Abstract
Objective
Chronic pain affects approximately 7.6 million Canadians and access to care remains an issue. The Power Over Pain (POP) Portal offers immediate access to evidence-based resources ranging from low- (e.g. education, self-management), to high- (e.g. individual counseling) intensity. We explored the POP Portal's acceptability, usability, and perceived usefulness among patients newly referred to a tertiary care pain clinic.
Methods
We used a descriptive, qualitative approach with a prospective cohort of 60 adult patients recently referred to The Ottawa Hospital Pain Clinic. Patients were offered an orientation session and asked to participate in a seven-week follow-up interview. Data were thematically analyzed in an iterative process, whereby responses were reviewed and coded by two members of the research team.
Results
Of the 60 patients referred to the POP Portal by clinic clerks, 45 participated in the orientation session, and 40 completed a four-week follow-up. All 40 patients had used the POP Portal and recommended that we continue to offer the POP Portal to patients awaiting care. We identified overarching themes of acceptability (five subthemes), usability (ten subthemes), accessibility (three subthemes), and patient value of the POP Portal (three subthemes). This includes (1) the POP Portal provides easy access to chronic pain resources; (2) the POP Portal is helpful in developing an understanding of chronic pain; and (3) improvements to the POP Portal are needed to increase usability and foster a user-friendly experience.
Conclusions
The POP Portal offers accessible and diverse resources for people living with pain awaiting a tertiary care consultation; however, patients would like to see resources specific to diagnosis. Improvements are suggested to allow greater increase the POP Portal usability.
Chronic pain (CP) affects approximately 7.6 million youth and adults living in Canada. 1 Access to care can be challenging; more than 50% of patients referred to specialized programs wait more than 6 months (the threshold for medically unacceptable wait times), 2 with some patients waiting years or never being seen because of clinic inclusion/exclusion criteria. 3 Digital self-management resources have robust evidence attesting to their effectiveness in reducing pain severity and improving quality of life among people living with pain (PLWP) 4 ; however, these resources are not localized, and can be difficult to find.
The Power Over Pain (POP) Portal (poweroverpain.ca) is a digital platform for PLWP, codesigned by a team of researchers, healthcare providers, and PLWP. The Portal was created by and for Canadians, but it is freely accessible worldwide to anyone with an internet access, providing access to symptom self-assessments, personalized feedback on outcomes, and access to a collection of free evidence-informed interventions. These interventions include low-intensity resources such as education (e.g. LivePlanBe+ and PainU Online), medium-intensity resources including internet-delivered pain self-management courses, based on acceptance-commitment therapy or cognitive behavioral therapy (e.g. the Pain Course5–9), peer support, and live or recorded virtual workshops, and high-intensity resources such as individual counseling through Wellness Together Canada. 10 Together, these interventions can be curated for the management of a host of concerns (e.g. sleep, mood, movement). Resources are selected for the POP Portal by Lived Experience and Scientific Advisory Committees based on existing evidence of the resource, delivery, location (i.e. virtual, province specific, Canada specific), and topic (e.g. sleep quality, diagnosis, medications and substance use, financial aid). All resources are required to be free of cost to be included on the platform. The POP Portal's Lived Experience Advisory Committee consists of PLWP who meet weekly to discuss the development and direction of the POP Portal, providing insight to the Scientific Advisory Committee on how the Portal may be improved to meet the needs of PLWP. The Scientific Advisory Committee, consisting of researchers and healthcare professionals, takes this feedback to iteratively refine the POP Portal using an evidence-informed approach. Together, the two committees collaborate to have a digital platform which is curated for PLWP by PLWP while maintaining a stringent level of quality.
The Ottawa Hospital (TOH) Pain Clinic recently adapted and implemented the Stepped Care 2.0 framework 11 which resulted in improved access to a range of care options for patients. 12 Wait-times to access the pain clinic orientation session, which then provides access to several of the pain clinic's programs is between 2 and 3 months; but patients may wait several more months to access some of the clinic services. There remain windows of opportunity to support patient engagement with different treatments and resources to improve their overall ability to cope with pain and improve their well-being. As such, TOH Pain Clinic leadership is interested in integrating the POP Portal into patient's care pathway as part of ongoing quality improvement initiatives. The National Implementation Research Network (NIRN) offers guidance on the sequential steps to implementing programs into clinical settings, including (1) exploration of the problem and potential evidence-based solutions; (2) adapting the system for program installation; (3) initial implementation and making changes to the practice; and (4) full implementation of the program into the system as standard practice. 13 Aligning with NIRN's third phase of implementation, 13 the present study documents a pilot implementation of the POP Portal into the referral pathway of TOH Pain Clinic and evaluates the POP Portal acceptability and usability among patients using the Portal while awaiting their first visit.
