Abstract
Objectives
Despite rapid technological advances, the adoption and deployment of digital health and virtual reality (VR) applications in healthcare appears to be progressing slowly. This scoping review is part of the Scale-Up4Rehab (SU4R) project, which aims to create a virtual rehabilitation clinic hosting high-quality digital health interventions. The aim of this review was to identify existing high-quality digital health evaluation frameworks, and from these, extract criteria to inform a new set of guidelines for assessing the applications that will be hosted on the SU4R platform.
Methods
The review followed Arksey and O’Malley's scoping review framework and was reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. A search strategy that included relevant keywords encompassing the domains of interest; digital health, evaluation frameworks and digital health applications was created between January 2007 and December 2023, across seven medical and computer science databases. Data from each study were extracted by a team of four reviewers using a customized data extraction tool.
Results
The review included 18 frameworks from 11 countries, incorporating 775 criteria. Nine evaluation frameworks were identified from the included papers (n = 12) and a further nine frameworks from grey literature. The criteria were grouped into 19 categories, with the largest proportion of identified criteria grouped into the categories ‘Data Security and Privacy’ and ‘Validation’.
Conclusion
The criteria extracted from the reviewed frameworks will contribute to the creation of a comprehensive evaluation framework. This new evaluation framework will form part of the approval process for the SU4R Virtual Rehabilitation Clinic. This will facilitate a rigorous selection process for the digital health and VR applications to be hosted on the virtual clinic.
Background
Global healthcare is evolving, driven by aging populations and the increasing prevalence of chronic diseases.1,2 These factors place significant demands on healthcare systems, highlighting the need for innovative solutions to deliver efficient person-centred care. With advancements in technology, there is growing interest in utilising digital health interventions to address healthcare challenges. 3 The digital health market has been growing rapidly in recent years and is expected to continue on this growth trajectory. The global digital health market size was valued at approximately $211 billion in 2022 and is expected to grow at a compound annual growth rate of 18.6% from 2023 to 2030. 4
Virtual reality (VR) interventions have emerged as promising digital health interventions in various domains of healthcare, offering innovative solutions for patient treatment, rehabilitation, and education. VR uses a Head Mounted Display (HMD) to simulate a reality in which the user is immersed in a virtual environment, creating the impression that the user is physically present within this virtual space. 5 It is emerging as a viable solution in healthcare across a variety of medical specialties, from teaching and training, 6 surgery, 7 psychology, 8 and rehabilitation. 9 Furthermore, VR interventions have been piloted to assist in the treatment of many medical conditions, for example chronic pain management, 10 post-stroke rehabilitation, 11 the management of depression 12 and symptom burden in patients who are terminally ill with cancer. 13 These studies highlight the potential for VR interventions to revolutionise healthcare delivery by providing easily accessible, engaging and personalised experiences for patients and clinicians alike.
Despite the growth of research in this field, evidence suggests the uptake of digital health and VR interventions in clinical practice is low and underutilised.14–18 This may be explained by the complexities of implementation within an established but fragmented sector such as healthcare. From the patient's perspective, there may be challenges in using new technologies due to low digital health literacy or limited access to technology, especially for older adults and people with lower digital literacy. 19 Poor design of technology and/or application design, technology experience, resistance to change and costs of acquiring technology 20 may act as barriers to patient engagement. This can be seen in the work presented by Agnew et al. 21 where they concluded that shoulder pain-related applications that are currently available do not provide an appropriate quantity and quality of information to users, thus resulting in a failure of the application to achieve an engaging impact. With regard to VR specific digital health interventions, the potential issue of cybersickness may in some cases present as a further barrier to patient engagement.22–24 In addition, a large number of applications appear to be developed without public and patient engagement or healthcare professional involvement. 25 Furthermore, Wicks and Chiauzzi 26 identified insufficient technology support and interoperability with other pre-existing health technology as additional challenges.
