Abstract
Introduction
Diabetes is a major global health issue, requiring nursing interns to develop essential diabetes management skills. Traditional teaching methods are limited by clinical settings, hindering the development of comprehensive theoretical and clinical competencies. This study developed a Virtual Simulative Diabetes Care Program to address these limitations.
Methods
A quasi-experimental design was employed. Nursing interns were assigned to an intervention group (virtual simulation) or a control group (traditional face-to-face training). Self-directed learning ability and clinical thinking skills were assessed using the validated Independent Learning Ability Scale and Clinical Thinking Skills Scale. Pre- and post-intervention measurements were conducted, and data were analyzed using independent t-tests and Mann–Whitney U tests, with significance set at P < .05.
Results
The intervention group showed significantly higher self-directed learning ability (104.53 ± 7.75 vs. 99.00 ± 13.77, P < .05) and clinical thinking skills (99.71 ± 12.15 vs. 91.69 ± 17.44, P < .05) compared to the control group. Within the intervention group, both abilities significantly improved from pre- to post-internship (P < .05). Practical skills, including blood glucose monitoring and insulin injection, also improved, with higher scores in the intervention group. The virtual simulation program was rated as effective, with an overall score of 8.37 ± 1.20 and "Excellent" ratings for learning functionality.
Conclusions
The virtual simulation-based diabetes care program significantly improved nursing interns’ learning and clinical skills.
Introduction
Type 2 diabetes mellitus (T2DM), is a metabolic disorder characterized by chronic hyperglycemia. 1 With improvements in living standards and quality of life, the prevalence of diabetes has been steadily increasing, making it a globally prevalent disease. 2 According to statistics, in 2019, there were 536.6 million individuals worldwide suffering from diabetes, and by 2045, this number is projected to rise to 783.2 million, imposing a significant socio-economic burden and health threat to the global healthcare system. 3 Since T2DM not only affects the metabolic system but also leads to complications involving the cardiovascular, renal, nervous, and ocular systems, departments such as cardiology, nephrology, ophthalmology, and surgery must actively participate in the management and care of these complications. 4 The impact of T2DM extends beyond the realm of endocrinology, becoming a key focus across various clinical specialties. 5 Consequently, the management of T2DM represents an important area for multidisciplinary collaboration throughout the hospital. 6 For clinical nursing interns, mastering diabetes disease knowledge, nursing skills, and health education methods is essential. 7 In addition, nursing interns must be capable of providing health education to patients and their families, aiding in the patients’ long-term self-management. 8 Mastery of these skills not only enhances the quality of nursing care but also plays a crucial role in the treatment and rehabilitation of patients. 9
Virtual simulation is a computer-generated representation of specific clinical scenarios that provides an interactive, immersive, and simulated learning environment for nursing education. 10 This system integrates 3D simulation technologies with accessible web-based platforms, allowing learners to engage in scenario-based practice using devices such as computers, tablets, and smartphones. 11 The aim of this study was to create an experience that is comparable to that of a real environment, including feelings and experiences associated with networked, digital, and intelligent technical tools. 12 It incorporates elements of virtual reality, which is characterized by authenticity, interactivity, conceptualization, and immersion, and has been found to be highly acceptable and effective in nursing teaching and training. 13 It also has been widely used in nursing education, including surgical nursing, 14 emergency nursing, 15 and critical care nursing, 16 penetrating various teaching fields such as nursing theory, clinical skills, humanistic care, and comprehensive ability,17,18 enhancing their learning interest and training effect, and cultivating independent learning ability and clinical thinking ability. 19 The study demonstrated that virtual simulation teaching was more effective than traditional teaching methods in terms of interns’ evaluations of theoretical performance, operational skills performance, and teaching effectiveness. 20 Furthermore, virtual simulation can stimulate interns’ interest in learning and deepen their understanding of knowledge than traditional training methods. It is more capable of exercising interns’ ability to analyze problems, engage in self-study, develop clinical thinking, and foster communication and collaboration within teams. 21
