Abstract
Background
Adopting electronic health records (EHR) is critical for improving healthcare efficiency, yet implementation remains inconsistent, particularly in developing countries. This study applies a scoping review approach to evaluate the macro-environmental factors influencing EHR adoption in Tanzania using the PEST (Political, Economic, Social, and Technological) analysis framework.
Objectives
This study explores the adoption of EHR systems in Tanzanian healthcare using the PEST analysis framework to identify macro-environmental factors influencing implementation.
Methods
A scoping review methodology was employed, examining 35 studies published between 2010 and 2024. A comprehensive search was conducted in Scopus, PubMed, JSTOR, and Emerald. Reference lists of relevant studies were also reviewed for additional sources. Data were systematically extracted using a standardised framework categorising studies under political, economic, social, and technological domains. Thematic synthesis was applied to identify key patterns.
Results
The review included 35 studies, highlighting that political inconsistencies, economic constraints, social resistance, and technological limitations hinder EHR adoption. Key barriers include weak policy enforcement, unsustainable funding, workforce resistance, and poor ICT infrastructure. However, potential solutions such as strengthening governance frameworks, leveraging public–private partnerships, targeted digital literacy training, and improving ICT infrastructure were identified.
Conclusion
This study provides valuable insights into the macro-environmental challenges affecting the adoption of EHR systems in Tanzania. Addressing these barriers through a comprehensive policy and infrastructure development strategy is critical to ensuring successful digital health transformation.
Keywords
Introduction
The adoption of electronic health record (EHR) systems has been widely recognised as a transformative approach to enhancing healthcare delivery and improving clinical decision-making worldwide.1–3 These systems are designed to collect, store and manage patient information electronically, replacing traditional paper-based methods and offering a range of benefits, such as improved data accuracy, streamlined workflows and enhanced decision support for healthcare providers. 4 EHR systems can improve patient access and support timely clinical decisions, reduce medical errors and improve overall healthcare outcomes by enabling better access to patient information.5,6 Despite their potential, implementing and optimising EHR systems remains complex, particularly in developing countries like Tanzania, where healthcare systems face unique structural and contextual challenges.7–9
In Tanzania, the government has prioritised digitising healthcare services as a key component of its broader strategy to strengthen the health system. The Digital Health Investment Roadmap (2017–2023) and the Tanzania National eHealth Strategy have laid the foundation for integrating Information and Communication Technologies (ICT) into healthcare delivery,10,11 emphasising the adoption of EHR systems. These initiatives have facilitated the rollout of EHR systems in various healthcare facilities, particularly within primary healthcare settings. However, the adoption of EHR systems remains inconsistent, with notable disparities in functionality, user uptake and system performance between urban and rural healthcare facilities. 8 While some district hospitals and health centres in urban areas have achieved moderate success in implementing EHR systems, many rural facilities continue to struggle with challenges such as poor infrastructure, inadequate internet connectivity and limited technical expertise among staff.
Building on these efforts, the Government of Tanzania Hospital Management Information System (GoTHOMIS) has emerged as the primary EHR system used across healthcare facilities. According to the President's Office – Regional Administration and Local Government (PORALG), 12 4820 healthcare facilities in Tanzania – accounting for 66.57% of all healthcare facilities – currently use GoTHOMIS. These include 185 district hospitals (99.47% coverage), 836 health centres (90.67%) and 3778 dispensaries (61.71%). However, adoption remains particularly low in smaller clinics, with only three clinics (30% coverage) utilising the system. While the widespread implementation of GoTHOMIS represents a significant step toward digital transformation, the uneven adoption across different facility levels highlights the need for targeted interventions to improve EHR systems uptake in underrepresented areas, particularly through investment in infrastructure, staff training and technical support.
Understanding the factors influencing the adoption and sustainability of EHR systems requires a comprehensive analysis of the broader macro-environmental context in which these systems are implemented.13–15 EHR systems are not isolated; their success depends on various external factors influencing their design, deployment and use.16,17 These factors include political priorities, economic constraints, social acceptance and the availability of suitable technologies. A PEST (political, economic, social, and technological) analysis provides a structured framework to evaluate these external factors systematically. 18 This approach examines the political, economic, social and technological dimensions of EHR system adoption and offers valuable insights into the challenges and opportunities that can shape the success of EHR system implementation efforts.
