Abstract
Objective
This study explores how AI-powered consultation services in internet hospitals influence patient satisfaction through perceived value and emotions. A dual-path analytical framework was developed: the technical path uses the E-S-QUAL model to assess the quality of intelligent consultation guidance services in terms of efficiency, system availability, privacy, and fulfillment; the experiential path is based on the Patient Experience-Driven Model, which integrates service encounter theory (focusing on patient-system interactions) and the Stimulus–Organism–Response theory (explaining how external stimuli trigger psychological and behavioral responses).
Methods
The dual-path framework includes two submodels. The technical path examines how service quality dimensions affect patient satisfaction through perceived value (i.e., patients’ subjective evaluation of the service's usefulness and reliability). The experiential path investigates how service encounters—including interaction, recommendation, and security—indirectly influence satisfaction via perceived value and patient emotions. A structural equation model was applied to analyze data from 1113 valid survey responses.
Results
Both paths significantly influenced satisfaction. Fulfillment and privacy had the most significant effects in the technical path. In the experiential path, service encounters impacted satisfaction through perceived value and emotions. Emotions acted as psychological amplifiers, with positive emotions enhancing the positive effect of perceived value on satisfaction, while negative emotions weakened this effect. Notably, service encounters suppressed negative emotions more strongly than they enhanced positive ones.
Conclusions
This study clarifies the dual role of technical service quality and emotional experience in shaping patient satisfaction, providing theoretical and practical insights for optimizing AI-powered healthcare consultations.
Keywords
Introduction
The rapid advancements in mobile internet and IoT technologies have significantly transformed the healthcare sector. As an innovative healthcare service model under the “Internet Plus” initiative, internet hospitals not only expand the boundaries of medical services and address the issues of high medical costs and difficult access to medical services but also achieve cost optimization and resource integration through technological innovation and the restructuring of service delivery models. For example, the “Yi Zhan Deng” Internet Hospital reduced the overall cost per medical consultation by 40% through remote follow-up services. 1 The Internet Hospital of the Second Hospital of Lanzhou University has provided over 92,974 online outpatient visits, 2 offering services such as online consultation, diagnosis, and medication purchase, which not only enhance patient convenience but also reduce the operational costs of physical hospitals. Consequently, actively developing internet hospitals has become a key priority for advancing digital society construction during China's 14th Five-Year Plan period. 3
The existing research on Internet hospital focuses on three aspects: medical service capacity, system optimization, and service system construction. In terms of healthcare service capacity, scholars have confirmed that internet hospitals significantly enhance the accessibility of medical resources through innovative service models such as telemedicine collaboration, 4 AI-powered triage and patient routing, 5 and full-cycle care management 6 —particularly demonstrating unique emergency response value during public health crises. Regarding system optimization, researchers have been committed to building integrated online–offline internet hospital platforms with comprehensive functionality.7–9 In terms of service systems construction, existing studies have developed multidimensional evaluation models for internet hospital services. For example, Duan et al. employed the SERVQUAL-IPA model to identify key dimensions such as assurance and empathy that influence patient experience, 10 while Tan et al. proposed the MES model, which evaluates internet medical services based on user engagement, service content, and treatment effectiveness. 11 Although these models have been applied to internet healthcare settings, their emphasized dimensions primarily focus on interpersonal interaction, and do not fully reflect the distinctive technological characteristics of AI-powered online medical services—such as system efficiency, technical stability, privacy protection, and service fulfillment. Unlike traditional service quality (SQ) models (e.g., SERVQUAL, HEALTHQUAL, and Donabedian models), which emphasize interpersonal interaction, physical environments, and clinical outcomes, the E-S-QUAL model is specifically designed for evaluating electronic service contexts. 12 It is more effective in capturing key dimensions of online technological interaction—making it particularly suitable for assessing intelligent consultation guidance services in internet hospitals.
Intelligent consultation guidance services refer to AI-enabled services in internet hospitals that collect and analyze patients’ symptom information through human–computer interaction and provide department recommendations to achieve efficient and accurate preliminary triage. 13 In recent years, with the rapid proliferation of internet hospitals, intelligent consultation guidance services have gradually become the first point of contact for patients seeking online medical care. The quality of these services directly affects patients’ online healthcare experience, and in turn, influences their overall satisfaction and intention to continue using such services. However, most existing studies have remained focused on the technological development and algorithmic innovation of services.14–16 A thorough review of the literature reveals that while some research has explored the application of the Technology Acceptance Model 17 and perceived risk theory 18 in internet-based healthcare services, the underlying mechanism through which AI-powered services influence patient satisfaction (PS), particularly by affecting patients’ psychological perceptions such as perceived value (PV) and patient emotions, has not been thoroughly investigated. This remains a critical “black box” that has yet to be fully understood. In particular, the way in which intelligent consultation guidance SQ impacts PS through PV and emotional experience remains an urgent issue. This question has not received sufficient academic attention or effective solutions in practice.
This study addresses these challenges as follows: (1) Using the E-S-QUAL model and relevant studies, a measurement scale is developed to evaluate intelligent consultation guidance services across four dimensions—efficiency, system availability, privacy, and fulfillment—with PV introduced as a mediating variable to construct the first research framework. (2) This study integrates the E-S-QUAL model with service encounter theory and the Stimulus–Organism–Response (S–O–R) theory to propose a theoretical framework driven by patient experience—the Patient Experience-Driven Model (PEDM). From the patient's perspective, a patient's experience is influenced not only by the technical quality of the service but also by emotional responses and value perceptions. Based on this, PEDM divides the quality of intelligent consultation guidance services into three dimensions: service interaction encounter (SIE), service security encounter (SSE), and service recommendation encounter (SRE). The model explores how these dimensions affect PS by influencing PV and emotions. This constitutes the second research framework of this study. (3) Structural equation modeling (SEM), exploratory factor analysis (EFA), and bootstrap sampling are used to validate the models and hypotheses. (4) Key elements influencing PS are identified, their interrelationships analyzed, and practical recommendations provided.
The study makes four main contributions: (1) Research on the impact of intelligent consultation guidance SQ on PS in the context of internet hospitals is still lacking. This study, based on the E-S-QUAL model, identifies key SQ indicators and innovatively applies them to the internet hospital context, thereby filling the theoretical gap in the field of internet hospital services. (2) By integrating service encounter theory and the SOR framework, it proposes the PEDM, offering new insights into the pathways through which SQ impacts satisfaction. (3) This study integrates the E-S-QUAL model with the PEDM to construct a systematic dual-model research framework. The validation of the dual models enhances the reliability and robustness of the research findings, providing a new methodology for integrating multiple models to study the relationship between SQ and PS. (4) The findings of this study not only deepen the theoretical exploration of intelligent consultation guidance services but also provide management and practical recommendations for optimizing SQ in internet hospitals.
This paper is organized as follows: “Literature review” section reviews and analyzes relevant literature; “Research framework and hypotheses developing” section presents the theoretical framework and research hypotheses; “Methods” section details the research methods; “Results” section presents the research results; and the final discussion provides theoretical and managerial insights, along with a discussion of the study's limitations and directions for future research.
Literature review
Intelligent consultation guidance services
Recent advancements in intelligent consultation guidance services focus on software design and technological innovation. Researchers have enhanced system functionality by aligning hospital workflows with patient needs, utilizing technologies such as knowledge graphs, decision trees, and deep learning. For example, Xu and Jia developed a system incorporating disease self-checks, appointment and registration guidance, medical consultations, and auxiliary diagnosis using knowledge graphs and deep learning. 19 Yuan et al. added mobile voice transcription and star-based recommendations, increasing convenience. 20 Quan et al. employed knowledge graphs and intelligent polling to improve the accuracy of department recommendations. 21 These innovations have established a solid foundation for enhancing SQ.
From an application perspective, intelligent consultation guidance services have significantly improved healthcare service efficiency and patient experience. Deng et al. found that their diverse functionalities enhance PV and strengthen users’ continued usage intentions. 22 Xie et al. observed that these services reduce registration errors and improve PS compared to traditional self-scheduling. 23 During public health emergencies, their 24/7 availability and ability to minimize person-to-person contact alleviate operational pressures on healthcare institutions and lower infection risks. 24
Although existing research has made certain advancements in technological innovation, function optimization, and practical applications, there are still gaps in the literature regarding theoretical development and empirical analysis. First, current studies tend to focus on technical issues such as algorithm optimization, knowledge graph construction, and neural network model design, lacking a systematic evaluation of the overall impact of intelligent consultation guidance SQ on PS from the perspective of patient experience and SQ. Second, the theoretical analysis in existing literature is relatively underdeveloped, and the specific mechanisms by which intelligent consultation guidance SQ influences satisfaction through subjective factors such as PV and emotions have not been thoroughly explored. Third, most existing studies adopt a single theoretical model and lack cross-validation between multiple theoretical perspectives, resulting in fragmented and incomplete research on the evaluation of intelligent consultation guidance SQ.
In summary, significant gaps still exist in both theoretical development and empirical analysis. Further investigation is needed to explore how intelligent consultation guidance SQ influences PS through mechanisms such as PV and emotions.
E-Service quality
With the rapid growth of e-retailing and e-services, scholars and businesses have explored standards for evaluating online SQ, focusing on differences from offline services and methods to measure and improve it. Parasuraman et al. defined e-SQ as a website’s ability to facilitate efficient and effective shopping, purchasing, and delivery. 25 Fassnacht et al. generalized this, describing it as the extent to which e-services meet customer needs effectively and efficiently. 26 Aguila-Obra et al. added that e-services are interactive services mediated by the Internet, 27 applicable across platforms such as online shopping, social media, and online banking. Scholars have also explored e-SQ from various perspectives.
Scholars have developed multidimensional evaluation models tailored to specific contexts, such as e-Qual, 28 SITEQUAL, 29 WebQual 4.0, 30 PWQ, 31 eTailQ, 32 E-S-QUAL/E-RecS-QUAL, 33 and eTransQual, 34 as detailed in Appendix A. Others have examined how e-SQ affects behaviors such as satisfaction, trust, and loyalty,35–37 offering insights into its underlying mechanisms.
Research and application of electronic SQ in the field of Hospital Information Systems (HIS) have also made certain advancements. Ayaad et al. compared SQ in hospitals using paper-based versus electronic medical records (EMR), 38 while Alzahranid et al. found that factors such as efficiency and content quality during COVID-19 influenced patients’ willingness to use mobile healthcare applications. 39 Li and Guo, using the Delphi method and AHP method, evaluated the SQ of online healthcare platforms based on four major indicators: organizational quality, process quality, outcome quality, and overall quality. 40 These findings provide important insights into understanding the characteristics and influencing factors of electronic SQ in the healthcare sector.
Despite progress, research on medical information systems in HIS remains limited, especially regarding how e-SQ of internet hospital affects PS. This study focuses on intelligent consultation guidance services within internet hospitals, aiming to reveal how SQ influences PS and provide theoretical and practical guidance for improving these services.
Patient satisfaction
Patient satisfaction, originally derived from the concept of customer satisfaction in marketing, has now become a key indicator for measuring healthcare SQ. 41 Risser defined PS as the extent to which actual perceived service aligns with ideal expectations. 42 Pascoe further pointed out that patients form their satisfaction evaluation based on their expectations for medical needs or improvements in quality of life. 43 Ríos-Risquez et al. argued that PS not only reflects the quality of doctor–patient interactions but also serves as an important indicator for midterm evaluations of the nursing process. 44 In traditional healthcare settings, satisfaction research has mainly focused on dimensions such as optimizing medical processes, doctor–patient communication, and service environments.
With the development of internet healthcare, satisfaction research has expanded into the online service domain. The focus of research has gradually shifted toward establishing a scientifically sound online satisfaction evaluation system, identifying key influencing factors, and exploring effective improvement strategies. Ma et al. found that physician response time significantly affects PS. 45 Wu et al. emphasized the role of communication strategies employed by physicians in shaping PS during doctor–patient interactions. 46 Nguyen et al., based on the S–O–R theory, discovered that e-health services not only enhance satisfaction but also increase patient engagement in health management. 47
Building on this, some studies have introduced new theories and methods to further expand the analytical dimensions. Shah et al., combining Herzberg's Two-Factor Theory with digital topic modeling techniques, conducted a comprehensive analysis of the key factors influencing PS and dissatisfaction in physician services. They identified communication skills, professionalism, and emotional care as the main drivers of satisfaction, while poor communication and emotional neglect were the primary sources of dissatisfaction. 48 Hudson et al. employed a mixed-methods approach to compare satisfaction differences between virtual healthcare and traditional face-to-face services. They found that while online services excel in efficiency and convenience, they still have significant shortcomings in personalized care and emotional interaction. 49
Although these studies provide rich perspectives on understanding PS, two gaps still exist in the current literature: first, there is a lack of a unified standard framework and clear evaluation system for assessing satisfaction in online healthcare services; second, most studies focus on doctor–patient communication and medical processes, while research on how AI-powered service modules (such as intelligent consultation guidance services) impact PS and their underlying mechanisms is still insufficient. In particular, the pathway through which intelligent consultation guidance services influence satisfaction via PV and emotions has yet to be fully and systematically revealed.
Patient PV
Patient perceived value (PPV) is derived from the customer PV theory, which emphasizes the trade-off between the benefits obtained and the costs incurred when acquiring a product or service. 50 Therefore, PPV is a comprehensive comparison. It contrasts the benefits gained from treatment outcomes, SQ, and the medical environment with the time, money, and potential risks invested by the patient. This forms an overall evaluation of medical technology and service effectiveness. 51
As healthcare services increasingly focus on patient needs, researchers have begun to explore the connotations of PPV and its influencing mechanisms from various perspectives. One line of research uses PPV as a standard for evaluating healthcare SQ, constructing multidimensional evaluation models of PPV. For example, Liu conducted a survey of outpatient patients at a public hospital in China and developed and validated a PPV model with 8 dimensions and 29 items, including functional, emotional, and social value. 52 Another strand of research emphasizes the subjective experience of patients during healthcare, particularly focusing on how specific service characteristics influence their perceptions of value. For instance, research by Sanıl and Eminer shows that accessibility, affordability, and acceptability significantly impact PPV. 53 Akin and Okumus found that factors such as online experience, doctor–patient interaction, trust, and accessibility in service encounters are key pathways affecting patient perceptions. 54
As seen, the relationship between healthcare services and PV has become increasingly complex, prompting research to incorporate theories from service management, psychology, and behavioral decision-making to more comprehensively reveal the mechanisms and pathways of patient value judgment. In the context of internet healthcare, PPV presents both opportunities and challenges. On the one hand, the spatiotemporal convenience of internet healthcare offers diverse services such as online appointments, follow-ups, report inquiries, and medication delivery. On the other hand, the virtual nature of online interactions and issues of information asymmetry may weaken emotional exchanges between physicians and patients, leading to communication barriers. Thus, how to effectively enhance PPV in the internet healthcare context has become a critical issue requiring urgent resolution.
Service encounter theory
Service encounter theory, a foundational concept in service marketing and management, was first proposed by Solmon et al., emphasizing the interaction between service providers and recipients in a service context. 55 Initially, the theory focused on face-to-face, bidirectional interactions. However, with the growing integration of technology, the scope of service encounters has evolved. 56 Today, the theory encompasses a complex system of interactions involving service organizations, service personnel, and customers, highlighting the critical role of technology and the physical environment in shaping service experiences.57,58
In the context of intelligent consultation guidance services within internet hospitals, service encounters encompass both human interactions (e.g., communication between patients and customer support) and nonhuman interactions (e.g., user operations, service stability, privacy protection, and diagnostic recommendations). The interplay of these touchpoints shapes patients’ overall experience, making service encounter theory a valuable framework for understanding and guiding complex interaction patterns in internet hospitals.
Existing research has focused on two main areas: (1) assessing the impact of service encounters on service performance 59 and (2) examining service encounters as outcome variables across different service environments. 60 However, studies specific to internet hospitals are limited, particularly in analyzing service encounters in the context of intelligent consultation guidance services.
This study applies service encounter theory to intelligent consultation guidance services in internet hospitals, redefining SQ dimensions to refine the analysis of service touchpoints. By capturing key features across technological, procedural, and interactional aspects, it explores the intrinsic mechanisms linking SQ, PV, and PS.
Stimulus–Organism–Response theory
The S–O–R theory, introduced by Mehrabian and Russell, 61 explains how external environmental stimuli (S) influence specific behavioral responses (R) through individuals’ internal psychological states (O). The theory highlights the critical mediating role of perception and emotion in bridging the process from stimulus to response. With its concise structure and broad applicability, S–O–R theory has found broad use in service marketing, consumer behavior, and information systems, with increasing application in healthcare and online medical studies.
In traditional offline healthcare, S–O–R theory commonly examines how service environments and interactions influence patient behavior. For instance, studies have shown that service experiences, as external stimuli, can significantly enhance patients’ willingness to seek care through the mediating variable of “trust.” 62 Additionally, service attitudes and interaction experiences in healthcare environments can directly influence patients’ emotions, shaping their satisfaction and sense of well-being. 63 These findings demonstrate the strong compatibility of S–O–R theory in deconstructing patients’ cognitive and behavioral pathways in offline healthcare services.
In technology-driven online healthcare scenarios, S–O–R theory similarly exhibits robust explanatory and predictive power. For example, Wu and Dong explored user behavioral responses in electronic health services, 64 while Liu et al. validated how content presentation and interaction design in mobile health services enhance user engagement and recommendation behaviors through trust and PV. 65
S–O–R theory is widely applied to online and offline healthcare, explaining patient decision-making under external stimuli. This study applies the S–O–R framework to intelligent consultation guidance in internet hospitals, identifying service encounters as stimuli (S), PV and emotions as the organism (O), and PS as the response (R). By leveraging this framework, the study explores how SQ impacts PS, offering theoretical and practical guidance for enhancing internet hospital services.
Patient emotions
Emotions, as complex psychological and physiological responses, are central to both service and healthcare fields. In service interactions, emotions are defined as “subjective feelings and emotional feedback generated during product or service interactions.” 66 Jiménez-Herrera et al. define patient emotions as reactions to internal and external events, involving cognition, subjective experience, physiological changes, and behavioral expressions. 67
Patient emotions are commonly categorized into positive emotions (e.g., trust, reassurance, joy) and negative emotions (e.g., anxiety, fear, frustration). Positive emotions enhance treatment confidence, improve outcomes, and reduce depression risks,68–70 while negative emotions increase psychological burdens and hinder recovery.71–73
Emotions play a vital role in evaluating service encounters, especially in highly interactive environments.74,75 They influence not only treatment outcomes but also overall service experience and satisfaction. 76 High-quality healthcare services, such as friendly attitudes and excellent delivery, can improve patient emotions, boosting happiness and satisfaction. 63 However, little research has systematically examined patient emotions as mediators between intelligent consultation guidance SQ and satisfaction in internet hospitals.
This study defines patient emotions as responses triggered during the use of intelligent consultation guidance services, shaped by service experiences, interactions, and outcomes. These emotions include cognitive judgments (e.g., SQ evaluation), subjective feelings (e.g., satisfaction or dissatisfaction), physiological reactions (e.g., anxiety-induced rapid heartbeat), and behavioral expressions (e.g., complaints or praise). Positive emotions may arise from efficient service and clear guidance, while negative emotions may stem from misleading recommendations or technical failures.
Positioning patient emotions as mediators, this study explores how emotional responses connect SQ with satisfaction. This framework not only deepens understanding of emotions in internet hospital contexts but also provides practical insights for improving intelligent consultation guidance services and enhancing PS.
Literature review summary
E-service quality, PS, and PV are central to healthcare services, but existing studies often fail to address their interconnections fully. In the context of intelligent consultation guidance services in internet hospitals, several gaps remain unaddressed:
From a content perspective, while research has linked SQ to PS, the unique attributes of intelligent consultation guidance services have been overlooked. These services, as digital healthcare innovations, differ from traditional e-services and offline healthcare in terms of technical complexity, processes, and user experiences. However, their mechanisms for enhancing PS remain underexplored. This study bridges the gap by investigating their role in satisfaction improvement.
Methodologically, most studies rely on single models, limiting robustness and overlooking the advantages of integrating multiple frameworks. To address this, the study adopts a dual-model approach. The E-S-QUAL framework identifies SQ elements and their impacts on satisfaction, while the S-O-R theory and service encounter theory form a patient experience-driven model to explore emotional and value-based pathways. This integrated approach enhances the study's reliability and offers innovative theoretical perspectives.
Existing research has primarily focused on the direct effects of SQ on satisfaction, with limited attention to mediating factors such as emotions and PV. Perceived value assesses the balance between costs and benefits, while emotions reflect psychological responses during service interactions. Both likely mediate the relationship between SQ and satisfaction but lack systematic exploration. This study incorporates these mediators to clarify this link and provide theoretical insights.
In summary, the study constructs a dual-model framework. The first, based on the E-S-QUAL framework, investigates mechanisms linking SQ and satisfaction. The second combines S-O-R theory and service encounter theory to examine how emotions and PV mediate service experiences and satisfaction. By validating these models, the study uncovers core mechanisms of intelligent consultation guidance services and offers practical guidance for optimizing SQ in internet hospitals.
Research framework and hypotheses developing
Research framework based on the E-S-QUAL model
Scale development
The research framework includes three core variables: SQ of intelligent consultation guidance services, PS, and PPV.
The SQ scale is adapted from the E-S-QUAL model,
33
incorporating the functional features of intelligent consultation guidance services and evaluating four dimensions: efficiency (EFF), system availability (SYS), privacy (PRI), and fulfillment (FUL). Efficiency measures the service’s ability to provide fast, agile, and user-friendly experiences. System availability assesses the reliability and functionality of the service features. Privacy evaluates the protection of patient information and confidentiality. Fulfillment reflects the service’s ability to recommend appropriate departments and meet patient needs. Based on expert recommendations, the E-S-QUAL model, and the characteristics of intelligent consultation guidance services, this study refines these dimensions and develops measurement items (see Table 1). The measurement of PS is adapted from Wu et al.'s
77
study on consumer satisfaction, incorporating modifications specific to intelligent consultation guidance services (see Table 2). The measurement of PPV is adapted from Yang et al.'s
78
study on consumer PV, with modifications tailored to intelligent consultation guidance services (see Table 3).
Scale of intelligent consultation guidance service quality.