Recent advancements have been made in the integration of virtual simulation technology into diabetes care training, particularly in developed countries such as the United States and the United Kingdom. The American Diabetes Association and the American Heart Association had partnered to launch "A1CVD Pro," a virtual patient simulation educational program to educate healthcare professionals about the cardiovascular complications of diabetes. 22 In the United Kingdom, Ritwika et al. developed a Diabetic Emergency Care: Virtual Interactive Clinical Education (DEVICE) software in which interns can assess patients for symptoms and deal with emergencies such as diabetic ketoacidosis, hyperosmolar hyperglycemic states. 23 Similarly, Hamid Taghinejad's research highlights the use of online gamification to enhance nursing students’ skills in electrocardiogram interpretation and self-directed learning, showcasing an innovative approach to virtual simulation in nursing education. 24 These initiatives demonstrate the emphasis placed on leveraging virtual simulation to enhance the preparedness of healthcare professionals in clinical operations. In contrast, the application of virtual simulation technology in nursing education within China remains limited. Current nursing training programs utilizing virtual simulation in China predominantly focus on areas such as maternal care, cancer care, stroke care, psychiatric-psychological care, and invasive procedures like nasogastric feeding, urinary catheterization, and venepuncture.25,26 While virtual simulation has been widely adopted to address these fields, its integration into diabetes care education is relatively underdeveloped. Notably, existing programs in China are often incorporated into general chronic disease management initiatives, lacking targeted training for nursing interns to acquire diabetes-specific knowledge and skills. 27
In order to address the limitations of traditional teaching methods, which were constrained by time, space, and resources, a virtual simulation-based program for teaching diabetes care (D training) was developed in this study.
Methods
Study design
This study was a single-center, single-blind, parallel-group randomized controlled study. Participants were enrolled in the trial and randomized to either the experimental group or the control group. The trial was registered at the Chinese Clinical Trial Registry (registration number: ChiCTR2300074996). Ethical approval for the study was obtained from the Ethics Committee of the Xiangya School of Nursing, Central South University (approval number: E202333).
Participants
The sample size was estimated using the formula for interventional studies: N1 = N2 = 2[(tα/2 + tβ)S/δ]2. 28 This study was designed as a two-sided test with α = .05, t0.05/2 = 1.96, β = 0.10, tβ = 1.28; where S represents the estimated standard deviation of the two populations, and δ is the difference between the two means. Based on the preliminary study results of self-directed learning ability (S = 1.01,δ = 1.19) and accounting for a 20% attrition rate, the minimum sample size required for each group was calculated to be 18 participants.
Potential participants were recruited using a convenience sampling method from the Second Xiangya Hospital of Central South University in Changsha, China, between July 2023 and January 2024. The inclusion criteria for the participants were as follows: (1) Nursing interns from the endocrinology department of the selected hospital; (2) Willingness to participate in the study voluntarily. (3) Achieved a theoretical score of >75 in the endocrinology entry exam. The exclusion criteria were as follows: (1) Nursing interns who were absent from their internship for more than half a month due to reasons such as suspension or sick leave; (2) Nursing interns who failed to complete the assigned teaching tasks for other reasons.
Figure 1 presents a flow diagram of participant allocation to the two groups. A total of 69 nursing interns were included in this study. Among them, 36 were assigned to the intervention group, with 2 dropouts, resulting in a dropout rate of 5.56%. The control group consisted of 37 participants, with 2 dropouts, yielding a dropout rate of 5.41%. The overall dropout rate for the study was 5.48%.

Flow diagram of the allocation.
Setting and procedures
A total of 3 nursing educators were responsible for implementing the program, and they were supported by 2 diabetes specialists. All team members were thoroughly trained on the study protocol and assessment tools to ensure a comprehensive understanding of the study's objectives, methodologies, and implementation procedures.
During the internship period, nursing interns in the intervention group utilized the virtual simulation teaching program to acquire skills in blood glucose monitoring, insulin injection, and hypoglycemia management. In the control group, traditional on-site demonstration methods were employed, with a lead instructor conducting standardized teaching sessions on the same topics. The remaining teaching content and hours were consistent across both groups, following the standardized teaching plan developed by the hospital's academic office.
