Abstract
Objective
The acceptability of being offered a choice from a suite of digital health service options to support optimal diet and exercise behaviors in adults with complex chronic conditions was evaluated. This study sought to understand many areas of acceptability including satisfaction, ease of use, usefulness and user appropriateness and perceived effectiveness.
Methods
This mixed-methods study was embedded within a randomized-controlled feasibility trial providing digital health services managing diet and exercise for adults from specialist kidney and liver disease clinics. Post study surveys and semistructured interviews were used to determine patients’ acceptability of the trial interventions. Quantitative (surveys) and qualitative (surveys and interviews) results were merged using integrative analysis and mapped to each construct of the modified version of the Theoretical Framework of Acceptability.
Results
Seventeen interviews (intervention group) and 50 surveys (
Conclusions
Recipients of digital health services that supported diet and exercise interventions found these useful, effective, and safe. Individualized care, technical support and patient confidence remain important to improve the acceptability of digital health service interventions.
Keywords
Introduction
Chronic conditions are the leading cause of death and disability worldwide, accounting for seven out of 10 premature deaths globally 1 with an estimated 100 million additional quality-adjusted life years lost in 2019. 2 Healthy lifestyle behaviors that include a high-quality diet and regular physical activity are a first-line treatment strategy in this population.3–5
Patient access to diet and exercise support across Australian public health services are often fragmented and under resourced,6,7 relative to the increasing demand complex chronic conditions are placing on the system. Several barriers exist to receiving high quality care, including services being siloed to disease specialities with an increased risk that patients with multimorbidities receiving either repetitious or conflicting diet and exercise advice from a variety of practitioners. 8 At the organizational-level, often tertiary health services are faced with high patient cancelation rates, 9 which continues to be a significant resource burden in outpatient settings. Some of the reasons for lack of attendance relate to overcrowding, long wait times, lack of continuity, infrequent interactions with healthcare professionals, being too unwell to attend, impact on work commitments, travel, and associated costs. 10 There is also little shared decision making with regards to when, where and how patients receive healthcare. 11 Therefore, there is a need to focus on innovative health services which can improve the patient's experience and result in more reliable attendance.
Digital health services are well suited to the management of chronic conditions as they can support assessment and self-monitoring, facilitate virtual repeated contacts with health professionals and offer on-demand access to digital resources. 12 Digital health can involve a wide range of service-provision modalities, including (but not limited to), mobile health applications, video consultations and wearable devices to track behavior. 13 Recent reviews investigating the use of digital health in chronic condition populations have demonstrated improvements in diet quality14,15 and physical activity.16,17 This may be related to improvements in self-efficacy and self-management of lifestyle-related behaviors such as diet and exercise. 18 In addition, there is evidence that digital health lifestyle interventions are feasible for both patient use and service provision for complex chronic conditions.19–22 However, these previous interventions are typically highly prescriptive with limited opportunity for patient choice in the type of digital health services used and amount of engagement with these services.19–22
Integrating patient choice within an intervention could be key to individualizing healthcare and improving clinical outcomes.23,24 Such interventions require rigorous evaluation involving evidence-based approaches. The acceptability of various interventions, including those in digital health, has been evaluated using the Theoretical Framework of Acceptability (TFA),25–29 which consists of seven component constructs. 30 It provides a robust framework for evaluating the acceptability which is important as digital health interventions can be highly complex involving multiple components, interactions, and outcomes. Therefore, the aim of this study was to evaluate the acceptability of being offered a choice from a suite of digital health service options to support optimal diet and exercise behaviors in adults with complex chronic conditions by utilizing the constructs of the TFA.
Mixed Method
Study design and setting
This convergent parallel mixed-methods study 31 was embedded in a single-center 26-week feasibility randomized controlled trial.32,33 The convergent parallel mixed-methods study design, which allows complementary data to be analyzed separately and then integrated together, 31 helped to address the complexity of the research aim. The Utilizing technology for Diet & Exercise Change In complex chronic conditions across Diverse Environments (U-DECIDE) trial was conducted from October 2020 to April 2022, to test the feasibility and acceptability of a digital health diet and exercise intervention. The current study is a component of the U-DECIDE randomized controlled trial and details of this prospectively planned acceptability mixed methods analysis are available via the Australia and New Zealand Clinical Trial Registry: ACTRN12620001282976. https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id = 378337.