From a political perspective, the adoption of EHR systems is shaped by government policies, regulatory frameworks and the allocation of resources. 19 Strong policy support and effective governance mechanisms are critical for ensuring that EHR systems align with national health priorities and that implementation efforts receive the necessary funding and oversight. 15 Economic factors, such as the cost of procurement, implementation and maintenance and the availability of financial support from development partners, also play a significant role in determining the feasibility of EHR systems projects.20,21 On the social front, user acceptance, cultural attitudes toward technology and the capacity of healthcare providers to adapt to digital systems influence the success of EHR system adoption.22–24 Finally, the technological environment, including ICT infrastructure, system interoperability and access to reliable power and internet connectivity, determines the operational efficiency of these systems.25,26
Despite the growing global shift toward digital health, the adoption of EHR systems in Tanzania remains uneven, and it faces unique contextual challenges. While previous studies have explored general barriers to EHR systems implementation,7,27 there is limited research that systematically examines the macro-environmental factors influencing adoption through a structured framework like PEST. This study addresses this gap by holistically understanding how political, economic, social and technological factors impact EHR systems adoption. The findings contribute to academic discourse and policy formulation, offering evidence-based recommendations relevant to Tanzanian healthcare.
This paper applies the PEST analysis framework to evaluate the macro-environmental factors affecting EHR systems adoption in Tanzanian healthcare facilities. Through a systematic literature review, the study identifies critical barriers and enablers across the political, economic, social and technological domains. The findings are expected to offer actionable recommendations for policymakers, healthcare administrators and other stakeholders working to foster a supportive environment for EHR systems adoption. Furthermore, this study contributes to the broader discourse on digital health transformation in developing countries, providing insights that can guide future initiatives to enhance healthcare delivery through technology. By highlighting macro-environmental challenges and leveraging opportunities, this paper underscores the importance of strategic planning to ensure the effective and sustainable adoption of EHR systems in Tanzania.
PEST analysis framework
The PEST analysis framework is a strategic tool to assess external macro-environmental factors influencing organisational decision-making and implementation processes. 28 PEST analysis offers a structured approach to understanding the broader contextual dynamics affecting various sectors, including healthcare, by categorising these factors into political, economic, social and technological domains. 29 In the context of this review, PEST analysis serves as a lens to examine the multifaceted influences on the adoption and sustainability of EHR systems in Tanzanian healthcare facilities. Figure 1 illustrates the PEST analysis framework, categorising macro-environmental factors into four domains: political, economic, social and technological.

The PEST analysis framework adapted from Sousa and Castaneda. 28
Political factors encompass government policies, legal and regulatory frameworks, political stability and institutional support, significantly impacting EHR systems adoption. For instance, national health policies and data protection regulations are crucial in shaping implementation efforts. 30 A study by Pham et al. 31 highlights how supportive government policies can facilitate the successful integration of EHR systems in healthcare settings.
Economic factors focus on financial constraints, funding mechanisms and cost-benefit considerations related to EHR systems. Resource allocation, maintenance costs and financial support from donors or public–private partnerships are critical. 32 World Health Organization emphasises that adequate funding and economic incentives are essential to implement EHR systems effectively. 33
Social factors include workforce readiness, cultural attitudes toward digital health tools and the training and education of healthcare providers. 34 These elements determine user acceptance and stakeholders’ adaptability to EHR systems.35,36 A study by Mwogosi and Kibusi 6 indicates that healthcare providers’ perceptions and attitudes toward EHR systems significantly influence their adoption and utilisation.
Technological factors examine ICT infrastructure, system interoperability, data security and the availability of technical expertise. 37 Robust technological ecosystems are critical for ensuring the efficiency and effectiveness of EHR systems.38,39 Kabukye et al. 40 discuss how technological readiness, including infrastructure and technical support, is vital for successfully deploying EHR systems.
Methodology
This review uses the PEST analysis framework to investigate the macro-environmental factors influencing the adoption of EHR systems in Tanzanian healthcare facilities. A scoping review methodology was employed to systematically synthesise available evidence, ensuring a comprehensive exploration of relevant studies and their implications for EHR systems adoption.