Scale of patient satisfaction.

Scale of patient perceived value.

Hypothesis development
The E-S-QUAL model extensively analyzes how online SQ affects customer satisfaction, highlighting essential e-SQ aspects and their link to satisfaction.79,80 E-Mamakou et al., based on user data from e-commerce platforms, empirically validated that each dimension of E-S-QUAL has a significant positive impact on user satisfaction. 12 This relationship also holds true in the digital healthcare service domain. For instance, Pal et al. found that the operational efficiency of healthcare platforms significantly affects PS, especially in online services where quick feedback and smooth operation are essential. 81 System availability, as a critical factor for service continuity, has been shown in the study by Kim et al. to have a positive effect on user satisfaction: the more stable and accessible the platform, the higher the user satisfaction. 82 Moreover, privacy protection is crucial in services involving sensitive medical information. Research by Sun et al. indicated that the extent to which an online healthcare platform safeguards patient privacy significantly determines PS. 83 Chang et al. also confirmed that service fulfillment, defined as the degree to which a platform meets its expected service functions, directly and positively influences user satisfaction. 84
Therefore, based on the E-S-QUAL theory, this study evaluates the SQ of intelligent consultation guidance in internet hospitals across four dimensions: EFF, SYS, PRI, and FUL and proposes the following hypotheses: H1a: Efficiency in intelligent consultation guidance services positively influences patient satisfaction. H1b: System availability in intelligent consultation guidance services positively influences patient satisfaction. H1c: Privacy protection in intelligent consultation guidance services positively influences patient satisfaction. H1d: Fulfillment in intelligent consultation guidance services positively influences patient satisfaction.
Perceived value is considered a key indicator in SQ assessments.
85
Existing studies have clearly pointed out the positive impact of electronic SQ dimensions on user-perceived value. In their research on the e-retail industry, Zia et al. found that dimensions of E-S-QUAL, such as service efficiency, system stability, privacy protection, and service fulfillment, significantly enhance users’ overall value perception.
86
Similar relationships have also been supported in the digital healthcare field: for example, Neves et al.'s survey on the impact of digital telemedicine services found that service efficiency has a positive impact on patients’ PV.
87
Alsohime et al. discovered that the effectiveness of healthcare information systems significantly improved patients’ overall value assessment of services.
88
Yin pointed out that the good protection of user privacy on online healthcare platforms significantly enhanced users’ PV.
89
Additionally, Panggabean et al.'s research indicated that the fulfillment of platform services is significantly positively correlated with user-perceived value; the higher the degree of service fulfillment, the stronger the overall value perception of users.
90
Hence: H2a: Efficiency in intelligent consultation guidance services positively influences patient perceived value. H2b: System availability in intelligent consultation guidance services positively influences patient perceived value. H2c: Privacy protection in intelligent consultation guidance services positively influences patient perceived value. H2d: Fulfillment in intelligent consultation guidance services positively influences patient perceived value.
In the digital healthcare environment, existing studies have pointed out that the impact of SQ on PS is often mediated by PV. Sreejesh et al. found that the SQ of digital healthcare platforms first enhances patients’ overall PV, which then significantly increases PS.
91
Ananda et al. also confirmed, in their empirical study on digital healthcare apps, that system quality indirectly promotes satisfaction by enhancing patients’ PV.
92
Yesilada et al. further pointed out that patients’ perception of telemedicine SQ first increases the PV of the service, which then enhances overall service satisfaction.
93
Hence: H3: Patient perceived value positively influences patient satisfaction. H3a: Patient perceived value mediates the relationship between efficiency and patient satisfaction in intelligent consultation guidance services. H3b: Patient perceived value mediates the relationship between system availability and patient satisfaction in intelligent consultation guidance services. H3c: Patient perceived value mediates the relationship between privacy and patient satisfaction in intelligent consultation guidance services. H3d: Patient perceived value mediates the relationship between fulfillment and patient satisfaction in intelligent consultation guidance services.
In summary, this study builds on existing research to construct the first research framework based on the E-S-QUAL model (Model 1, see Figure 1). It evaluates the quality of intelligent consultation guidance services across four dimensions, incorporating PV as a mediator to analyze its effect on PS.