A scoping review (n = 74 studies) investigating safety concerns with consumer facing mobile health applications identified 80 safety concerns, the majority of which were related to the quality of the information presented and inappropriate responses by the applications to patient's needs. 25 Furthermore, research by Powel et al. 26 identified the majority of publicly available reviews of mobile Health (mHealth) apps have been based on personal experiences, with few evidence-based, unbiased evaluations of clinical performance and data security. 26 In the context of data security in mHealth technologies, a literature review 27 investigating privacy protections and data ownership in mHealth identified a range of issues related to data security and access, confidentiality and consent. These reviews suggest that the implementation of digital health and VR applications in healthcare appears to be lacking quality assurance and as such, recommendations have been made to verify the quality, accuracy and usefulness of the digital health applications before their release for clinical use. 28
A number of national and international groups have produced guidelines focusing on digital health interventions.29,30 Despite the growing interest and adoption of VR in healthcare, there remains a lack of standardised protocols and best practice guidelines governing their design, development and deployment. With the emergence of VR in healthcare, professionals may struggle to navigate guidelines related to patient safety, ethical considerations, technical standards, treatment effectiveness and interoperability, 20 when incorporating VR into clinical practice, and in the absence of practice guidelines that refer specifically to VR interventions. Currently, clinicians must navigate a complex landscape of VR platforms, each with its own technical specifications and requirements, which can vary widely depending on the intended use and target patient population. Addressing these challenges requires collaboration between clinicians, application developers, and experts in the fields of regulation and compliance in order to develop standardised protocols and procedures.
Comprehensive guidelines are essential to provide evidence-based recommendations, address technical and ethical considerations, and to guide the development, evaluation, and implementation of treatment strategies in healthcare. 31 The authors acknowledge that due to the novelty of VR in healthcare that there may not currently be VR-specific guidelines for evaluating VR health interventions; however, by leveraging insights from existing evaluation frameworks for digital health applications, we can effectively gather knowledge that will contribute to the development of a future comprehensive framework capable of evaluating both. The development of comprehensive and evidence-based guidelines specific to digital health and VR applications in healthcare may provide a pathway to assist in the responsible and optimal integration of these innovative technologies into patient care pathways. Given the rapidly evolving digital health application environment, it is important to understand which criteria are included in existing digital health evaluation guidelines and frameworks in order to create a comprehensive evaluation method required for analysis of applications to be hosted on the future Scale-Up4Rehab 32 (SU4R) virtual rehabilitation clinic.
Objectives
The primary aims of this scoping review are to (i) identify existing digital health evaluation frameworks that have been utilised by national or international governing bodies to assess digital health and VR interventions, and (ii) categorise criteria within the identified frameworks. This scoping review will inform a subsequent framework analysis and consensus study to establish a final draft of a comprehensive evaluation framework. This framework will be utilised to evaluate applications seeking inclusion on the future virtual rehabilitation clinic platform.
Methods
Study design
This scoping review followed the five-stage framework of Arksey and O’Malley, 33 including: (i) identification of the initial research questions; (ii) identification of relevant studies; (iii) study selection; (iv) charting the data; and (v) collating, summarising, and reporting the results. This will be reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Extension for Scoping Reviews guideline. 34 The scoping review was registered on the Open Science Framework in December 2023 (https://doi.org/10.17605/OSF.IO/CQHPE) prior to commencing the literature search.
Search strategy
The following research questions were identified; (i) What are the existing high-quality frameworks governing digital health applications globally? and (ii) What categories and criteria of assessment are used in existing frameworks evaluating digital health applications? The search strategy (Supplemental Material, S1) was planned and created by a team of five academics from rehabilitation and computer science fields, with experience in scoping and systematic reviews. The strategy included relevant keywords which encompass terms for the three domains of interest: (i) digital health, (ii) evaluation frameworks, (iii) digital health interventions and applications. In addition, search strategies from relevant reviews were also utilised. 35 The search strategy was first developed for PubMed (Supplemental Material, S1) using medical subject headings where available, and adapted for other databases to account for differences in indexing across databases.
Searches were conducted on databases ranging from 2007 (the advent of digital applications following the release of the first Apple Inc. Iphone), until 12th December 2023, on the following databases: Association for Computing Machine's Digital Library (ACM DL), Institute for Electrical and Electronics Engineers Xplore Digital Library (IEEE Xplore), PubMed (PubMed), Cinahl (Ebsco), Scopus (Elsevier), Embase (Elsevier) and SportsDiscus (Ebsco). As 2007 is regarded as a pivotal moment in the evolution of digital technology with the advent of the iPhone, frameworks prior to this were not systematically searched for in the databases, as novel elements of evaluation specific to mobile digital health applications will not have been considered in these frameworks. These databases were selected to include research from both medical and computer science-oriented databases. Reference lists of included studies were hand-searched for potentially eligible articles and additional sources of grey literature were searched, (Supplemental Material, S2) which included World Health Organisation (WHO) and government websites. Web searches using specific search strings on Google were also conducted. To ensure quality in the grey literature findings, the inclusion criteria ‘the digital application evaluation method identified was required to be validated/endorsed/utilised by a national/international regulatory body or a national healthcare system’ was applied.
