Abstract
Introduction
An estimated one billion people globally are currently suffering from hypertension. Prevention and management of hypertension are suboptimal especially in low- and middle-income countries leading to increased complications and deaths. With increased mobile phone coverage globally, this study aims to review mobile health technologies used for the prevention and management of hypertension.
Methods
We conducted a literature search on electronic databases using identified keywords involving “hypertension”, “mobile health technology” and their synonyms. Snowballing technique was also used. Papers were screened at two levels by independent reviewers. The targets were studies published in peer-reviewed journals reporting mobile health interventions for hypertension prevention and management. Only primary research studies published in English from January 2017 to April 2024 were included. Google Forms were used to extract the data along with other characteristics, and selected articles were categorised into: mobile application, web-based solutions, and Short Message Service (SMS) and other offline solutions.
Result
The search yielded 184 articles, and 44 studies were included in the review. Most (n = 26) were randomised control trials. Twenty-two studies (22) focused only on mobile applications solutions, 12 on SMS and other offline mHealth, 5 web-based solutions, and 5 combined more than one type of mobile health technology. The United States of America had the majority of studies (n = 17), with 6 studies from other American countries, 11 from Asia and nine from Europe, while only one from Africa. A total of 36 studies reported that mobile health technology significantly improved hypertension care through reduced blood pressure, improved adherence to follow-up visits and medications, and lifestyle changes. SMS and offline mHealth strategies have also demonstrated effectiveness in promoting self-management and reducing racial disparities in hypertension care.
Conclusion
Mobile health technology has the potential to play a significant role in the prevention and management of hypertension. However, there is a need for mobile health solutions for hypertension prevention and management in African countries and other developing countries. Integrating mHealth into primary healthcare delivery would also go a long way in strengthening patient care and reducing the burden on healthcare systems.
Introduction
It is estimated that approximately one billion people worldwide suffer from hypertension. 1 Approximately 80% of these problems are seen in low- and middle-income countries. 2 It is predicted that by 2025, one in every three people will be suffering from hypertension. 3 Complications of uncontrolled hypertension include chronic kidney disease, cerebrovascular accident, cardiomyopathy, and heart failure. These complications are, however, preventable through adequate management. This is cost effective and improves outcome. Expensive interventions, such as cardiac bypass surgery and dialysis, may be required when hypertension is poorly managed. Although antihypertensive drugs are effective and lifestyle adjustments have a positive impact on blood pressure, hypertension control rates are still far from ideal. 4 One of the best ways to manage hypertension is by self-management, which encourages people with the condition to take more responsibility for their own health. 5
Researchers and healthcare professionals have been inspired to explore the various features and applications of technology since its emergence in the healthcare system in order to enhance illness management and prevention. Following these efforts, mobile health technology (mHealth) has been noted to have the potential to facilitate and optimise patients’ self-management. 6 Previously, mobile health interventions focused on voice or text-based short messaging services (SMS), but the growing accessibility and usability of smartphone applications have enabled a considerable increase in the number of mobile applications that can be used to modify health behaviour. 7 The proliferation of mobile health (mHealth) care devices and software has greatly expanded self-care capabilities across the health care spectrum. 1 The increase in smartphone devices over the past few decades has been rapid. 8 This sharp rise in smartphone usage is mirrored by a surge in mobile applications that provide health services and information.9,10
This study aims to review mobile health technologies used for the prevention and management of hypertension.
Methodology
We carried out a scoping review to map relevant literature in the field of mHealth and its utilisation in the care of hypertension. This study design was favoured as Munn et al. 11 highlighted scoping reviews as the more useful approach for reviewing evidence rapidly in novel or emerging topics, under which mHealth falls, as well as identification and analysis of knowledge gaps to inform future questions about the field. The review was done following the five-stage framework developed by Arksey and O'Malley, 12 which consists of the stages outlined below:
Identification of the research question
We were interested in assessing mobile health technologies in the prevention and management of hypertension.
