Abstract
Background
Mental health care during the postpartum period is notably underexplored within Asian demographics, with barriers such as stigma, privacy concerns, logistical challenges, and a shortage of mental health professionals that limits access to optimal mental healthcare. Previous studies found that mobile health (mHealth) technology has been offering a promising solution to these issues. However, the perspectives of mothers on existing mental health services and their mHealth needs are still not well understood and warrant further exploration.
Objective
This study aimed to explore the postpartum experiences of Malaysian mothers with postpartum depression (PPD) symptoms and their perspectives on using an mHealth technology to improve mental health care during the postpartum period.
Methods
We carried out in-depth interviews with six mothers, which were transcribed verbatim and thematically analysed. Collaborative discussions and consensus were employed to enhanced reliability.
Findings
Five main themes related to mothers’ postpartum experiences and perspectives emerged, namely, the existing circumstances of mothers, psychosociological reactions, maternal needs, innovation of care, and suggestions for pragmatic mHealth elements. These themes emphasized the emotional challenges of meeting societal, cultural, and personal expectations. The essential resources identified to be included in the mHealth technology were education on PPD, professional guided self-care, cognitive restructuring, validation of diverse infant feeding practices, and fostering partner support. Furthermore, interactive mHealth features such as mood trackers, notifications, platforms to share, and motivational tools aimed at elevating maternal well-being were also sought.
Conclusions
Mothers expressed a desire for mHealth services emphasizing the need for these educational tools to be culturally sensitive, accommodating local language and religious practices, and offering support during confinement, to effectively address the unique needs of postpartum mothers. This study highlights the importance of prioritizing practical mHealth interventions as strategic support services to enhance positive postpartum mental care in resource-stricken countries.
Keywords
Background
Pregnancy has the potential for heightened risks of mental disorders, with postpartum depression (PPD) emerging as a significant concern globally.1,2 According to Wang Zi Yi et al., 3 approximately 17.22% of postpartum women worldwide suffer from PPD, with prevalence rates varying significantly by region and socioeconomic status. In Asia, the prevalence is notably higher, with Klainin 4 reporting that PPD prevalence can reach up to 63.3%. Rahmadhani 5 reported that in 2022 the incidence of PPD in Indonesia was as high as 50%, while Hajipoor 6 found the incidence in Iran to be 67%. A systematic review by Ekpenyong 7 further highlighted that the prevalence of PPD varies significantly across different cultures in Asia, underscoring the need for maternity healthcare providers to consider cultural practices in their care strategies. In Malaysia, PPD prevalence ranges from 3.9% to 22.8%.8–11 In 2021, Hairol 12 reported an incidence of 14.5% in an outpatient postpartum clinic. Additionally, the 2022 Malaysian National Health Morbidity Survey found that 10.4% of mothers experienced PPD. PPD's consequences extend beyond mothers; it may also impact children's cognitive, emotional, and behavioural development.13,14 Despite the existence of maternal and child health services, many Asian countries lack national programmes targeting mental health among postpartum mothers, especially in middle- to low-income countries. 15
This deficiency has been reported to be perpetuated by cultural norms, insufficient mental health literacy, and strict postpartum practices. 16 Cultural practices in many countries often restrict postpartum women from leaving their homes, limiting social interaction and access to external support, potentially impacting mental health during the postpartum period. 17 Particularly, in Malaysia, the six-week postpartum period is marked by specific practices aimed at ensuring the mother's recovery and preventing ailments associated with cold and wind. 18 Common practices during this period across the Malay and Indians include hot compresses, herbal baths, body wraps, and massages; and dietary restrictions favour warm foods and herbal tonics while avoiding cold, ‘windy,’ or potentially harmful foods. 19 Bathing practices among the Chinese are often caution against early bathing or frequent hair washing with limitation of water intakes. 20 These cultural practices often result in mothers being confined to their home during this period.10,19
In addition, the shortage of mental health professionals further compounds the situation. 21 Furthermore, the existing psychological treatment options have their limitations arising from the social stigma attached to accessing them, resource scarcity, and logistical difficulties.21,22 Consequently, facilitating a more accessible avenue for healthcare services and health information becomes imperative to support these mothers.
In Malaysia, the National Department of Statistics 23 reported that in 2021 approximately 98.7% of the citizens used mobile phones. Household access to information technologies was also notably high, with 95.5% of households having internet access, 99.6% owning a mobile phone, and 88.3% having a computer. 23 With the widespread use of smartphones across different socioeconomic groups in Malaysia, where there is only a small margin of difference in internet usage between rural (94.5%) and urban areas (98.3%), digital tools offer a promising opportunity to improve the delivery of mental health care. 24 mHealth technologies, such as mobile applications and SMS-based support, have the potential to revolutionize the management and treatment of PPD. These digital interventions can provide continuous mental health support, education, and monitoring to new mothers, effectively bridging gaps in traditional healthcare services. The success of digital health initiatives in Malaysia, such as the KOSPEN@Activ 25 program and the MySejahtera application 26 during the COVID-19 pandemic, highlights the potential of mHealth to engage and motivate users. MySejahtera, for example, enabled wellness self-assessments and health monitoring, and supports the Ministry of Health in tracking health needs and implementing timely interventions. 26
Adapting similar strategies for PPD could significantly improve access to care, reduce stigma, and provide culturally sensitive support tailored to the specific needs of Malaysian mothers. Moreover, mHealth solutions can be easily scaled and adapted to various contexts, ensuring that even the most underserved populations receive the mental health support they need. The mHealth technologies offer a promising solution to these challenges, but they require improvement in terms of user-centred design and quality development. Compared to their Western counterparts, mHealth technologies specifically tailored for the Asian population are limited.27,28 Additionally, a systematic review reported minimal studies are currently available on the use of mHealth for perinatal depression in low- and middle-income countries. 29
Existing interventions often lack a user-centred design from the outset and frequently include users during the later stages of testing, resulting in the prototype being ultimately designed by healthcare providers instead of end-users. 30 User-centred design (UCD) is an iterative process that prioritizes the needs, wants, and limitations of end users, ensuring the final product is highly usable, accessible, and enjoyable. 31 Although patient engagement was included in the development of interventions, it was focused on pre-existing content and lacked emphasizing their digital capability, thus rendering the developments truly non-user-centred.32–35 The World Health Organization (WHO) advocates for integrating the user-centred approach into the lifecycle of mHealth technologies to ensure effective outcomes, addressing both functionality and usability. 36
The underrepresentation of Asian mothers’ perspectives as recipients of mHealth technologies also calls for additional evaluation to create impactful interventions. Hence, the objectives of this study were to gain insights into the experiences of Asian mothers, particularly in Malaysia, when dealing with PPD and to explore their perspectives regarding mHealth technologies during the postpartum period.