E-S-QUAL-based service quality model (model 1).
Research framework based on the patient experience-driven model
Model development
As a crucial step preceding patient consultations on internet medical platforms, the quality of intelligent consultation guidance services plays a pivotal role in shaping patient experiences. Multidimensional service encounters serve as effective communication bridges between medical platforms and patients. 94 This study integrates service encounter theory with the S–O–R framework to develop a patient experience-driven model, identifying key factors influencing PS.
The study redefines SQ into three core dimensions of service encounters: SIE, SSE, and SRE. Using the S–O–R framework, it examines how service encounters (S) affect PS (R) through PV and patient emotions (O). The S–O–R theory, widely applied to analyze patient behavior, attitudes, and usage intentions, 95 explains how external stimuli, such as intelligent consultation guidance services, elicit emotional and cognitive responses that shape satisfaction.
Service interaction encounters involve the interactive experience between patients and services, including ease of operation, response speed, system availability, and efficiency. As the initial contact point, effective interaction reduces effort and builds trust. Quick responses and smooth operations enhance initial experiences and lay the foundation for future evaluations. 96
Service security encounters reflect platform stability and privacy protection. Reliable system performance minimizes negative experiences, while robust data protection boosts trust. When patients trust the safety of their information, their acceptance and reliance on the service increase significantly. 97
Service recommendation encounters highlight the service's ability to meet patient needs through accurate, efficient, and comprehensive recommendations. Accuracy builds trust, efficiency saves time, and comprehensiveness ensures full coverage of patient needs. Effective recommendations significantly enhance satisfaction and loyalty. 98
This model offers both theoretical innovation and practical value. By emphasizing patient experience, it integrates key service encounter dimensions and addresses evolving patient needs during service use. It provides systematic guidance for optimizing SQ by illustrating how service touchpoints in intelligent consultation guidance services influence satisfaction. Designed to align with internet hospital scenarios, the model ensures practical applicability and feasibility.
Scale development
The research framework includes four variables: intelligent consultation guidance service encounters (SE), PS, PPV, and patient emotions (PE).
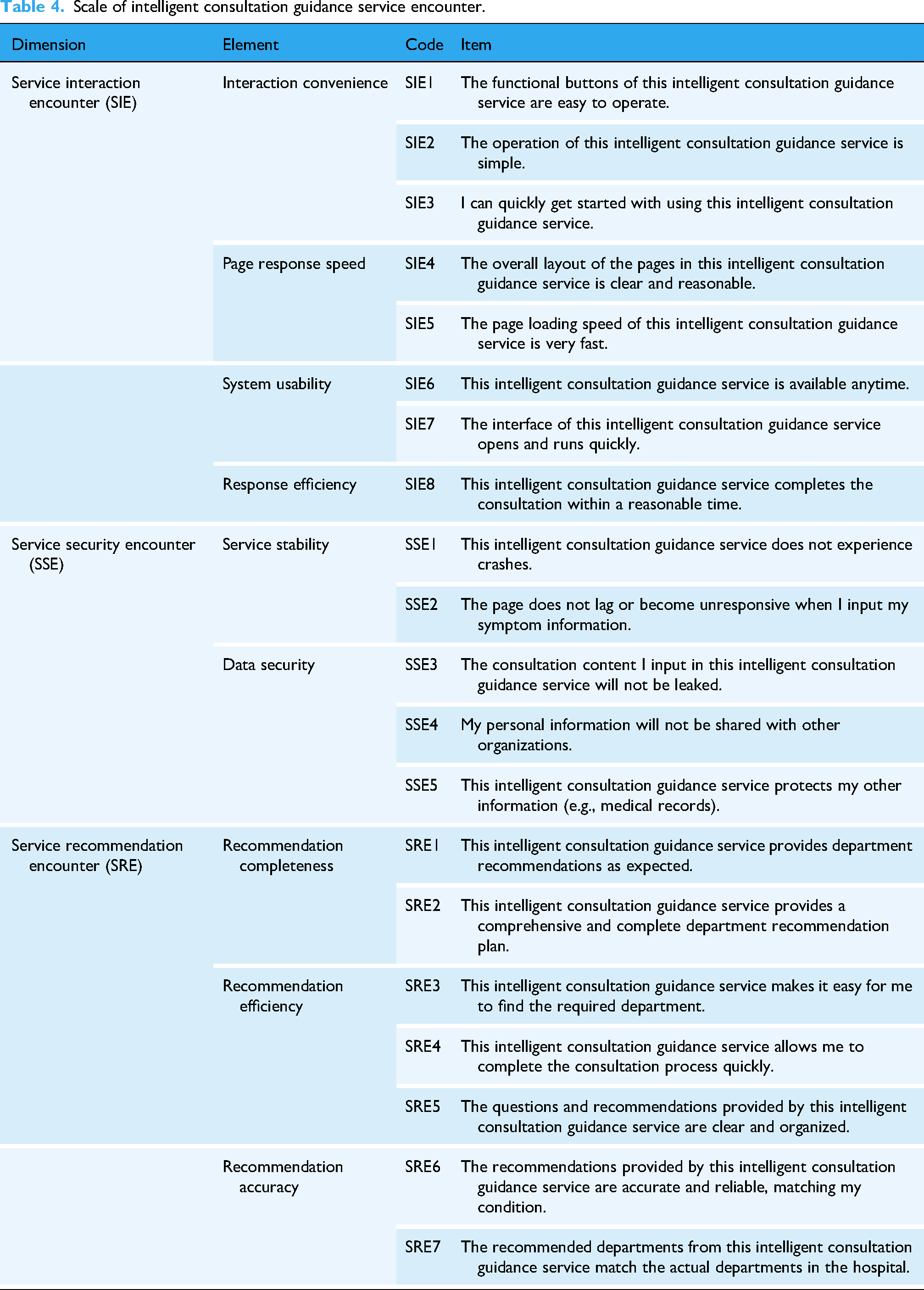
Intelligent consultation guidance service encounters are restructured into three dimensions: SIE, SSE, and SRE. Service interaction encounter focuses on convenience, operational experience, and response efficiency. Service security encounter emphasizes service stability and privacy protection. Service recommendation encounter covers completeness, accuracy, and efficiency in diagnostic and recommendation processes. Scale items are listed in Table 4. Patient emotions are categorized into two dimensions: patient positive emotions (PPE) and patient negative emotions (PNE). The scale items are developed based on the studies of Nadarzynski et al.,
99
Kumar et al.,
100
Fekonja et al.,
101
Fernandes et al.,
102
and Yang et al.
78
The detailed scale items are presented in Table 5. Patient PV and PS are measured in the same way as in Model 1, as shown in Tables 2 and 3.
Scale of intelligent consultation guidance service encounter.
Scale of patient emotions.

Hypothesis development
In the context of intelligent consultation guidance services, patients obtain information and complete the guidance process through various service encounters. These encounters serve as stimuli (S), triggering emotional responses and evaluations of PV (O), which ultimately influence satisfaction (R). Based on the S–O–R theory and service encounter theory, the following hypotheses are proposed.
Studies show that patients’ evaluations of service encounters are closely linked to their emotional responses during and after the service process.
103
According to service encounter theory, emotions play a vital role in evaluating service experiences. Mahmud et al.
104
noted that different environmental stimuli elicit varying emotional reactions. In intelligent consultation guidance services, SIE, SSE, and SREs are key external stimuli that directly impact patient emotions. User-friendly platforms enhance convenience and experience, evoking positive emotions such as trust and satisfaction. Privacy and data security alleviate anxiety, generating positive emotions. Personalized and accurate recommendations increase trust and satisfaction. Therefore: H4a: Service interaction encounters positively influence patient positive emotions. H4b: Service security encounters positively influence patient positive emotions. H4c: Service recommendation encounters positively influence patient positive emotions.
Conversely, negative service encounters can provoke negative emotions, adversely affecting the experience. Complex operations or unfriendly designs cause confusion and frustration. Privacy breaches or security issues create anxiety and fear. Inaccurate recommendations lead to dissatisfaction and disappointment. Therefore: H5a: Service interaction encounters negatively influence patient negative emotions. H5b: Service security encounters negatively influence patient negative emotions. H5c: Service recommendation encounters negatively influence patient negative emotions.
High-quality service encounters enhance PPV.
105
In intelligent consultation guidance services, interaction encounters improve efficiency and convenience, security encounters foster trust through privacy protection, and recommendation encounters meet patient needs with personalized suggestions. Therefore: H6a: Service interaction encounters positively influence patient perceived value. H6b: Service security encounters positively influence patient perceived value. H6c: Service recommendation encounters positively influence patient perceived value.
Perceived value is a critical factor in PS, acting as a bridge between service encounters (S) and satisfaction (R).
106
Thus: H7: Perceived value positively influences patient satisfaction. H7a: Perceived value mediates the relationship between service interaction encounters and patient satisfaction. H7b: Perceived value mediates the relationship between service security encounters and patient satisfaction. H7c: Perceived value mediates the relationship between service recommendation encounters and patient satisfaction.
Emotions significantly influence satisfaction, especially in healthcare contexts. External stimuli, such as SQ, affect emotions, which in turn shape satisfaction.
107
Positive emotions foster engagement and trust, reinforcing favorable evaluations, while negative emotions reduce trust and PV, lowering satisfaction. In intelligent consultation guidance services, these emotions mediate the relationship between service encounters and satisfaction. Therefore: H8: Patient positive emotions positively influence patient satisfaction. H8a: Patient positive emotions mediate the relationship between service interaction encounters and patient satisfaction. H8b: Patient positive emotions mediate the relationship between service security encounters and patient satisfaction. H8c: Patient positive emotions mediate the relationship between service recommendation encounters and patient satisfaction. H9: Patient negative emotions negatively influence patient satisfaction. H9a: Patient negative emotions mediate the relationship between service interaction encounters and patient satisfaction. H9b: Patient negative emotions mediate the relationship between service security encounters and patient satisfaction. H9c: Patient negative emotions mediate the relationship between service recommendation encounters and patient satisfaction.
In summary, based on the S–O–R theory and service encounter theory, this study constructs a “PEDM” (Model 2, see Figure 2) suitable for the context of intelligent consultation guidance services. The model approaches service encounters from three dimensions: service interaction, service security, and service recommendation, exploring how they influence overall satisfaction with healthcare services through patient emotions (both positive and negative) and PV. Specifically, the three types of service encounters act as external stimuli (S), which, by triggering patients’ emotional states and value judgments (O), further impact their satisfaction evaluations (R). This path structure not only aligns with the logical framework of the S–O–R theory but also fits the practical characteristics of intelligent consultation guidance as a technology-driven service.
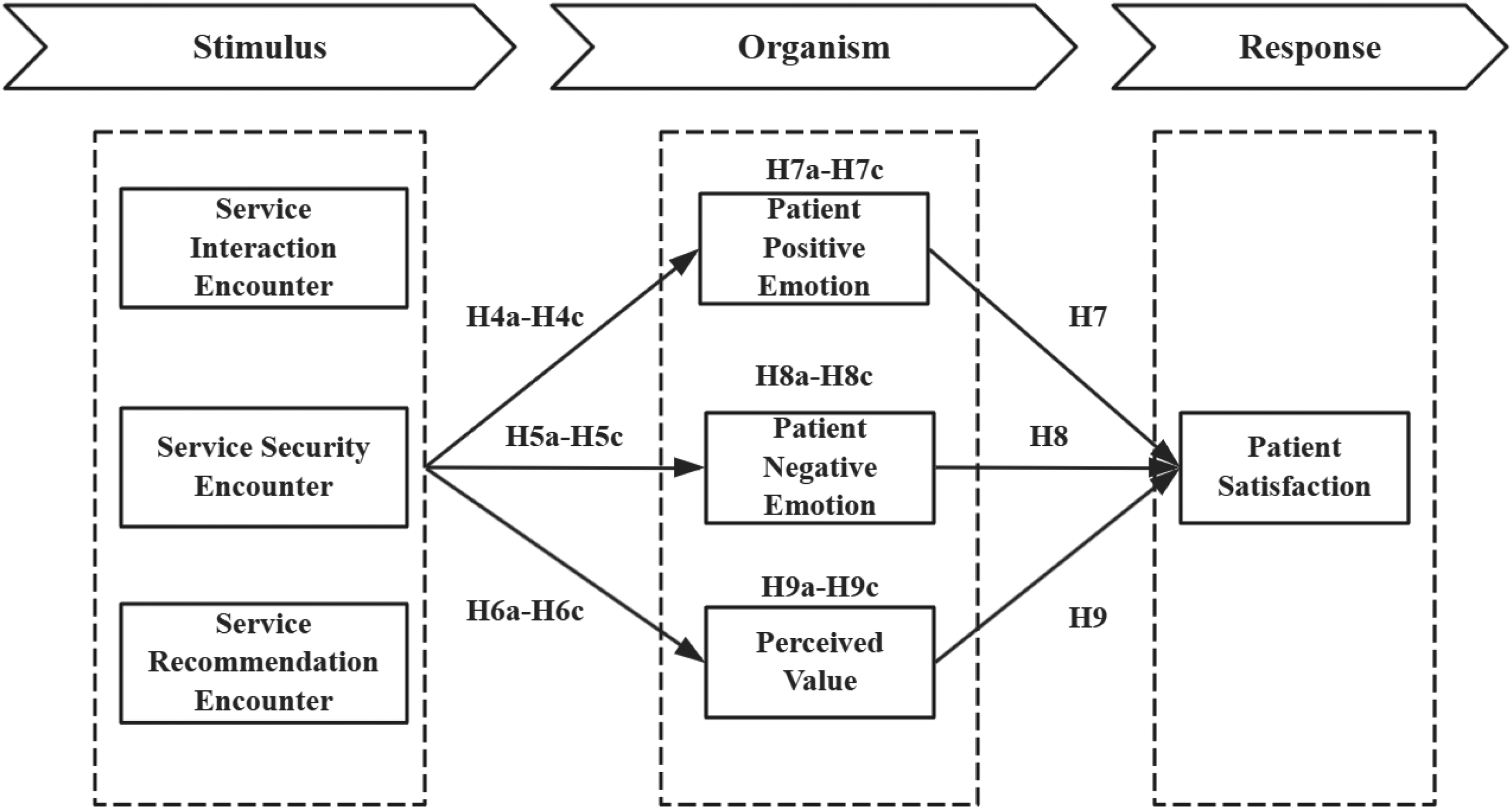
Patient experience-driven model (model 2).
Compared to Model 1, Model 2 places more emphasis on the subjective experience of patients during the service process, particularly the mediating roles of emotional and cognitive factors. It aims to reveal the internal pathways through which SQ influences satisfaction via psychological mechanisms. This model provides a new theoretical perspective for understanding the impact mechanism of intelligent consultation guidance services and offers a reference for optimizing user experience and improving satisfaction in internet hospitals.
Building on the previous discussion, Figure 3 presents the overall research framework of this study, which consists of two submodels based on the E-S-QUAL theory (Model 1) and service encounter theory/S–O–R theory (Model 2). Model 1 focuses on the four system quality dimensions (EFF, SYS, PRI, and FUL) of intelligent consultation guidance services in internet hospitals, exploring their influence on PS through PV, with an emphasis on the impact mechanism of technological service attributes. Model 2 introduces the three dimensions of service encounters (SIE, SSE, and SRE), further incorporating emotional variables (PPE, PNE), and explores the influence of intelligent consultation guidance services on PS from a psychological perception perspective, emphasizing the role of user experience and emotional mechanisms.