Research design
The scoping review methodology, as outlined by Arksey and O’Malley, was chosen due to its suitability for exploring complex and broadly defined topics. 41 This approach involves several stages, including defining the research questions, identifying and selecting relevant studies, extracting and charting data and synthesising findings to address the research objectives.42–44 The PEST framework served as the analytical lens, allowing for a structured examination of the political, economic, social and technological factors influencing EHR adoption. PEST analysis is a long-established methodology commonly applied ‘for understanding the external macro-environment in which an organisation operates’. 45 No formal protocol was pre-registered for this review. Future studies should consider protocol registration in platforms like PROSPERO for enhanced transparency and reproducibility.
Research questions
The review was guided by the following research questions, which were systematically addressed within the PEST framework. These questions are presented in Table 1 for clarity.
Research questions.

Source: Developed by authors based on study objectives and PEST framework.
Search strategy
A comprehensive search of academic databases, including Scopus, PubMed, JSTOR and Emerald, was undertaken to identify relevant literature systematically. This approach aimed to locate peer-reviewed journal articles, government reports and grey literature pertinent to adopting Electronic EHR systems in Tanzania. The search incorporated a range of carefully selected keywords and phrases to ensure a broad yet targeted scope. These search strings included terms such as ‘Electronic Health Records’, ‘EHR systems adoption in Tanzania’, ‘PEST analysis’, ‘political factors’, ‘economic barriers’, ‘social acceptance’ and ‘technological infrastructure’. To further enhance the comprehensiveness of the search, reference lists of relevant studies were manually reviewed, enabling the identification of additional literature through snowball sampling. Table 2 illustrates the search strings applied during the systematic review. Search filters were applied to include only peer-reviewed journal articles and government reports. Grey literature was considered if it provided substantial insights. The search was last updated in December 2024.
Search strings used in the study.

The search focused on publications released between 2010 and 2024, a period characterised by significant advancements in digital health initiatives in Tanzania. This timeframe was selected to include contemporary insights and developments relevant to the study's objectives. While the primary focus was on studies specific to Tanzania, literature from comparable settings was also considered, provided it offered significant insights that could apply to the Tanzanian context. This strategic approach aimed to capture the diverse and dynamic factors influencing the adoption of EHR systems, ensuring the robustness and relevance of the review.
Inclusion and exclusion criteria
The inclusion criteria required studies to focus on EHR systems or related digital health technologies within the Tanzanian context. Studies had to address macro-environmental factors relevant to the PEST framework and include sufficient detail on the political, economic, social or technological dimensions. Peer-reviewed journal articles, institutional reports and conference proceedings were included. Literature had to be published in English.
Studies that focused solely on internal organisational factors without reference to external influences were excluded. Moreover, studies that did not specifically address the Tanzanian context or lacked sufficient relevance to developing countries were excluded. Publications before 2010 were omitted to ensure the findings reflected contemporary developments in digital health technologies.
Study selection
Study selection followed a two-stage screening process. Initially, titles and abstracts were independently reviewed by two researchers to assess relevance. Full-text screening was conducted using predefined inclusion and exclusion criteria. Discrepancies between reviewers were resolved through discussion, and a third reviewer was consulted when necessary to reach a consensus. Inter-rater reliability was assessed using Cohen's kappa coefficient, with a score of 0.85 indicating a high level of agreement.
The study selection process was documented systematically to ensure transparency and replicability. A PRISMA flow diagram (Figure 2) outlines the progression of study selection, detailing the number of records identified, screened, reviewed in full and ultimately included in the analysis. This structured selection approach ensured that the final studies provided comprehensive insights into the external factors shaping the adoption of EHR systems in Tanzanian healthcare.

The study selection process follows the PRISMA guideline adapted from Page et al. 46
Data charting
Data were extracted using a standardised charting form (Table 3), including author, year, study focus, methodology, key findings and alignment with PEST categories. Two researchers independently conducted the charting, and discrepancies were resolved through discussion. The final dataset was reviewed to ensure consistency before thematic synthesis.
Data extraction template.