Methodology
Approach
A qualitative methodology was utilized to capture mothers’ viewpoints on PPD issues. Given the sensitivity of the topic, especially within the cultural and religious contexts of Malaysian women, an in-depth interview approach was chosen instead of a focus group discussion. This method provided a more personalized and secure environment, allowing participants to discuss sensitive issues without the discomfort of group dynamics. It also minimized the risk of participants feeling pressured or inhibited by more dominant group members, ensuring they could freely express their views and foreclose topics they found uncomfortable. 37 Furthermore, the Malaysian culture emphasizes indirect communication, humility, accommodation, and politeness, particularly when discussing sensitive topics like mental health.38,39 In our study, these cultural values were respected by delivering questions based on participants’ cues and responses. The interviewer carefully respected each participant's responses, ensuring that they felt comfortable sharing their experiences with PPD. This approach allowed for an open dialogue that honoured both the cultural and religious contexts of the participants, including the importance of faith in God.
Research setting
The research took place in public hospitals located in the Selangor State of Malaysia after obtaining the relevant ethical approval from the Malaysian Medical Research and Ethics Committee (MREC), with reference number: NMRR ID-22-00169-FGH (IIR), as well as the Universiti Kebangsaan Malaysia Medical & Research Committee, with reference number: UKM PPI/111/8/JEP-2021-890. Selangor, one of the 13 states of Malaysia, is located in the western part of Peninsular Malaysia and is the most populous and highly urbanized state with approximately 6.5 million residents (Department of Statistics Malaysia, 2021), contributing 25.9% to Malaysia's GDP in 2023. According to the Department of Statistics Malaysia (2020), Selangor has the highest birth rate in the country, with a total of 95,211 live births in 2019. 40 In Malaysia, women received postnatal care in Community Health Clinics, and if symptoms suggestive of PPD were identified, they were referred for further evaluation and treatment to the hospital's psychiatric clinic. This study was conducted at the public hospitals’ psychiatric clinic. Written informed consent was obtained from all patients prior to the conduct of the interviews. To protect the privacy and confidentiality of the participants, all identifiers were removed. Data collection was from January 2022 to June 2022. The Consolidated criteria for reporting qualitative research (COREQ) guideline was adopted in reporting this research (see Supplemental file II).
Sampling and recruitment
Mothers were purposively sampled from the Malaysian public hospital outpatient follow-up psychiatric clinics in the state of Selangor. They were recruited if they had symptoms suggestive of PPD according to the Diagnostic and Statistical Manual of Mental Disorders (Fifth Edition), 41 were literate in the English or the Malay languages, were within the first year postpartum, and were at least 18 years old. Those who were unstable with psychotic symptoms (i.e. mothers with active symptoms of psychosis as reported by the attending doctor or Glascow Coma Scale of less than 15), had a history of drug abuse (to eliminate other pre-causal factors for depression), or had a previous experience of stillbirth or intrauterine death were excluded from the study. A research advertisement was circulated within the psychiatric clinics to aid in recruitment. Additionally, treating doctors also approached potential participants to inquire about their interest in joining the research. Totally 10 mothers were approached, and six consented for the research. Upon agreement, the mothers who consented were then approached online to be included in the in-depth interviews. The mothers were consistently reminded about the option to withdraw voluntarily, decline to answer any questions, and have the freedom to halt the interview if they felt uncomfortable at any point during the process.
Data collection and analysis
A semi-structured interview guide (Table 1) was pre-tested prior to its use by SSK, a female medical doctor with more than 10 years of clinical experience and a certified mental health first aider, together with SS, a team member experienced in qualitative research and familiar with the target group. The participants were assigned pseudonyms during their interviews. They were informed that the researcher conducting the study had a professional background in public health, with a specific interest in PPD. The researcher's personal goal was to understand the lived experiences of mothers facing PPD to improve postpartum mental health. The participants were aware that the research aimed to contribute to better healthcare services and support for women experiencing PPD. No prior relationship was established between the researcher and participants before the study began.
Semi-structured questions in the interview guide.

The interviews were conducted using a secure online platform, with audio recordings that were kept anonymous and delivered by SSK. During the interviews, the initial questions listed in Table 1 were followed by specific prompts based on the participants’ answers. For example, if a participant mentioned no mental health assessment was done at the postnatal clinic, we would prompt further with questions such as, ‘Can you elaborate on that?’ or ‘How did that make you feel?’. To ensure a comprehensive exploration of participants’ experiences, we used additional prompts tailored to each primary question. Examples include: For PPD Experience: ‘Can you describe how PPD affected your daily life?’, ‘What specific challenges did you face during this time?’, or ‘What did you do to cope with PPD?’. For Postnatal Care and Mental Health: ‘Were there any aspects of the care that you found particularly helpful or unhelpful?’ or ‘What was your expectation?’. For Technology and mHealth: ‘Have you used any digital tools for mental health support or health before?’ or ‘What would make you more likely to use such technology?’. For Features of mHealth for PPD: ‘What specific features would you find helpful in a digital tool for PPD?’ or ‘Can you share more about any particular app or resource you have used?’. These prompts facilitated in-depth discussions, enabling us to capture nuanced insights into the participants’ experiences.
