Abstract
Telemedicine refers to the process of utilizing communication technologies to exchange disease information, perform surgery and educate care providers remotely, breaking through the distance limit and promoting the health of individuals and communities. The fifth-generation (5G) technology and the COVID-19 pandemic have greatly boosted studies on the application of telemedicine in urology. In this study, we conduct a comprehensive overview of the knowledge structure and research hotspots of telemedicine in urology through bibliometrics. We searched publications related to telemedicine in urology from 2004 to 2024 on the Web of Science Core Collection (WoSCC) database. VOSviewer, CiteSpace and R package “bibliometrix” were employed in this bibliometric analysis. A total of 1,357 articles from 97 countries and 2,628 institutions were included. The number of annual publications on telemedicine in urology witnessed a steady increase in the last two decades. Duke University was the top research institution. Urology was the most popular journal, and Journal of Medical Internet Research was the most co-cited journal. Clarissa Diamantidis and Chad Ellimoottil published the most papers, and Boyd Viers was co-cited most frequently. Effectiveness evaluation of telemonitoring, cost–benefit analysis of teleconsultation and exploration of telesurgery are three main research hotspots. As the first bibliometric analysis of research on telemedicine in urology, this study reviews research progress and highlights frontiers and trending topics, offering valuable insights for future studies.
Introduction
In an era when the increasing cost of health care and the inequality of access to medical resources call for a more efficient care delivery model, one promising initiative has been telemedicine. Telemedicine refers to the process of utilizing telecommunications technologies to share medical knowledge, exchange disease information, and even perform operational practice, which breaks through the distance limit and advances the health of individuals and their communities. 1 Traditional telemedicine mainly encompasses three sub-categories: (1) telemonitoring, involving doctors monitoring the physiological index and physical symptoms of patients, as well as managing their health status; (2) telesurgery, allowing surgeons to perform operations by controlling surgical robot located at a distance from operating theater; 2 (3) telementoring, focusing on guidance and consultation between remote specialists and local doctors or students.
Firstly proposed by Thomas Bird in the 1970s, the concept of telemedicine received significant attention from the medical community. 3 In the United States, the success of the Space Technology Applied to Rural Papago Advanced Health Care (STARPHAC) project marked a breakthrough in telemedicine adoption and prompted its development in the following years. 4 Over the next two decades, with the advancement of communication technologies, the adoption of telemedicine across the globe grew exponentially. In 2001, Jacques Marescaux in New York performed the first remote laparoscopic cholecystectomy on a patient in Strasbourg, verifying the feasibility of telesurgery. 5 However, the lack of official regulations, the expensive cost and the limitation of network systems impeded the practice and popularization of telemedicine in the last two decades. Until recent years, with the integration of new technologies, such as the fifth-generation (5G) internet, 6 and in response to the coronavirus disease (COVID-19) pandemic, the modern development of telemedicine has greatly boosted. 7 More subsets of telemedicine were developed, such as teletherapy, telepharmacy and telepathology, and assessments on their implementation and outcomes were conducted.8–10
To date, telemedicine has been used in a wide array of medical fields, especially in urology due to three advantages. First, the diagnosis of urological diseases relies more on the assessment of imaging data. Differences in experience exert no obvious effect on the result of urological physical examinations, which compensates for the inability of experts in remote locations to conduct physical examinations in person. Second, the anatomical positions of urinary system organs are relatively fixed, making remote surgery less challenging compared to surgeries on organs with greater variability. Third and most critically, urology has led the way in the development of telerobotic surgery. 11 In 1995, Intuitive Surgical was founded and introduced the first da Vinci robotic surgical system to the market in 1999. 12 In 2001, the first cases of robot-assisted radical prostatectomy were performed in Europe. In 2005, Vattikuti Institute completed 2005 robotic prostatectomies, symbolizing the largest single experience of robotic surgery internationally, catapulting urology into the premier surgical robotic specialty. 13 Since then, robotic systems have been widely used in urology and are best versed in surgery of the kidney, prostate and bladder. 14
Bibliometrics is a systematic examination method that uses statistical, data mining and visualization techniques to quantitatively analyze scientific literature. It aimed at identifying patterns, trends and impact within a particular field.15,16 Specifically, the evaluation comprises information about authors, countries, journals, institutions, references and keywords. Compared to traditional systematic reviews, bibliometric analysis offers distinct advantages, such as providing a broad quantitative overview of research trends and impacts and enabling the identification of emerging fields and influential studies with greater efficiency.17,18 By applying bibliometrics to analyze the research progress of medical issues, valuable reference information can be provided to clinicians to guide clinical practice and improve treatment protocols. Additionally, this analytical approach contributes to facilitating academic exchanges, enhancing patient education levels and driving continuous development and innovation. 19 Bibliometric tools, such as CiteSpace, VOSviewer, and R package “bibliometrix,” are commonly utilized to visualize the results, 20 offering a dynamic and comprehensive view of research patterns and connections.
Existing research in the past two decades has drawn contradictory conclusions on the effect of telemedicine in urology. Technology advancement also altered the challenges and limitations of telemedicine over time. Furthermore, bibliometric research on telemedicine associated with urology remained empty. Therefore, this study performed a bibliometric analysis of existing publications, leveraging its advantages over traditional reviews to provide possible explanations for the inconsistent outcomes and serving as a reference study for future studies to validate the effect of telemedicine.