Methods
Study design and setting
The present study is a qualitative observational implementation study, for the implementation of the POP Portal at TOH Pain Clinic, a tertiary care pain clinic in Ottawa, Ontario, Canada. This study received research ethics board exemption through a quality improvement stream by the Ottawa Health Science Network Research Ethics Board. We used the Standards for Reporting Qualitative Research and Consolidated Criteria for Reporting Qualitative Research reporting guidelines when writing our report.14,15
Patients
Patients were invited to participate in this study by TOH Pain Clinic clerks after receiving a referral to the clinic (and prior to triage process). Patients referred from January 2023 to March 2023 were screened for eligibility by clinic clerks and included (1) being 18 years of age or older; (2) had CP (ongoing, persistent, or recurrent pain for more than three months 16 ); (3) spoke French or English; (4) had access to the internet via computer, phone, or tablet; and (5) agreed to participate in the study. Eligible patients, up to a total of 60, were invited to participate in the study, whereby clinic clerks informed the patient there was an online platform called the POP Portal which offers free online pain self-management resources. Clinic clerks further asked if the patient was interested in an orientation session; if so, their information was forwarded to the research assistant. Given the aim of the study, the specificity of questions asked, application of theory, brevity of dialogue, and cross-case analysis, we anticipate reaching saturation and good information power within 60 participants. 17
Procedure
Patients who expressed interest in the POP Portal to the TOH Pain Clinic clerk were contacted via phone by a research assistant (AZ). The research assistant introduced themselves as a research assistant from TOH and confirmed the patients’ interest in being contacted about the pilot project. Information was provided about the pilot project and offered a POP Portal orientation session (refer to Figure 1). Patients provided verbal informed consent prior to participating in the study, an approved form of consent by TOH Research Institute. The orientation session was conducted by the research assistant, spanned 10–15 min, and involved an introduction to the POP Portal, navigation, and account creation as an optional enhancement feature. Patients were asked if they intended to use the Portal and informed about the opportunity to participate in a follow-up interview. Patients who attended the orientation session and agreed to a follow-up session used the POP Portal with no set instructions. Patients were contacted by the research assistant to complete an interview after a four-week period.
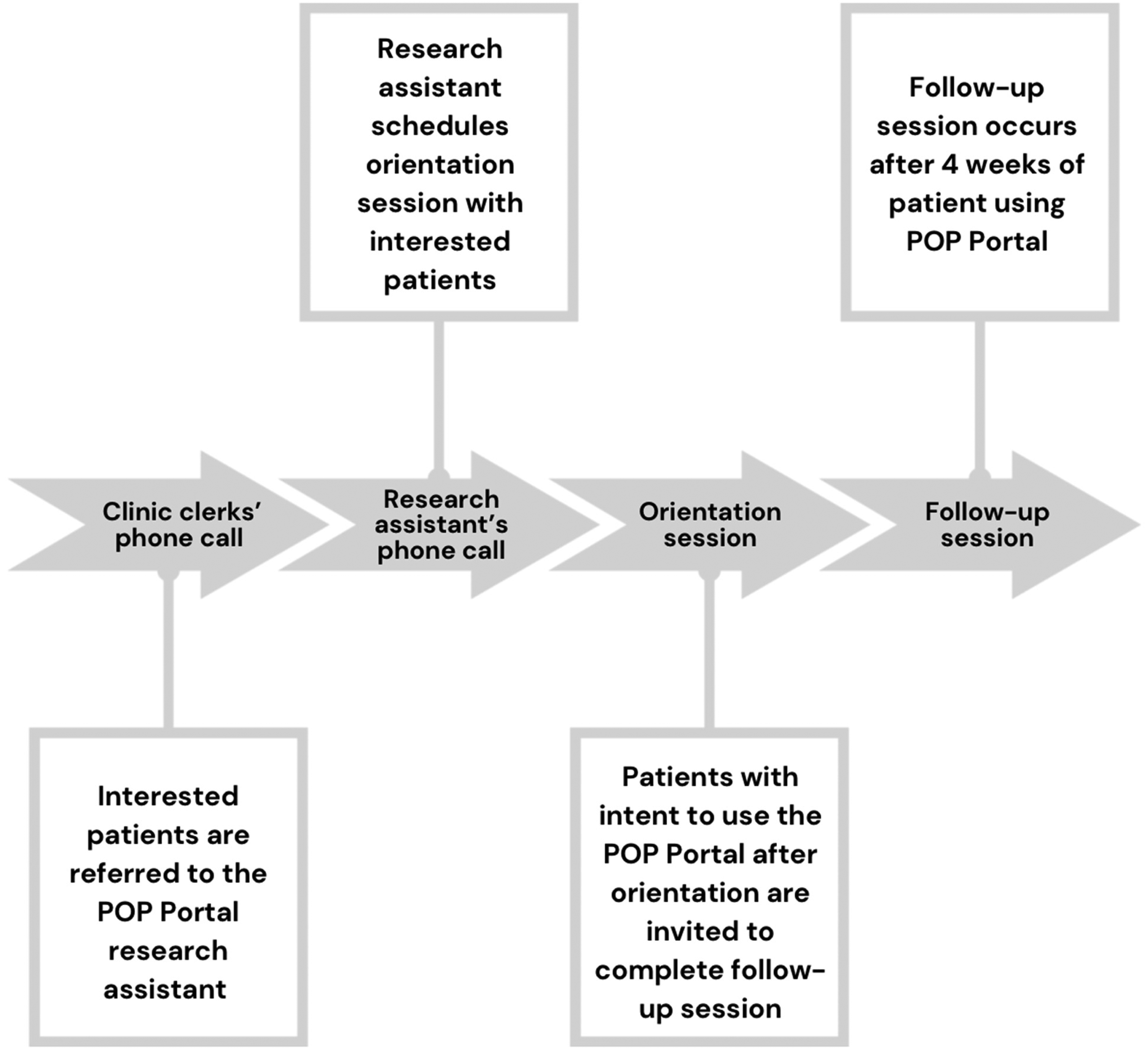
Summary of procedures.
Measures