Based on the mothers’ preferences, one interview was conducted in the English language, while five other interviews were conducted in the Malay language. While Malay language is the national language of Malaysia, English language is also widely used by the population. 42 Iterative questioning was employed to resolve discrepancies and acquire clarifications on issues raised by the mothers. This involves asking additional questions to clarify and ensure accurate understanding of the patients’ statements. After each interview, notes were made on the mothers’ emotions and non-verbal cues. Mothers were enrolled in the study until data saturation was attained, a point agreed upon by all members of the research team whereby further interviews were unlikely to yield substantially new insights. Repeat interview was not required. All transcripts were transcribed verbatim. To guarantee preservation of the original context, two separate researchers examined the interview transcripts while cross-checking them with the field notes recorded during the interviews. The translation and transcription processes were conducted by researchers who were bilingual in the native Malay language and proficient in the English language. To prevent loss of meaning, they were instructed to retain the original context and cultural expressions, using literal translations where possible and adding notes for idiomatic phrases without direct English equivalents. The researchers were aware of potential interpretation bias, so the translators, who were familiar with the local context and culture of Malaysia, ensured that interpretations stayed true to the participants’ experiences and cultural perspectives.
A thematic analysis approach was employed to examine the data, enabling the recognition of recurring patterns, themes, and underlying meanings. 43 We used Atlas.ti 9 software to facilitate the data coding. Two researchers independently coded the data using an inductive approach, allowing themes and sub-themes to emerge naturally. They began with open coding techniques, identifying and labelling relevant phrases, sentences, and sections to capture significant codes. These initial codes were organized into categories. As the analysis progressed, the researchers refined and finalized the emerging themes and sub-themes through consensus. The research team engaged in closed discussions, ensuring proper disclosure and identification of categories, codes, and themes. Inconsistencies were resolved through team consensus, which ultimately led to the selection of meaningful themes. Trustworthiness was enhanced through investigator triangulation, inter-coder reliability assessment, and reflective memos. 44 This rigorous method ensured a thorough and accurate interpretation of the findings. After conducting six interviews, data saturation was reached. 45 This was mutually agreed by all team researches whereby additional of further input would not yield significant new insights.
Result
Sociodemographic data of respondents
Six in-depth online interviews were carried out, each lasting 60 min. The mean age of the respondents was 33.50 (SD = 2.76) years. The respondents were Malay (n = 5, 83%) and Chinese (n = 1, 17%). The majority (n = 5, 83%) were employed. Of the six mothers, four attained tertiary higher education from universities or colleges (66%), and two (34%) had completed secondary education. The period during which the women experienced symptoms of PPD occurred within 1 to 12 months before the interviews. All participants are currently under psychiatric follow-up with four diagnosis of Major Depressive Disorder and two diagnosis of adjustment disorder. All participants were referred during the postpartum period for symptoms of PPD. Among the six cases, four women reported a lack of attachment to their babies, with two experiencing severe anxiety and intrusive thoughts. Two women faced abusive environments, and four struggled with suicidal ideation and self-harm. Three women were on medication for their mental health. All mothers were receiving psychotherapy and/or counselling. Two reported that their husbands were often absent due to work commitments. The participants encountered significant challenges, including financial difficulties, lack of support, and negative thoughts about their parenting abilities (Table 2).
Sociodemographic profile of the respondents.

SD: standard deviation.
Themes
Upon exploring the experiences of PPD and perspectives on mHealth needs among Asian mothers, the following five key themes emerged: (i) existing circumstances, (ii) psychosociological reactions, (iii) maternal needs, (iv) innovation of care, and (v) pragmatic elements as depicted in Figure 1. Two overarching main themes emerged, namely, the Mother's Experiences and MHealth Elements (see Supplemental file I for table of themes, sub-themes, and codes).

Emergence of themes and sub-themes from in-depth interviews of mothers.
Existing circumstances: intrapersonal limitations during the postnatal period
The ‘Intrapersonal Limitations’ theme highlights the challenges mothers faced internally and externally during the postnatal period affecting their adaptation to motherhood.
The setting of unrealistic expectations was identified as a major concern, with mothers holding themselves to often unattainable standards, particularly in the realm of child care. This sentiment was vividly captured by one respondent, who stated, ‘So, for me, when it comes to work, I don’t really care about as much. But when it comes to kids, it has to be perfect’ (37 y/o, Respondent 1). This highlights the self-criticism and disappointment when these standards were not met. She further informed about her frustration with the lack of support, ‘I expected more help, but he [husband] didn’t meet that expectation…I am the one have to burn out, right?’ (37 y/o, Respondent 1).
The stress related to feeding ideals further exacerbated mothers’ experiences. The pressure to exclusively breastfeed led to significant stress, as evidenced by one mother's statement, ‘Because baby depends on me for food, for milk…I’m not going to give her any bottle during that first 3 months’ (37 y/o, Respondent 5). The burden was intensified by breastfeeding difficulties and the perception that feeding the baby was solely the mother's duty as lamented by another mother, ‘…like nothing is flowing out…So, basically, no one can feed baby except me’ (37 y/o, Respondent 1).
Moreover, the normalization of postpartum struggles as a universal acceptance of motherhood presents another barrier to seeking help. One mother's reflection, ‘…it is something, you have to suck it up lah. ‘Cause indeed, all mothers struggle That's the thing. It's a normal thing’ (37 y/o, Respondent 1). Paranormal beliefs also played a role, with respondents considering them part of the postnatal experience, ‘I just think that maybe it's just the disturbance of the paranormal being…I think it's normal’ (29 y/o, Respondent 3).