Participants were provided written and/or verbal instructions relative to the digital health materials they used or had access to at the baseline data collection session. All participants provided written informed consent prior to the study initiation. The study was conducted in an Australian public tertiary hospital in Brisbane (Princess Alexandra Hospital). This current study has been reported using the Standards for Reporting Qualitative Research, 3 Consolidated Criteria for Reporting Qualitative Research, 35 and the Good Reporting of A Mixed Methods Study checklist 36 (Supplementary Material 1-3). Ethics approval for this study was obtained from the Human Research Ethics Committees of Metro South Health (HREC/2019/QMS/58285) and the University of Queensland (2020000127).
Context
The U-DECIDE study involved a suite of patient selfselected digital health services to support diet and exercise behaviors.32,33 In brief, all intervention and comparator participants had an initial appointment with a dietitian and were provided with usual medical and specialist care. The comparator group continued with standard care which involved patient-centered individualized dietary reviews (either face-to-face or telephone) at a frequency deemed appropriate by the treating clinicians. There was no routine access to exercise specialists in the comparator group.
After the initial dietetic appointment, the intervention group received all subsequent dietary education that aligned with heart healthy guidelines
37
and exercise interventions that aligned with the Australian physical activity guidelines
38
and follow-up reviews via digital health services. All intervention group participants received:
Text messages about healthy eating and physical activity underpinned by behavior change techniques including goal setting, social support, information on health consequences and problem solving. These were semi-personalized as participants could select their desired text message frequency (at least once and up to three times per week). Nutrition mobile application (app) (Sophus Nutrition Pty Ltd, Australia) with mobile and web access, which was available throughout the entire study. Exercise app (PhysiTrack® Ltd, London/UK) with mobile and web access, which was available throughout the entire study. Group-based 45 minute monthly dietetic consultations, via videoconference for five months. Group-based 60 minute weekly supervised exercise training sessions, via videoconference for five months.
Additionally, they had optional (self-selected) access to:
At the start of the intervention period, the intervention group selected their desired text message frequency and which optional digital health services related to diet and exercise they wished to access.
Participants and recruitment
A detailed description of the participant selection and recruitment for the U-DECIDE trial is reported elsewhere. 32 Adults under the outpatient care of specialist kidney and liver disease and kidney/liver transplant clinics were recruited. They were eligible to participate if they had at least one feature of metabolic syndrome 39 and had been referred to a dietitian to improve diet quality, had access to a mobile device or computer with internet access, and were considered suitable to participate by both a medical and an exercise professional. People who were diagnosed as malnourished, were non-English speaking, had a life expectancy of less than six months, were under 18 or over 80 years of age, were pregnant or breastfeeding were excluded. Computer-generated randomization occurred via REDcap 40 electronic data capture tool hosted by The University of Queensland, with stratification of groups by referral speciality (kidney, liver and transplant).
All participants who completed the U-DECIDE trial were invited by email by the research project officer to complete an online feedback survey. A sub-sample of the intervention group of the U-DECIDE trial were purposively sampled based on their health condition (chronic liver disease/transplant and chronic kidney disease [CKD]/transplant) and self-selected digital health use (nutrition app, exercise app, diet and/or exercise video consultations). This group were contacted by phone call and invited by the researcher project officer to provide further in-depth feedback regarding their experience with the study via an individual interview. The participants did not have any knowledge of the interviewer.
Data collection
This study used participants’ characteristics data from the U-DECIDE trial and collected data on the acceptability of digital health services they utilized using online surveys and interviews. Data were collected between April 2021 and April 2022. Study codes were used to deidentify data and ensure anonymity for participants.
Participant characteristics
A research project officer with an allied health professional background collected information on the assigned specialist clinic, age and metabolic features of the participants via the hospital's electronic medical records. Other demographic information including gender, ethnicity and education level were self-reported within an online survey via REDcap 40 prior to U-DECIDE baseline assessment.