Demographic information (e.g. age, sex, gender, date of referral to the pain clinic, and pain diagnosis) was collected from patient's medical records. Information pertaining to patient retention throughout the study was collected during the orientation session and at follow-up. This included: (1) interest in learning about POP; (2) completion of the orientation session; (3) intent to use POP (post-orientation); and (4) actual Portal use (at follow-up session).
Semistructured interviews were conducted with patients who agreed to take part in the follow-up session to evaluate the acceptability and usability of the Portal (refer to Appendix A for interview guide). The interview used a grounded theory approach, targeting patient experience, intent to use the POP Portal, and areas of which the POP Portal may be improved. 1:1 interviews were conducted by a male research assistant (AZ) using the videoconferencing software MS Teams and lasted up to 15 min. Field notes were taken by the research assistant to document patient responses to questions for later analysis. Research assistants within this study are trained in interviewing methods and are supervised by a registered psychologist (PP).
Analysis
Descriptive statistics were conducted using SPSS Statistics software to describe sample characteristics and patient retention throughout the study. Characteristics of patients who did or did not participate in an orientation session were evaluated using independent samples
Results
Sample characteristics
Descriptive statistics are presented in Table 1. A total of 60 patients were referred to the POP Portal research assistant by the clinic clerk. The majority of referred patients were female (
Sample characteristics.

Out of the 60 patients referred to the POP Portal research assistant, majority (

Flow diagram of patient retention.
Semistructured interviews
A summary of the qualitative findings is presented in Table 2. Saturation was reached after the completion of 40 interviews, whereby no new information was presented.
Summary of findings.

Accessibility of the portal
Users indicated that the POP Portal offers a variety of resources that were easily accessible. Many PLWP expressed their excitement and enthusiasm to have readily available resources at their fingertips: “
Several users suggested additional resources that are not presently available to be included on the Portal, including: 1) medication education resources; 2) time management courses; and 3) 1:1 consultation with a pain specialist: “
Usability of the portal
Patients offered suggestions to improve user experience, including additional features: “
One patient mentioned that some aspects of the Portal did not meet their standards of usability, including difficulty with visuals presented on the Portal. The patient noted difficulty reading text due to the size of the font.