Identification of relevant studies
We conducted a literature search on electronic databases including MEDLINE, PubMed, PubMed Central, Google Scholar, and Scopus using a combination of keywords involving “hypertension”, “mobile health technology” and their synonyms identified from previous studies. The search strings are shown below in Table 1. Snowballing technique was also used by screening the bibliographies of identified papers for other relevant studies. Only articles published in peer-reviewed scientific journals were considered for review.
Search strategy.

Study selection
The title and abstracts of the search results were screened by two independent reviewers. Conflicts were resolved through team consensus. Inclusion criteria included: (1) papers published in peer-reviewed journals reporting mobile health interventions for hypertension prevention and management, (2) papers published in English language, (3) publications from January 2017 to August 2022 (time of search conduction), (4) only primary research studies. The exclusion criteria were: (1) papers published in other languages, (2) papers focusing on other non-communicable diseases, including pregnancy-induced hypertensive disorders, (3) papers published before January 2017 or after August 2022, (4) all types of reviews. The time window was chosen in order to avoid outdated data, likely to be of less relevance or obsolete in a rapidly evolving field like mHealth, thus improving the accuracy of results.
The full manuscripts of the selected papers were screened for data extraction by eight reviewers and final decision for inclusion. The papers were shared among the eight reviewers divided into four pairs, with members of each pair working together to screen assigned manuscripts. Conflicts between them were resolved by an independent ninth reviewer who oversaw the whole process.
A recent search was further carried out by two reviewers using similar keywords to seek out more recent studies between time of original search (August 2022) and time of final submission (April 2024). Obtained studies were screened in full by the two reviewers, with conflicts being resolved by a third reviewer.
Quality assessment
The quality assessment was done using the CASP Critical Appraisal Tools.13–15 This is due to the fact that it has checklists for different study designs. Data was extracted by three reviewers using Google Sheet (Supplemental material).
Data charting
The data was extracted using online Google Forms and included variables such as year of publication, country of study, study design, type of mobile health technology, aim of study, key findings, significance of mHealth, study limitations and final decision on inclusion. The data extracted was subsequently exported into an excel sheet for cleaning, sorting and synthesising.
Collating, summarising and reporting the findings
The data was categorised based on the mobile health technology used, that is, (1) SMS and other offline solutions, (2) mobile application solutions, and (3) web-based solutions. Other characteristics were also analysed, allowing us to clearly explore the different mHealth approaches, as well as to identify possible gaps. Figure 1 illustrates the process of identifying relevant papers for inclusion in data extraction and final synthesis.

Flow diagram illustrating the article selection process.
Results
A total of 44 studies were included in this review (Table 2). The selected studies were grouped into three categories based on the type of the mobile health technology. A total of 22 studies4,16–36 focused on only mobile applications solutions, 1237–48 on SMS and other offline mHealth, five49–53 web-based solutions only, and five54–58 combined more than one type of mobile health technology.
Review of digital health intervention for hypertension management.