Some mothers’ struggle was deeply revealed by their inadequate coping mechanisms, including self-harm and aggression towards the baby, as one informed, ‘Maybe if I’m depressed or stressed, maybe I hit the pillow, hit myself with a ruler, hanger like a ruler, or [similar] things like that’ (29y/o, Respondent 3). While another shared, ‘I yell at the baby. I say, ‘Shut up, shut up’ I feel so stressed at that time. I feel like one day I want to throw my baby, hit my baby's head to the wall’ (37 y/o, Respondent 5).
Existing circumstances: unsupportive environmental conditions
Mothers frequently faced the challenge of their husbands’ absence and inaccessibility due to demanding work schedules, which left them feeling isolated. One mother shared, ‘I feel like [living] alone. Raise this child, [with] no husband. One, because my husband is [working] offshore. It is difficult to contact him’ (29 y/o, Respondent 3). Another added the difficulty of coping with her husband's shifts, ‘Night work, night shift, double shift. I didn’t receive much support from my husband’ (37 y/o, Respondent 5).
Conflicting sociocultural beliefs further compound these challenges, especially for those living with in-laws and parents. Differences in parenting styles, feeding practices, and the stigma associated with seeking mental health support led to stress, as one mother elaborated, ‘Their [in-laws] way is a bit strict…Sometimes [only] sleep for an hour…was so stressful there’ (32 y/o, Respondent 4). The stigma around mental health was another source of tension, ‘I once wanted to go to counselling; Mom and Dad knew, and they got angry’ (32 y/o, Respondent 4).
Negative family conflict and unrealistic expectations also intensified the postpartum stress. Occurrences of verbal and physical abuse were not uncommon, ‘She [mother-in-law] tells bad stories about me…she always hits me’ (31 y/o, Respondent 2). Finally, unintended events such as unplanned pregnancies and health complications brought about significant stress. The overwhelming feeling is as described as, ‘the main reason would be it's like an unplanned one, so first problem already. So then, of course, not prepared and overwhelmed’ (36 y/o, Respondent 1). Emotional turmoil of having a child in the Neonatal Intensive Care Unit (NICU) was also particularly distressing, as one described, ‘I can’t sleep, as long as my son is in the NICU, I don’t feel happy’ (29 y/o, Respondent 3).
Theme 2: psychosociological reactions
The postpartum period often brings about profound psychosociological changes, encompassing alterations in emotions, cognition, and social interactions, which significantly impact mental health and overall well-being. Mothers articulated deep-seated feelings of inadequacy and failure, with one stating, ‘I think my main problem is I feel like a failure, like a failed mum…I always have this fear’ (37 y/o, Respondent 1). Such self-doubt extended to severe aversions, as another mother confessed, ‘It felt like I didn’t want to hold my child…Please take it away; I didn’t want to see [the baby]’ (35 y/o, Respondent 6). The intensity of these emotions sometimes escalated into psychosis, with hallucinatory experiences linked to profound guilt and stress, ‘I couldn’t sleep. Then I saw her [in-law] shadow…all that was going around in my head’ (31 y/o, Respondent 2), and, ‘I was hearing things… ‘I’m a useless mother’’ (29 y/o, Respondent 3).
Negative emotions often led to adverse temperamental actions and detachment issues, revealing a darker aspect of parenthood that involved anger and aggressive behaviours previously unrecognized by the mothers themselves. This was illustrated by a mother who discovered her capacity for anger post-childbirth, ‘A lot of things. Is mainly, it's anger…a lot of people only started seeing their angry self after they have kids’ (37 y/o, Respondent 1). Another mother's aggressive act towards her baby underlines the severity of these changes, ‘My mother saw me throw the baby on the bed’ (29 y/o, Respondent 3), while bonding issues were also noted, ‘1 month after I settle [established] the breastfeeding before I [actually] felt attached [to the baby]’ (37 y/o, Respondent 1).
Additionally, mothers reported physiological impacts, including loss of appetite and neglect of self-care, further complicating their postpartum recovery, ‘I really did not have any appetite to eat, to sleep. I didn’t want to take care of myself because my focus was on my child’ (32 y/o, Respondent 4).
Theme 3: maternal needs
Unaccommodating access to professional care
Mothers expressed concerns over health clinic staff prioritizing physical health over mental well-being, feeling overlooked in their psychological needs. One mother described the detached treatment as, ‘People act like robots. Not even once they asked: how are you doing? How are you doing as a mother?’ (37 y/o, Respondent 5). The lack of mental health support was echoed by another, ‘Sometimes at the clinic, those posters [health promotion] do help…but I don’t see posters about mental health’ (35 y/o, Respondent 6). Privacy concerns and difficulty building rapport in clinical settings were also highlighted, with mothers feeling uncomfortable discussing personal issues, ‘The rooms, for the mother's room, they want to check [examination], it's small…I am ashamed to tell you that I have a problem’ (31 y/o, Respondent 2).
Challenges of well-being
Neglect of self-care was commonly expressed with mothers putting their babies’ needs first, leading to physical health consequences, ‘So, I didn’t take care of my stomach, until my caesarean stitches opened’ (31 y/o, Respondent 2). The need for resources in baby care and handling was evident, with suggestions for videos, ‘I think if there is an app that could really explain to you what you should do as a new mother to create that bond’ (37 y/o, Respondent 5), and, ‘Maybe they could provide videos of activities with children’ (29 y/o, Respondent 3). Respecting a mother's feeding choice is essential, as one mother emphasized, ‘So, even if she wants to stop, I think we should respect the decision’ (37 y/o, Respondent 1). Conversely, providing breastfeeding support were also highlighted, ‘Can provide food that can make a lot of milk. How to latch, erm, [the] baby?’ (32 y/o, Respondent 4).