A few users highlighted the limitation of the Portal technology requirements. One user said, “
Acceptability of the portal
Some patients indicated that the POP Portal was helpful. “
Others commented on the usefulness of the features available on the Portal. “
Some patients believed that the POP Portal was not suitable for their current needs. Some users reported time constraints as a barrier, while other users reported seeking medical interventions and 1:1 treatments that were not included on the POP Portal
Patient value of the POP portal
Some patients reported benefit to accessing the POP Portal while waiting for care at the clinic, and all recommended we continue to offer the POP Portal for those who are waiting: “
Others endorsed the POP Portal and encouraged others to avail of it, including PLWP, friends/family, and healthcare professionals: “
Some highlighted the uniqueness of the Portal, indicating the centrality of resources: “
Discussion
The present study explored the initial implementation of the POP Portal in the referral pathway at a tertiary pain clinic and evaluated the experiences of PLWP using the Portal while waiting for care, acting as the first evaluation of acceptability for the POP Portal. Findings suggest that some patients waiting for care at a tertiary pain clinic who were introduced to the POP Portal found it: 1) enhanced access to a variety of online resources in one a centralized location; 2) helpful in their journey to self-management; and 3) potentially beneficial for anyone who is waiting for pain care at a tertiary car pain clinic. Although the POP Portal was found to be helpful for most participants in this study, individuals who looked for primarily medical interventions and high-intensity services (i.e. 1:1 support from a physician or pain specialist) did not feel as though their needs were met when using the POP Portal. Suggestions were made to improve the POP Portal to be inclusive of differing pain diagnoses and increase user engagement with resource materials by addressing shortcomings in Portal usability.
One of the major impetuses behind the POP Portal is to address the unmet needs of patients referred to tertiary CP care clinics through a person-centric approach that provides a stepped-care continuum of resources for self-management of pain, mental health, and substance use health. From this initial implementation project, the POP Portal was reported by PLWP to satisfy their pain management needs in an accessible way while they waited for an appointment at TOH Pain Clinic. Additionally, the POP Portal is accessible internationally to any person living with pain. At end of March 2023, the POP Portal reached a total of 1852 users. More recently, as of June 2024, the POP Portal reached a total of 233,243 users across the world, of which 227,200 were Canadian users. The POP Portal increases access for clients by curating evidence-informed CP self-management resources in a single website. Platforms such as the POP Portal have shown acceptability and usability among patients. A meta-analysis and systematic review that included 67,884 patients across 65 studies indicated that the use of web-based programs (e.g. psychoeducation, support groups, CBT) reduces barriers of participation in care, allowing higher patient retention and satisfaction, and greater program usability when compared to in-person equivalents. 21 Another study reported that patients attending a physical self-regulation program at an orofacial pain clinic in-person were less likely to complete all three sessions than those who completed via telehealth. 22 This may suggest that digital resources, such as those seen on the POP Portal, offer convenient access to care by removing influential barriers. One difference that separates the POP Portal from other web-based programs is the diversity of resources available to the user. The POP Portal offers not only diverse resource types (i.e. articles, videos, webinars, workshops, peer support, etc.) but it also reaches beyond CP to provide resources touching on topics that are often a top-of-mind concern for PLWP, including sleep hygiene, medication, diagnosis, financial supports, indigenous supports, and mental health. Centralization of resources acts to reduce barriers PLWP may experience when seeking pain self-management, as all of the resources they may be interested in at that moment in time are readily available, free of charge, in one convenient location with no need to search website to website which can be time-consuming and frustrating for the user.
Further, some patients have indicated that the use of resources on the POP Portal, including sleepwell.ca and the self-directed course Empowered Management, have been helpful in reducing symptoms associated with pain (e.g. mood, self-efficacy). Internet-based pain management interventions, including iCBT and iACT, have been shown in many studies to improve pain intensity, pain catastrophizing, and symptoms of anxiety and depression.9,23–25 A randomized control trial comparing patient outcomes of iCBT to a waitlist control reported improvements to disability, depression, anxiety, and pain intensity greater than 30% in the treatment group and was sustained at three-month follow-up. 9 It may be beneficial within a broader context to introduce self-management resources, such as self-directed courses, as a complimentary step within an individual's CP management and preparing the individual for treatment in a tertiary care clinic. As many waitlisted patients may experience a deterioration in their condition as they wait for a first appointment, 26 access to such resources may be beneficial for maintaining their condition until they receive treatment from a healthcare professional.