Methods
Data collection
We conducted a literature search using the Web of Science Core Collection (WoSCC) database (https://www.webofscience.com/wos/woscc/basic-search) on 17 July, 2024. The search terms consisted of two parts: the first part focused on telemedicine with terms, such as “telemedicine”, “telehealth” and “telecommunication”; the second part encompassed terms associated with urologic non-tumorous diseases and neoplastic diseases, including kidney cancer, bladder cancer and prostate cancer. The detailed search terms are listed in the Supplemental Material. Publication years were limited from 1 January, 2004 to 17 July, 2024. The type of documents was set to “article” and “review article.” Documentations in non-English were excluded. The detailed flowchart is provided in Figure 1.
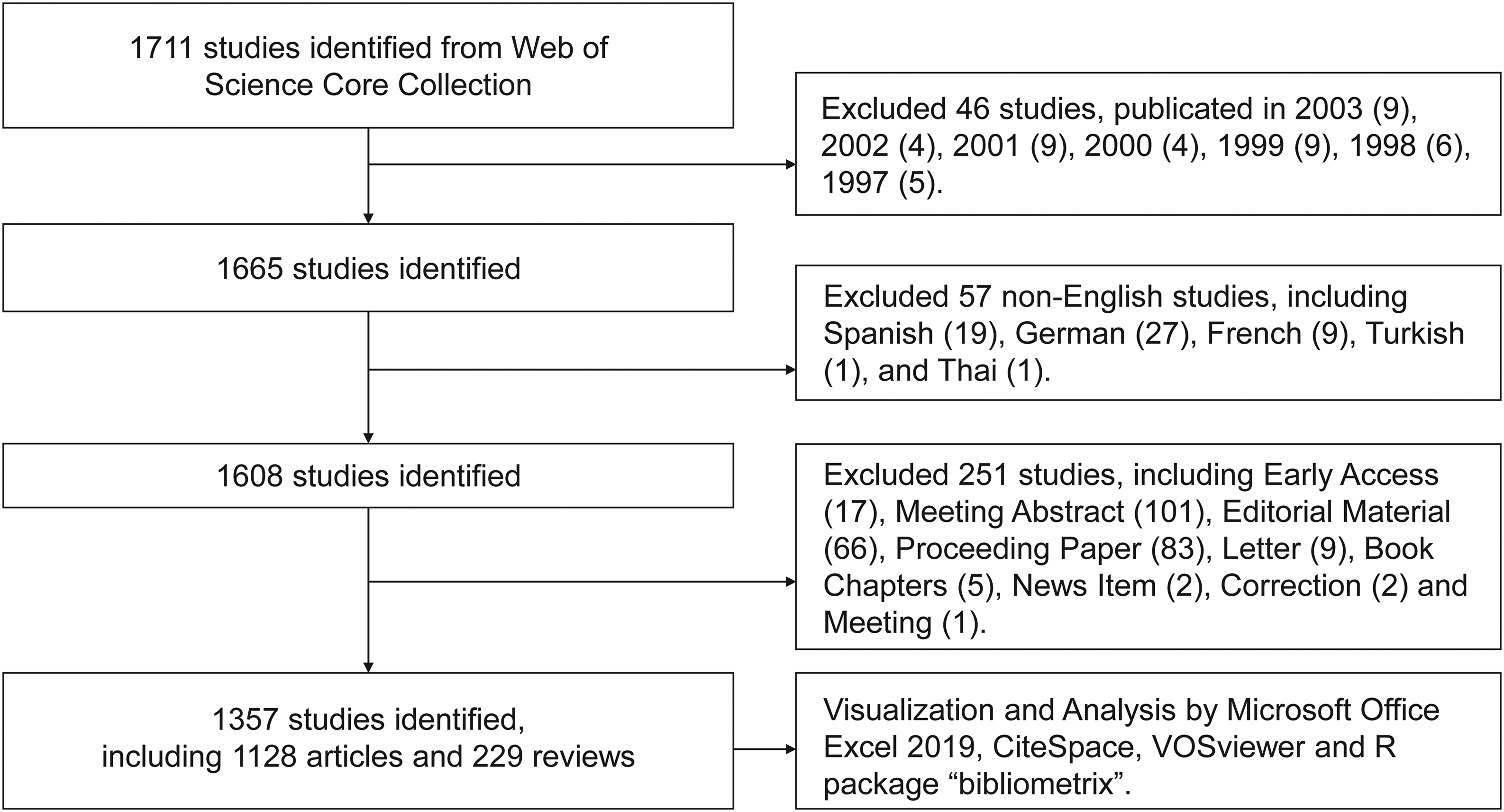
Publications screening flowchart.
Data analysis
Microsoft Office Excel 2019 was used to conduct data analysis and to visualize the annual number of publications. VOSviewer (version 1.6.20) can extract information from literature and explore relationships among relevant academic fields. 21 In our study, VOSviewer was utilized to investigate networks for country, institution, journal, author and keyword analysis. CiteSpace (version 6.2.R7) was used to construct a dual-map overlay of journals and to analyze references with citation bursts. The R package “bibliometrix” (version 4.0.0) (https://www.bibliometrix.org) was applied for a global distribution network of publications and trend topic analysis. 22 The quartile and impact factor of the journal were obtained from Journal Citation Reports 2023.
Results
Quantitative analysis of publications
The number of publications over a period can reflect the research speed and trend in a field. A total of 1,357 studies from 1 January, 2004 to 17 July, 2024 were included. The whole period can be divided into three periods shown in Figure 2. Few studies focused on telemedicine in urology in Period I with an average annual publication number of less than eight, representing that it has garnered a novel beginning. From 2011 to 2019, the number witnessed a gentle, but steady growth. In 2020, the number spiked almost twice, indicating a high interest in this field. In Period III, the number of publications has remained constant around 200 from 2020 to 2023, with 93 publications in the past 7 months in 2024, demonstrating a burgeoning attention on telemedicine in urology.