Online surveys
A link to the online feedback survey managed via REDcap, was sent to all U-DECIDE intervention and comparator group participants via email prior to their final assessment visit (six months after baseline collection) (Supplemental Material 4, Table S4-1). The survey assessed the acceptability of care with seven survey items asked of both groups. Questions were designed for both groups to assess perceptions on overall support received, as well as the perceived effectiveness of their respective interventions for improving motivation, understanding and confidence related to diet and exercise. The intervention group received additional questions related to the text messages and each of the digital health service options (nutrition app, exercise app, diet and/or exercise video consultations), with questions corresponding to their individual selection, up to an additional 32 items regarding satisfaction, ease of use, usefulness, user appropriateness, perceived effectiveness, and influence on behavior. Questions were developed and piloted with a diverse clinical and research team from the fields of exercise, nutrition, metabolic medicine, eHealth, and psychology. Participant responses were either a 5- or 6-point Likert scale, yes or no, or short answer and open-ended written responses. All survey data was securely stored and retrieved from REDcap for further download and analysis.
Interviews
Individual semistructured interviews were conducted by the primary author (AB) who had no role in providing services to the intervention and comparator groups. The primary author had previous experience conducting qualitative research. Interviews were scheduled for approximately 30 minutes either in person at the final assessment visit at the clinic or via a telephone call at the convenience of the participant. Semi-structured interview questions (Supplementary Material 4, Table S4-2) and prompts were developed by the same diverse clinical and research team as the questionnaire, to gain a deeper understanding on the acceptability of digital health services. Adjustments were made to the interview schedule after the first five interviews to improve the clarity of questions. These were audio-recorded in a private setting (clinic room or telephone) with only the researcher and participant present, transcribed verbatim online using Microsoft Azure Cognitive Services 41 and checked for accuracy against the recording prior to analysis.
Data analysis
Quantitative data
In order to identify significant demographic differences between participants who were included in the current study and those who were not, data were analyzed with descriptive statistics using SPSS (IBM Version 29.0). Shapiro-Wilks test was used to assess the normality of these data. Categorical data was analyzed using the Fisher Exact or Pearson Chi-square nonparametric tests to compare those in the study who completed and those who did not complete the survey.