Overall research framework.
Figure 3, by integrating both theoretical models, constructs a systematic dual-path analysis framework: the left path represents the experiential path (psychologically driven), while the right path represents the system quality path (technologically driven), both converging at the outcome variable of PS. The validation of this dual-model framework not only enhances the robustness of the theory but also reveals, from multiple perspectives, the complex pathways and underlying mechanisms through which intelligent consultation guidance SQ influences PS.
Methods
Research design and sample definition
This study is a cross-sectional study that utilizes a questionnaire survey method. The data collection period was from July 2024 to September 2024, and the survey was conducted at the Affiliated Hospital of Guangdong Medical University in Zhanjiang, Guangdong Province, China. The hospital, the largest Grade A tertiary hospital in western Guangdong Province, serves over 1.85 million outpatient and emergency visits annually. Its internet hospital has served more than 1.5 million users and ranks among top 100 internet hospitals in China. 1
The study subjects were patients who had used the intelligent consultation guidance services of the hospital in the past year and completed the full medical process (including online consultation guidance and subsequent treatment). Inclusion criteria include (1) having used the internet hospital's intelligent consultation guidance services and (2) being able to complete an electronic or paper questionnaire.
Questionnaire content and data collection process
This study designed two structured questionnaires to measure the core variable relationships of two theoretical models:
Questionnaire 1 (see Appendix B), based on the E-S-QUAL SQ model, aims to measure the quality of intelligent consultation guidance services (including the four dimensions of efficiency, system availability, privacy, and fulfillment), PV, and PS. The main section of this questionnaire contains 26 items, with an additional 5 items collecting basic demographic information (gender, age, education, occupation, and monthly income), totaling 31 items. Questionnaire 2 (see Appendix C), based on service encounter theory and the S–O–R theory, constructs the “PEDM” (Model 2). The variables measured include three dimensions of service encounters (SIE, SSE, SRE), patient emotions (PPE, PNE), PV, and satisfaction (PS). The main section of this questionnaire contains 32 items, with the demographic section identical to Questionnaire 1, bringing the total to 37 items.
Both questionnaires use a 5-point Likert scale (1 = Strongly Disagree, 5 = Strongly Agree) for measurement. Content validity was ensured through pretesting, expert reviews, and logical revisions (see Chapter 3 for scale construction).
Before data collection officially began, ethical approval was obtained from the Academic Committee of the School of Business Administration at Guangxi University. All participants were fully informed about the study's objectives, data usage, and privacy protection measures before completing the questionnaires and provided written informed consent to participate voluntarily. The data were collected anonymously, and no personally identifiable information was involved in the study.
Data collection was conducted in two phases. The first phase was a pretest phase, where 11 graduate students, 10 IT professionals, and 23 patients (44 participants in total) were invited to test the questionnaires. Through two rounds of feedback, the wording of the items was optimized, ambiguities were removed, and redundant items were eliminated to ensure good content validity. The second phase was the formal survey phase, which employed a combination of online and offline methods. The offline survey primarily involved randomly inviting patients who had used the intelligent consultation guidance service to complete paper questionnaires in the hospital's outpatient waiting area. The online survey was distributed via the official WeChat account of the Affiliated Hospital of Guangdong Medical University (a popular social media platform in China), with a screening question to ensure respondents had relevant experience.
To ensure the validity and representativeness of the data, strict exclusion criteria were applied to the questionnaires: (1) respondents who selected the same answer for all items; (2) respondents exhibiting obvious answering patterns; and (3) respondents with missing values for key variables.
Sample size calculation and demographic characteristics
To ensure the reliability and representativeness of the study results, an appropriate sample size was determined based on classic sample size calculation methods.
Given the large and difficult-to-estimate population of internet hospital users, the study assumes a large and unknown population size, independent responses from participants, and that the data meet the normal distribution requirement under large sample conditions. Therefore, this study applies the standard sample size calculation formula suitable for scenarios with an unknown or extremely large population size:
In the formula, Z represents the statistical value corresponding to the confidence level. This study uses a 95% confidence level (Z ≈ 1.96), meaning we are 95% confident that the survey results truly represent the overall situation. p is the estimated proportion of the population. Since the exact proportion of satisfied or dissatisfied users is unknown, the most conservative estimate (p = 0.5) is used to ensure that the sample size is large enough and the survey results are more reliable. E is the acceptable margin of error, which is set at 0.05 in this study, indicating that the error in the survey results will not exceed ±5%, thus maintaining survey accuracy without requiring an excessively large sample size. Substituting these values into formula (1) yields n = 384.16, which is rounded up to 385. Therefore, the minimum sample size required for this study is 385.
Given that the two questionnaires measure different models, separate surveys were conducted, and responses were collected accordingly. After excluding invalid responses (e.g., identical answers throughout, patterned responses, or missing data), the study obtained a total of 1113 valid questionnaires: 602 for Questionnaire 1 and 511 for Questionnaire 2. Details are shown in Table 6.
Demographic characteristics of the study sample.

Females slightly outnumbered males in the sample. In Questionnaire 1, males accounted for 44.0% and females 56.0%, while in Questionnaire 2, males accounted for 45.4%. Most participants were aged 30–49, comprising 46.2% in Questionnaire 1 and 45.4% in Questionnaire 2. Education levels were predominantly associate degree or below, accounting for 64.6% and 68.9% in Questionnaires 1 and 2, respectively. Occupations showed a higher proportion of government and public sector employees (17.8% in Questionnaire 1 and 20.9% in Questionnaire 2) and other occupational groups (40.0% and 37.0%, respectively). For monthly income, most participants fell within the 2000–5000 RMB (39.4% and 38.4%) and 5000–10,000 RMB (24.4% and 27.8%) ranges.
Data analysis methods
To verify the validity of the measurement tools used and to test the relationships among variables in the research hypotheses through data analysis, this study employed a variety of statistical methods. SPSS 25.0 and AMOS 28.0 were employed as statistical software, combined with techniques such as reliability analysis, validity analysis, SEM, and the Bootstrap sampling method, to systematically process the data. The selection of each analytical method was based on the structural complexity of the research questions and the characteristics of the variables and was carried out in stages. The specific steps are as follows:
First, common method bias (CMB) test and reliability analysis. In the initial stage of data analysis, this study first conducted a Harman single-factor test using SPSS to identify the presence of CMB. This test controls for systematic errors potentially introduced by the questionnaire design, thereby ensuring data validity. Subsequently, reliability analysis was performed on all scales using SPSS to assess their internal consistency and stability, thereby ensuring the reliability of the measurement tools.
Second, validity analysis. In the validity analysis, EFA was first conducted on the “service encounter” dimension to determine the aggregation of items and to ensure the rationality of the dimension division. Since the “service encounter” scale was newly constructed based on service encounter theory, EFA is a necessary preliminary analysis to confirm structural validity. After identifying the structure, confirmatory factor analysis (CFA) was employed to test the measurement model's fit. Confirmatory factor analysis can assess the structural validity, convergent validity, and discriminant validity of the model, thereby verifying the validity of the measurement tools.
Third, path relationship modeling. After testing the latent variable structure, SEM was employed to model and analyze the path relationships among variables. Compared with regression analysis methods, SEM can simultaneously handle direct and indirect relationships among multiple latent variables and incorporate measurement errors for comprehensive estimation. Since this study constructed two theoretical models containing multidimensional latent variables and mediating paths, SEM is more suitable for analyzing complex path mechanisms and providing overall fit assessment.
Fourth, mediating effect test. To assess the mediating role of PV and emotional variables in the path relationships, this study employed the Bootstrap sampling method to test the significance of indirect effects. Unlike the Sobel test, the Bootstrap method does not rely on the assumption of normal distribution (in actual research, data often fail to meet the prerequisite of normal distribution, which may lead to biased results). By repeatedly sampling with replacement from the original data, the empirical distribution of the mediating effect is generated, thereby obtaining more robust test results.
Results
Common method bias analysis
To reduce CMB, this study adopted multiple measures. First, a pretest was conducted to ensure that the questionnaire content was clear and unambiguous. Second, questionnaires were distributed both online and offline, with confidentiality promised to enhance response authenticity. Additionally, Harman's single-factor test was conducted using SPSS 25.0 for both research models. Results showed that the unrotated variance explained by the first factor was 48.68% for Model 1 and 44.70% for Model 2, both below the 50% threshold, 108 indicating no significant CMB.
Reliability test
Reliability testing evaluates the consistency and reliability of questionnaire items, with Cronbach's α being the most widely used indicator. SPSS 25.0 was used to assess the reliability of Questionnaires 1 and 2. Results are shown in Tables 7 and 8. All Cronbach's α coefficients exceeded 0.8, 109 indicating high reliability for both questionnaires.
Reliability test results of model 1
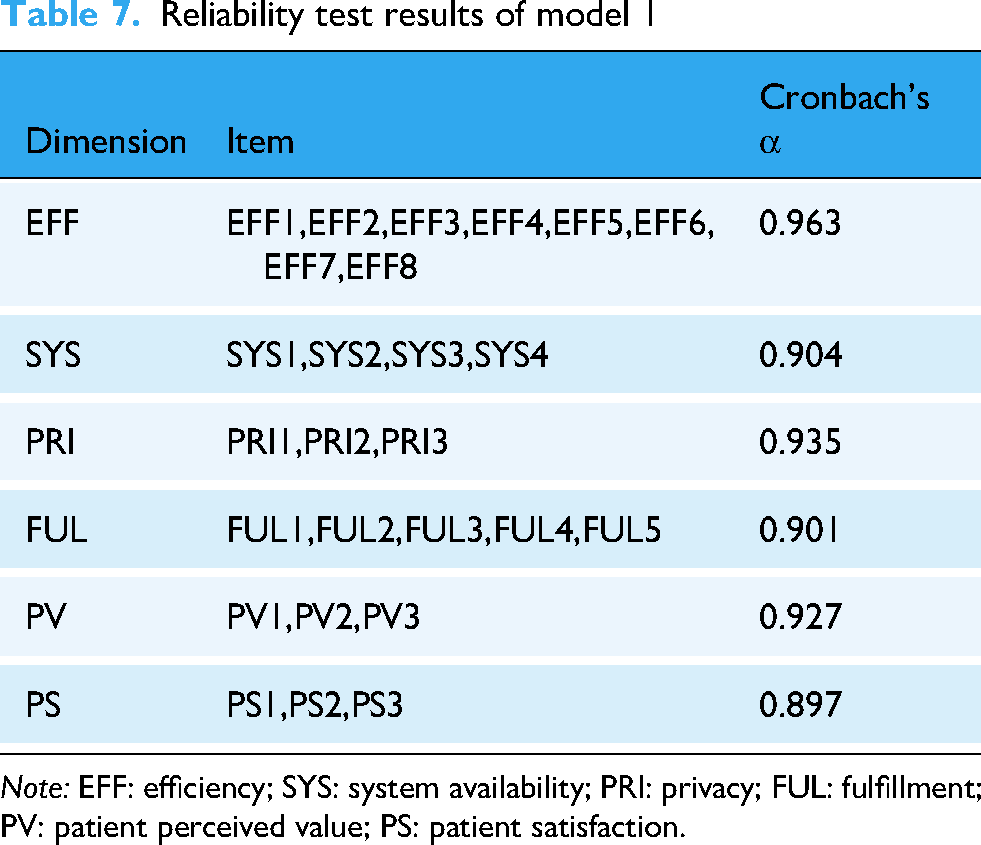
Note: EFF: efficiency; SYS: system availability; PRI: privacy; FUL: fulfillment; PV: patient perceived value; PS: patient satisfaction.
Reliability test results of model 2.
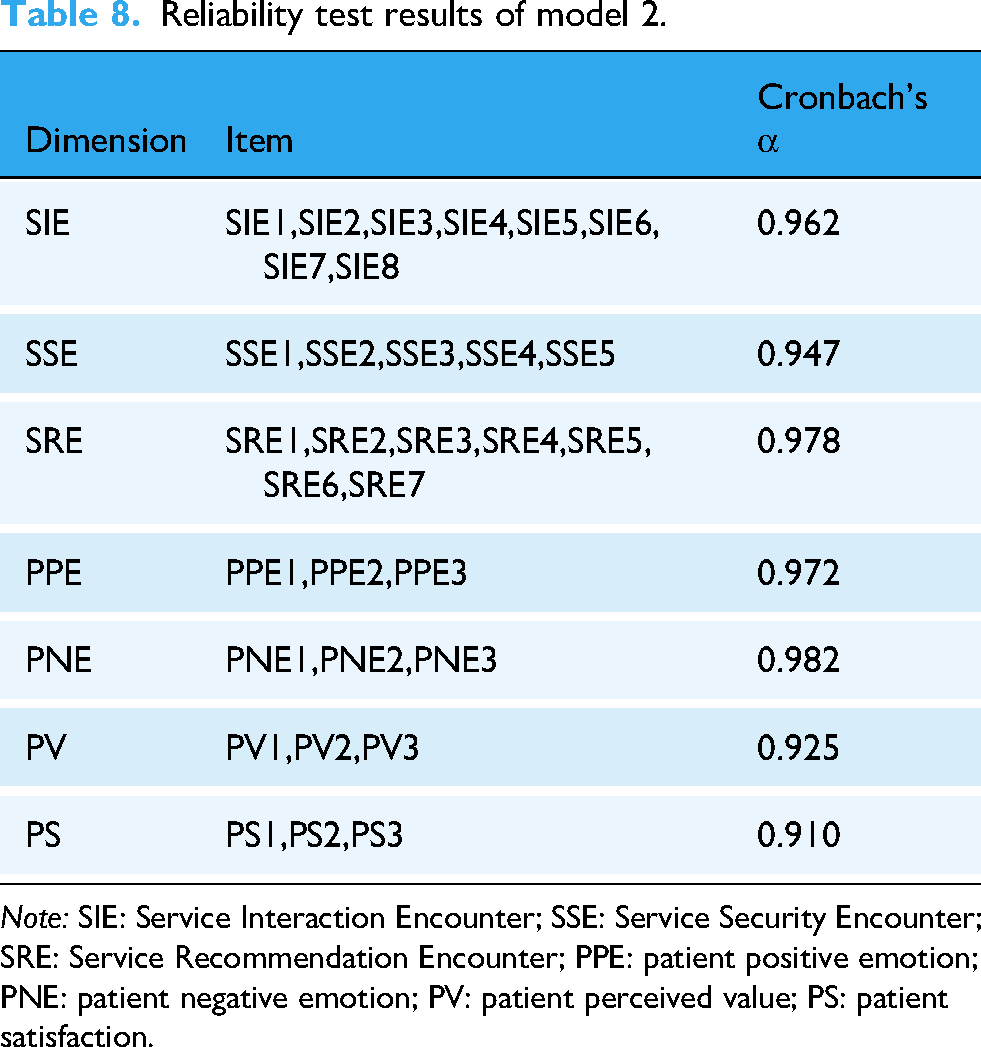
Note: SIE: Service Interaction Encounter; SSE: Service Security Encounter; SRE: Service Recommendation Encounter; PPE: patient positive emotion; PNE: patient negative emotion; PV: patient perceived value; PS: patient satisfaction.
Validity test
Validity test for model 1
As shown in Table 9, the fit indices of Model 1 are good, with all values meeting the recommended standards, indicating that Model 1 has good structural validity.
Fit indices of model 1.