Annual number of publications on telemedicine in urology.
Countries and institutions
These publications originated from 97 countries and 2,628 institutions. The largest number of publications was from the United States, the United Kingdom and China, accounting for 44.4%, 10.8%, and 9.2% of the total counts, respectively (Table 1). The combined number of publications from the United States and the United Kingdom accounted for more than half of the total (55.2%). A connection network was visualized in Figure 3(A) based on literature from 46 countries, with a minimum number of five documents. The United States displayed a close relationship with most countries such as Germany, Canada, China and the United Kingdom. Notably, Ireland only collaborated with the United States. The average publication year of the United States, the United Kingdom, Germany and other European countries has fallen between 2019 and 2020, while many Asian countries, such as China, Malaysia, and India have not conducted concentrated studies until 2021 or even 2022.

The visualization of countries (a) and institutions (b) on research of telemedicine in urology.
Top 10 countries and institutions on research of telemedicine in urology.

The top 10 institutions are distributed in three countries, with six of them located in the United States. Duke University (
Journals and co-cited journals
Relevant publications were published in 556 journals. Urology (

The visualization of journals (a) and co-cited journals (b) on research of telemedicine in urology.
Top 15 journals and co-cited journals on research of telemedicine in urology.

The right part of Table 2 displayed the top 15 co-cited journals. Two journals were co-cited more than 800 times. Journal of Medical Internet Research (co-citation = 914) was the most co-cited journal, followed by American Journal of Kidney Disease (co-citation = 803) and Journal of Urology (co-citation = 785). The impact factor of Lancet was the highest (IF = 98.4), followed by New England Journal of Medicine (IF = 96.2) and JAMA-Journal of the American Medical Association (IF = 63.1). Journals with a minimum co-citation equal to 20 were filtered to map the co-citation network (Figure 4(B)). The size of the visualization circle is determined by the strength of the journal's connections with others. Diabetes Care had positive co-citation relationships with the abovementioned three high-IF journals as well as the largest link strength with other journals.
The dual-map overlay mapped out the intricate web of citation relationships between journals and co-cited journals, displaying citing journals on the left side and cited journals on the other side. In Figure 5, research in Health/Nursing/Medicine journals was frequently cited by Medicine/Medical/Clinical journals.
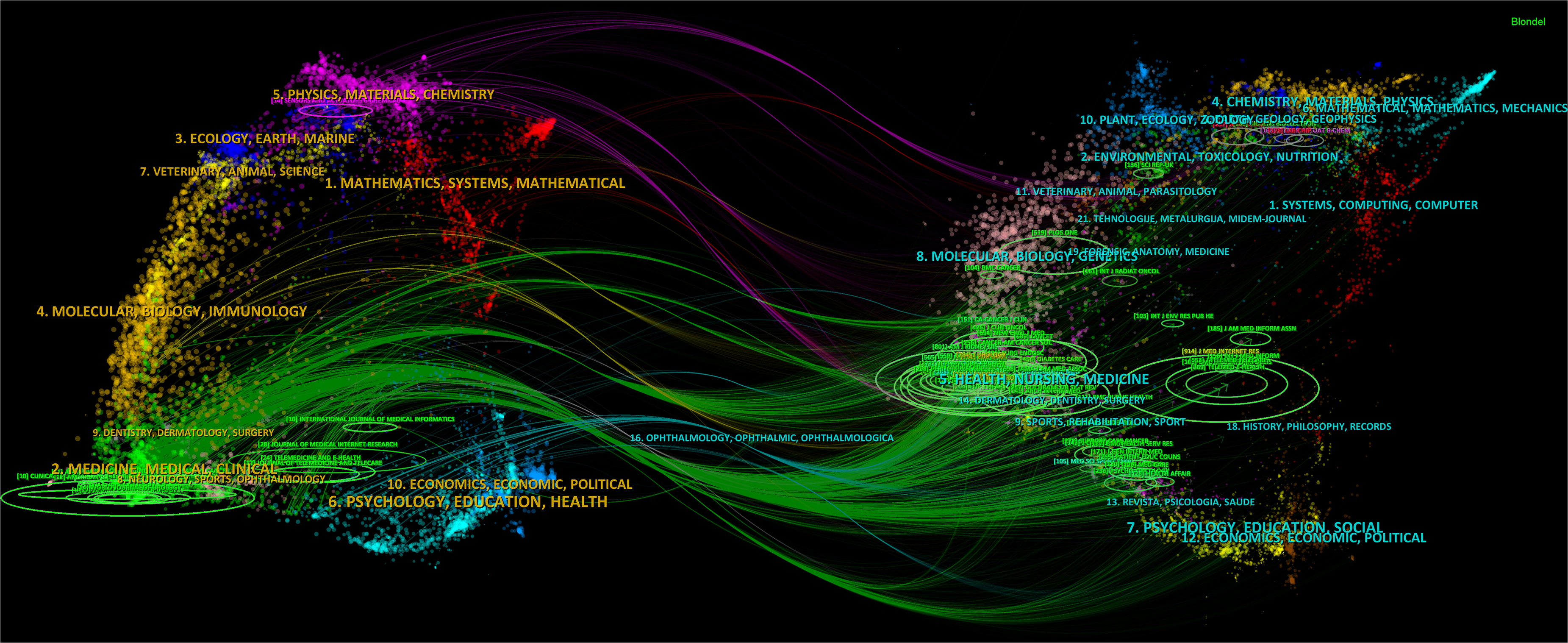
The dual-map overlay of journals on research of telemedicine in urology.