Eligibility criteria
Only articles published as full text in the English language in peer-reviewed journals were included. Acceptable articles had to include reference to (i) evaluating a digital application, (ii) used in healthcare (any setting), (iii) for any medical condition, and (iv) the digital application evaluation method identified was required to be validated/endorsed/utilised by a national/international regulatory body or a national healthcare system. If information required was not available from the source material or via contact with the corresponding authors, the framework was not included in the final analysis. Frameworks identified in the grey literature or in reference lists of included studies that were published prior to 2007 were eligible for inclusion.
Screening
Articles obtained following the searches were exported and saved into an online review management platform (Rayyan). An automated deduplication process was carried out using the Rayyan software for articles with duplication findings of >95% duplication. Further duplicates, suggested by the software, with <95% duplication were reviewed by two members of the research team (EOR, OD) and a decision was made regarding deletion of duplicates. After deduplication was completed, study titles, authors, journal titles and abstracts were visible to the reviewers and screened independently for eligibility by six pairs of 12 collaborating reviewers, including clinicians and academics in both computer science and healthcare across three academic institutions. Disagreements between reviewers over eligibility were resolved by discussion and consensus, and when required, the assistance of a third reviewer as arbiter.
Study selection and data extraction
Data extraction from included studies was based on reported procedures. 36 Prior to full data extraction, four studies were subjected to a blinded pilot data extraction tool by two reviewers (EOR, OD) that enabled any inconsistencies in the data selection to be resolved. Data were then extracted from each study by four reviewers (OD, EOR, DM, MY) independently using a customised data extraction tool in the form of an MS Excel spreadsheet (Supplementary Material, S3). Extractors were masked to data extracted by the second extractor until all papers were completed following the trial. If any disagreements occurred in data extraction that could not be resolved between the two extractors, a third data extractor was available for a deciding opinion.
The following data were extracted: study title, year of publication, authors’ names, study design, study objective, application details (if mentioned), name of framework, country/region of framework development, availability of framework for use, categories analysed in the framework.
Data analysis/synthesis planning
This scoping review focused on the identification and detailed description of the identified frameworks. Descriptors of the identified frameworks included: framework title, framework creators/authors/governing authority, year of publication, availability of content, country of origin, number and names of categories described, and number and names of criteria identified. The complete set of/criteria identified within each framework was then collated and reviewed by two reviewers. Using an iterative process, four members (EOR, OD, MY, DM) of the research team reviewed a sample of the collated criteria and identified a universally applicable set of categories that addressed all critical aspects of evaluating digital health interventions identified from the criteria. This process was followed by analysing the scope, purpose, and specifics of each criterion to determine its placement within the categories. Any disagreements in the collation of these categories were resolved through arbitration. Output files from the data synthesis have been stored as Microsoft Word and Excel files.
Results
Study selection
The stages of the scoping review are summarised in Figure 1. The electronic database search yielded 7025 records. After removal of duplicates and screening for eligibility, 12 papers were included. A total of 18 frameworks were identified, nine from the databases,37–48 and nine from the grey literature.49–57 The frameworks identified are outlined in Tables 1 and 2.

PRISMA flow diagram.
Frameworks identified in the database search.