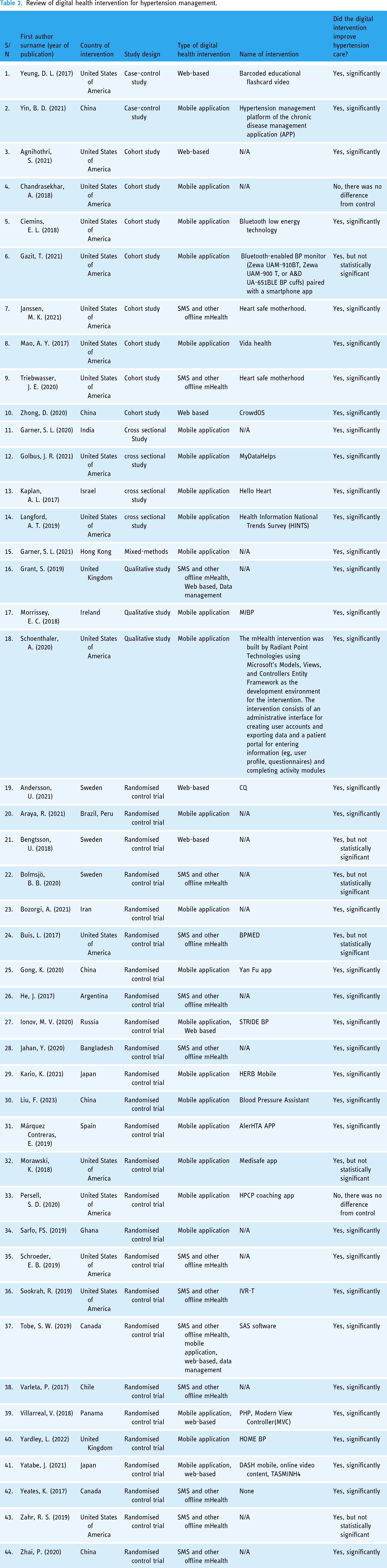
Most (n = 26) of the selected studies4,20–26,28,29,37,38,40–47,49,53,54,56–58 were randomised control trials. Other study designs found were cohort studies (n = 8),30–33,39,48,51,52 qualitative studies (n = 3),18,19,55 and other observational studies (n = 7).16,17,27,34–36,50
Most of the studies19,20,23,30–34,36,39,41,42,44,47,48,50,52 were conducted in the United States of America (n = 17). There were six studies21,38,45,46,54,57 from other American countries, 114,16,22,25,27,29,35,37,40,51,56 from Asia, and nine17,18,24,26,43,49,53,55,58 from Europe. Only one study 28 was conducted in Africa.
A total of 36 studies4,16–19,21,22,24–31,34–40,42,45–48,50–58 reported that mobile health technology improved hypertension care significantly, while the remaining (n = 8)20,23,32,33,41,43,44,49 showed no statistically significant improvements. All studies (n = 5)54–58 that combined more than one type of digital technology significantly improved hypertension care. Improvement of hypertension care included reduced blood pressure (systolic or diastolic), improved adherence to follow-up visits, increased literacy, lifestyle changes and other prevention and management measures of hypertension in adults, Table 2.
Discussion
Interventions using Mobile application technology
Mobile applications (apps) and other mobile health (mHealth) interventions have been promoted as promising strategies to aid in the self-management of hypertension and other chronic conditions. 24 By offering reminders for taking medication and ordering refills, monitoring biometric findings, providing information, and facilitating social interactions that offer support and encouragement, these systems support long-term management of these conditions. Of the papers reviewed in this study that focused on mobile application technology as a digital health intervention and fulfilled the inclusion criteria (n = 26),4,16–36,54,56–58 only four20,23,32,33 reported no statistical improvement in hypertension care. Studies that showed improvement included 12 randomised control trials,4,21,22,24–26,28,29,54,56–58 thus offering high enough level of evidence on the benefits of this form of intervention.