General information, familiarity with virtual simulation learning, self-directed learning ability, and clinical thinking ability were uniformly collected from nursing interns in both groups before and after their internship in the endocrinology department.
Randomization, allocation, and blinding
The study was conducted with nursing interns from the Department of Endocrinology at a tertiary hospital in Changsha, who participated in the internship program from March to June 2024. Following screening and assessment, eligible participants were randomly assigned to either the intervention group or the control group in a 1:1 ratio using a computer-generated randomization sequence. The randomization sequence was generated and managed by an independent statistician who remained blinded to participant recruitment, assessment, and intervention procedures throughout the study. The allocation sequence was concealed in sequentially numbered, opaque, sealed envelopes to ensure the concealment and randomness of the allocation process. Outcome measures were assessed by two independent researchers.
Interventions
Development of the virtual simulative diabetes care program
Collaborative design planning
The team comprised endocrinologists, nurses, and graduate nursing interns from a tertiary care hospital, pedagogy experts, software engineers, and data analysts, whose contributions ensured the scientific and technical usability of the program.
The results of our previous online survey of 883 nursing interns from 23 provinces in China showed that the skills and knowledge that nursing interns most desired to acquire included hypoglycemia treatment (626/883, 70.9%), functional test simulation (610/883, 69.1%), and blood glucose monitoring techniques (485/883, 54.9%). 29 A questionnaire survey of nursing interns in the Department of Endocrinology was conducted with the objective of elucidating the current knowledge of nursing interns regarding virtual simulation, as well as their requirements for the content and format of the diabetes virtual simulation teaching program. This provided a foundation for the program's design. The results demonstrated that the three areas of knowledge that nursing interns expressed the greatest interest were specialty nursing operation techniques (29.2%), disease-related knowledge (21.0%), and disease-related health guidance (19.3%). The three most popular virtual simulation technology application scenarios were insulin injection (39.9%), hypoglycemia treatment (23.0%), and glucose monitoring (18.9%). A majority of respondents indicated that the optimal duration for each training session would be between 11 and 30 min.
Design of app prototype
The provincial nursing experimental teaching center served as a foundation for the development of a virtual simulation program. This program employed a range of technological tools, including 3D simulation, Virtual Simulation technology, animation technology, communication technology, simulation formation, and others, to create a comprehensive and engaging learning experience. 30 The project was comprised of three principal components: front-end development, back-end development, and interface development (Figure 2).

D training program structure.
The app interface includes four sections: the home screen (theoretical knowledge and nursing of diabetes), scenario simulations (blood glucose monitoring, insulin injection, hypoglycemia treatment), theory and skills tests, and the question and answer interface. Figure 3 shows the specific interfaces. The home screen provides key information on diabetes, including definitions, dietary and exercise guidelines, and procedures for hypoglycemia treatment, insulin injections, and blood glucose monitoring. In the scenario simulation section, interns select tools or actions from a menu on the left side. If the wrong action is chosen, an error message appears until the correct one is selected. The three scenarios are blood glucose monitoring, insulin injection, and hypoglycemia treatment. The exam interface includes a theory test and a skills test, each with 10 multiple-choice questions. A question and answer interface allows interns to submit difficulties they encounter, with educators providing responses to help them overcome challenges.

The interfaces of D training.
Intervention
Intervention group
The intervention was led by a multidisciplinary team, including endocrinologists, specialized nurses, nursing graduate students, and APP design experts. Over four weeks, it aimed to enhance diabetes care knowledge and skills through structured education and simulation-based training.
Week 1 focused on departmental orientation, including disease overview and nursing specialties, followed by offline lectures on “Endocrinology Overview” and “Introduction to Diabetes.” Interns participated in a theoretical exam and received one-on-one mentorship. A live blood glucose monitoring demonstration was conducted, followed by practice and online issue resolution via the program.
Week 2 covered “Diabetes Diet” and “Diabetes Exercise Therapy” through offline lectures and insulin injection demonstrations. Interns practiced insulin injection simulations and received online guidance from mentors.
Week 3 included lectures on “Hypoglycemia Management,” “Oral Hypoglycemic Drugs,” and “Diabetic Foot Care.” Interns practiced hypoglycemia management via the program, with online resolution of any issues.