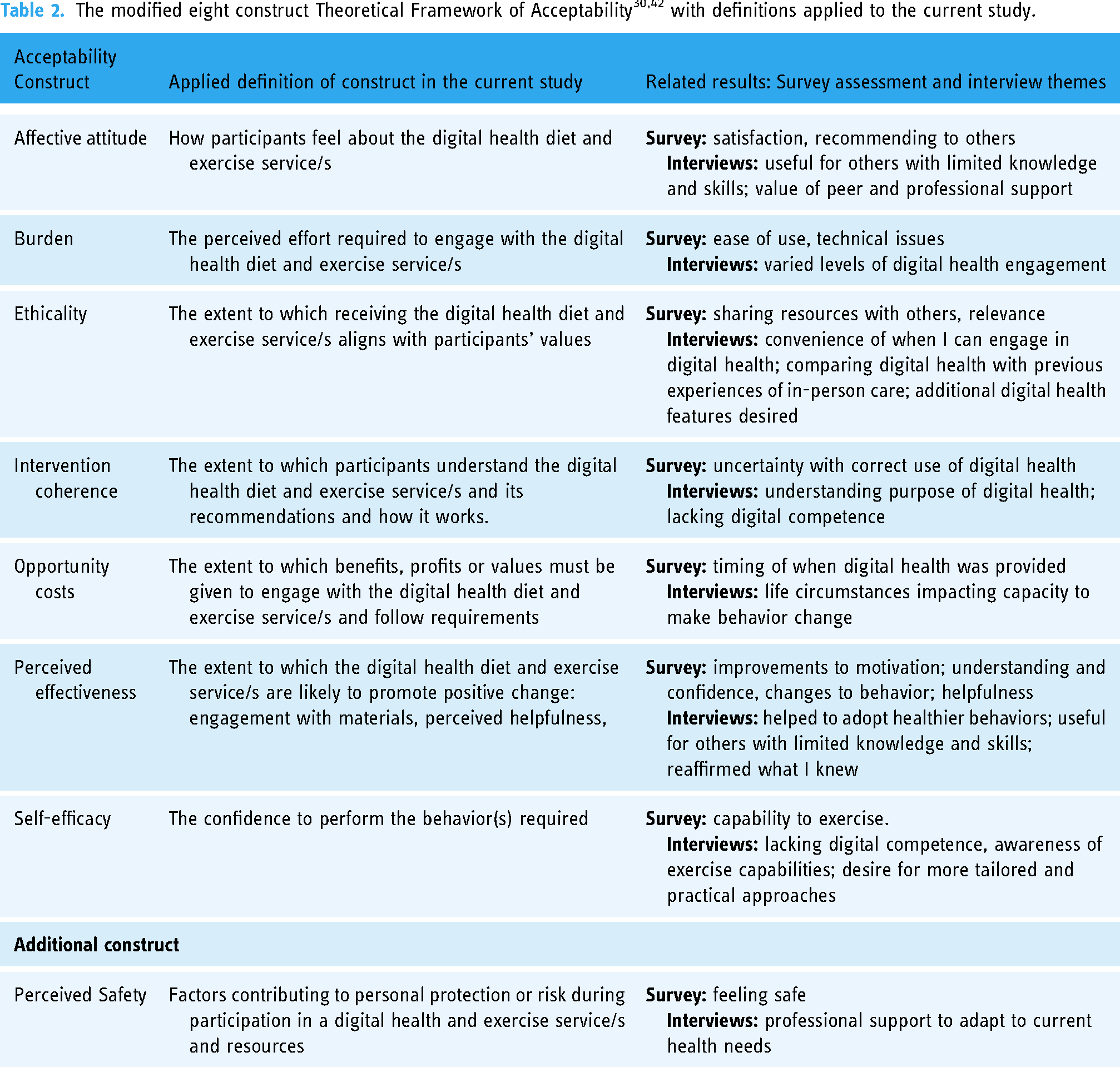
The same tests were used to identify significant differences between the comparator and intervention groups to understand how their respective interventions impacted their understanding of diet/exercise; their confidence to choose healthy meal and snack options/suitable exercise options; and their motivation to eat healthily and exercise regularly. The survey results were then reported against the seven constructs of the TFA30 and the additional construct of safety as proposed by McDonald et al. 42 The TFA consists of seven constructs namely, Affective Attitude (feelings), Burden (perceived effort), Ethicality (fit with values), Intervention Coherence (comprehensibility), Opportunity Costs (what is given up), Perceived Effectiveness (likelihood of benefit), and Self-Efficacy (confidence to do what is required). An additional construct “perceived safety and risk” has also been added to the original TFA. 42 Safety can impact other areas of health including lifestyle management particularly when it is delivered remotely via digital health and involves self-management of behaviors. 43
Qualitative data
Individual semistructured interviews were thematically analyzed using an interpretivist approach.
44
The primary author (AB) familiarized themself with the data and deductively assigned codes to sections of the transcripts that were deemed relevant to the research aim and objectives using NVivo software (Version 12 Pro, QSR International Pty Ltd). Attempts to identify in-vivo codes
45
were made by highlighting words and phrases that commonly appeared in the transcripts. A subsample of transcripts (
Integration and presentation of results
Data integration occurred at the analysis and interpretation phase of the mixed methods design, with several authors (AB, JK, IH, NB, and SC) involved in the process. Quantitative (surveys) and qualitative (surveys and interviews) results were merged using integrative analysis and mapped to each construct of the modified version of the TFA. The themes from the interviews have been italicized in the main text. Definitions for each TFA construct were applied in context with the current study and presented in Table 2. Agree/strongly agree and disagree/strongly disagree Likert scale responses were combined to form two categories of agree and disagree, respectively. This was also done for the Likert scale results dealing with satisfaction, ease of use, helpfulness, and effectiveness. The midcategory options remained unchanged.