Authors and co-cited authors
More than 8,093 authors had participated in the research on telemedicine in urology. Both Clarissa Diamantidis and Chad Ellimoottil had published 11 papers, followed by Katrina Campbell and Jaimon Kelly with 10 papers per capita (Table 3). We built a collaborative network based on the minimum papers of five (Figure 6(A)). Strong collaborations among several groups were observed. For example, Katrina Campbell, Jaimon Kelly and Allison Tong had close cooperation with each other in the orange cluster.

The visualization of authors (a) and co-cited authors (b) on research of telemedicine in urology.
Top 10 authors and co-cited authors on research of telemedicine in urology.

Among the 33,043 co-cited authors, five authors were co-cited more than 65 times (Table 3). The most co-cited author was Boyd Viers (
Co-cited references
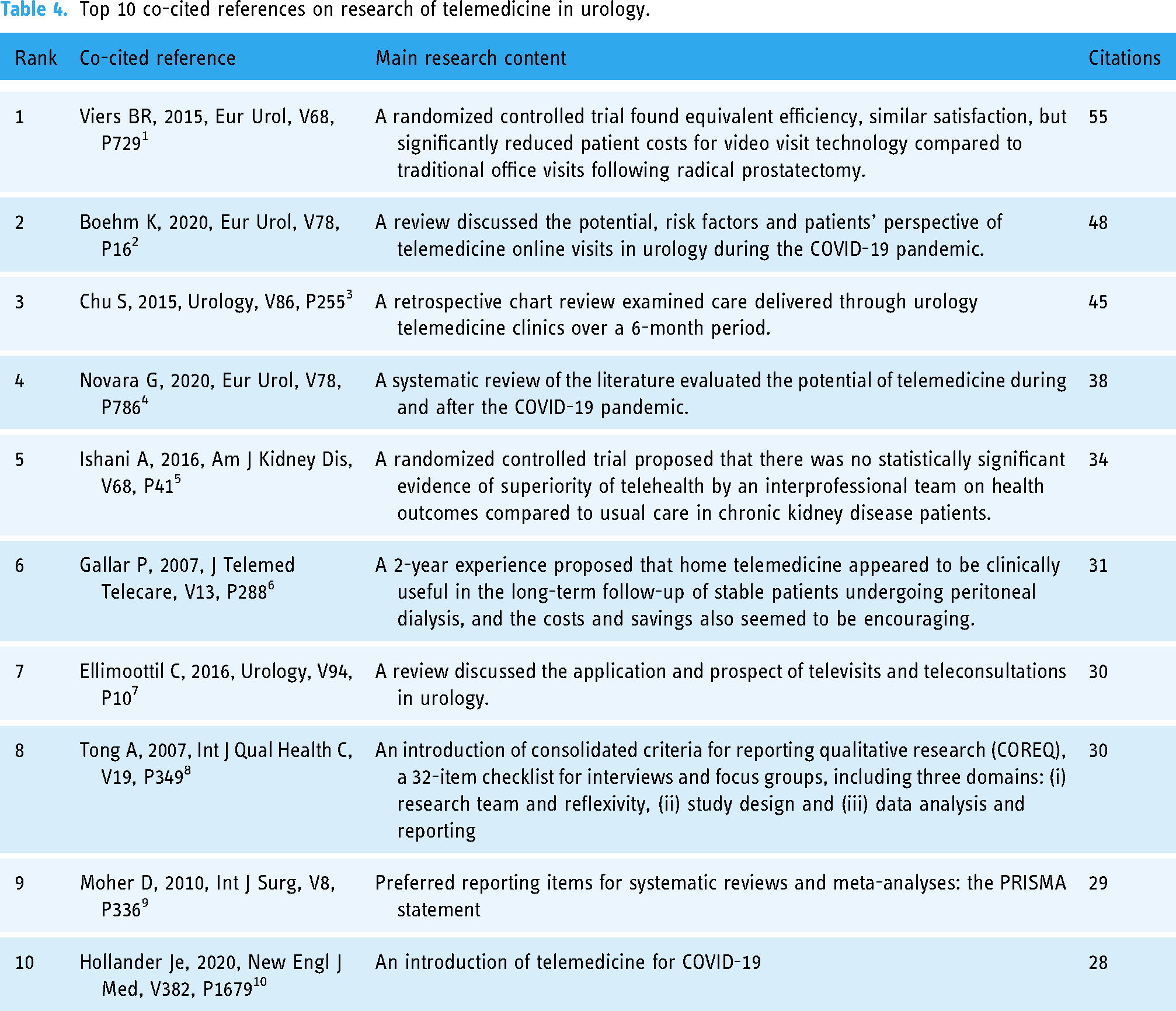
Co-cited references analysis indicates that two references are cited in the reference list of a third article. As depicted in Table 4, the top two co-cited references were both from European Urology, with citations of 55 and 48. We selected references with a minimum co-citation of 20 for constructing the co-citation network (Figure 7). “Viers Br, 2015, Eur Urol” showed active co-cited relationships with “Chu S, 2015, Urology,” and “Ellimoottil C, 2016, Urology,” etc., consistent with the bibliometric mapping relationship of the co-citation authors.

The visualization of co-cited references on research of telemedicine in urology.
Top 10 co-cited references on research of telemedicine in urology.
References with citation bursts
References with citation bursts refer to references that experience a surge in citations over a specified timeframe. A total of 25 references with strong citation bursts were identified by CiteSpace and sorted in chronological order of the beginning year of citation bursts (Figure 8). The burst strength ranged from 4.05 to 8.00, and endurance strength was from 2 to 4 years. The reference with the strongest citation burst (strength = 8.00) was titled “Telemedicine Online Visits in Urology During the COVID-19 Pandemic-Potential, Risk Factors, and Patients’ Perspective,” 23 authored by Katharina Boehm et al., with citation burst from 2017 to 2019. The reference with the second strongest citation burst (strength = 7.53) was titled “Health information technology (IT) to improve the care of patients with chronic kidney disease (CKD),” 24 authored by Clarissa Diamantidis et al., with citation burst from 2017 to 2019. Table 5 summarizes the main research contents of the 25 references.