Data synthesis
The extracted data were analysed through a rigorous thematic synthesis process to identify recurring patterns, trends and themes within the political, economic, social and technological domains. Thematic analysis, as outlined by Braun and Clarke, 47 involves systematically coding qualitative data and grouping similar insights into broader themes. This approach was used to categorise challenges and enablers affecting EHR system adoption in Tanzania, ensuring that all macro-environmental factors were comprehensively addressed. These thematic insights provided a detailed examination of external factors shaping EHR systems implementation, offering actionable recommendations to guide policymakers and healthcare stakeholders.
Furthermore, a comparative analysis with global trends highlighted that the barriers encountered in Tanzania align with those reported in similar resource-limited settings. The synthesis of findings provided a holistic understanding of the multi-faceted nature of EHR systems adoption, emphasising the need for integrated policy frameworks and scalable ICT solutions to enhance healthcare delivery and decision-making processes.
Quality assessment
The quality of included studies was assessed using the Joanna Briggs Institute's critical appraisal tool, evaluating methodological rigour, data reliability and study relevance. Studies were scored based on criteria such as clarity of objectives, appropriateness of methodology and data validity. High-scoring studies (above 70%) were prioritised in the synthesis, while lower-scoring studies were reviewed for contextual insights. This process allowed for a structured evaluation of the evidence base, ensuring the review relied on credible, high-quality studies. Studies demonstrating greater methodological strength and relevance to the research objectives were prioritised during synthesis to enhance the robustness of the findings.
Figure 3 presents the quality assessment form used in this review. The form outlines the criteria applied to evaluate the studies, including methodological rigour, clarity of objectives and relevance to the PEST framework and Tanzanian context. Each criterion includes specific assessment questions, scored as either 1 (Yes) or 0 (No), to determine the quality and applicability of the study.
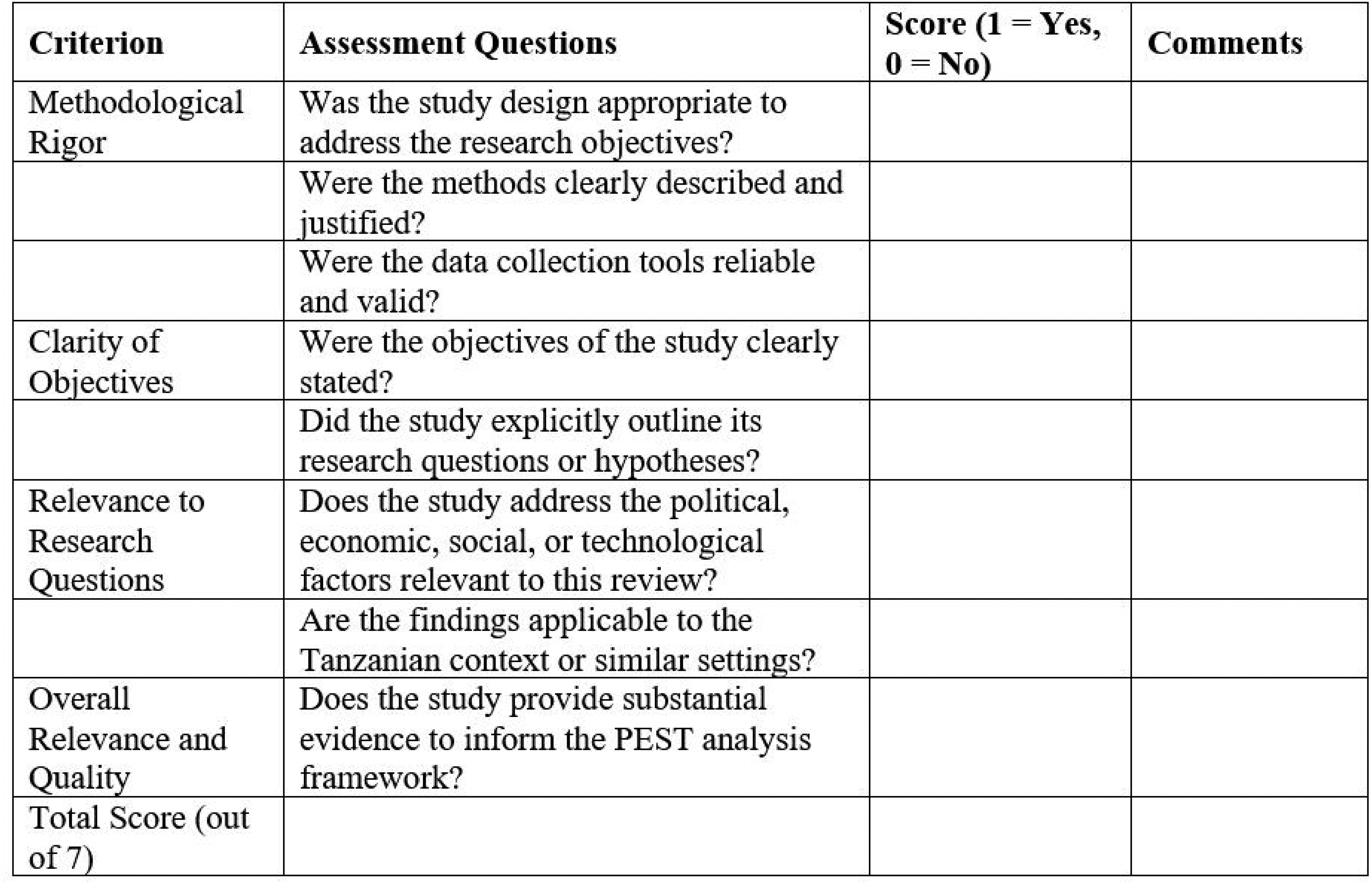
Quality assessment form.