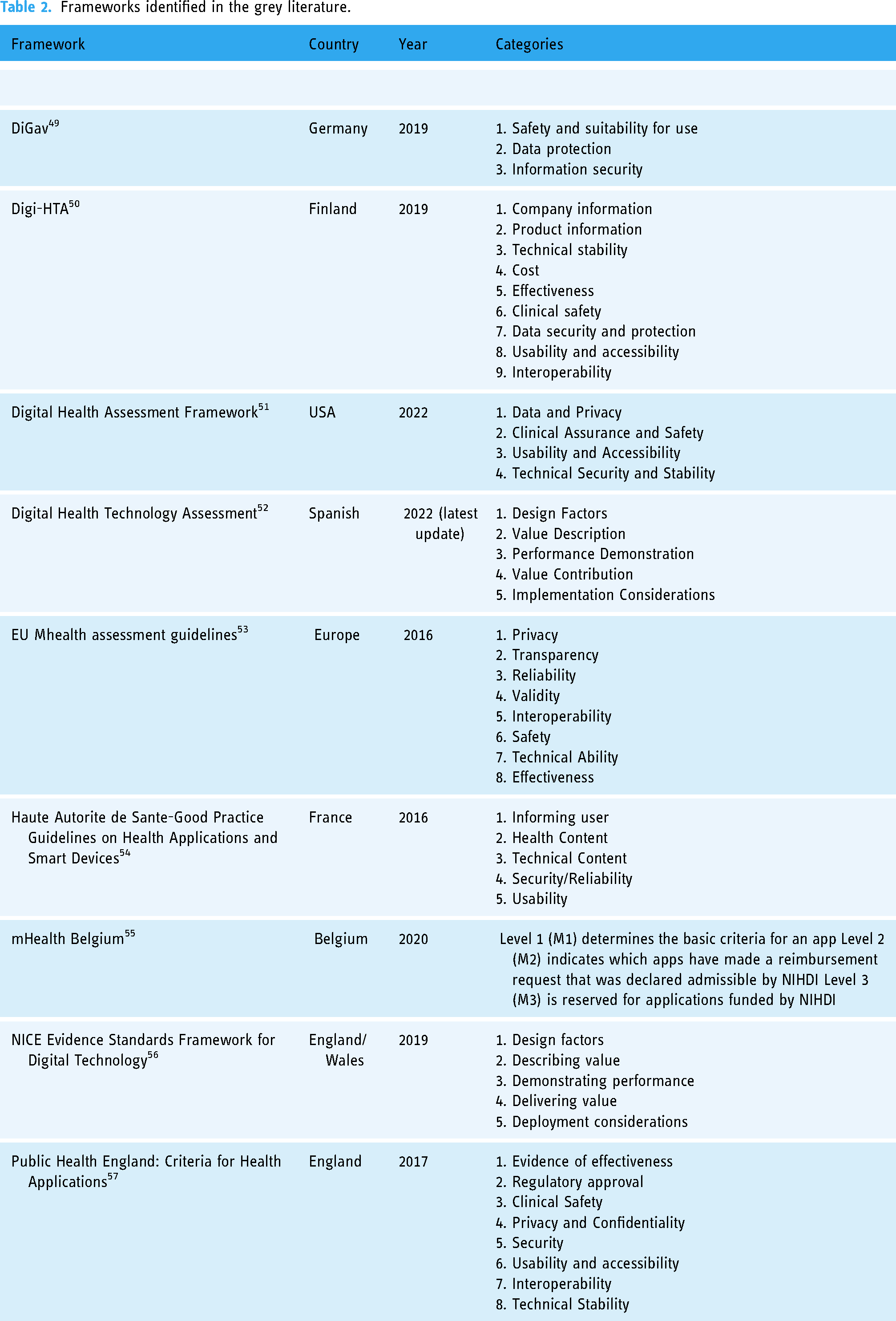
Frameworks identified in the grey literature.
Criteria identified
A total of 775 evaluation criteria (Supplemental material, S4) were identified from the 18 frameworks. Two independent assessors (EOR, OD) were assigned to a collection of criteria to classify them under domain specific sub-categories (Figure 2). The findings revealed that the most frequently cited criterion pertained to ‘Data Security and Privacy.’ Criteria within this category underscored the importance of protecting patient information and ensuring that digital health applications comply with stringent privacy regulations. The criteria also highlighted procedures to minimise security breaches or mishandling of personal health data. The second most commonly referenced criteria were grouped under ‘Validation.’ Criteria included in this category highlighted the necessity of establishing the efficacy and reliability of digital health and VR interventions. Definitions of the criteria groupings are described in (Supplemental material, S5).

Grouping of the framework criteria.
Discussion
This scoping review identified 18 evaluation frameworks and 775 analysis criteria, utilised by national and international governing bodies spanning 11 countries, for the evaluation of digital health interventions and applications. Nineteen domain specific sub-categories encompassed the 775 criteria, with the most frequently cited criteria relating to ‘Data Security and Privacy. No evaluation framework was identified for inclusion that specifically evaluated VR healthcare interventions, however a number of the analysis criteria identified were generic to a range of digital health interventions and applications. The extent to which they apply to VR applications and hardware with disparate and additional functionalities is not known. Our findings suggest that universal gold-standards for the appraisal of digital health and VR applications are lacking, indicating the need for a new evaluation framework to ensure a comprehensive assessment procedure is created for the future SU4R ‘virtual clinic’. The findings from this scoping review will inform the development of an evaluation framework for the VR applications used in the SU4R ‘virtual clinic’.