Support from husband and others
Mothers desired more understanding and involvement from their partners and families. Fathers’ lack of confidence in childcare was a barrier, ‘He saw the baby crying, at that time he also panicked’ (37 y/o, Respondent 5). Another shared, ‘Like [husband] helping to cook, helping to take care of the children. Help, yes, help from many angles, both mentally and physically. Just be there, even my mother is around, I still want my husband to be here’ (32 y/o, respondent 4). The need for family awareness on mental health was stressed, ‘At first, my mother really couldn’t accept it. They think like, mentally ill people are crazy. They don’t know’ (29 y/o, Respondent 3), alongside the desire for emotional support beyond mere positivity, ‘A lot of time, they [husband] just say you just think positive…But that doesn’t help’ (37 y/o, Respondent 1).
Theme 4: innovation of care
Digital support hub
Mothers found virtual platforms particularly practical during the confinement period and the COVID-19 pandemic. One mother shared, ‘These moms, it's not that they don’t want to get help, but they are not confident; they are scared or embarrassed. So, the first step is to get help from the virtual world’ (39 y/o, Respondent 3). The ease of access to virtual consultations was valued, ‘Even my first consultation with psychiatrist was done virtually. I couldn’t find anyone to take care of my child for too long’ (37 y/o, Respondent 1), while another suggested using QR codes for easy access to information, ‘[For example] Please scan this to join us. You can do it at the hospital and at home as well’ (35 y/o, Respondent 6). The convenience of having resources available on a phone was also appreciated, ‘It's easy to find information’ (32 y/o, Respondent 4).
Nurturing self-care
Professional-guided therapies were highlighted for effective support, with one mother emphasizing the importance of seeking professional advice, ‘If I go to a professional, counselling, I know. It is possible to diagnose this diagnosis’ (32 y/o, Respondent 4). Early intervention was recommended, ‘I think my advice to the mothers: if you have [symptoms], you just need to talk to someone. Find someone, professional, get help early’ (37 y/o, Respondent 5). Emotional coping strategies such as breathing techniques and music therapy were shared, ‘Yes, the breathing technique is there [available]…can be applied, very helpful’ (29 y/o, Respondent 3), and spiritual practices were mentioned as coping mechanisms, ‘Dzikir … can calm the soul for the mothers if people can feel’ (37 y/o, Respondent 5). The importance of self-care was stressed, with mothers advocating for reminders to prioritize their well-being, ‘Self-care, I guess, is important as well lah. Need to learn to take care of self’ (37 y/o, Respondent 1), and finding joy in personal hobbies, ‘So just plant some plants…My house is like a garden…it's effective lah, it makes me happy…Until the voice disappeared. Can remind others to do things they enjoy’ (31 y/o, Respondent 2).
Theme 5: pragmatic elements
Engagement for relevance
Pragmatic elements in mHealth refer to the practical features and usability aspects that enhance the effectiveness and user engagement of mHealth solutions. For mHealth technologies to succeed, they must be culturally relevant and locally accessible. This theme highlights the importance of content localization, language options, automatic reminders, motivational prompts, and supportive platforms. One mother noted the lack of Malaysian content, ‘No… don’t think there's anything from Malaysia’ (37 y/o, Respondent 1), while another stressed the need for Malay language options, ‘But there isn’t yet in Malay language. If can let it be in the Malay language, everyone can hear and understand’ (31 y/o, Respondent 2). This localization fosters a sense of comfort and connection, as mothers prefer engaging with content reflecting their own community, ‘Look at people like us who have the same problem…if from our [own] people, I will feel more comfortable’ (31 y/o, Respondent 2).
Automatic reminders and motivational prompts were also seen as essential features to enhance app effectiveness. Mothers suggested mood check-ins and inspirational quotes, ‘Maybe a reminder thing, a notification thing that asks how are you feeling this morning?’ (37 y/o, Respondent 1), and, ‘Example an app, they release the best verses of the Quran [The Quran is the holy book of Islam, serves as the ultimate source of guidance for Muslims 46 ]….This is my suggestion’ (29 y/o, Respondent 3).
Furthermore, the importance of a supportive platform for sharing experiences and receiving professional guidance was highlighted as it alleviates feelings of isolation and overthinking, ‘When an expert speaks, we tend to follow their guidance…If not, we just keep overthinking and feeling stressed’ (35 y/o, Respondent 6). The ability to document moods and events was suggested to aid in medical consultations, ‘It [bullet journal] actually provides like a mindfulness exercise lah, and somehow you are calm, good for you to actually write’ (37 y/o, Respondent 1), and, ‘Better to write a diary…anything happens in the app…We can show [the doctor], we don’t know what to say’ (29 y/o, Respondent 3).
Discussion
This study aimed to explore the experiences of mothers accessing mental health care in Malaysia, which unveiled noteworthy themes that may be incorporated for future mHealth technologies targeting postpartum mothers. Malaysia, with its rich tapestry of multi-ethnicities offers a distinctive context for examining PPD, especially in a setting where mHealth technologies have predominantly been orientated towards the Western and high-income countries. 29
Similar to a local study 47 where mothers perceived PPD as a minor and temporary emotional issue tied to personal challenges, our research identified a more profound connection between detrimental core beliefs and unachievable maternal expectations, which heightened the risk of PPD. Personal and societal expectations define what it means to be a ‘good mother’, which often pushes our mothers to prioritize their baby's needs over their own. This sets a high standard for mothers that includes the pursuit of nurturing the perfect baby. Consequently, mothers will then face increased scrutiny about their maternal capabilities. Research by Sim & Waterfield, 48 Haga et al., 49 and Adams et al. 50 illustrate how such intense pressure not only reinforces unrealistic expectations but also heightens feelings of inadequacy, guilt, and shame when these standards are not met. Through mHealth technologies, self-care education and dealing with unrealistic expectations and negative thoughts, while also reducing feelings of comparison and inadequacy among mothers, remains important.