Top 25 references with strong citation bursts. The red bar indicates high citations in that year.
Main research contents of the 25 references with strong citations bursts.

Hotspots and frontiers
As displayed in Table 6, we tended to divide author keywords into mainly two categories: disease-related keywords and telemedicine-related keywords. Keywords concerning kidney diseases, such as chronic kidney disease (occurrence = 135), dialysis (occurrence = 41), diabetic kidney disease (occurrence = 34), nephrology (occurrence = 21) and kidney transplantation (occurrence = 20), had received a relatively high total occurrence, followed by prostate cancer (occurrence = 121). Telemedicine-related keywords comprised e-health (occurrence = 108), m-health (occurrence = 99), telesurgery (occurrence = 20), etc. Other high-frequency keywords included COVID-19 (occurrence = 135) and randomized controlled study (occurrence = 25).
Top 30 keywords on research of telemedicine in urology.

We filtered the top 49 author keywords with a minimum occurrence number of 13 and performed cluster analysis (Figure 9(A)). We obtained five clusters in red, purple, blue, green and yellow, representing the main research directions.

Keyword cluster analysis (a) and trend topic analysis (b).
Trend topic analysis (Figure 9(B)) showed that in Period I (2004–2010), research probably focused on the initial attempt of virtual reality technology on urological surgery including nephrectomy and laparoscopic radical prostatectomy. From 2011 to 2019 (Period II), teleconsultation by online connection witnessed a high trend. Over the recent years (2020–2024), topics related to chronic disease management, including quality of life, chronic kidney disease and prevention had frequently appeared.
Discussion
General information
The number of publications exhibited an overall growth trend. From 2004 to 2010, research in this field was still in its infancy. As technological infrastructure evolves, studies on telemedicine in urology had a steady rise from 2011 to 2019. The number of publications in 2017 had a 50% growth from last year, which may be attributed to the rise of 5G technology in 2016, when Qualcomm announced the first 5G modem, while Huawei (China) and DOCOMO (Japan) declared the first large-scale trial of 5G network worldwide. Subsequently, two factors may account for the dramatic increase from 2019 to 2020. One is the utilization of 5G technology for commercial purposes, offering more reliable and faster connections and providing technological possibilities for the advancement of telemedicine. Its transmission capacity of up to 10 gigabits per second (Gbps) especially enables growth in high-quality remote training, offering patients the option of being treated remotely by experts. The other is the outbreak of the COVID-19 pandemic, leading to numerous precautions, including social isolation, quarantine policies and lockdown limitations. 25 In this case, telemedicine, which emphasizes on non-contact patient care, allows providing healthcare remotely and has emerged as an indispensable choice. As COVID-19 subsides, the interest of urologists seems to be shifting toward telesurgery, particularly fueled by the proliferation of surgical robots. Furthermore, reimbursement policies that include telemedicine services in insurance coverage and offer favorable reimbursement rates encourage patients and providers to adopt telemedicine. The development of clear guidelines and policies that balance innovation with patient welfare and fiscal responsibility is crucial for the sustainable growth of telemedicine in urology. In recent years, the number of publications remained high. Thus, it is predictable that the field of telemedicine in urology will continue to garner increasing interest.
Countries from North America, Europe and Asia almost accounted for the top 10 contributing countries to the research of telemedicine in urology. The United States took a dominant place based on not only the total publications (
Research on telemedicine in urology was mostly published in Urology, which made it the most influential specialty journal in this research field. Most journals performed well in Quartile in Category with three journals not included in the latest Journal Citation Reports. This phenomenon reflected an uneven situation of telemedicine in urology, as well as a broad developing space requiring more high-quality research. Notably, the term “kidney disease” frequently appeared in the bibliometric map of journals with red and yellow clusters (Figure 4(A)), which supported a wide application of telemedicine in kidney diseases. 32 Besides, the journal cluster in light blue reflected the need to develop applications for telemedicine in urology, and the dark blue cluster represented the combination of internet and clinical management, both of which were important underlying infrastructure in this research field. The large number of publications in Physics/Materials/Chemistry shown in Figure 5 proved the point. Additionally, the terms “diabetes” and “hypertension” obviously appeared in the map of co-cited journals (Figure 4(B)), which may attributed to the strong relationship between diabetes/hypertension and secondary kidney disease, indicating the focus of telemedicine on the application of mobile health intervention in diabetic kidney disease (DKD) and chronic kidney disease (CKD). 33
Both Clarissa Diamantidis and Chad Ellimoottil published 11 papers, mainly focusing on the management effectiveness of telehealth in DKD and the economic benefits of telemedicine in urologic consultation services, respectively. The Slow Progression of Diabetic Kidney Disease (STOP-DKD) study, an RCT, was conducted to evaluate the effectiveness of remote medication management in several DKD patients and several dimensions, including glomerular filtration rate (GFR) decrease, blood pressure fluctuations, blood glucose monitoring and urinary albumin excretion record.34–38 All the results concluded a remarkable effectiveness of telemonitoring in DKD management. Chad Ellimoottil conducted several retrospective studies, indicating that remote video consultations and follow-ups have reduced the costs for patients and are feasible in urology,39–46 supporting the promotion of telementoring in urology outpatient services. Katrina Campbell and Jaimon Kelly jointly published 10 papers, admiring the utilization of a reliable telehealth-delivered dietary coaching program for CKD management. Based on two cross-sectional studies,47,48 two pilot randomized controlled trials, named ENTICE-CKD trial,49,50 one focus group study, 51 one qualitative interview study, 52 one mixed-methods process evaluation 53 and one review, 54 they recommended CKD patients to accept telehealth coaching as a way of self-management.