Following the COVID-19 pandemic which highlighted the shortcomings of conventional medical care and the need for telemedicine, 59 new chances to care for patients with cardiac problems remotely have been made possible by mobile phones, especially smartphones. In the past, telemedicine called for giving patients specialised monitoring equipment to use at home. However, mobile apps and wearable technology offer enormous potential for monitoring health through calls, texts, data recording, highly portable peripheral devices, and activity monitoring, which may find utility for novel models of healthcare delivery that are affordable, accessible, and patient-centred. 52
This can be accomplished by integrating healthcare into daily life through the delivery and collection of health information and services in a convenient, accessible, and interactive manner. 60 The use of a physician-supervised mobile health app was strongly linked to better health outcomes (reduced BP). For individuals with high levels of severity, the improvement was notable. 52 As a result, using an mHealth app can help a healthcare system be proactive (especially with regard to a silent killer like hypertension) and vastly enhance the quality of care. 61
A wide variety of applications were utilised in the reviewed studies with novel apps like MIBP employing user-centred interventions focused on self-BP monitoring, physical activity, reduced sodium intake, and medication adherence to improve hypertensive care. 18 Another study by Contreras et al., made use of an app, AlerTHA, on hypertensive patients’ mobile phones to enhance BP control and pharmacological therapy adherence via health education and reminder of appointments. 24 Social media platforms have also shown to be crucial with a study in China demonstrating how WeChat app, through health education, health promotion, group chats, and blood pressure monitoring, help patients lower blood pressure and improve the effectiveness of self-management.61,62
Additional benefits have also been described when blood pressure telemonitoring is offered under the supervision of healthcare personnel.62,63 The effective treatment of hypertension requires self-management, and with the development of mobile technologies, mHealth assists in the management of hypertension. 64 Also, it was noted that patients’ medication adherence and self-management behaviours had improved when mobile app was used to control patients’ hypertension. 25 According to Li et al., 64 the most effective mobile apps integrate customised messages, interactive communication, and complex features.
In order to motivate patients to engage in healthy behaviours and embrace healthy lifestyles, mobile applications that contain gamification aspects, such as prizes and challenges, are also available.65,66
Interventions using short message service technology (or other offline mHealth strategies)
Eleven37–40,42,45–48,54,55 out of 14 papers reviewed with focus on SMS and other offline mHealth interventions (n = 14)37–48,54,55 improved hypertension management significantly. Most of the papers were randomised controlled trials (n = 8).37,38,40,42,45–47,54 Most studies39,42,47,48 were conducted in the United States of America (n = 4).
The self-management and control of chronic illnesses, including hypertension and diabetes, have benefited from the usage of Short Message Service (SMS), chatbots, and other offline mHealth techniques that communicate mostly through short texts in telecommunications.62,67
SMS has been shown to be effective in reminding patients to take their daily meds at a low cost with high results. 68 In fact, it has been a significant source of patient–physician monitoring for brief and rapid communication, especially in difficult-to-reach places. SMS is a remarkable mHealth intervention in the treatment of hypertension that helps prevention of disruption of daily routines, preference for natural therapies, anxiety about side effects, forgetfulness, and inconvenience. 19
More specifically, SMS has made it possible to monitor and evaluate clinical and behavioural outcomes of patients as this brief messaging and offline technique improves patients’ adherence as a form of reminder for the control and management of blood pressure. 64
In order to achieve quality health delivery while keeping patient care in mind, offline mHealth strategies have indeed been helpful in minimising racial disparities. 39 Additionally, it has given healthcare professionals the chance to spend time caring for other patients by reducing the number of unnecessary hospital visits by patients managing hypertension. Due to the present shortage of healthcare professionals, mHealth technology has been supporting the need to prioritise scheduling more patients in order to ensure that they can receive high-quality care. 69
Interventions using web-based or websites
A total of 10 papers49–58 reviewed included web-based technology as its intervention to improve hypertension management. Only one 49 study reported no significant improvement in hypertension care. A total of six papers49,53,54,56–58 were randomised controlled trials. Two (2) studies were conducted in the United States of America50,52 and Sweden49,53 while a paper each from Russia, 58 Canada, 54 Panama, 57 China, 51 Japan, 56 and United Kingdom. 55
Sam Liu et al. conducted a randomised controlled trial to show the significance of expert-driven web-based interventions compared to the self-guided interventions. 70 This study reported a greater systolic blood pressure reduction among the expert-driven group when compared to the control group. However, systolic blood pressure reduction did not significantly differ between user- and expert-driven. A self-monitoring automated electronic sphygmomanometer was studied in relation to the usual care of routine clinic visits in Taiwan. 71 The intervention group also reported a significant decrease in the overall defined daily dose of medications and a significant improvement in health-related quality of life in comparison with the control. 71 Villarreal et al., developed a platform which is an integrated form of mobile application and a web-based application called AmIHealth. 57 The mobile application is the main platform for patient interaction which allows the recording and storing of vital signs of patients in a local database, while the web application obtains data from the mobile application when there is internet connectivity. Doctors can then have access to and follow up on the records of their patients from the web application thereby allowing for the generation of a prevention plan more appropriate to each patient.