Furthermore, the sense of overwhelming responsibility felt by the mothers was considered customary, culturally acceptable, and a part of their motherhood journey that they were expected to bear alone. This normalization of PPD may be rooted in deep-seated false beliefs from patriarchal ideologies, cultural norms, and religious beliefs, which can present a significant barrier for Asian mothers seeking assistance.51–53 In Malaysia, negative connotations such as ‘meroyan’ and ‘gila’ (crazy or madness) are commonly used to describe post-childbirth emotional instability. 54 Moreover, our study also highlights maternal experiences of PPD as a common aspect of motherhood. Approximately 80% of mothers will experience ‘baby blues’, defined as a short duration of symptoms with no long-lasting effects.55,56 However, this perception of normalcy extends further among our mothers. States of delusion and hallucination are considered normal aspects of confinement, at the same time linking them to paranormal disturbances. Dean et al. 57 explained that paranormal belief refers to the acceptance of phenomena that were beyond the scope of scientific explanation, such as telepathy, life after death, and supernatural occurrences. Attributing psychological illness to supernatural forces like Jinn or the evil eye is a widespread belief among Muslims, especially in Middle Eastern countries. 58 Similarly, in Malaysia, there's a tendency among traditionally conservative individuals to eschew medical treatments and seek help from religious practitioners. A local study reported that 54% of patients had at least one contact with a traditional healer before engaging psychiatric services. 59 This highlights the need to embed PPD education in mHealth technologies to challenge cultural misconceptions and promote acceptance of professional mental health support.
Interestingly, in contrast with previous researches emphasizing the value of peer support,60–63 our study highlights the noteworthy sense of isolation experienced during the confinement period. This intriguingly persisted even when mothers had their own female caregivers with them. Yamada, Isumi, & Fujiwara 64 also showed that Japanese mothers faced a substantial risk of PPD in the absence of partner support, despite peer assistance. Some husbands appeared unsure about what to do when they were present. This ‘parental loneliness’ may lead to difficulties in establishing intimacy and emotional closeness, while increasing risks of PPD.65–67 As a result, the mothers in our study expressed a wish for their husbands to be more involved and understanding, suggesting the inclusion of straightforward instructions in the mHealth technology for both newborn and maternal care.
Some of the mothers reported the emotional toll of living with extended family and adhering to traditional confinement practices. While some studies have found such support to be beneficial, 68 our findings align with research in the Arab context showing the negative effects of such support, particularly due to extended family interference in self-care and baby care. 69 Similarly, as reported, poor family relationships can adversely affect maternal mental health.7,70,71 Mothers in the study needed support but couldn't easily express their needs. Malaysia's traditional gender roles further limit mother's opportunities to develop interpersonal skills outside caregiving, often prioritizing family responsibilities over personal or professional growth.72,73 Cultural norms in Malaysia emphasize conservative behaviour to avoid actions that bring shame to maintain one's reputation within the community. 73 The distinct communication patterns in Malaysia's collectivist culture prioritize group needs over individual ones, promoting harmony and consensus but potentially limiting open dialogue and individual expression. 38 Combined with the conservative nature of Malaysian society, this can complicate interactions within family and healthcare settings.38,39
Incorporating interpersonal skills into mHealth technology is essential for better communication between mothers, their partners, and families, ensuring needs are clearly articulated and met. An mHealth app can effectively bridge these cultural gaps. By providing educational content tailored to these cultural contexts, the app can offer comprehensive information on postpartum care and mental health. It can include guidelines on when and how to seek help, what symptoms to watch for, and available resources. Studies have shown that mHealth technology can significantly improve maternal health outcomes by providing accessible, cost-effective, and relevant support.74–77 For example, educating mothers on the importance of proper hydration and nutrition despite traditional confinement practices can reassure them that these are crucial for recovery and mental health.
Modules on assertive communication techniques can help mothers practice and develop their communication skills in a safe environment without feeling guilty about saying ‘no’.78,79 Enhanced communication skills lead to better postpartum care, as mothers can articulate their needs more effectively, adhere to medical advice, and seek help promptly, reducing health risks for both mother and baby. 80 These skills also promote marital satisfaction through more effective and satisfying interactions between spouses, aiding in conflict resolution and reducing stress.80,81 Improved communication reduces feelings of isolation and helplessness common in the postpartum period, boosting confidence and self-efficacy, and leading to better mental health outcomes.80,82
In the context of increasing urbanization in Asia, countries like Malaysia, classified as a middle-upper income country, 83 are witnessing a cultural shift towards Western norms, which prioritize individualistic responsibilities. 17 This transformation, coupled with the social isolation and economic pressures that urban living often entails, has been linked to heightened symptoms of depression among mothers. 84 The reduction in domestic support, due to fragmentation of families and the tendency for being distanced from relatives, are contributing factors to the escalating rates of depression. 84 Recognizing these shifts, it is also crucial to provide remote support to some mothers facing isolation and adapting to these changes alone.