Notes: Chi/DF: Chi-square to Degrees of Freedom ratio; RMSEA: root mean square error of approximation; GFI: goodness-of-fit index; AGFI: adjusted goodness-of-fit index.
Chi/DF measures the parsimony of the model. RMSEA is used to evaluate the overall goodness-of-fit of the model. GFI and AGFI both of which reflect the degree to which the model explains the covariance among variables. NFI, IFI, CFI, and TLI are all comparative fit indices, used to compare the fit of the hypothesized model with that of the independence model.
Convergent validity evaluates the consistency of items within a dimension, assessing whether these items measure the same construct. Commonly used indicators include standardized factor loadings, composite reliability (CR), and average variance extracted (AVE). As shown in Table 10, all measurement indicators in Model 1, except for the reference indicator set to 1, have factor loadings that are significant at the p < 0.001 level. The standardized factor loadings for all observed variables exceed 0.6, 113 indicating that the observed variables adequately reflect their corresponding latent variables. The CR values for all latent variables exceed 0.8, 110 demonstrating good internal consistency among items. Additionally, the AVE values for all latent variables exceed 0.6, 110 indicating that the latent variables explain a substantial portion of the variance in their corresponding items.
Convergent validity test results of model 1.

Notes: ***p < 0.001.
EFF: efficiency; SYS: system availability; PRI: privacy; FUL: fulfillment; PV: patient perceived value; PS: patient satisfaction.
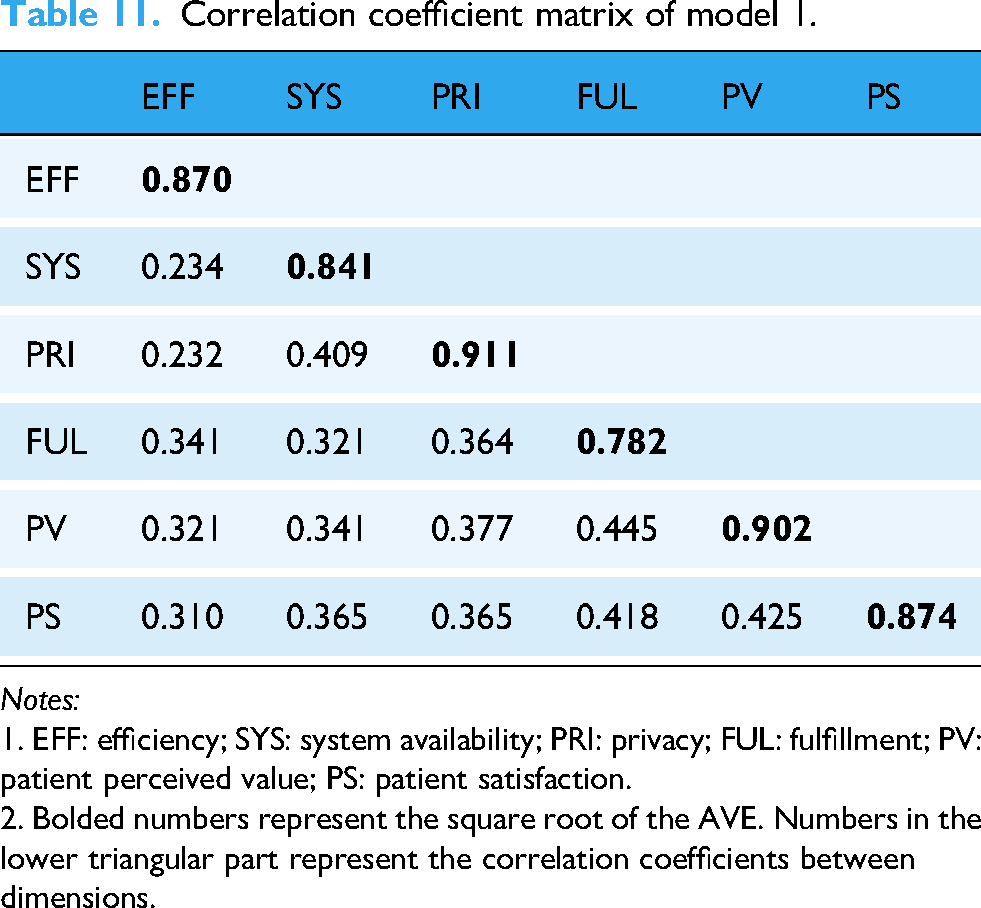
Thus, Model 1 exhibits good convergent validity, with items consistently and effectively reflecting their respective latent variables. Discriminant validity evaluates whether a scale can effectively distinguish between different dimensions, meaning there should be clear distinctions between dimensions. The commonly used statistical indicator is the correlation coefficient matrix (see Table 11). The square root of the AVE for each dimension (bolded in Table 11) should exceed the correlation coefficients between that dimension and others (values in the lower triangular part of Table 11). 114 As shown in Table 11, the correlation coefficient matrix for Model 1 meets this requirement, indicating that Model 1 demonstrates good discriminant validity.
Correlation coefficient matrix of model 1.
Notes:
1. EFF: efficiency; SYS: system availability; PRI: privacy; FUL: fulfillment; PV: patient perceived value; PS: patient satisfaction.
2. Bolded numbers represent the square root of the AVE. Numbers in the lower triangular part represent the correlation coefficients between dimensions.
Validity test for model 2
For Model 2, as its service encounter scale for intelligent consultation guidance services was adapted and restructured based on theoretical frameworks from previous studies, this study used SPSS 25.0 to perform EFA to ensure the validity and applicability of the scale. Exploratory factor analysis helps clarify the internal relationships among dimensions, identify whether the latent variable structure aligns with the research context and theoretical model, and provides a foundation for subsequent CFA.
The KMO and Bartlett's test results for the service encounter scale are shown in Table 12. Bartlett’s sphericity test yielded an approximate chi-square value of 13,460.160 with 190 degrees of freedom and a significance p-value of 0.000. At a significance level of α = 0.05, the null hypothesis was rejected, indicating significant differences between the correlation matrix and the identity matrix. Additionally, the KMO sampling adequacy measure was 0.945. According to Kaiser’s standard, this indicates that the scale items are suitable for factor analysis.
KMO and Bartlett's test.

This study used principal component analysis for factor extraction, determining the number of factors based on the Kaiser criterion (eigenvalue greater than 1). The factors were then refined through Varimax rotation, which maximizes the variance and enhances the distinctiveness and interpretability of the factors. The retention criterion for factor loadings was set at greater than 0.5, with no significant cross-loadings observed. As shown in Table 13, three factors were finally extracted: SIE, SSE, and SRE. All item loadings were greater than 0.7 and were clearly attributed to the corresponding factors, indicating that the scale has good structural validity and convergent validity.
Rotated component matrix a .

Notes:
Extraction method: Principal Component Analysis.
Rotation method: Kaiser-normalized varimax rotation.
Rotation converged in five iterations.
This study continued to use AMOS 28.0 to construct the SEM for Model 2 and performed CFA. The results of the structural validity, convergent validity, and discriminant validity tests for Model 2 are presented in Tables 14, 15, and 16, respectively. Based on the analysis of validity test indicators discussed earlier, Model 2 demonstrates good structural validity, convergent validity, and discriminant validity.
Fit indices of model 2.
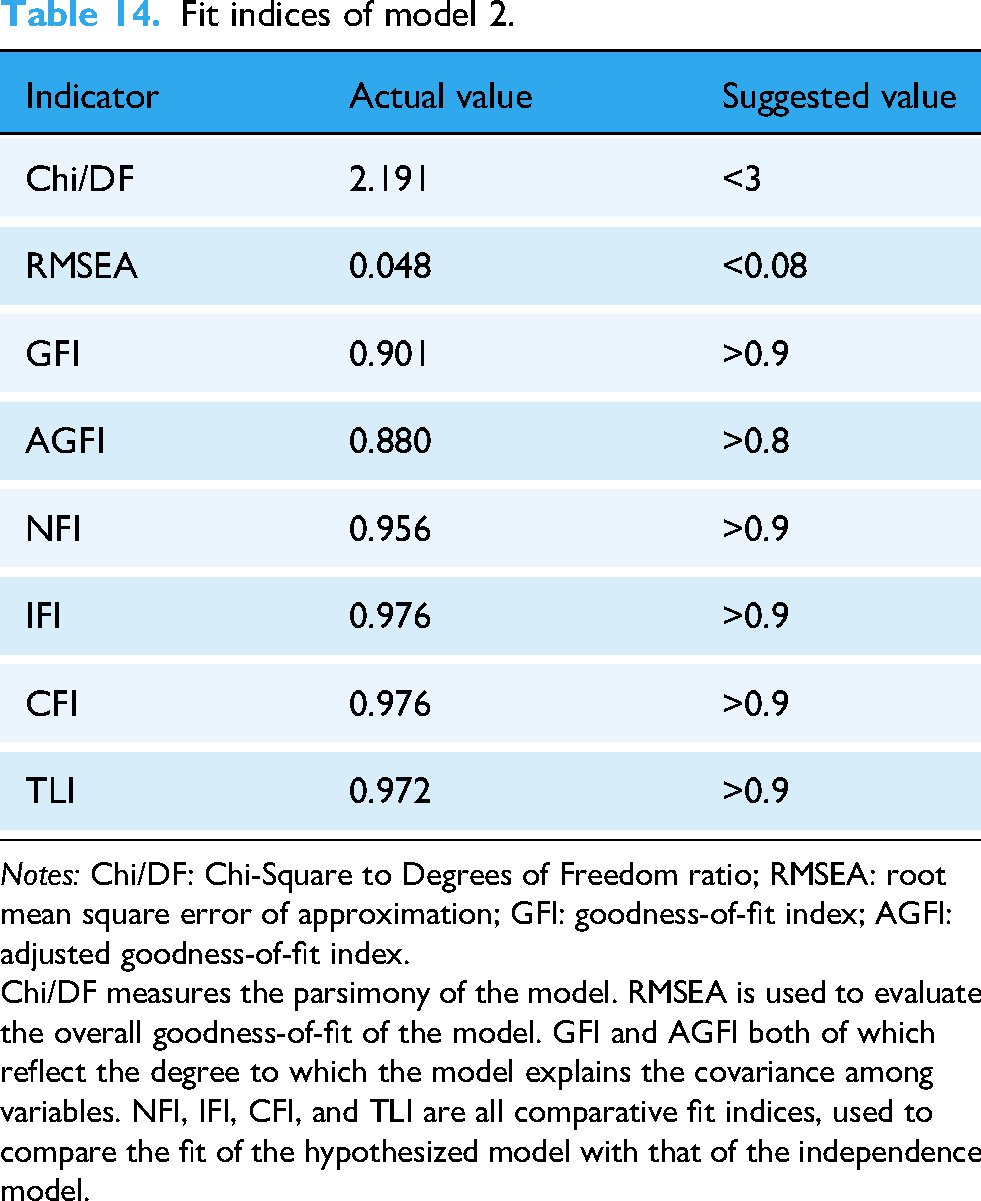
Notes: Chi/DF: Chi-Square to Degrees of Freedom ratio; RMSEA: root mean square error of approximation; GFI: goodness-of-fit index; AGFI: adjusted goodness-of-fit index.
Chi/DF measures the parsimony of the model. RMSEA is used to evaluate the overall goodness-of-fit of the model. GFI and AGFI both of which reflect the degree to which the model explains the covariance among variables. NFI, IFI, CFI, and TLI are all comparative fit indices, used to compare the fit of the hypothesized model with that of the independence model.
Convergent validity test results of model 2.