People living with pain have endorsed the POP Portal as a platform which provides a variety of resources for pain management; however, some have indicated that the POP Portal does not provide resources addressing the needs associated with living with specific chronically painful conditions. Research conducted on digital pain management websites have indicated that the availability of a variety of resources is important for acceptability and engagement, specifically highlighting the need for diagnosis-specific resources. 27 While many CP self-management strategies are appropriate across several chronically painful conditions, CP is complex and some conditions leading to CP may benefit from more tailored approaches. 16 As such, the inclusion of diagnosis-specific resources on a digital platform such as the POP Portal may help to improve acceptability and engagement across a larger population and should be considered as the POP Portal continues to evolve.
Future directions
Our goal is to leverage the experiences of PWLP using the Portal during initial implementation to improve the POP Portal in an iterative manner to better suit the needs of PLWP. Results of the present study will be used to inform changes to the POP Portal, including additional resources and improved usability. We will also continue to work on the implementation of the POP Portal and study a range of patient, implementation, and health system outcomes. This will include the next step of this project, a hybrid implementation-effectiveness type III pilot study to evaluate the feasibility of conducting a future definitive trial. The trial will provide important information pertaining to the acceptability and usability of the POP Portal using validated measures, as well as exploration of the Portal's impact on patient outcomes after three months of use. Further, future research will explore the need for diagnosis-specific resources to inform future development of the POP Portal. We aim to integrate participant feedback into the POP Portal in an iterative process so that the Portal may continue to grow to fit the needs and preferences of PLWP. Additional research will explore the integration of the POP Portal into clinical practice, highlighting the barriers and facilitators of implementation, healthcare provider perceptions of the POP Portal, and factors which may impact long-term sustainability in clinical practice. We will also conduct research to determine the characteristics of users within each resource and further evaluate the acceptability and usability of the resources across age, diagnosis, sex, and gender. Finally, we will explore the implementation of the POP Portal within primary care settings, evaluating the benefits, barriers, and facilitators of implementation, as well as the development of a decision-support intervention to support sustainable integration of the POP Portal within primary care pathways.
Study limitations
The use of qualitative methods built on theoretical frameworks and with sufficient sample size for information power (
Conclusion
Overall, the present study conducted semistructured interviews with PLWP who have used the POP Portal while waiting for care at a tertiary care pain clinic. Present data illustrate most participants found the POP Portal helpful for their concerns and gaining an understanding of CP. The POP Portal also met their standards of accessibility, providing easy access to pain self-management when it is needed most, although improvements may be made to provide additional resources and meet usability needs.
Footnotes
Acknowledgements:
The authors would like to thank the Power Over Pain Scientific Advisory Committee for their feedback and suggestions for the improvement of this manuscript.
Availability of data and materials
Deidentified data will be made available to researchers upon request with a methodologically sound proposal. Data sharing may be enacted with a data-transfer agreement between the sending and receiving institutions. Proposals should be directed to the corresponding author.
Contributorship
Conceptualization: AK, AM, AR, AZ, EB, YS, PA, PP, JAR, RB, and RW; Methodology: AK, AZ, EB, PP, and YS; Data curation and analysis: AK, AZ, EB, and PP; Writing – original draft: AK, EB, PP, and YS; Writing – Reviewing and editing: AM, AR, AZ, JAR, PA, RB, and RW; Project administration: PP and YS. All authors provided important intellectual content, contributed to interpretation, and have reviewed and approved the final version of this manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
The Ottawa Health Science Network Research Ethics Board approved a research ethics board exemption for this study through a quality improvement stream.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article This study was funded by Health Canada's Substance Use and Addictions Program [Grant #: 2223-HQ-000044] and The Ottawa Hospital Academic Medical Organization Innovation Fund [Grant#: TOH 22-010]. The views expressed may not represent those of Health Canada.
Informed consent
Participants provided informed consent before participating in the associated study.
Guarantor
PP