Compared to their Western counterparts, Asian populations have traditionally shown a lower tendency towards seeking and utilizing mental health services. 85 This reluctance is largely attributed to cultural factors such as shame and a concern for maintaining family honour, which greatly inhibit their readiness to pursue mental health support, as highlighted in studies by Goffman (2009) 86 and Gee et al. (2020). 87 Similarly, mothers in our study identified stigma, lack of awareness, and privacy concerns as factors that limit their access to care. Mothers felt that the healthcare system often falls short in addressing mental health. Privacy issues and perceived work pressures on healthcare professionals, as previously highlighted in the literature, restrict time and empathy for addressing maternal mental health.47,70 Additional obstacles such as slow rapport with counsellors and logistical issues during confinement were reported. Compounding this issue, the impacts of COVID-19 drastically limited access to mental health support. A 2020 survey by the WHO indicated that over 60% of countries reported diminished access to antenatal or postnatal services as a consequence of the pandemic. 88
Despite giving birth in a WHO-endorsed ‘baby-friendly hospital’ as part of the breastfeeding initiative, 89 mothers still faced breastfeeding challenges, particularly at home. The availability of lactation experts and diverse feeding techniques was deemed inadequate. According to the 2022 Malaysian national survey, 90 only half of the mothers continued breastfeeding past the first year. The pressure to exclusively breastfeed often left them feeling overwhelmed, inadequate, and compelled to meet societal and self-imposed standards. A local study showed that while higher breastfeeding knowledge is linked to a greater likelihood of exclusive breastfeeding, the discrepancy between knowledge and practice, as seen in a Saudi Arabian study, underscores the importance of addressing this gap.91,92 De Roza et al. 93 also advocated the need for ongoing support and improvements in breastfeeding self-efficacy, pointing out the crucial role of sustained efforts in boosting knowledge and skills for comprehensive breastfeeding support at home.
In designing future mHealth technology, our mothers highlighted mHealth as a pivotal tool that can provide quick and remote assistance. This approach aligns with international practices of utilizing technology for multifaceted support.94–96 Our mothers stressed the significance of culturally resonant contents in the local language in order to boost accessibility.70,97 Incorporating mood trackers and motivational elements was also highlighted to foster user engagement and mental well-being, drawing upon positive psychology and behavioural intervention principles.98,99 The mHealth could also offer remote access to exercises aimed at managing negative thoughts and promoting constructive thought patterns based on cognitive–behavioural theories. 100 Incorporating simple spiritual elements, such as prompts for reciting spiritual prayers, into mHealth technology was advocated by our mothers. This suggestion is supported by research indicating a protective association between spirituality and depression.101–103 Mothers also suggested engagement features like automatic notifications that are aimed at addressing retention challenges.98,99
Recent research highlights the importance of comprehensive care for PPD, including psychoeducation, relationship management, and self-care, all necessitating healthcare worker involvement.104–106 The United States Reach Out, Stay Strong, Essentials (US ROSE) programme, a leading preventive measure for PPD, offers several prenatal sessions and a postnatal booster, delivered by healthcare professionals. 106 However, the scarcity of mental health professionals in Asia, particularly in countries such as Malaysia with a psychiatrist-to-population ratio of only 1.27 per 100,000, underscores a significant challenge. 21 This issue is exacerbated in the broader Southeast Asian region, where most countries fall into the low-income category and face a treatment gap of 90% due to financial constraints and a severe shortage of human resources. 21 With 9 out of 11 countries in this region having fewer than one psychiatrist per 100,000 people, which is significantly below the WHO's recommended 1:10,000,21,107 the need for innovative digital solutions becomes even more critical in prioritizing preventive care.
Malaysia's national clinical guidelines recognize treatment for PPD, yet the absence of targeted preventive strategies in health policy and the impact of the pandemic call for digital solution-driven national policies. 108 In Malaysia, mental health services are primarily managed in the hospital through referrals from the primary care (community clinics). Leveraging technologies with elements in Figure 2 can significantly enhance early detection and prevention, streamlining the path to mental health services for mothers within the primary care. This holistic approach resonates with The American College of Obstetrics & Gynaecology's 2018 recommendations and WHO's latest recommendation of digital communications in 2022 for positive postnatal experiences.109,110 For example, Australia's government-backed digital Perinatal Mental Health Check Program using the iCOPE digital screening tool and the UK's extended digital postnatal care plans shows the promising benefit of technology in addressing PPD.111,112 These initiatives underscore the effectiveness of leveraging technology to address PPD and illustrate the vital role that national policies play in catalyzing the adoption of digital health technologies. Importantly, dedicated funding, multidisciplinary approaches, and a network that connects private, non-governmental organizations (NGO), and public sectors with patients remain crucial. The early postpartum period is crucial for adopting mHealth technologies and aligns with mothers’ preferences for a blend of self-guided and remote professional support. Integrating such technologies into primary healthcare can improve comprehensive follow-up care accessibility, enhance health outcomes, and offer preventive and therapeutic measures for PPD.