Ethical considerations
Ethical approval was not required since the study involved a review of existing literature. Nonetheless, the review adhered to principles of academic integrity, including accurate citation of all sources and transparency in reporting findings. Efforts were made to ensure the analysis and recommendations were credible and replicable.
Results
Search results
The systematic search identified 523 studies from four databases: Scopus, PubMed, JSTOR and Emerald. After removing 167 duplicate records, 356 unique studies remained for screening. These studies were assessed based on their titles and abstracts, excluding 251 studies that did not meet the inclusion criteria. The remaining 105 studies underwent full-text review to determine their relevance to the research objectives.
Following the full-text screening, 70 studies were excluded due to reasons such as lack of alignment with the PEST framework (37 studies), insufficient focus on the Tanzanian context or comparable settings (22 studies) and absence of empirical findings (11 studies). This process resulted in the final inclusion of 35 deemed relevant studies for thematic synthesis. A PRISMA-ScR-compliant flow diagram (Figure 2) illustrates the study selection process, detailing the number of records identified, screened, reviewed and excluded, with reasons for exclusion. This enhances transparency and adherence to scoping review best practices.
Study characteristics
The 35 studies in this review demonstrated diverse characteristics regarding their focus areas, methodologies, geographic coverage and relevance to the PEST framework. Most studies (26 out of 35) were conducted within the Tanzanian healthcare system,6–8,48–71 while the remaining studies explored comparable settings in other developing countries, offering insights applicable to the Tanzanian context.70,72–76 These studies primarily addressed issues related to the adoption of EHR systems, with a specific emphasis on macro-environmental factors.
Regarding methodological approaches, quantitative studies were the most common in the included literature, accounting for 60% (21 studies).54–57,59,60,62,63,65,66,68–70,72,77,78 These studies employed statistical analyses to assess the impact of specific macro-environmental factors, such as financial constraints and technological readiness. Qualitative studies comprised 31.4% (11) and predominantly used interviews, focus groups and case studies to investigate the contextual factors influencing EHR systems adoption.7,48–50,52,58,61,64,67,71,73,79 The remaining 8.6% (3) were mixed-method studies, integrating qualitative and quantitative approaches to provide a more detailed understanding of EHR system implementation challenges and opportunities.6,8,53
The studies’ publication periods ranged from 2010 to 2024, aligning with the review's inclusion criteria. Most studies were published after 2015, reflecting the Tanzanian government's efforts to accelerate digital health adoption through the digital health investment roadmap (2017–2023) and the national eHealth strategy (2013–2018). Studies published before 2015 focused on early implementation challenges and the foundational stages of EHR systems in Tanzania, particularly in rural and resource-constrained settings.
Alignment with the PEST framework revealed that most studies concentrated on technological factors, encompassing challenges such as poor infrastructure, system interoperability and internet connectivity issues. Economic factors were the second most frequently addressed domain, explored, focusing on financial sustainability and resource allocation. Social factors included workforce training and stakeholder engagement, while political factors were examined in a few studies, highlighting gaps in policy enforcement and governance. Many studies spanned multiple PEST domains, reflecting the interconnected nature of these macro-environmental factors.