Notes: *** p < 0.001.
SIE: service interaction encounter; SSE: service security encounter; SRE: service recommendation encounter; PPE: patient positive emotion; PNE: patient negative emotion; PV: patient perceived value; PS: patient satisfaction.
Correlation coefficient matrix of model 2.
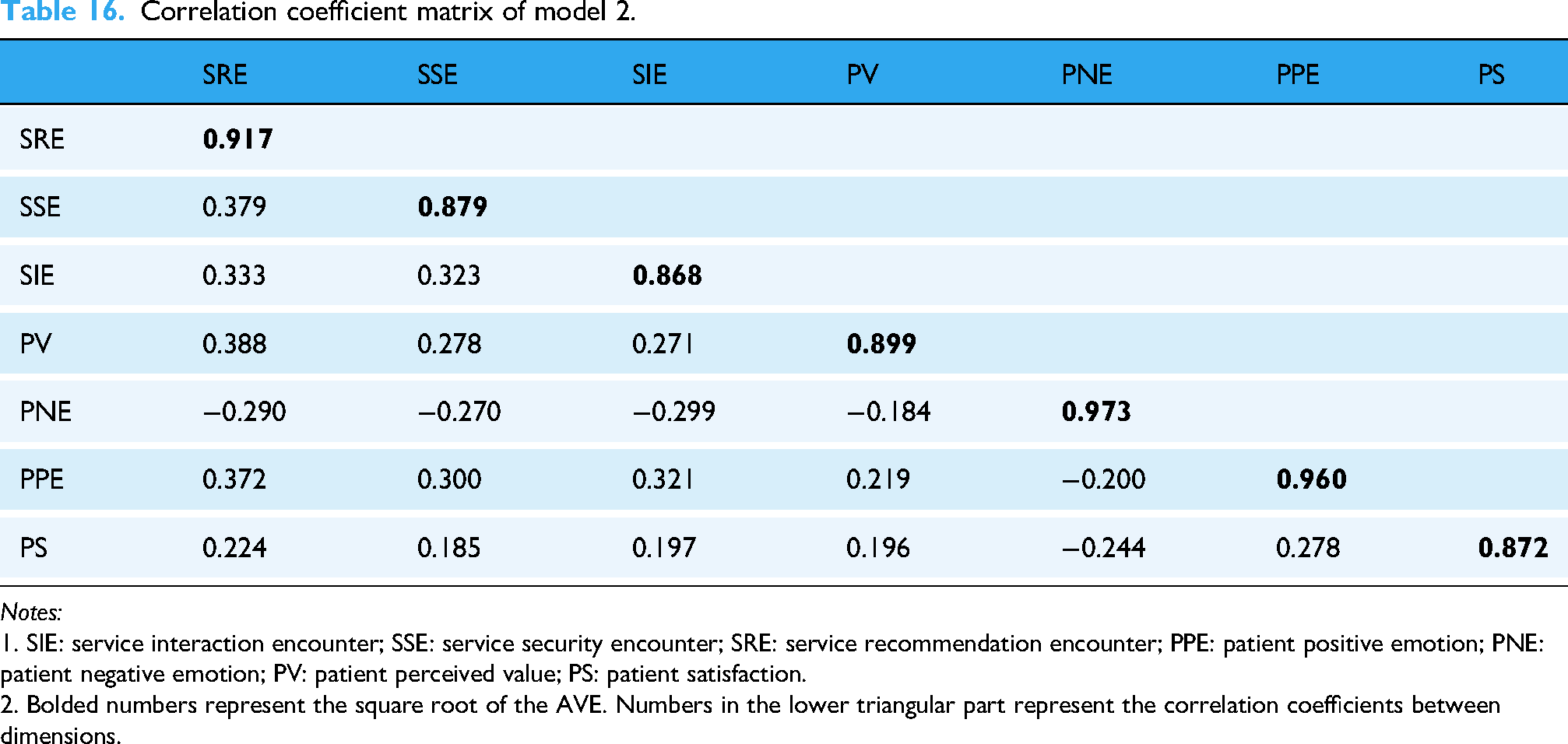
Notes:
1. SIE: service interaction encounter; SSE: service security encounter; SRE: service recommendation encounter; PPE: patient positive emotion; PNE: patient negative emotion; PV: patient perceived value; PS: patient satisfaction.
2. Bolded numbers represent the square root of the AVE. Numbers in the lower triangular part represent the correlation coefficients between dimensions.
Hypothesis testing
Direct path effects analysis for model 1
Using AMOS 28.0, this study constructed a SEM to examine the relationships between the four dimensions of intelligent consultation guidance SQ (EFF, SYS, FUL, and PRI) and PV as independent variables, and PS as the dependent variable.
Table 17 and Figure 4 present the estimated values and significance levels of each path in Model 1. Based on the model results, the path effects are explained in detail as follows:
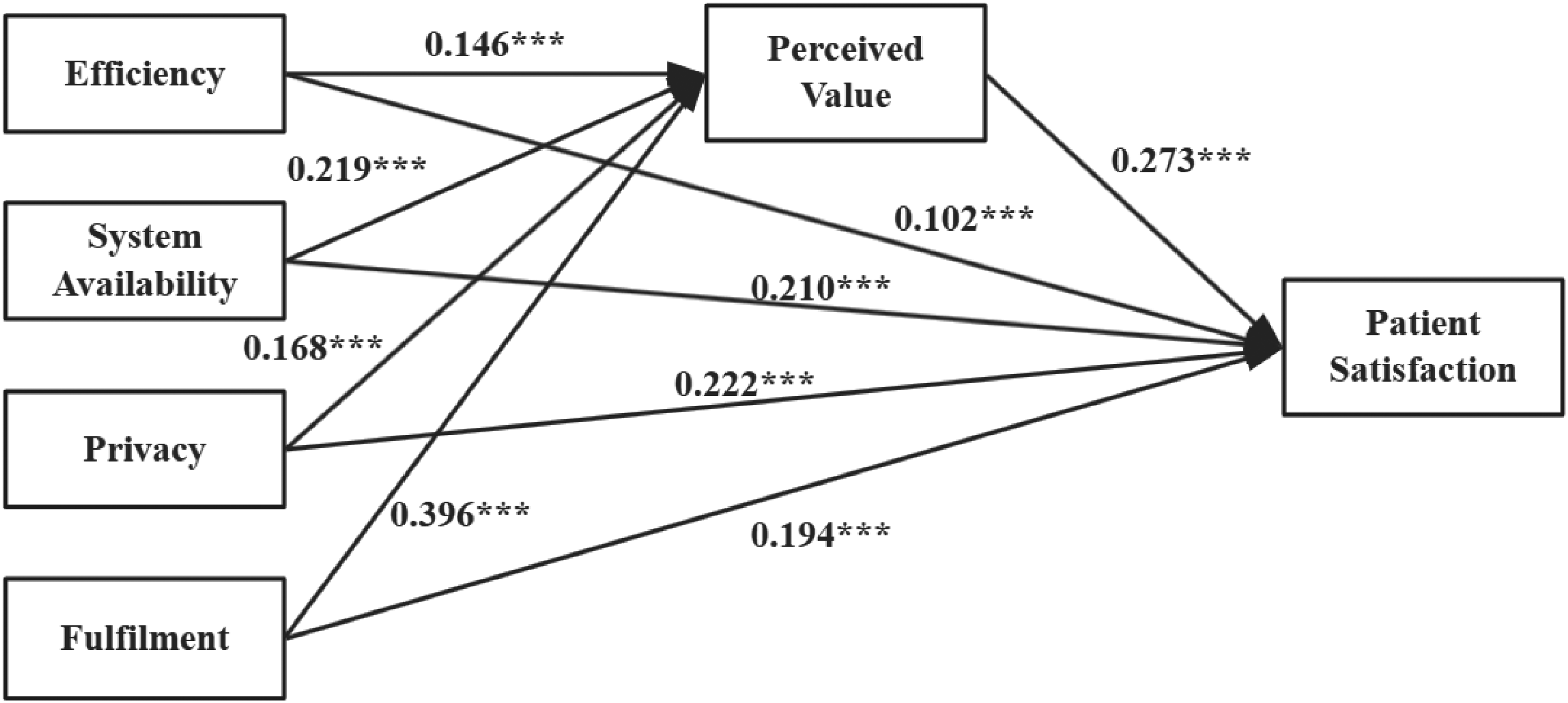
Direct path effect results of model 1.
Direct path effect of model 1.
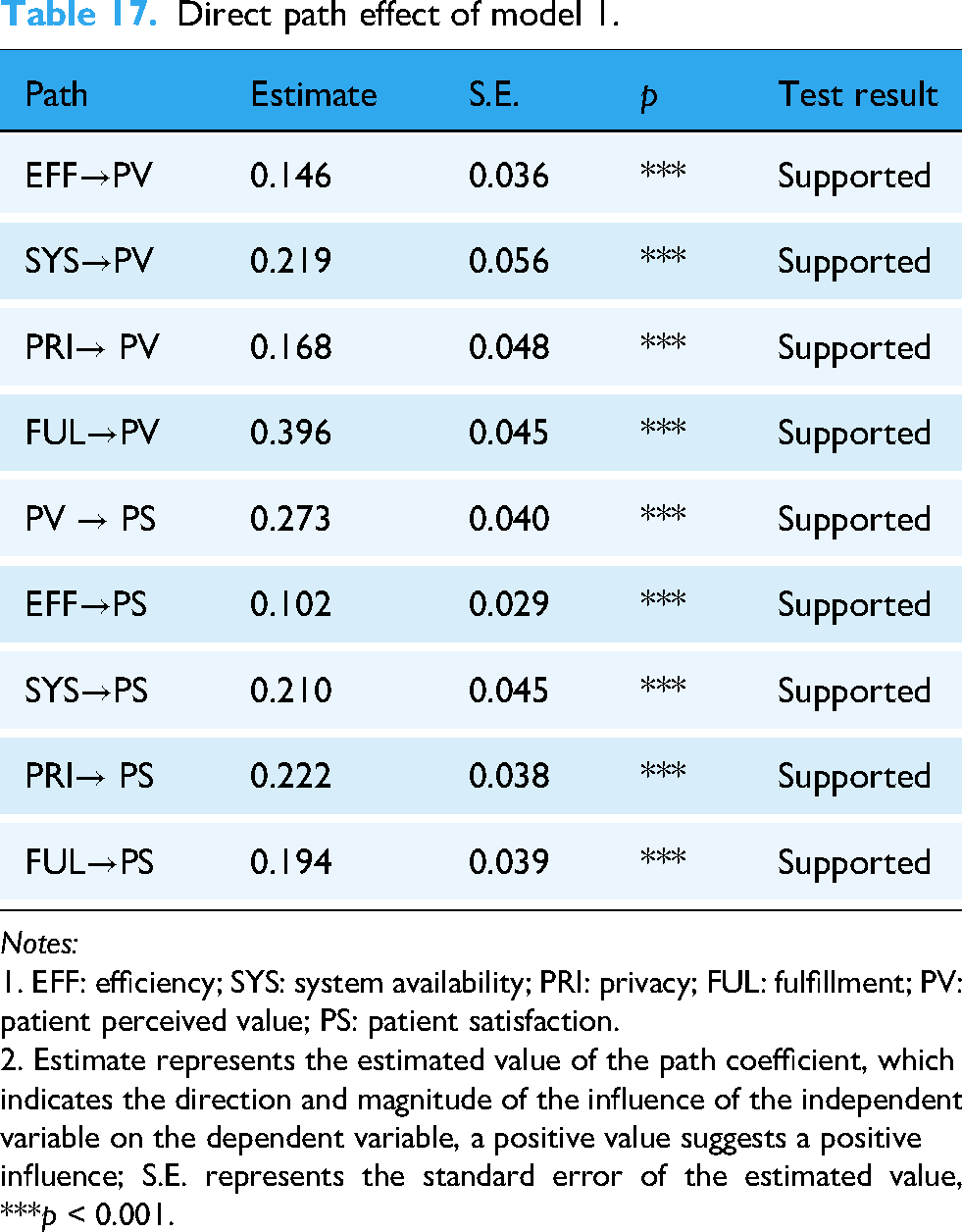
Notes:
1. EFF: efficiency; SYS: system availability; PRI: privacy; FUL: fulfillment; PV: patient perceived value; PS: patient satisfaction.
2. Estimate represents the estimated value of the path coefficient, which indicates the direction and magnitude of the influence of the independent variable on the dependent variable, a positive value suggests a positive influence; S.E. represents the standard error of the estimated value, ***p < 0.001.
First, regarding the direct effects of SQ dimensions on PS, efficiency (β = 0.102, p < 0.001), system availability (β = 0.210, p < 0.001), privacy (β = 0.222, p < 0.001), and fulfillment (β = 0.194, p < 0.001) all demonstrated significant positive effects on PS, supporting hypotheses H1a, H1b, H1c, and H1d. Among them, the direct effect of privacy on satisfaction is the strongest, reflecting the high sensitivity and importance that patients place on data security in the digital healthcare environment.
Second, regarding the direct effects of SQ dimensions on PV, efficiency (β = 0.146, p < 0.001), system availability (β = 0.219, p < 0.001), privacy (β = 0.168, p < 0.001), and fulfillment (β = 0.396, p < 0.001) all exhibited significant positive effects, supporting hypotheses H2a, H2b, H2c, and H2d. Among them, the effect of fulfillment is the most prominent, indicating that the completeness of service functions and the relevance of recommendations are key to enhancing patients’ overall value perception.
Finally, PV demonstrated a significant positive effect on PS (β = 0.273, p < 0.001), supporting hypothesis H3. This indicates that PS is not only dependent on the service itself but is also driven by their subjective perception of the service's value.
Direct path effects analysis for model 2
After verifying the impact of the objective SQ dimensions of intelligent consultation guidance services on PS in Model 1, this study further incorporated patients’ subjective feelings and psychological evaluations, namely service encounter experience, emotions, and PV, to construct the PEDM (Model 2). Unlike Model 1, which focuses primarily on the SQ itself, Model 2 emphasizes the psychological experience of patients during service reception. It delves into how service encounters influence PS through emotions and PV, thereby complementing and expanding the understanding of the mechanisms underlying PS formation.
This study constructed a SEM using AMOS 28.0 to examine the relationships among the three dimensions of service encounter (SIE, SRE, and SSE), PV, emotions (PPE and PNE), and PS.
Table 18 and Figure 5 present the estimated values and significance levels of each path in Model 1. Based on the model results, the path effects are explained in detail as follows:
Direct path effect results of model 2.
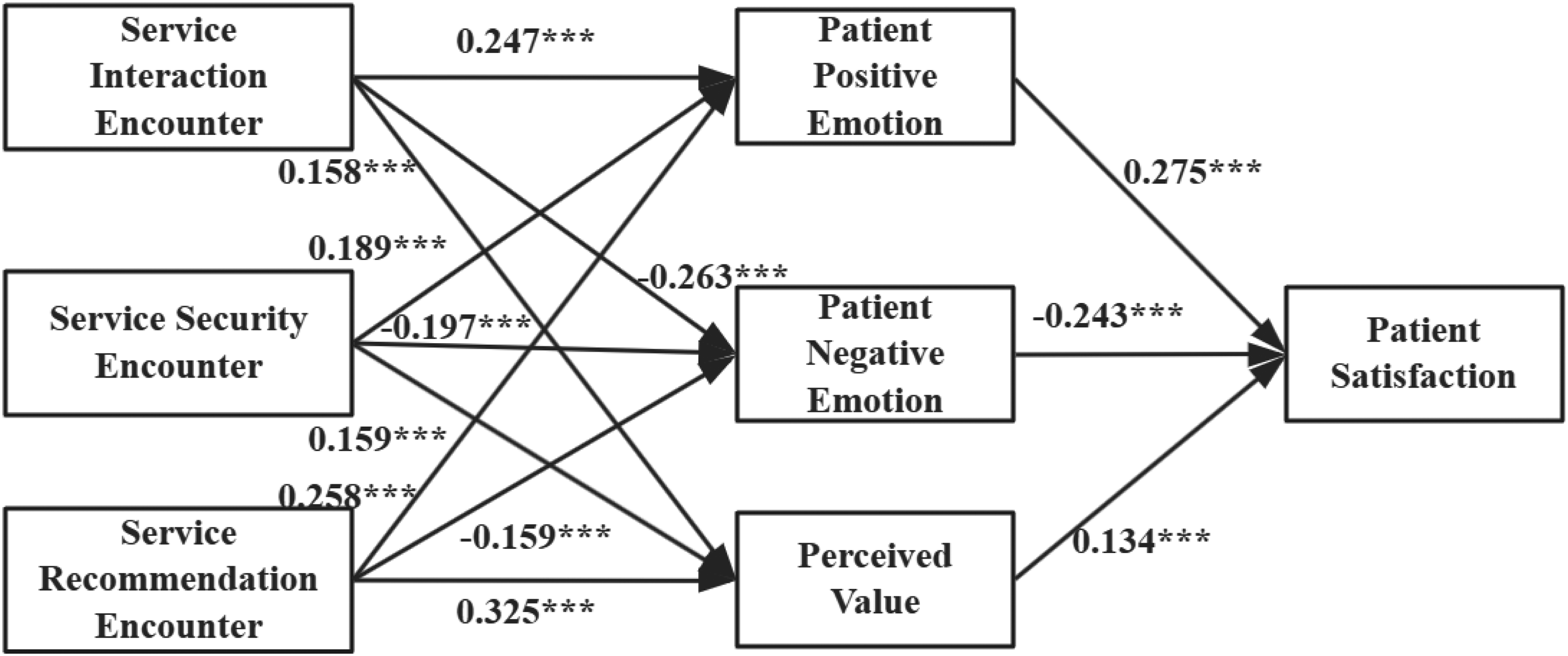
Direct path effect of model 2.