Results
Seventy-five percent (
Participant characteristics. Data are median [IQR] or
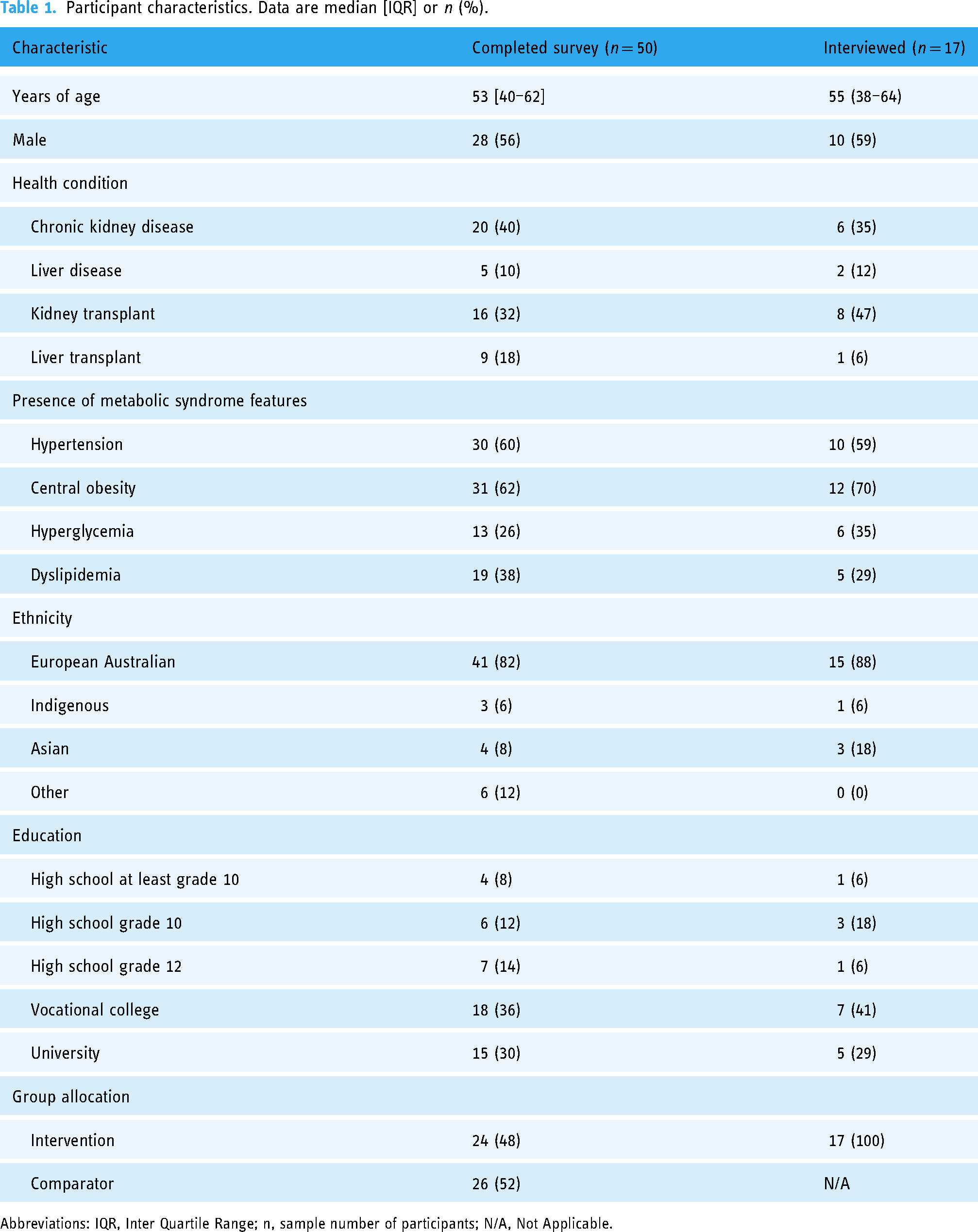
Abbreviations: IQR, Inter Quartile Range; n, sample number of participants; N/A, Not Applicable.