Week 4 involved participation in ward rounds and a final examination.
Control group
The control group underwent the same orientation, lectures, and live demonstrations at the same time as the intervention group, with identical content. However, unlike the intervention group, the control group did not use virtual simulation technology. Instead, the training was based on conventional clinical teaching, where mentorship, practical exercises, and problem-solving were conducted during the clinical internship.
Measures and outcomes
Sociodemographic characteristics
This section of the self-report questionnaire included demographic information such as gender, age, educational level, internship duration, clinical experience, experience with video games, mobile learning, and prior exposure to virtual simulation-based nursing education.
The Independent Learning Ability Scale
The Self-Directed Learning Ability Scale for nursing interns, developed by Lin Yi et al., was used to assess the participants’ self-directed learning abilities. 31 The scale consists of 28 items, divided into three subscales: self-management, information ability, and learning cooperation ability. It is based on a 5-point Likert scale, with scores ranging from 1 to 5, where 1 represents "strongly disagree" and 5 represents "strongly agree" for items 1–21. Items 22–28 are scored in reverse, from 5 to 1 (A to E). Some items, such as 1, 2, 5, 10, 11, and 13, are reverse-scored. The total score for the scale ranges from 28 to 140 points, with subscales scoring as follows: self-management ability (50 points), information ability (55 points), and learning cooperation ability (35 points). The scale demonstrates good reliability, with a Cronbach's alpha of .86 for the overall scale and between .69 and .79 for the subscales. 32
The Clinical Thinking Skills of Medical Interns Scale
The Clinical Thinking Ability Evaluation Scale for Medical interns, developed by Song Junyan et al. in 2015, was used to assess participants’ clinical thinking abilities. 33 The scale consists of 24 items, scored using a 5-point Likert scale (1–5), with a total score of 120 points. Higher scores indicate better clinical thinking abilities. The scale is divided into three dimensions: systems thinking ability (55 points), critical thinking ability (30 points), and evidence-based thinking ability (35 points). The scale demonstrates good reliability and validity, with a Cronbach's alpha coefficient of .91. 33
The Virtual Clinical Case Application Effectiveness Evaluation Scale
The Virtual Clinical Case Application Effectiveness Evaluation Scale, developed by Chen Lili et al. 34 in 2014, was used to assess the effectiveness of the virtual clinical case program. The scale consists of 15 items, with a total score of 10 points. It includes four primary indicators, each with the following corresponding weightings: interface design (1.5 points), technical performance (1.5 points), learning content (3.0 points), and learning function (4.0 points). The overall evaluation value is calculated as the actual score for each primary indicator divided by its maximum score, with a range from 0 to 1. Based on the evaluation value, the effectiveness of the virtual case application is classified as follows: "Excellent" for values between 0.85 and 1, "Good" for values between 0.70 and 0.84, "Moderate" for values between 0.60 and 0.69, and "Poor" for values below 0.60. The scale demonstrates good reliability and validity, with a Cronbach's alpha coefficient of .84. 26
Furthermore, the study documented the activities performed by the nursing interns in the program, including the scores from three simulated operations (glucose monitoring, insulin injection, and hypoglycemia treatment) and two theory and skills tests. The data were recorded automatically via the program, with operation scores and test scores assigned a value of 100 and 10, respectively, to ensure comprehensive coverage and assessment of the educational content.
Statistical analysis
Data were double-entered and analyzed using SPSS version 25.0 (IBM Corporation, Armonk, USA). Demographic and clinical data between the groups were presented using appropriate descriptive statistics. Homogeneity between the groups was assessed using independent 2-tailed t-tests, Mann–Whitney U tests, chi-square tests, and Fisher's exact tests, as appropriate.
For self-directed learning ability, clinical thinking ability, post-test scores, and normally distributed data were expressed as means with standard deviations, and between-group differences were analyzed using independent 2-tailed t-tests. Non-normally distributed data were reported as medians with interquartile ranges, and the differences between the groups were evaluated using the Mann–Whitney U test.