Notes:
1. SIE: service interaction encounter; SSE: service security encounter; SRE: service recommendation encounter; PPE: patient positive emotion; PNE: patient negative emotion; PV: patient perceived value; PS: patient satisfaction.
2. Estimate represents the estimated value of the path coefficient, which indicates the direction and magnitude of the influence of the independent variable on the dependent variable, a positive value suggests a positive influence; S.E. represents the standard error of the estimated value, ** p < 0.01, ***p < 0.001.
First, regarding the direct effects of service encounter on emotions, SIE (β = 0.247, p < 0.001), SSE (β = 0.189, p < 0.001), and SRE (β = 0.258, p < 0.001) significantly enhanced positive emotions, supporting hypotheses H4a, H4b, and H4c. Among them, the effect of SRE is the most significant, indicating that the accuracy and relevance of the intelligent consultation content play the most critical role in enhancing patients’ emotions. At the same time, these dimensions had significant negative effects on negative emotions, with β values of −0.263, −0.197, and −0.151, respectively (p < 0.001), supporting hypotheses H5a, H5b, and H5c. Among them, the effect of SIE is the most significant, suggesting that a good interaction experience can minimize patients’ negative emotions to the greatest extent.
Second, regarding the direct effects of service encounter on PV, SIE (β = 0.158, p < 0.001), SRE (β = 0.325, p < 0.001), and SSE (β = 0.159, p < 0.01) all had significant positive effects, supporting hypotheses H6a, H6b, and H6c. Among them, SRE had the most significant impact. This indicates that patients place particular importance on the accuracy and relevance of the recommendations during the intelligent consultation guidance process, which serves as the core basis for their value judgment.
Finally, for the direct effects of PV and emotions on PS: PV had a significant positive effect on PS (β = 0.134, p < 0.001), supporting hypothesis H7. Positive emotions (β = 0.275, p < 0.001) had a significant positive effect on PS, supporting hypothesis H8. Negative emotions (β = −0.243, p < 0.001) had a significant negative effect on PS, supporting hypothesis H9. These results indicate that positive emotions and PV significantly enhance PS, while reducing negative emotions is key to improving the patient experience.
Mediation effect analysis for model 1
To further elucidate how the SQ of intelligent consultation guidance services in internet hospitals influences PS through PV, merely verifying the direct relationships between the dimensions of SQ and PS is insufficient. Therefore, this study introduced PV as a mediating variable to explore whether the various dimensions of SQ indirectly affect PS by enhancing PV.
According to the mediation effect testing procedure proposed by Wen et al., a prerequisite for mediation analysis is a significant correlation between the independent variable and the dependent variable. 115 Based on the previous analysis, Model 1 satisfies the conditions for mediation effect testing.
This study employed the Bootstrap method to test the mediating effects, with the number of bootstrap samples set at 5000 and the confidence interval at 95%. Specifically, the Bootstrap method yields a 95% confidence interval for the mediating effect (where BootLLCI represents the lower limit of the confidence interval and BootULCI represents the upper limit). If this interval does not include zero, it indicates that the mediating effect is significant. The results are shown in Table 19.
Mediation effect test of model 1.

Note: EFF: efficiency; SYS: system availability; PRI: privacy; FUL: fulfillment; PV: patient perceived value; PS: patient satisfaction.
The findings indicate that PV plays a significant mediating role in the relationships between the four dimensions of SQ (EFF, SYS, PRI, and FUL) and PS, supporting hypotheses H3a, H3b, H3c, and H3d.
Mediation effect analysis for model 2
To more comprehensively reveal the mechanisms through which the experience of intelligent consultation guidance services affects PS, examining only the direct path relationships between service encounter dimensions and satisfaction is insufficient. This study further introduced patient emotions and PV as mediating variables to explore how different types of service encounters indirectly influence PS through emotions and value perception. This analysis not only helps identify the deeper psychological mechanisms in the formation of PS but also provides more operational suggestions for optimizing the design of internet medical services.
Consistent with the approach in Model 1, this study employed the Bootstrap sampling method for testing mediating effects, with the number of bootstrap samples set at 5000 and the confidence level at 95%. The results are presented in Table 20.
Mediation effect test of model 2.