Themes synthesis
The findings from the reviewed studies provide a holistic understanding of the factors influencing the adoption and implementation of EHR systems and other digital health systems in Tanzania. These factors are analysed through the PEST framework, and Table 4 summarises them.
PEST framework summary.

Source: Authors work adapted from Sousa and Castaneda. 28
Political factors
Government leadership and policy frameworks emerged as central to adopting digital health systems. Many studies58,68,69 highlighted the importance of the Tanzanian Ministry of Health in shaping the strategic direction for EHR systems adoption through initiatives like the National eHealth Strategy and the Digital Health Investment Roadmap. However, inconsistent policy enforcement and weak regulatory frameworks were common challenges, particularly in data interoperability and privacy.59,67 Gaps in alignment between national policies and local needs further worsened fragmentation in implementation efforts.61,68 Figure 4 illustrates the distribution of studies addressing specific political factors influencing EHR systems adoption in Tanzania.

Distribution of studies addressing political factors in EHR systems adoption in Tanzania.
Several studies emphasised the need for robust governance mechanisms to address these challenges. For example, Mwogosi and Mambile (2024) suggested stronger accountability measures for data protection, while Dolan et al. (2020) called for better policy coordination between national and subnational levels. The role of international partners and donors in supporting policy formulation was also noted as critical in bridging resource gaps.52,80
Economic factors
Financial constraints were a recurring theme across the reviewed studies. Many facilities relied heavily on donor funding for the initial implementation of EHR systems, leaving sustainability uncertain once external support ceased.53,67 High costs associated with ICT infrastructure, training and system maintenance further strained healthcare budgets, particularly in rural settings.59,69 Studies like Mang’ana et al. 81 emphasised that limited financial planning at the national level compounded these challenges.
Despite these barriers, opportunities for financial sustainability were identified. Public–private partnerships were frequently recommended as a viable solution to offset costs and ensure long-term system viability.51,58 Open-source platforms were also suggested as cost-effective alternatives to proprietary systems. 64 Moreover, some studies highlighted the potential for EHR systems to reduce operational costs through improved efficiency and streamlined processes. 66 Figure 5 represents the distribution of studies addressing economic factors influencing the adoption of EHR systems in Tanzania.

Distribution of studies addressing economic factors in EHR systems adoption in Tanzania.
Social factors
Resistance to change among healthcare workers emerged as a critical social barrier. Limited training, low digital literacy and fears of increased workload were key contributors to this resistance.60,67 Studies like Nehemiah 57 noted that inadequate user involvement in system design further hindered acceptance. However, positive attitudes toward digital systems were observed when the benefits of these technologies, such as improved workflow and data accuracy, were demonstrated.7,62,69 Figure 6 represents the distribution of studies addressing economic factors influencing EHR systems adoption in Tanzania.

Distribution of studies addressing social factors in EHR systems adoption in Tanzania.
Capacity-building initiatives were highlighted as essential for overcoming social barriers. Many studies recommended targeted training programs, on-the-job mentorship and stakeholder engagement to build confidence and competency among healthcare workers.52,81 Involving end-users in system customisation and implementation was also suggested to enhance system usability and acceptance.51,64
Technological factors
Technological challenges, including unreliable electricity, limited internet connectivity and inadequate ICT infrastructure, were prominent across the studies.53,66 These issues were particularly pronounced in rural areas, where facilities often faced power outages and slow internet speeds. Furthermore, interoperability problems between different EHR systems created data silos and hindered seamless information sharing.58,61,78
Advancements in mobile technologies and cloud-based solutions were noted as promising opportunities to address these challenges.52,82 Offline functionalities and scalable ICT solutions were frequently recommended to enhance system usability in resource-limited settings.67,69 Furthermore, adopting standardised protocols and user-centred design principles was emphasised to improve system integration and user experience.57,83 Figure 7 represents the distribution of studies addressing economic factors influencing EHR systems adoption in Tanzania.

Distribution of studies addressing technological factors in EHR systems adoption in Tanzania.