Non-adherence to medications has been found to be a remarkable cause of treatment failures, increasing mortality, and costing about $100b every year.25,72 A prospective study was carried out by Yeung et al. involving 68 patients with the aim of investigating the effectiveness of low-health literacy educational interventions such as paper flashcards and quick response coded online videos in improving medication adherence in patients using heart failure, hypertension, and diabetes medications. 50 The study reported that 88% of patients were satisfied with the educational intervention and would recommend it to family and friends. 50 Web-based intervention can allow patients to take an active role in the management of their hypertension. For instance, a randomised control trial using an interactive web-based system conducted showed that people who made use of the web system had a good understanding of how their blood pressure was affected by their lifestyle and are inspired to live a healthy lifestyle. 53
Limitations of mHealth
mHealth, despite its benefits and ease of use, is however not void of limitations. A major one noted during this review was the fact that hypertension status was self-reported by the patients in a number of studies, thus giving way for over- or underreporting, as well as patient recording errors.25,34,61 A wide variability was also noted among participants with varied literacy and health literacy levels. 16 High attrition rate was also noted as a major challenge among participants due to changes in location, as well as forgetfulness. 25
Of the interventions using web-based or websites and Short Message Service Technology (or other offline mHealth strategies), no limitation was specifically mentioned or stated for any improvement yet. These could be due to limited publications yet in mHealth and digital health in the prevention and management of hypertension.
Limitations of study
This scoping review has some limitations. First, the search period was narrow. This is because of the rapid advancement of digital health technology and a high number of available studies in recent years. Also, the scoping review did not include some databases such as Cochrane database and conference proceedings. The CASP critical appraisal tools used for risk assessment do not have a standardised scoring of quality of study. However, it was chosen because of the availability of checklists for different study designs.
Conclusion
In conclusion, this review shows the potential of mHealth in improving hypertension prevention and management globally including the low- and middle-income countries. It shows the need to combine digital health technologies to achieve better outcomes. It shows the need for more mHealth interventions in Africa to prevent and manage hypertension.
Supplemental Material
sj-xlsx-1-dhj-10.1177_20552076241277172 - Supplemental material for Mobile health technologies in the prevention and management of hypertension: A scoping review
Supplemental material, sj-xlsx-1-dhj-10.1177_20552076241277172 for Mobile health technologies in the prevention and management of hypertension: A scoping review by Abdulhammed Opeyemi Babatunde, Deborah Abisola Ogundijo, Abdul-Gafar Olayemi Afolayan, Olutola Vivian Awosiku, Zainab Opeyemi Aderohunmu, Mayowa Sefiu Oguntade, Uthman Hassan Alao, Abdulrahman Ololade Oseni, Abdulqudus Abimbola Akintola and Olanrewaju Adams Amusat in DIGITAL HEALTH
Footnotes
Acknowledgements
The authors appreciate Dimaji A. Olawuyi and all members and volunteers of the SmileBuilders Initiative for the support in conducting the research.
Consent for publication
All authors provided consent to publication.
Contributorship
AOB and OAA conceptualised and designed the study. ZOA and DAO performed the literature search. DAO, AGO, OVA, ZOA, MSO, AOO, OAA, AAA screened and reviewed articles for inclusion. DAO, OVA, AGO, AAA, AOB, ZOA wrote the first draft of the manuscript. UHA, AGO, AOB did the final literature review, proofreading and copyediting. All authors reviewed the manuscript and approved for submission.
Data availability
Available upon request.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