Note: SIE: service interaction encounter; SSE: service security encounter; SRE: service recommendation encounter; PPE: patient positive emotion; PNE: patient negative emotion; PV: patient perceived value; PS: patient satisfaction.
The findings reveal that the three dimensions of service encounter (SIE, SSE, and SRE) significantly influence PS through the mediation effects of positive and negative emotions, supporting hypotheses H8a, H8b, H8c, and H9a, H9b, H9c.
In summary, this study systematically revealed the impact pathways between the SQ of intelligent consultation guidance services and PS through the validation of two models. In Model 1, we confirmed the mediating role of PV between the four dimensions of SQ and satisfaction, thereby fulfilling research objective (1). Model 2 further elucidated how service encounters influence satisfaction through emotions and PV, thereby supporting research objective (2). Both models were validated through SEM and Bootstrap sampling methods, ensuring the robustness of hypothesis testing, which corresponds to research objective (3). The theoretical and managerial implications will be elaborated in the subsequent discussion section to address research objective (4).
Discussion
This study systematically explored how intelligent consultation guidance services in internet hospitals influence PS using a dual-model framework that incorporates SQ and service encounter dimensions. By introducing PV and emotions as mediators, the study revealed direct and indirect pathways of impact, enhancing the robustness of conclusions and providing theoretical and practical guidance for optimizing internet medical services.
The research results indicate that the core dimensions of intelligent consultation guidance SQ in internet hospitals (efficiency, system availability, privacy, and fulfillment) all have a significant positive impact on PPV and satisfaction. Among these, fulfillment (β = 0.396, p < 0.001) has the most significant impact on PPV, while privacy (β = 0.222, p < 0.001) has the most prominent effect on satisfaction. Unlike the traditional “reliability” and “empathy” dimensions in offline healthcare services, which typically serve as key predictors of satisfaction,116,117 this study finds that the fulfillment of online intelligent consultation guidance and privacy protection has become the core factors influencing patient perceptions and satisfaction. This shift is due to the absence of doctor–patient interaction and the lack of tangible environmental cues in the intelligent consultation scenario, which makes patients more reliant on the completeness of the information provided by the platform and the security of their data. In the context of information asymmetry, fulfillment helps alleviate uncertainty by improving the accuracy of recommendations and the closure of the service loop, playing a key role in helping patients “understand themselves and find direction.” This viewpoint is further supported by Major's research, which suggests that reducing patient uncertainty can significantly enhance their PV and evaluation of healthcare services. 118 Privacy, as the most critical factor affecting satisfaction, reflects a shift in how users build trust in the platform—from offline interpersonal trust to focusing on system security. This aligns with Alhammad et al.'s findings in mHealth research, 119 which also indicate that in the absence of doctor–patient communication, patients’ sense of security largely comes from institutional guarantees rather than emotional interactions. These findings suggest that, in the design of intelligent healthcare services, the most predictive variables are no longer interpersonal interaction dimensions, but rather the technological and institutional capabilities of the system, such as “Can the system get it right?” and “Is the platform secure?” This shift also reflects the transition from the “relationship trust-service encounter” chain in offline healthcare to the “system trust-recommendation fit” in online healthcare. This structural change also places new demands on the design of online healthcare services, emphasizing the establishment of trust through data accuracy and security transparency, replacing the role of “doctor–patient communication” in traditional healthcare.
The introduction and validation of the PEDM is another important innovation of this study. This model breaks through the traditional SQ assessment paradigm in two ways: first, it is the first to incorporate emotional experience into the evaluation system of intelligent healthcare services, breaking the limitation of past research that focused solely on functional indicators; second, it provides a more detailed classification of service encounter dimensions, enabling a more precise portrayal of the patient experience. In traditional offline healthcare services, service encounters usually center on face-to-face interpersonal interaction.120,121 However, in the intelligent consultation scenario, patients’ service experience relies more on system performance and process guidance. In this context, the smoothness of interaction design and the personalization of recommendations not only significantly affect patient emotions but also largely shape their perception of service value. Therefore, this model places the patient experience at its core, dividing the intelligent consultation process into three key dimensions of service encounter: SIE, SSE, and SRE, thus covering the main touchpoints in the user-system interaction.
The study found that SRE not only significantly enhances positive emotions (β = 0.258, p < 0.001) but also has the strongest positive impact on PV (β = 0.325, p < 0.001). The difference in the size of this effect can be explained by the decision-making psychological process of patients. In the intelligent consultation service, patients often face uncertainty when selecting departments and doctors. At this point, precise recommendations can directly enhance their trust and confidence in medical decisions, thus eliciting positive emotions such as trust and enjoyment. In terms of PV, accurate recommendations not only help patients reduce decision-making difficulties but also make them feel that the recommendations are highly aligned with their needs, enhancing their overall value perception of the healthcare service. From a psychological perspective, the accuracy of recommendations influences patients’ cognitive assessments and emotional reactions. Accurate recommendations more directly meet patients’ needs, thereby having a more significant impact on emotions and value perception. Meanwhile, the significant inhibitory effect of SIE on negative emotions (β = −0.263, p < 0.001) reveals the key role of good human–computer interaction in reducing patient anxiety, consistent with Zhong et al.'s research. 122 These results further reveal that in intelligent consultation guidance services, “encounter experience” not only affects patients’ immediate emotions but also influences their overall evaluation of the service through the “cognitive processing” process.
Therefore, we further explore the key role of PV and emotions as mediating variables between service encounters and satisfaction. The study results show that PV is not only directly influenced by SQ and service encounter dimensions but also plays a mediating role between them and satisfaction. This finding supports Gómez-Carmona et al.'s research, which suggests that enhancing patients’ PV of the service can effectively improve PS. 123 Moreover, emotional variables also play a critical role in this process, especially the mediating role of positive and negative emotions between service encounters and satisfaction. Positive emotions directly promote PS by enhancing trust and the experience of using the service, while the reduction of negative emotions significantly alleviates patients’ dissatisfaction. This aligns with the hypothesis proposed by Heyn et al., which states that patients, guided by positive emotions, may form a more favorable evaluation of the service experience. 124 These findings also validate Manthiou et al.'s experimental results under the service encounter theory framework, further emphasizing the importance of emotional management in enhancing patient experience. 125 Overall, internet hospitals can improve PPV and satisfaction by optimizing SQ, service encounters, and emotional management, thereby achieving a better patient experience.
In conclusion, in traditional offline healthcare, service encounters more often rely on doctor–patient communication, empathy, and trust to build satisfaction. However, this study finds that in online scenarios, the key factors determining patient emotions and satisfaction lean more toward “how smooth the interaction is,” “how accurate the information is,” and “how trustworthy the system is.” This structural difference suggests that the optimization focus of digital healthcare services should shift from emotional relationships to process experience and security guarantees.
Theoretical implications
The theoretical contributions of this study to the field of intelligent healthcare services are reflected in the following three aspects:
First, this study extends the application of the E-S-QUAL model in the context of intelligent consultation guidance services, building upon existing SQ models. It also integrates service encounter theory and the S–O–R theory, proposing measurement dimensions and path mechanisms that better align with the characteristics of intelligent consultation guidance services. Previous studies using the E-S-QUAL model mostly focused on commercial fields such as e-commerce and online banking. For instance, Zia et al. used the E-S-QUAL model to measure e-commerce SQ, 86 and de Melo et al. applied it to assess online shopping SQ. 126 Although the dimensional structure is generally similar, specific indicators often need to be adjusted due to the differences in service scenarios. This study, based on the characteristics and service process of intelligent consultation guidance, redesigned the specific indicators for each dimension, thereby improving the explanatory power and adaptability of the model in the context of intelligent consultation guidance services. Additionally, previous studies based on the E-S-QUAL model mainly used single-path analysis to examine the direct impact of SQ on user satisfaction, such as Ahmed et al.'s use of the E-S-QUAL model to explore the single-path relationship between online banking SQ and customer satisfaction. 127 In contrast, this study, while exploring the “service quality-perceived value-satisfaction” path, integrates the S–O–R theory and service encounter theory, proposing the “PEDM.” It treats service encounters as “external stimuli,” PV and emotional variables as “organisms,” and satisfaction as the final “response.” This integration not only expands the explanatory ability of the SQ model regarding interaction mechanisms but also helps identify key influence paths in online healthcare services. For example, how the service fulfillment provided by the platform affects patients’ cognitive evaluations and emotional reactions, and how privacy protection translates into satisfaction through a sense of security. The theoretical framework of this study offers a more structured perspective on understanding online healthcare service experiences and provides an important reference for the application of the E-S-QUAL model in professional service contexts.
Second, this study expands the understanding of PPV in the context of internet healthcare, emphasizing the crucial role of emotions during service encounters. While previous research has explored the concept of PV and its impact on satisfaction, dedicated studies on internet hospital consultation services remain limited. Blut noted that PV has characteristics such as product differentiation, contextual differentiation, and dynamism, 128 which align with the high sensitivity of intelligent consultation guidance services to variations in user diseases, information needs, and the interaction process. This study emphasizes that PV should be seen as a core component of patients’ overall service evaluation, which will help future research gain a deeper understanding of the relationship mechanism between service encounters and value perception in the context of intelligent healthcare. Furthermore, this study further identifies the key mediating role of emotional variables in the “service encounter-satisfaction” path. The study finds that key touchpoints, such as service interaction, security, and recommendations during the intelligent consultation guidance process, continuously affect patients’ emotional states, thereby shaping their satisfaction. This result is consistent with Bradshaw et al.'s research, which states that service encounters continuously shape and influence patient emotions. 129 Notably, most service encounter dimensions have a stronger negative effect on negative emotions than their positive effect on positive emotions, indicating that negative experiences are more likely to trigger emotional fluctuations in patients. For instance, service crashes, information delays, or data security concerns can quickly trigger anxiety and dissatisfaction in patients, which then amplify the overall evaluation. Therefore, optimizing intelligent consultation guidance services should not only focus on creating positive value but also address the potential risk of negative emotions arising from poor experiences in key service encounters, which may lead to an amplified impact on the overall service evaluation.
Third, the use of a dual-model mutual validation methodology overcomes the limitations of using a single theoretical perspective to explain the satisfaction mechanism. By structurally validating the E-S-QUAL model and the PEDM, this study reveals the complementary relationship between technical indicators and emotional experiences in the assessment of internet healthcare SQ, further enhancing the reliability and theoretical adaptability of the findings. This approach provides a methodological paradigm for validating multipath mechanisms and has potential for application in other intelligent service scenarios.
Managerial implications
The research results provide the following four managerial implications for the optimization of Internet hospital services:
First, build symbolic capital to foster patient trust. Symbolic capital refers to intangible resources based on social recognition and symbolic meaning, including honor, reputation, status, and cultural identity. 130 In the online healthcare setting, patients cannot assess a doctor’s professionalism and credibility through traditional face-to-face interactions. Therefore, internet hospitals need to rebuild trust mechanisms through various methods. One way is for internet hospitals to establish a digital symbolic capital system to enhance the platform’s professional image and service credibility. For example, “Haodf Online” (www.haodf.com) builds a “social proof” mechanism for doctors through real-name authentication (such as medical qualifications, professional certifications, and facial recognition), reputation indicators (e.g., “Top Doctor of the Year”), and user behavior data (e.g., total number of patients, post-consultation ratings). Additionally, displaying the affiliation of doctors with top-tier hospitals or key departments (e.g., “Rehabilitation Medicine Department, Peking Union Medical College Hospital”) forms a dual symbolic capital structure of “platform certification + institutional endorsement.” The platform also publicly displays doctors’ service data and growth curves (e.g., service ratings, number of consultations completed), dynamically showing their professional accumulation and user recognition.
Second, stimulating positive emotions and controlling negative emotions. This study found that emotions play a key mediating role in the experience of intelligent consultation guidance services. Most service encounter dimensions have a stronger negative impact on negative emotions than a positive effect on positive emotions, suggesting that negative experiences are more likely to trigger emotional fluctuations and amplify their impact on overall service evaluation. Therefore, emotion management should address both the “stimulation” and “control” dimensions. On one hand, the platform can provide a more interactive and emotionally engaging service experience by introducing humanized interfaces (such as virtual assistants with facial expression feedback) and integrating large language models (LLM), thereby enhancing patients' sense of trust and enjoyment. On the other hand, attention should be given to improving user-system interaction and identifying and optimizing service touchpoints, such as high-risk moments such as page freezes, inaccurate recommendations, and complicated data entry. By simplifying the interface, providing feedback prompts, improving process guidance, and enhancing recommendation explanation mechanisms, frustration and anxiety during the usage process can be minimized, optimizing service touchpoint design and improving overall user experience.
Third, enhance service fulfillment to improve PPV. Service fulfillment is a key factor influencing PPV, encompassing all critical stages of the service chain in internet hospitals. To improve service fulfillment, a comprehensive service support system can be established across the preconsultation, consultation, and postconsultation stages. In the preconsultation stage, optimize consultation prompts and guidance by providing real-time push notifications, such as department navigation and waiting time reminders, to help patients plan their time and reduce waiting anxiety. Additionally, offer operational guides and a “large-font” interface for first-time users and elderly patients to lower accessibility barriers. Proactively push health knowledge and precautions to give patients a clear understanding of the diagnostic and treatment process. In the consultation stage, strengthen doctor–patient communication and humanistic care by conducting emotional management training for medical staff and customer service personnel. Ensure they communicate with patients using a gentle tone and encouraging language to provide positive emotional support. In the postconsultation stage, enhance follow-up management by pushing personalized educational articles. Establish patient communities and communication platforms to promote experience sharing and exchanges among patients, and offer consultations with mental health experts to help patients manage their emotions. Additionally, link follow-up data with EMR to improve the completeness and continuity of information during follow-up visits.
Finally, strengthen privacy protections to reduce security concerns. Privacy protection, a critical touchpoint, directly influences patient trust. Platforms must implement robust data security mechanisms and use visual tools (e.g., privacy notices, user consent prompts) to communicate these measures. Regular updates and transparent disclosures reduce negative emotions, fostering trust.
Limitations and future research directions
This study identifies limitations for future research to address:
First, the data collection relied on surveys and offline methods, with a limited sample size. Employing web-scraping techniques to gather user reviews from online health communities could expand the dataset and improve objectivity.
Second, the study focused solely on patients, neglecting perspectives from doctors and nurses, whose feedback is crucial for improving SQ. Future research should incorporate these key stakeholders to provide a more comprehensive analysis.
Third, regarding the variable design of the theoretical model, future research could further enrich the composition of mediating variables based on real-world scenarios. For example, by integrating patients’ actual experiences during the online service process, PV could be broken down into different dimensions, such as functional value, emotional value, and social value, to more comprehensively depict patients’ overall perception of intelligent healthcare services.
Finally, with advancements in LLMs like ChatGPT, future studies could investigate their applications in consultation guidance services. Large language models have the potential to transform such services into personalized medical assistants, offering empathetic support, understanding patient needs, and enhancing medical decision-making and health management.
Conclusions
This study investigates how AI-powered consultation guidance services in internet hospitals influence PS through both technical SQ and emotional experiences. The findings show that core SQ dimensionslefficiency, system availability, privacy, and fulfillment—significantly impact PS, with fulfillment and privacy being the most influential. Additionally, PV and patient emotions serve as mediators in shaping satisfaction.
The PEDM integrates service encounter theory and the S–O–R framework, revealing how service interactions, emotions, and PV influence satisfaction. Specifically, SREs have the strongest impact on both positive emotions and PV, while SIEs play a critical role in alleviating negative emotions and reducing patient anxiety.
Practical recommendations include building symbolic capital to enhance trust, improving emotional engagement through personalized interactions, enhancing service fulfillment at all stages of the patient journey, and strengthening privacy protections to foster patient confidence. These insights contribute to the design of future AI-driven healthcare services and offer guidance for optimizing patient experience in digital healthcare settings.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076251358673 - Supplemental material for How AI-powered consultation services in internet hospitals influence patient satisfaction: A structural analysis
Supplemental material, sj-docx-1-dhj-10.1177_20552076251358673 for How AI-powered consultation services in internet hospitals influence patient satisfaction: A structural analysis by Junkai Wang, Linru Fu, Zeguang Huang, Kan Hu, Zhizhuo Lin and Qiuhong Tang in DIGITAL HEALTH
Footnotes
Acknowledgements
This study owes a great deal to the patients who participated in the survey. Their sincere responses and assistance have been indispensable to the research's success. This study is a project approved by the Health Economics Association of Guangdong Province in 2024 (NO.2024-WJMF-06).
Ethical considerations
This study was approved by the Academic Committee of the School of Business Administration at Guangxi University.
Author contributions
Junkai Wang: Conceptualization and writing—original draft. Linru Fu: Writing—original draft. Zeguang Huang: Data curation and Investigation. Kan Hu: Data curation and investigation. Zhizhuo Lin: Data curation and investigation. Qiuhong Tang: Writing—review & editing.
Funding
The authors did not receive support from any organization for the submitted work.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data for the study are available upon reasonable request from the corresponding author.
Supplemental material
Supplemental material for this article is available online.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