Discussion
The adoption of EHR systems in Tanzanian healthcare facilities is influenced by a complex interplay of political, economic, social and technological factors. Using the PEST framework, this study provides insights into the external macro-environmental dynamics shaping EHR systems adoption and offers recommendations for policymakers and stakeholders. While Tanzania has made progress in digital health transformation through initiatives such as the National eHealth Strategy and the Digital Health Investment Roadmap, challenges remain in enforcement and interoperability. The findings align with Edward et al. 67 who emphasise that governance mechanisms must be strengthened to ensure a successful system rollout. Furthermore, as noted by Simba et al. 66 the reliance on donor-driven policies highlights the need for sustainable, locally tailored policy frameworks that align with Tanzania's long-term healthcare goals.
Financial constraints emerged as a significant challenge, particularly in rural and resource-limited settings, where infrastructure and maintenance costs strain healthcare facilities. Similar trends have been observed in other developing countries, where limited funding affects EHR adoption. While donor support has been crucial in initiating EHR systems, its long-term sustainability remains uncertain, as demonstrated by Dolan et al. 53 and Mang’ana et al. 81 Public–private partnerships and cost-effective alternatives, such as leveraging open-source platforms, offer viable solutions to alleviate financial burdens. These findings align with experiences in Ghana, Ethiopia and Mozambique, where innovative funding mechanisms have played a crucial role in ensuring continued adoption and system maintenance. 84
Resistance to change among healthcare workers remains a major barrier to EHR systems adoption, particularly in rural areas with low digital literacy levels. Studies in Nigeria, Ghana and Ethiopia have shown that user distrust and resistance often stem from concerns about workflow disruptions, data security and lack of technical skills. 85 In Tanzania, the findings of this study indicate that insufficient training and limited stakeholder engagement contribute to low system adoption rates. Msami et al. 60 and Ayebazibwe et al. 69 emphasise the importance of structured capacity-building initiatives, including targeted training and on-the-job mentorship, to foster user confidence and competency. Moreover, stakeholder engagement, particularly involving end-users in system customisation, is critical for enhancing usability and acceptance. These findings are consistent with studies in Nigeria, where a lack of training has fuelled digital distrust and slowed the adoption of electronic health services. 86
Technological challenges, including unreliable electricity, poor internet connectivity and limited ICT infrastructure, remain key barriers to EHR systems implementation, particularly in rural healthcare facilities. This study echoes the findings of Simba et al. 66 and Mkayula et al. 61 who highlight the negative impact of infrastructural limitations on EHR systems functionality. Interoperability issues further exacerbate these challenges, leading to fragmented data systems that hinder seamless healthcare delivery. However, advancements in mobile technologies and cloud-based solutions offer promising opportunities for overcoming these obstacles. Mwogosi 7 underscores the importance of offline functionalities and scalable ICT solutions tailored to resource-limited settings. Comparatively, Ghana has implemented mobile-based EHR solutions to address connectivity issues, 87 while Ethiopia has leveraged cloud-based platforms to enhance system scalability. 88 These experiences provide valuable lessons for Tanzania in developing context-specific strategies to strengthen its EHR systems infrastructure.
Beyond financial and technological barriers, the role of digital distrust in EHR systems adoption is gaining prominence. The study by Ezeudoka et al. 86 highlights that in Nigeria, resistance to e-health services among older adults is strongly influenced by perceived risks, low self-efficacy and anticipated regret. This aligns with the findings of Talwar et al., 85 which emphasise that resistance is not merely the absence of adoption but a manifestation of user concerns about privacy, system reliability and trust. In Tanzania, similar sentiments were observed among healthcare workers hesitant to transition from traditional record-keeping methods to digital systems. This suggests that addressing cognitive and psychological barriers through awareness campaigns, policy interventions and trust-building measures is essential for promoting widespread EHR systems adoption.
The findings of this study contribute to the broader discourse on digital health adoption in developing countries by providing a comparative perspective on resistance and adoption drivers. While financial, technical and regulatory challenges are common across Tanzania, Nigeria, Ghana and Ethiopia, variations in digital literacy, policy enforcement and socio-cultural perceptions shape the adoption landscape differently. Addressing these challenges requires a holistic approach integrating policy reforms, financial sustainability, workforce training and user-centred system design. By learning from the experiences of other African countries, Tanzania can refine its digital health strategies to enhance the adoption and effective utilisation of EHR systems.
