's ability to estimate the relationship between ACEs and a history of depression. Additionally, Study 2 appreciably increased the representation of racially and ethnically diverse PwMS. This is particularly important for the assessment of ACEs and depression given the varying prevalences of both variables across race and ethnic groups.30,31
This study had several limitations. Reporting of ACEs is vulnerable to inaccurate recall as participants may not remember exposure to ACEs or may only remember the most traumatic type of ACEs, thus under-reporting. Additionally, all ACE items were binary (yes/no) which does not consider the duration, frequency, or intensity of the exposure. This limits our ability to thoroughly study the cumulative effects of ACEs. Similarly vulnerable to poor recall, a history of depression was measured using self-reported data. However, the lifetime prevalence of depression in our study was like those reported in other MS studies, reducing the concern for bias.1,3,4,7 We were also unable to determine the onset of the first depressive episode, so establishing the temporality of depression and MS diagnosis was not possible. Future work should determine whether the effects of ACEs on depression are specific to pre- or post-MS diagnosis depression, which could either represent the MS prodrome or a period before underlying MS biological processes start occurring.33,34 Despite these limitations, our findings were consistent with the findings of most prior studies on the effects of ACEs in the general population.
In summary, our findings suggest that experiencing multiple forms of adversity or notable abuse during childhood can have long-term consequences for PwMS. We observed a high prevalence of ACEs and depression among PwMS. Therefore, caregivers and clinicians should not only screen for depression but also consider a patient's history of ACEs. This awareness can help guide trauma-informed care, improving patient outcomes. 11 Our results underscore the importance of early diagnosis and treatment of depression among PwMS, as this may mitigate the negative impact on their quality of life. Future studies should thoroughly examine the relationship between ACEs and depression among PwMS. These investigations should explore how ACEs interact with MS symptoms to modify the risk of depression. Furthermore, it is essential to examine how these relationships vary among diverse populations.
Supplemental Material
sj-pdf-1-mso-10.1177_20552173231202638 - Supplemental material for Adverse childhood experiences in early life increase the odds of depression among adults with multiple sclerosis
Supplemental material, sj-pdf-1-mso-10.1177_20552173231202638 for Adverse childhood experiences in early life increase the odds of depression among adults with multiple sclerosis by Karla S Guerrero, Mary K Horton, Vidhu Choudhary, Kalliope H Bellesis, Pete Dorin, Jin Mei, Terrence Chinn, Travis J Meyers, Catherine A Schaefer and Lisa F Barcellos in Multiple Sclerosis Journal – Experimental, Translational and Clinical
Supplemental Material
sj-docx-2-mso-10.1177_20552173231202638 - Supplemental material for Adverse childhood experiences in early life increase the odds of depression among adults with multiple sclerosis
Supplemental material, sj-docx-2-mso-10.1177_20552173231202638 for Adverse childhood experiences in early life increase the odds of depression among adults with multiple sclerosis by Karla S Guerrero, Mary K Horton, Vidhu Choudhary, Kalliope H Bellesis, Pete Dorin, Jin Mei, Terrence Chinn, Travis J Meyers, Catherine A Schaefer and Lisa F Barcellos in Multiple Sclerosis Journal – Experimental, Translational and Clinical
Footnotes
Acknowledgements
We thank all members and staff of the Kaiser Permanente Division of Research and the University of California, Berkeley, Genetic Epidemiology and Genomics Laboratory.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute of Neurological Disorders and Stroke [grant numbers R01 NS 049510 to L.F.B. and F31 NS 108668 to M.K.H.] (https://www.ninds.nih.gov/); the National Institute of Allergy and Infectious Diseases [grant number R01 AI 076544 to L.F.B.] (https://www.niaid.nih.gov/); the National Institute of Environmental Health Sciences [grant number R01 ES 017080 to L.F.B.] (https://www.niehs.nih.gov/); and the National Institute of Nursing Research [grant number NR 017431 to L.F.B.] (![]() ). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