The effectiveness of virtual clinical case applications was evaluated based on score distributions. For normally distributed data, means and standard deviations were used, while non-normally distributed data were presented as medians with interquartile ranges. The intention-to-treat (ITT) principle was applied to analyze all randomized participants, regardless of adherence to the intervention. All participants were included in the analysis, as baseline data were available for all individuals. All statistical tests were two-sided, with the level of significance set at 0.05.
Ethics
The study was approved by the Ethics Committee of Xiangya School of Nursing, Central South University, under the approval number E202333. The research process was conducted in accordance with the ethical standards governing scientific research, respecting the subjects’ right to information and ensuring the strict enforcement of the principle of confidentiality. In addition, the study was carried out in full compliance with the ethical principles set forth in the Declaration of Helsinki, ensuring that the rights, safety, and well-being of the participants were prioritized throughout the research process.
Results
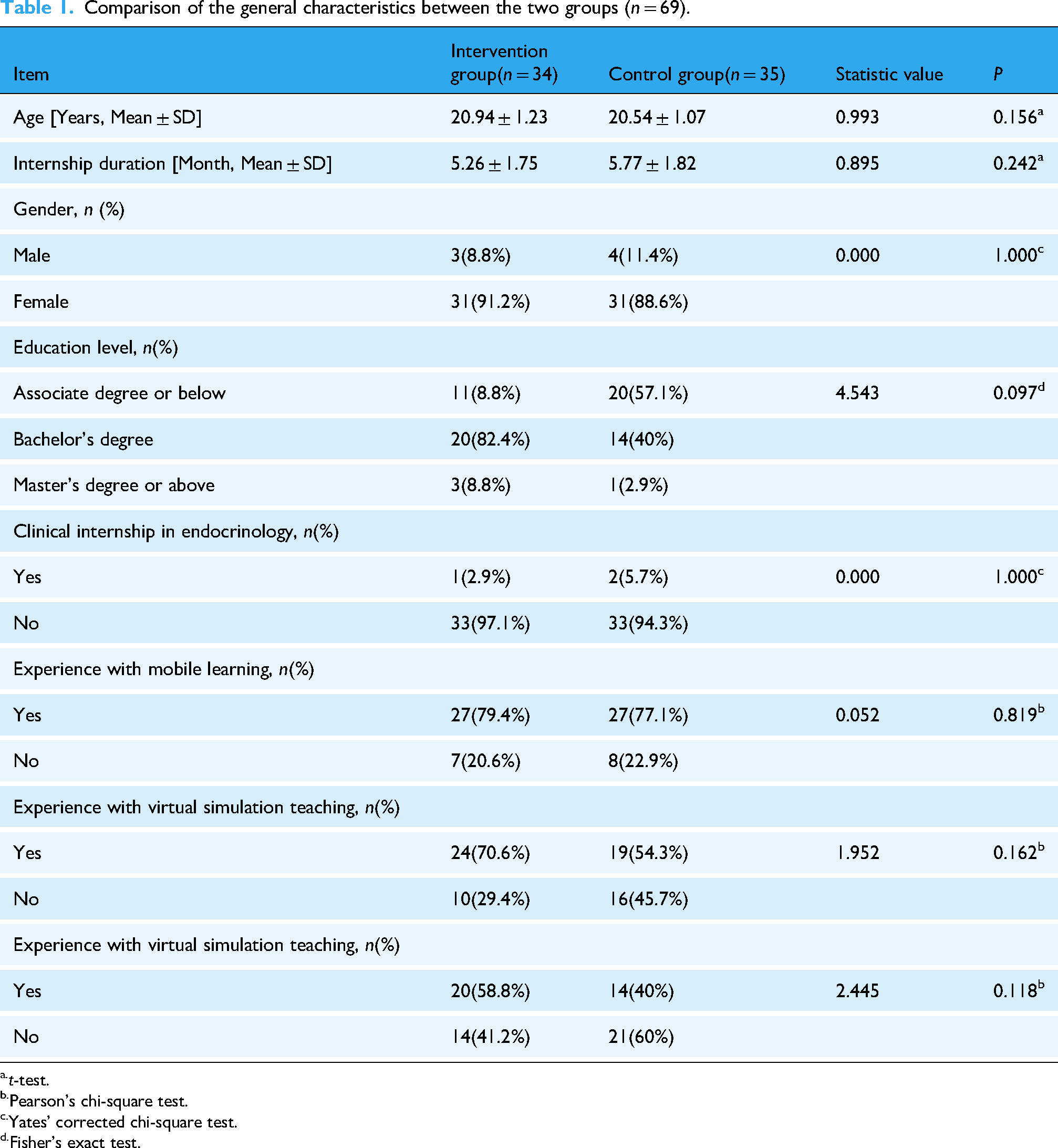
The baseline characteristics of the intervention and control groups are presented in Table 1. The overall average age of the study participants was 20.74 ± 1.16 years, with an average internship duration of 5.52 ± 1.79 months. In terms of educational background, the proportion of participants with a bachelor's degree was higher in the intervention group (82.4%) compared to the control group (40.0%), although the difference was not statistically significant (P=.097), suggesting a potential impact on the results. Regarding clinical experience in the endocrinology department, there was a minimal difference between the two groups (intervention group: 2.9%, control group: 5.7%, P = 1.000). Both groups had similar levels of experience with mobile learning and virtual simulation teaching, with no statistically significant differences (mobile learning: P = .819; virtual simulation teaching: P = .162).
Comparison of the general characteristics between the two groups (n = 69).
t-test.
Pearson's chi-square test.
Yates’ corrected chi-square test.
Fisher's exact test.
Overall, the baseline characteristics of the intervention and control groups were comparable, providing a solid foundation for the validity of subsequent results. However, the potential impact of differences in educational background on the results warrants further investigation.