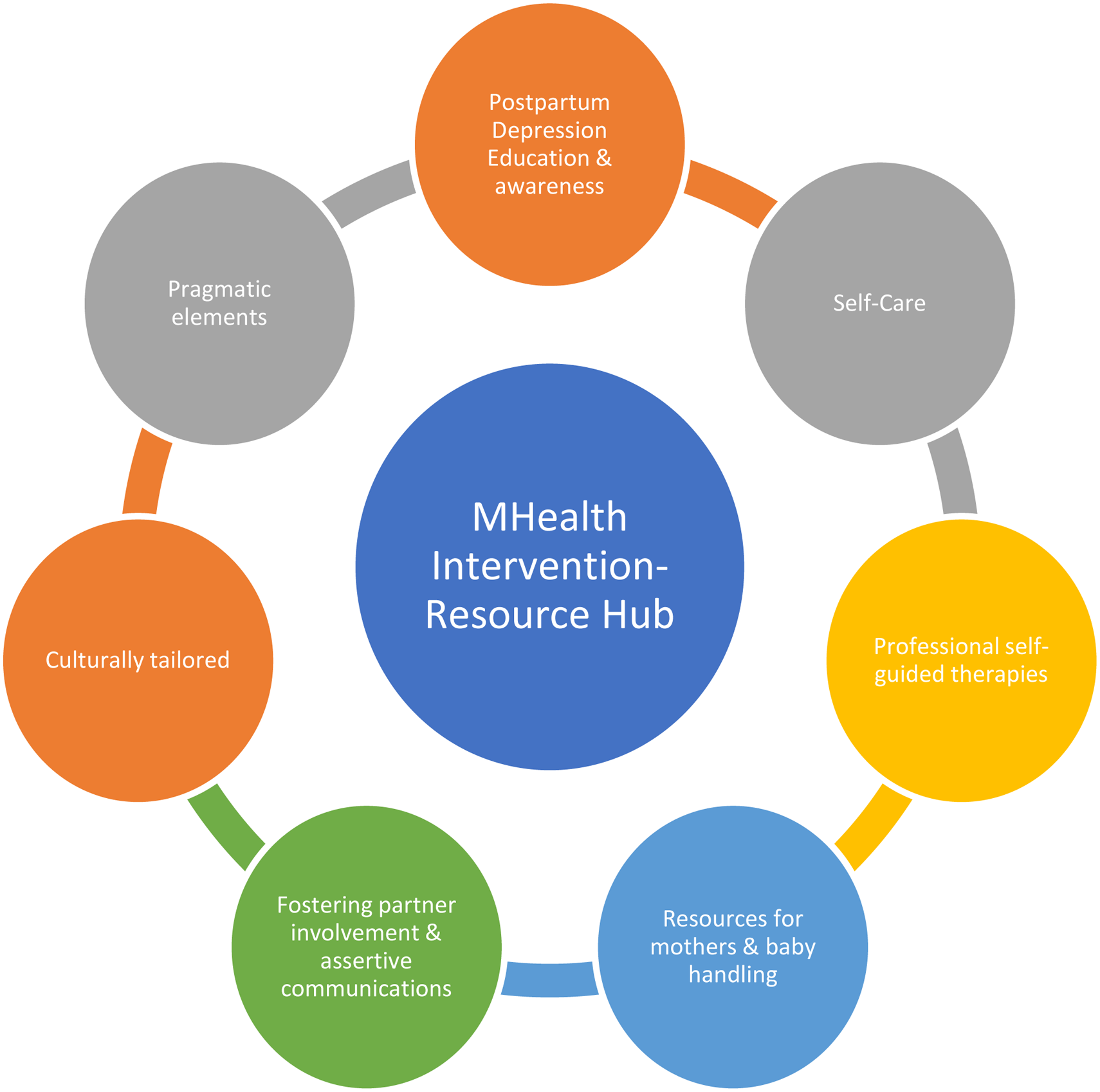
Elements for comprehensive postpartum mHealth hub suggested by respondents.
Strengths and limitations
We used in-depth interviews, which enabled the exploration of sensitive topics and the achievement of data saturation. Notably, our respondents were patients with real-time access who could offer valuable user-centric perspectives in an Asian context. This enriched our understanding of the current situation. However, it is important to note that the majority of respondents were Malays, the most prevalent ethnic group in Malaysia. Future research endeavours should aim to increase participation from other ethnic groups to encompass Malaysia's multi-ethnic culture and provide a more comprehensive perspective. Additionally, the sample size is relatively small, which is commonly reported in homogeneous groups. However, with purposive sampling, this approach supported deep, case-oriented analysis and the selection of ‘information-rich’ cases, allowing for a detailed and nuanced exploration of the phenomenon.
Conclusions
Our study sheds light on the complexity of PPD among Asian mothers highlighting how it is often normalized in their journey into motherhood. The study highlights that postpartum mothers need mHealth technology to provide remote guidance, self-care resources, professional assistance, and to foster partner involvement through assertive communication as these are viewed as viable solutions for enhancing mental health services especially in resource-constrained Asian countries.
List of abbreviation
Supplemental Material
sj-pdf-1-dhj-10.1177_20552076241292679 - Supplemental material for Exploring Asian maternal experiences and mHealth needs for postpartum mental health care
Supplemental material, sj-pdf-1-dhj-10.1177_20552076241292679 for Exploring Asian maternal experiences and mHealth needs for postpartum mental health care by Siti Sabrina Kamarudin, Idayu Badilla Idris, Norfazilah Ahmad and Shalisah Sharip in DIGITAL HEALTH
Supplemental Material
sj-docx-2-dhj-10.1177_20552076241292679 - Supplemental material for Exploring Asian maternal experiences and mHealth needs for postpartum mental health care
Supplemental material, sj-docx-2-dhj-10.1177_20552076241292679 for Exploring Asian maternal experiences and mHealth needs for postpartum mental health care by Siti Sabrina Kamarudin, Idayu Badilla Idris, Norfazilah Ahmad and Shalisah Sharip in DIGITAL HEALTH
Footnotes
Acknowledgements
The authors would like to express gratitude to the Department of Public Health Medicine, Faculty of Medicine, Universiti Kebangsaan Malaysia & Director General of the Health Ministry of Malaysia for the approval of the publication of this paper.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author upon reasonable request.
Contributorship
SSK, IBI, NA, SS: conceptualization. SSK & IBI: data curation. SSK & IBI: formal analysis. IBI: funding acquisition. SSK, IBI & SS: investigation. SSK, IBI, NA, SS: methodology. SSK: project administration. SSK: software. IBI, NA, SS: supervision. IBI, NA, SS: validation. SSK, IBI, NA, SS: visualization. SSK: writing – original draft. SSK, IBI, NA, SS: writing – review & editing.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this paper.
Ethical approval
The study proposal, interview guide, and written consent information sheet have been approved by the Malaysian Medical Research and Ethics Committee (MREC), with reference number: NMRR ID-22-00169-FGH (IIR), as well as the Universiti Kebangsaan Malaysia Medical & Research Committee, with reference number: UKM PPI/111/8/JEP-2021-890. Written informed consent was obtained from all patients prior to the interviews. To protect privacy and confidentiality of the participants, all identifiers were removed.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Guarantor
IBI serves as the guarantor for this paper, taking responsibility for the integrity of the work as a whole, including the accuracy of the data and analysis.
Supplemental material
Supplemental material for this paper is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