As for author co-citation analysis, Boyd Viers was the most frequently cited author, who specialized in radical prostatectomies.55,56 In 2015, Boyd Viers et al. published a prospective randomized controlled study and proposed that video visits were associated with equivalent efficiency, similar satisfaction and significantly lower patient costs when compared to office visits,57,58 which was also the most co-cited reference shown in Table 4. Intriguingly, as a global official organization, the World Health Organization ranked second in the co-citation author list. It provided several guidance for telemedicine in urology,59,60 laying a solid foundation for future collaboration across countries and institutions.
Knowledge base
Ten co-cited references were selected based on the number of co-citations, which revealed the foundational work of the development of telemedicine in urology. Among them, three references23,61,62 focused on the positive relationship between the occurrence of the COVID-19 pandemic and the development of telemedicine in urology, which accounted for the explosive increase of related publications in 2020. They all affirmed the successful implementation of telemedicine during the COVID-19 pandemic and at the same time emphasized more studies were needed to guarantee a safe and satisfactory outcome. The references ranked 1, 2 and 6 have affirmed the effectiveness of video consultations, remote nursing and remote dialysis management, respectively.23,58,63 However, the fifth reference by Ishani A et al., a randomized trial, suggested that compared to usual care for CKD patients, interprofessional telemedicine teams did not demonstrate statistically significant advantages in terms of health outcomes. 64
Evaluation on included publications
A cursory screening was taken on 1,357 publications consisting of 919 articles and 197 reviews, with the compliance of each with scientific norms confirmed. Twelve journals among the top 15 journals on telemedicine in urology were categorized in Q1 and Q2, with the high quality of the top 15 co-citation journals showing a qualified research environment. Additionally, the eighth and ninth co-cited articles introduced the consolidated criteria for reporting qualitative research (COREQ) and the PRISMA standards, respectively. The term “randomized controlled trial” ranked 19th in the top 30 author keywords. Both results demonstrate that the primary research studies on telemedicine in urology followed strict guidelines, which to a certain extent, validates the reliability of articles within this field. However, several studies focusing on the evaluation of patient satisfaction and cost benefits were constructed based on questionnaires, which were inevitable for subjective bias.
Hotspots and frontiers
According to the citation burst period (Figure 8) and the main research contents of references (Table 5), the early citation burst was driven by two references related to telesurgery and surgical procedures.5,65 Ten references referred to the COVID-19 pandemic.23,66–74 Although the concept of teleconsultation was proposed in 2015, 58 the outbreak of the COVID-19 pandemic motivated substantial interest in the integration of telehealth into routine urological practice, leading to more recommendations and review articles. The remaining references24,58,64,75–84 focused on experiences or experiments that evaluated the application of telemedicine, particularly in the management of CKD patients.
As the keyword occurrence analysis shown in Table 6 implies, the application of telemedicine in urology focused mainly on kidney disease, followed by prostate cancer, both of which are considered heavy health burdens among urological disorders. According to the author keyword cluster analysis (Figure 9(A)), we obtained five clusters in red, purple, blue, green and yellow, representing the main research directions: the surge in telemedicine within urology driven by the COVID-19 pandemic, the application of telemedicine in dialysis, the importance of mobile application and technology for telemedicine development, the focus on urological care of telemedicine and the effectiveness evaluation of telemedicine on managing kidney diseases. The term “randomized controlled trial” displayed high frequency in 2019, suggesting high-quality investigation on the clinical effect of telemedicine. Besides, the occurrence of the term “virtual reality” spanned from 2004 to 2021, providing a potential and persistent development direction for telemedicine in urology. To sum up, we listed three hotspots for medical professionals as follows.
Effectiveness evaluation of telemonitoring in non-tumorous disease management
Conventional telemonitoring narrowly refers to patients sending testing results or images to doctors on their phones. In contrast, novel telemonitoring emphasizes using apps and machine learning models to collect dynamic data and monitor health status in real time. The data can then be transmitted to patients themselves, family members and caregivers via communication tools for timely intervention, which is of great benefit in addressing disparities for individuals living in remote locations, as well as those facing mobility constraints. Overall, this method goes beyond patient–doctor communication and empowers patients, families, as well as communities to actively participate in healthcare management themselves, 85 revolutionizing the application scenarios of telemonitoring.
Telemonitoring has emerged as a hotspot in the management of chronic and secondary kidney diseases, such as DKD and hypertensive nephropathy.61,64,86 It tracks vital signs, medication adherence and symptoms, allowing for personalized and timely intervention. However, some studies proposed less ideal results with the advancement of clinical evaluation. For example, a clinical trial in 2024 87 found a non-significant promotion between the mobile phone-based intervention and no-monitor observation for physical activity in CKD patients. Developing prospective studies is the trend to investigate the effect of telemonitoring on treatment outcomes, cost-effectiveness and patient engagement. 88 Additionally, telemonitoring is tested and promoted in more non-tumorous diseases, such as male-specific health issues and urinary control disorders. The present results underscored its versatility and potential to address a broad range of non-tumorous conditions.41,42 We anticipate the popularization and effectiveness of telemonitoring in urological diseases.