A recent scoping review examined the implementation process of VR in healthcare 58 and found that the majority of studies identified in the review focused on barriers or facilitators to implementation that limit the uptake of VR. One of the barriers included was lack of personalisation of some VR applications to patient needs and treatment goals. Furthermore, this review suggested that the implementation process of VR in healthcare settings could be supported by implementation frameworks, further highlighting the need to examine each frameworks’ criteria and to establish robust eligibility criteria for VR applications to be hosted on the virtual clinic. 58 As digital health interventions and applications, including VR, continue to proliferate, selecting the most appropriate interventions has become increasingly challenging for both patients and clinicians. 59 For example, individuals typically rely on the use of star rating systems and user reviews in app stores, despite strong evidence that such evaluation methods are misleading. 60 The challenge for appropriate evaluation methods for patients and clinicians is multifaceted, including the rates of evolving evidence, risks of data privacy, concerns regarding usability and the fact that applications are continually updated and modified. 61 The range of evaluation frameworks identified in this review, in addition to large numbers of criteria within each framework introduces additional complexity to the evaluation process.
Nine out of the 18 frameworks included in the review were not published in peer-reviewed journals but on sources of grey literature (national and international websites dedicated to health implementation guidelines and information). This finding highlights a substantial gap in the scientific literature regarding the availability and dissemination of comprehensive evaluation frameworks for digital health applications. The absence of peer-reviewed validation for many of these frameworks may raise concerns about their scientific rigor and acceptance within the academic and clinical communities. In the current review, to be eligible for inclusion, the digital application evaluation method identified must be validated/endorsed/utilised by a national/international regulatory body or a national healthcare system. This inclusion criterion was applied in order to set a minimum quality for the frameworks included, as no gold standard evaluation process has been developed. However, given the number of frameworks used by national bodies not represented in peer-reviewed literature, there is a need for a more systematic and rigorous approach to their creation.
The 775 criteria categorised in the current review revealed an imbalance in the frequency of occurrence of criteria categories across frameworks. Approximately one-third (250/775) of the criteria identified ‘data security and privacy’, whilst less than 50 criteria were related to clinical functionality (see Figure 1). These findings are consistent with a number of other systematic reviews. Napetsching et al. (2023) 62 and Mc Cool et al. (2018) 63 also highlighted that sub-group data related to data protection and data privacy encompassed a broader range of content compared with other reported categories. Napetsching and colleagues 62 suggested an explanation for this may be that these topic areas are subject to more stringent regulatory standards and requirements and this may result in a larger amount of detailed explanations compared with other categories. While confidence in data privacy is paramount, the regulatory standards for the veracity of health or medical claims in many applications and digital interventions appear much less frequently. This lack of standards challenges the real-world utilisation of these interventions and affects the confidence healthcare providers have in incorporating them into patient care plans.
The current review also highlights that economic-based criteria were underrepresented within the evaluation criteria across the identified frameworks, despite economic limitations being reported as key barriers to the implementation of VR by both clinicians and patients. 64 Currently, digital health and VR applications and evaluation frameworks are typically developed through multidisciplinary collaborations between VR developers, computer scientists medical staff or health scientists. 65 However, there seems to be minimal input from experts in health economics and finance to oversee the financial planning to ensure that health applications are durable and that the companies involved have the necessary resources for ongoing technical maintenance and development.
In relation to financial stability, a study by Wang et al. (2006) 66 identified that measuring scalability both financially and technically is not a commonly undertaken process. While the current frameworks reviewed place low emphasis on scalability criteria, the SU4R project consortium has identified financial and scalability criteria as crucial for ensuring the sustainability and durability of the future online virtual rehabilitation clinic. The consortium has engaged experts in health economics in VR in order to analyse the criteria identified under both the ‘financial’ and ‘scalability’ categories. Analysis of these criteria and identification of additional criteria that will be considered for the final ‘virtual clinic’ approval process will ensure the model is financially viable and scalable.