Regarding self-directed learning ability (Table 2), there were no significant differences in the baseline scores between the intervention and control groups (P > .05), indicating comparable levels of self-directed learning ability prior to the intervention. After 4 weeks of intervention, the intervention group scored significantly higher than the control group in the overall self-directed learning ability (104.53 ± 7.75 vs. 99.00 ± 13.77, P = .044), suggesting that the virtual simulation diabetes care program effectively enhanced nursing interns’ overall self-directed learning abilities. Specifically, the intervention group also performed significantly better than the control group in information literacy (39.88 ± 3.67 vs. 38.91 ± 6.19, P = .044) and collaborative learning ability (27.32 ± 2.87 vs. 24.94 ± 4.39, P = .010), highlighting the positive impact of the program in improving information acquisition and processing skills, as well as teamwork and collaborative learning. However, although the intervention group showed improvements in self-management ability (37.32 ± 3.43 vs. 35.14 ± 5.14, P = .042), the difference between the two groups was only marginally significant, indicating that the effect on self-management ability requires further validation.
T test results of the nursing interns’ self-directed learning ability between the intervention and control groups.

Compared with the pre-intervention in the same group, *P < .05; compared with the control group, #P < .05
In terms of clinical thinking ability (Table 3), there were no significant differences in the baseline scores between the two groups (P > .05), indicating that the clinical thinking ability levels of both groups were comparable before the intervention. After 4 weeks of intervention, the intervention group scored significantly higher than the control group in the overall clinical thinking ability (99.71 ± 12.15 vs. 91.69 ± 17.44, P = .031), indicating that the virtual simulation diabetes care program had a significant positive effect on nursing interns’ overall clinical thinking ability. Specifically, the intervention group demonstrated a particularly notable improvement in systems thinking ability (46.53 ± 5.70 vs. 42.74 ± 7.33, P = .020), suggesting that the program was effective in helping interns analyze clinical problems from a holistic and systemic perspective. However, although the intervention group scored higher than the control group in critical thinking ability (25.29 ± 3.50 vs. 23.49 ± 4.42, P = .064) and evidence-based thinking ability (27.88 ± 3.88 vs. 25.46 ± 6.27, P = .058), the differences did not reach statistical significance, suggesting that the improvement in these two abilities may be limited by factors such as sample size or intervention duration.
T test results of the nursing interns’ clinical thinking ability between the intervention and control groups.

Compared with the pre-intervention in the same group, *P<.05; compared with the control group, #P<.05.