Cost–benefit analysis of teleconsultation after the COVID-19 pandemic
Beyond all doubts, the key driving force behind the proliferation of telemedicine lies in the COVID-19 pandemic, which greatly altered the way patients acquire medical help. Teleconsultation method has evolved from telephone calls to video conferencing and QR codes. To reduce the risk of COVID-19, a German urological office has built a system that allows patients to have video appointments with doctors in 2020. 89 So far, this concept of “virtual urologist” has confirmed its worth throughout the patient and doctor community.
As the world adapts to the new normal post-COVID-19, teleconsultation has become a frontier for providing continued healthcare. Despite potential drawbacks and limitations, studies have shown that teleconsultation has the potential to maintain equivalent efficiency while promising to reduce healthcare costs.57,58,89 While cost–benefit analyses remain relatively scarce, 77 we anticipate more comprehensive evaluation studies on a larger scale. This endeavor necessitates collaborative efforts from hospitals, insurance companies and society. Additionally, given that costs are intricately linked to the software utilized, technology companies must also contribute. The ultimate goal is to ensure that the expenses incurred online are lower than the combined costs of travel and time.
Exploration of telesurgery technologies
Table 5 shows that the first two citation burst references were related to robot-assisted laparoscopic prostatectomy, which was the foundation of telesurgery. Actually, the term “telesurgery” performed mediocre in this bibliometric analysis with a rank of 28 in the top 30 author keywords (Table 6) and a 6-year research trend from 2008 to 2014 (Figure 9(B)). However, we supported that telesurgery represents a frontier in medical technology that promises to revolutionize surgical practice after comprehensive consideration of the development of network technique and the application of robotic-assisted surgical systems in urologic surgeries especially in prostate cancer. Despite the current limitations posed by high costs and technological barriers, the potential benefits of telesurgery are immense, which requires significant upfront investment from governments, as well as innovative exploration of pioneer efforts. The ability to perform complex surgeries remotely can bridge the gap between regions with abundant surgical expertise and those lacking sufficient resources. Further research and development of surgical robots, particularly in terms of precision, dexterity and adaptability, are essential for realizing the full potential of telesurgery.
During a procedure with the robotic-assisted surgical system, the surgeon's hand movements are translated into precise movements of the robotic instruments. To date, the most used robotic procedures in urology are prostatectomy, partial and radical nephrectomy, ureteroplasty, cystectomy and retroperitoneal lymph node dissection (RPLND). 90 Among them, prostatectomy for localized prostate cancer attracted the most attention mainly because of its high heterogeneity and serious implications on life quality. Thus, it also acted as a pioneer in the study of urological telesurgery.
Table 7 provided a summarization of the robotic-assisted surgical systems used in telesurgery in humans. The earliest clinical practice was in 2001 when Bauer et al. described a percutaneous renal surgery, in which the surgeon was located in Baltimore, while the patient was more than 7,000 km away in Rome using a plain old telephone system (POTS) line. 91 In the same year, the first trans-Atlantic robotic-assisted laparoscopic cholecystectomy, also known as the “Lindberg Operation”, 92 symbolized the opening of modern telesurgery studies. Numerous remote surgical systems were invented over the years.93–96 From 2019, several studies on robot systems using 5G networks were carried out,97–100 marking a revolution in telesurgery. The wide application of 5G networks in the clinical area and the development of 5G+ networks in recent years remarkably shortened the time delay, resulting in more precision. The above successful surgeries further verified the feasibility and safety of telesurgery, also emphasizing the benefit of minimal injury and long-distance convenience compared to open surgery and traditional robot surgery. For future studies, interdisciplinary cooperation combining technological improvement and surgical innovation foresees a promising future.
Brief summarization of clinical practice of robotically assisted surgical systems used in telesurgery in humans.
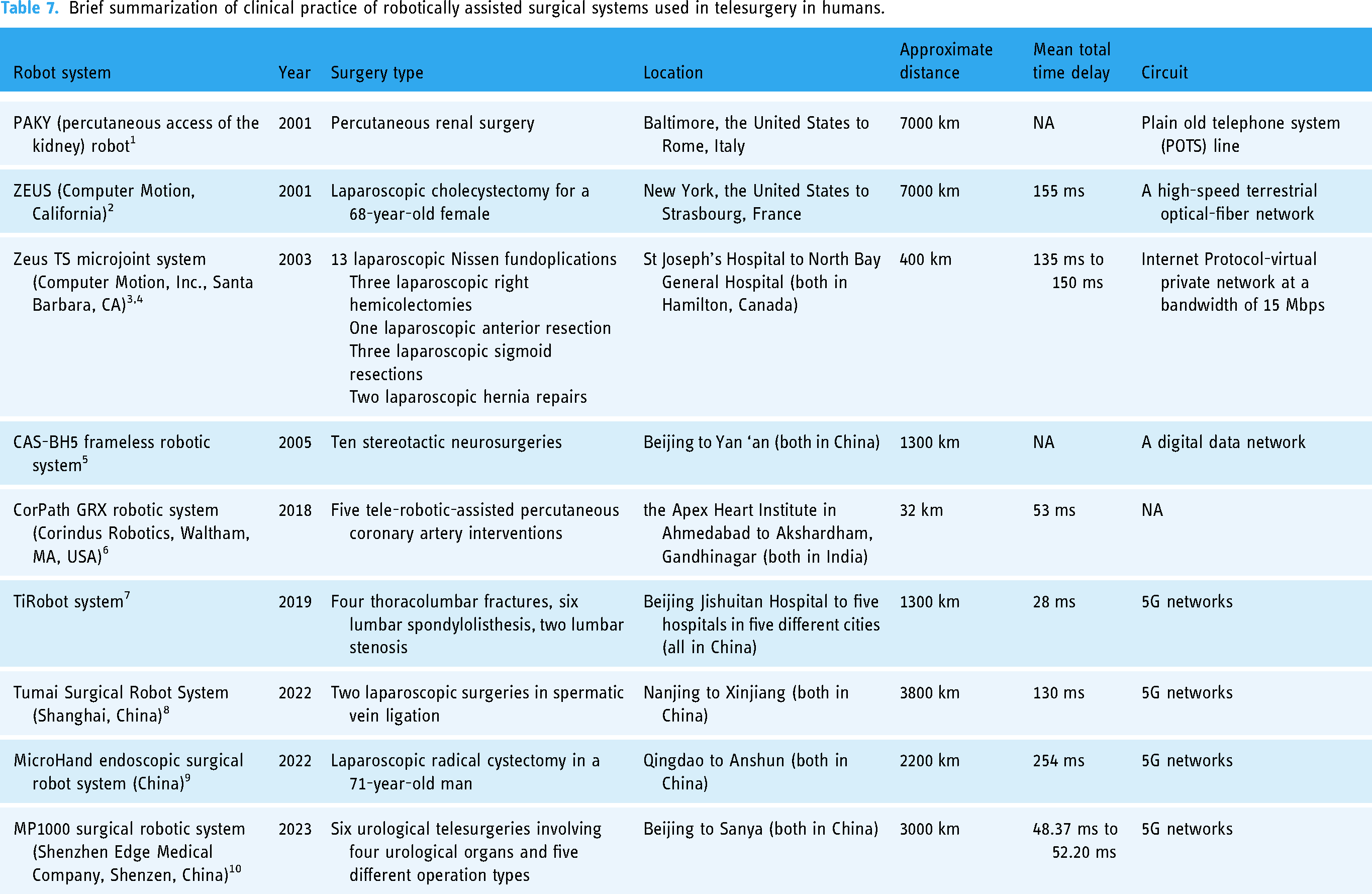