The implications of this study are significant for the successful adoption and sustainability of EHR systems in Tanzanian healthcare settings. The study highlights the critical political, economic, social and technological factors that influence EHR systems implementation by applying the PEST framework. It underscores the importance of robust policy enforcement, sustainable financing mechanisms and targeted capacity-building initiatives to overcome resistance and ensure effective system use. Furthermore, the study emphasises the need for improvements in ICT infrastructure, particularly in rural areas, to address connectivity issues and support the scalability of EHR systems. The findings offer valuable insights for policymakers, healthcare administrators and stakeholders to create a conducive environment for EHR systems adoption, leading to improved healthcare delivery, enhanced data management and better clinical decision-making across Tanzania's healthcare facilities.
Study limitations
This study has certain limitations. Firstly, it relies on a scoping review of existing literature, which may not capture the most recent real-time developments in EHR systems adoption in Tanzania. While the review synthesises available evidence, it does not include primary data collection, limiting its ability to reflect emerging trends or rapidly evolving policies.
Secondly, the study did not register a formal protocol in databases such as PROSPERO. Protocol registration enhances methodological transparency and reduces the risk of bias, and future scoping reviews should consider this step to strengthen credibility and reproducibility.
Thirdly, excluding non-English literature might have led to the omission of relevant studies published in Swahili or other local languages, potentially limiting insights into region-specific challenges and perspectives on EHR adoption. Future reviews should explore multilingual databases or include translated sources to enhance inclusivity.
Furthermore, while the PEST framework provides a structured macro-environmental analysis, it does not fully capture micro-level organisational and individual factors influencing EHR systems adoption, such as healthcare workers’ personal attitudes, managerial decision-making and institutional readiness. Future research should incorporate frameworks such as SWOT (Strengths, Weaknesses, Opportunities and Threats) or the Technology Acceptance Model to address these aspects comprehensively.
Lastly, the reliance on secondary data sources means the review is subject to the quality and completeness of the included studies. Some studies may have methodological weaknesses or reporting gaps that could affect the robustness of the findings. Future research should consider empirical investigations, such as case studies, mixed-methods approaches and longitudinal analyses, to complement these findings and validate the proposed policy recommendations.
Conclusion
This study systematically examined the macro-environmental factors influencing adopting EHR systems in Tanzania using the PEST framework. The findings indicate that political inconsistencies, economic constraints, social resistance and technological limitations collectively hinder EHR systems adoption. The primary barriers identified are key policy gaps, lack of financial sustainability, inadequate digital literacy and interoperability challenges. However, opportunities exist through strengthening policy enforcement, fostering public–private partnerships, implementing targeted training programs and investing in scalable ICT solutions. Addressing these factors in an integrated manner is crucial for ensuring the adoption of sustainable EHR systems. Future research should explore more granular aspects of user engagement and conduct empirical case studies on successful implementations in similar settings. These insights will further support stakeholders in formulating evidence-based strategies for digital health transformation in Tanzania.
Recommendations
Based on the findings of this study, several actionable recommendations are proposed to enhance the adoption and sustainability of EHR systems in Tanzanian healthcare facilities. First, policymakers should strengthen the enforcement of existing digital health policies and create standardised guidelines for data interoperability across systems. Second, exploring innovative funding mechanisms, such as public–private partnerships, donor collaboration and open-source platforms, can improve financial constraints and ensure long-term sustainability. Third, comprehensive capacity-building programs should be implemented to improve digital literacy and reduce resistance among healthcare workers, focusing on training, mentorship and stakeholder engagement. Finally, significant investments in ICT infrastructure are needed, particularly in rural areas, to address unreliable electricity and internet connectivity challenges. By prioritising these recommendations, Tanzania can create a more supportive environment for EHR systems implementation, driving healthcare delivery and data management improvements.
Footnotes
Acknowledgements
The authors sincerely thank the University of Dodoma for providing invaluable support and resources throughout this study. The institution's commitment to fostering academic excellence and research innovation has been instrumental in the successful completion of this work.
Author contributions/CRediT
The contributions to this study are as follows: Augustino Mwogosi was responsible for conceptualisation, data analysis and manuscript drafting, while Cesilia Mambile contributed through an extensive literature review and critical revisions.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