At the end of the internship, the intervention group nursing interns’ evaluation of the virtual simulation program was assessed using the Virtual Clinical Case Application Effectiveness Evaluation Scale. The overall application effectiveness score for the intervention group was 8.37 ± 1.20, with a composite evaluation score of 0.84, which was classified as "Good." The highest evaluation score was for the learning functionality of the program, which was 0.85 and rated as "Excellent." Other dimensions of the program's application effectiveness received a "Good" rating, as detailed in Table 4.
Evaluation of the application effectiveness of the virtual simulation program by nursing interns (n = 34).

Significant differences were observed between nursing interns’ scores in practical skills and theoretical tests. Specifically, the average scores for blood glucose monitoring (86.40 ± 7.82), insulin injection (90.20 ± 9.02), and hypoglycemia management (85.60 ± 11.73) indicated that interns generally performed better in practical tasks than in theoretical tests. This finding is closely related to the high-frequency, low-risk practice opportunities provided by virtual simulation-based teaching. Furthermore, after the implementation of virtual simulation teaching, significant improvements were observed in both self-directed learning ability and clinical thinking ability. Self-directed learning ability increased from(95.20 ± 6.41 to 103.80 ± 8.00), while clinical thinking ability improved from (82.70 ± 7.79 to 94.20 ± 13.97), with statistically significant differences (P < .05). These results suggest that virtual simulation teaching not only enhanced nursing interns’ practical skills but also contributed to the development of their self-directed learning and critical thinking abilities.
Discussions
This study developed a virtual simulation-based diabetes care teaching program (D Training), addressing the limitations of traditional teaching methods in terms of time, space, and resources. Virtual simulation technology has become widely used in medical training, offering risk-free practice environments that enhance teaching efficiency and improve clinical skills. 35 It also provides personalized learning recommendations through artificial intelligence, further enhancing outcomes. 36 This global technology helps overcome geographical barriers and promotes equity in medical education. 37 Our findings show that the program not only improved nursing interns’ theoretical knowledge and operational skills but also enhanced overall nursing education quality. 3 Specifically, virtual simulation significantly improved nursing interns’ self-directed learning abilities and clinical thinking skills, with notable improvements in information literacy, collaborative learning, and systems thinking. These findings support the widespread application of virtual simulation technology in nursing education and provide valuable insights for future teaching improvements.
Self-directed learning ability refers to a student's capacity to independently master learning content, set learning goals, and self-regulate learning strategies. 38 The present study demonstrates that virtual simulation teaching significantly enhances nursing interns’ self-directed learning ability, particularly in the areas of self-management and learning collaboration. Consistent with previous research, many studies have shown that simulation-based teaching can substantially promote nursing interns’ self-directed and active learning abilities. Yoe et al. found that nursing interns who engaged in simulation-based teaching scored significantly higher in self-directed learning than those in traditional classroom settings. 39 Similarly, Li L et al. confirmed that virtual simulation helps interns improve their independent learning and problem-solving skills. 40 We provide strong support for the effectiveness of virtual simulation in enhancing nursing interns’ self-directed learning ability in this study. In contrast, Al-Ghareeb questioned whether virtual simulation can effectively replicate real clinical scenarios, suggesting that it may not fully capture the complexity of clinical decision-making. 41 Furthermore, existing studies have shown that the effectiveness of virtual simulation programs may diminish over time, particularly when the courses are not regularly updated or tailored to the learners’ needs. 42 In the future, virtual simulation teaching design should prioritize the complexity and realism of simulated scenarios, alongside regular updates and customization of course content to sustain its long-term effectiveness. 43 Moreover, further research is needed to explore how virtual simulation can be optimized at various learning stages and across different contexts to maximize its impact, ensuring comprehensive training in clinical decision-making. 44