Notably, although the da Vinci surgical system is widely used in many routine surgical procedures, it is not put into practice for telesurgery in humans, but only conducted experiments in porcine models.101,102 Thus, we look forward to the clinical application of telesurgery on humans in the future.
Future study direction
To address the gaps and limitations in the current evidence base regarding telemedicine in urology, future research should focus on more detailed and actionable aspects. For example, studies could explore the effectiveness of specific telemedicine interventions in managing post-operative care for urological patients, comparing outcomes with traditional in-person care. Highlighting priority research areas, such as investigating access to telehealth care, patient satisfaction, treatment adherence and clinical outcomes, can enhance the clinical integration and real-world impact of telemedicine in urology. Intriguingly, with the current rapid development of artificial intelligence (AI), utilizing AI for personalizing telemonitoring to remarkably reduce doctors’ involvement and improve productivity is considered to be a potential topic for future research.
Meanwhile, methodological improvements are essential to strengthen the quality of future research. Existing evidence for the use of telehealth interventions in urological diseases is of low quality due to methodological limitations and heterogeneity of intervention types. Researchers could consider employing more rigorous study designs, such as randomized controlled trials, to assess the efficacy of telemedicine interventions. Furthermore, building up a specialized data set to gain meaningful assessment and selecting appropriate outcome measures can provide valuable insights into the effectiveness of telemedicine in improving patient outcomes.
Additionally, previous papers have comprehensively discussed the intricacies of telemedicine on reimbursement rates definition, patients’ privacy protection and accessibility and affordability insurance of telemedicine approaches.62,77,86,103 The lower quality of patient–clinician relationships and overtreatment due to false judgment and unclarified laws related to the responsibility of telemedicine also threaten the spread of telemedicine. Therefore, corresponding laws and regulations regarding information safety and legal responsibility should be enacted as soon as possible, and relevant paradigms and protocols should be strengthened.
By incorporating these suggestions into future research endeavors, we can advance the understanding and implementation of telemedicine in urology, ultimately improving patient care and outcomes in this specialized medical field.
Limitations
Inevitably, there are some limitations in this study. First, to ensure high-quality bibliometric analysis, the data are only from the WoSCC database. Relevant data from other databases have been ignored. Second, we only included studies published in English, meaning that some linguistic bias has been introduced. Finally, due to the restriction of the data analysis software, some data may not receive enough attention. For example, in the author co-citation analysis, VOSviewer included only the first author of a cited document, which may omit some valuable authors.
Conclusion
The research of telemedicine in urology has been significantly boosted during the COVID-19 pandemic and continued unabated up to now due to its easier medical care access, better patient convenience and greater potential for healthcare cost reduction. Current research hotspots mainly focus on the three dimensions: (i) effectiveness evaluation of telemonitoring, (ii) cost–benefit analysis of teleconsultation and (iii) exploration of telesurgery. Looking forward to an active settlement on barriers, such as patient acceptance, ethical considerations, legal challenges and financial issues compared with the traditional healthcare systems, we recommend more high-quality clinical trials related to telemedicine in urology and support its great potential.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076241287460 - Supplemental material for Knowledge mapping of telemedicine in urology in the past 20 years: A bibliometric analysis (2004–2024)
Supplemental material, sj-docx-1-dhj-10.1177_20552076241287460 for Knowledge mapping of telemedicine in urology in the past 20 years: A bibliometric analysis (2004–2024) by Na Zeng, Mei-Cheng Liu, Xing-Yu Zhong, Shao-Gang Wang and Qi-Dong Xia in DIGITAL HEALTH
Footnotes
Contributorship
Na Zeng and Mei-Cheng Liu analyzed the data, wrote the manuscript and drew the figures. Qi-Dong Xia and Shao-Gang Wang designed the study. Xing-Yu Zhong contributed to the critical revision of the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