Limitations
Several limitations relating to this review are acknowledged. It is important to recognise that the criteria within the final evaluation framework are expected to remain valid only for a limited time-frame, considering the rapid technological advancements in the digital technologies and VR healthcare market. 67 These variabilities highlight the need for continuous refinement and updates to the evaluation framework to maintain its relevance and accuracy in the face of evolving technology and diverse expert opinions. In addition, the multidisciplinary nature of the research group may have influenced the grouping and categorisation of criteria depending on their level of exposure and knowledge of digital health applications. It is noted that only papers published in the English language were included in the current review, which may have excluded frameworks published in other languages. Furthermore, this scoping review did not set out to review the pros and cons of the identified frameworks as this was not within the aims and outside the scope of the review. However, it is acknowledged that reviewing the pros and cons of the different frameworks would be a useful area for future research.
Conclusion
This scoping review represents the initial step in developing a core set of criteria tailored for the SU4R virtual rehabilitation clinic. A range of 775 criteria were identified from frameworks currently in use across various countries and were grouped into domain specific sub-categories for the purposes of future analysis. The criteria identified within the current scoping review will be analysed using a framework analysis in phase two of this project to inform the development of a comprehensive evaluation process. In the final phase of this project workshops will be conducted with experts with a range of expertise in digital health and VR applications (medical, technical, economic etc.). Through this iterative process the criteria will be further refined. The final evaluation framework will be utilised by an expert committee as a benchmarking tool to appraise and quality assure applications that may be hosted on the virtual clinic platform. Details of this process will be published in due course. The final evaluation framework will consist of criteria identified from a large number of high-quality published frameworks, and in addition, will include input from experts in the field of digital health and VR applications from a medical, technical, economic and compliance perspective. This will ensure the newly established framework will build and improve on previously identified key criteria, in addition to identifying nuances in the field identified by expert input. From a practical implementation perspective, the final evaluation framework will initially be piloted by the expert committee to identify any implementation issues. This will be followed by framework deployment phase which will include ongoing evaluation and monitoring of the framework's performance allowing for a feedback loop and improvement opportunities. As a result of the field's rapid progression, the most significant challenge in implementation of the framework will be ensuring the regular review and update of the evaluation framework to remain up to date with advances in the field. While there remains a lack of consensus on the precise nature of the criteria necessary to establish a comprehensive evaluation framework for digital health interventions, the initial identification of criteria from this review will provide a foundation to ensure a rigorous selection process for the SU4R virtual clinic, grounded in the best available evidence for evaluating digital health interventions.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-docx-1-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Supplemental Material
sj-docx-2-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-docx-2-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Supplemental Material
sj-xlsx-3-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-xlsx-3-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Supplemental Material
sj-xlsx-4-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-xlsx-4-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Supplemental Material
sj-docx-5-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-docx-5-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Supplemental Material
sj-docx-6-dhj-10.1177_20552076251315297 - Supplemental material for A scoping review of frameworks evaluating digital health applications
Supplemental material, sj-docx-6-dhj-10.1177_20552076251315297 for A scoping review of frameworks evaluating digital health applications by Orla Deegan, Eoghan O Riain, Denis Martin, Mai Yoshitani, Mairead O’Donoghue, Keith Smart, Sinead McMahon, Trish O’Sullivan, Declan J O’Sullivan, Aaron Cole, Ciara Hanrahan, Catherine Blake, Joseph G. McVeigh, Brona M Fullen and David Murphy in DIGITAL HEALTH
Footnotes
Acknowledgements
The authors extend their gratitude to Catherine Doody, Tara Cusack, and Marta Moreno Legero for their valuable expertise and contributions during group meetings throughout this scoping review process.
Authors’ contributions
BF, DM, JMcV, EOR and OD were responsible for the study conception and design. DOS, AC, CH, SMM, KS, BF, JMcV, DM, EOR, OD, TS undertook the article screening. With respect to this manuscript, the paper was drafted by OD, EOR and MOD and was critically revised by KS, SMM and DOS. Final revisions were made by DM, BF and JMcV. All authors read and approved the final manuscript.
Authors' note
Brona M Fullen is also affiliated with UCD Centre for Translational Pain Research, University College Dublin, Dublin, Ireland.
Consent for publication
Consent for publication is not applicable because this study is based exclusively on published literature.
Data availability
Data is available upon request from the corresponding author.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical considerations
Ethics approval was not required for this study as it was a scoping review of the literature, which involved synthesising existing published studies rather than conducting new research involving human participants.
Funding
The Scale-Up4Rehab project is funded by Interreg North-West Europe and co-funded by the European Union (Grant Code: NWE0100082).
Guarantor
Orla Deegan (odeegan@qu.edu.qa)
Eoghan O’Riain (eoghanoriain@ucc.ie)
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