Clinical thinking ability refers to the capacity of healthcare professionals to effectively analyze, assess, make decisions, and execute nursing tasks in clinical practice. 45 This study found that virtual simulation significantly enhanced nursing interns’ clinical thinking abilities, particularly in clinical reasoning, critical thinking, and decision-making. Complex and realistic scenarios in virtual simulations were shown to more effectively improve clinical thinking, especially when dealing with complex diseases and making clinical decisions. 46 This improvement in interns’ comprehensive judgment and adaptability helps them better understand patient conditions and make accurate clinical decisions. 47 These results are consistent with existing literature, which suggests that virtual simulation can effectively enhance nursing interns’ clinical thinking skills. 39 Song Y et al. noted significant improvements in clinical reasoning among nursing interns who participated in virtual simulation training, 48 while Salminen et al. observed that virtual simulation effectively promoted systems thinking. 49 However, some studies have raised concerns regarding the effectiveness of virtual simulation in clinical reasoning and critical thinking. Cho suggested that while virtual simulations provide valuable feedback, the ability to handle complex cases may still be influenced by individual differences. 50 By simulating real-world clinical environments, virtual simulation not only improves interns’ clinical knowledge and skills but also deepens their understanding of complex issues. 51 Additionally, the real-time feedback mechanism in simulation teaching allows interns to quickly identify and correct mistakes during practice, accelerating the development of clinical thinking skills. 52 However, some studies also indicate that over-reliance on simulation feedback may limit interns’ adaptability when faced with unfamiliar clinical problems. Therefore, further research is needed to explore how to balance virtual simulation with traditional teaching methods to comprehensively enhance clinical thinking abilities. 53
Virtual simulation teaching significantly improved nursing interns’ clinical operation skills. The high-frequency, low-risk practice opportunities offered by the system resulted in better clinical performance than theoretical tests, confirming that real-time feedback and precise simulations enhance confidence and practical skills. 54 These improvements underscore the value of virtual simulation in reinforcing clinical knowledge application. 55 Future programs should include more complex scenarios and case analyses to further develop interns’ abilities to manage complex clinical situations. Despite these positive outcomes, some interns reported concerns about the program's perceived usability, as noted in Irene's study. 56 This highlights the need for further optimization of interface design and system stability in future virtual simulation systems, ensuring smoother user experiences and minimizing technical issues that could disrupt the learning process. 57
Conclusions
Virtual simulation technology provides an innovative teaching method for nursing education, effectively bridging the gap between theory and practice. The primary finding of this study is that the virtual simulation-based diabetes care teaching program significantly improved nursing interns’ self-directed learning and clinical thinking abilities, particularly in areas such as self-management, learning collaboration, systems thinking, and clinical reasoning. By creating an interactive and immersive learning environment, virtual simulation facilitated the simulation and practice of complex clinical scenarios under low-risk conditions, thereby enhancing interns’ clinical decision-making and problem-solving skills.
Future research should further explore the long-term impact of virtual simulation technology on nursing interns’ clinical performance and career development, particularly in terms of skill transfer in real-world practice. Additionally, future studies could expand sample sizes and adopt multi-center designs to validate the effectiveness of virtual simulation teaching in diverse clinical settings, and investigate how different simulation scenarios and teaching models influence learning outcomes, aiming to optimize and personalize teaching approaches.
Footnotes
Acknowledgments
The authors would like to extend gratitude for the time and effort of the nursing interns who provided input and feedback on the app in usability testing. We would also like to thank Yuanyuan Luo for her assistance in designing the program. We express our thanks to Yuxiang Luo for professional assistance in proofreading the manuscript.
Guarantor
HW.
Ethical considerations
The study was approved by the Ethics Committee of Xiangya School of Nursing, Central South University, under the approval number E202333. Electronic informed consent had to be obtained from participants before they were enrolled in the study. The electronic version of the informed consent form was on the first page of the questionnaire, and only when the participant confirmed their consent to participate would they begin to complete the electronic questionnaire.
Author contributions/CRediT
T. Xu was responsible for the conceptualization, formal analysis, investigation, and writing of the original draft. H. Weng contributed to review, editing, and project administration. Q. Wang was involved in validation, investigation, and supervision. F. Liu handled the investigation, data curation, and visualization. L. Yang and R. Wang contributed to the resources.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Clinical Nursing Research Foundation of the Second XiangYa Hospital of Central South University (2021-HLKY-06).
Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