Affective attitude (satisfaction)
The survey results showed 83% (
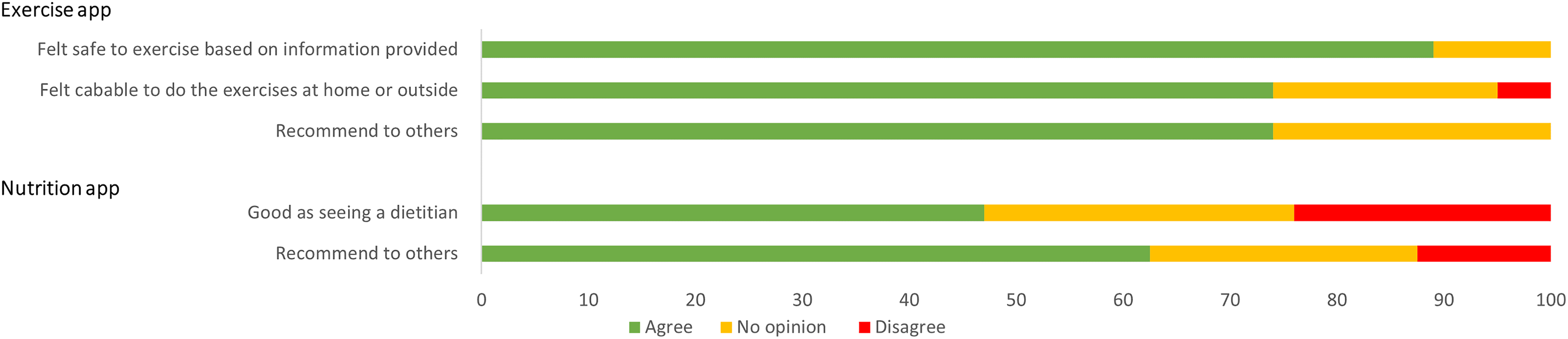
A bar graph showing how they feel about the exercise app (
Two interview themes reflected the affective attitudes construct. Participants reported that digital health services may be
Interview data indicated a theme that there were mixed attitudes toward the value of peer and professional support. Some participants had positive experiences in which they shared ideas and were inspired by discussion within their diet video consultations: “It was actually really good to have another study person because I picked up stuff from them” (47-years male, CKD). However, a minority of participants who were not exposed to a group setting had opposing views and were concerned about relevance of the group discussions: “The thought of just sitting online chatting to a load of old men about their bacon sandwiches just was like … I don't think I'll get much benefit from it, if you know what I mean” (40-years female, CKD). For some participants who had selected the exercise video consultations, scheduling a time held them accountable to attend sessions where they knew other participants and health professionals were involved: “I think with an exercise physiologist it was good because I knew I had to get up in the morning and do it … if I'm accountable, I'll do it” (65-years male, kidney transplant).
Burden (ease of use)
Survey and interview results indicated mixed degree of burden. The survey revealed that technical problems were encountered by approximately one in five participants using the digital health services (21%,

A bar graph showing perceived ease of use of the features embedded in the exercise app (
Varied levels of digital health engagement was a theme that emerged from the interviews related to the burden construct. Some participants reported that their engagement with the exercise app ranged from weekly to monthly use. Most participants who chose to use the nutrition app reported briefly looking at the resources at the beginning of the study: “Yeah, flicked through a few recipes, so not much (use)” (55-years female, CKD). Some indicated that they read the text messages straight away, while others read them later or did not read them at all. Several participants admitted to forgetting the digital health services they selected including the video consultations and the apps: “Sorry, I don’t remember using it” (22-years male, liver disease).
Ethicality (matching core values)
The survey and interview results show a mixed degree to which participants thought the intervention matched their values. Eighty-eight percent (
There were three themes related to participant values.
The interview theme of
Intervention coherence (understanding of requirements)
In the survey’s open-ended response, participants also described that digital health was challenging and expressed uncertainty about whether they were using it correctly.
The interviews demonstrated varying comprehension toward the digital health services. The theme
However, the theme
Opportunity costs (benefits, profits, and values given to engage)
The survey data revealed that 71% (
The interviews revealed that common “costs” of using digital health services were competing with life demands and time. The theme
Perceived effectiveness (positive impact on motivation and behavior change)
There were similar perceptions of the effectiveness of digital health and usual care services to improve motivation to eat healthily, 67% (

A bar graph showing the perceived effectiveness of the comparator (
Survey results revealed that since receiving the text messages, 38% (
However, several participants reported not using the fact sheets (38%,
Self-efficacy (confidence)
Survey data revealed 77% (
There were three themes related to self-efficacy. The theme
Perceived safety
Seventy-seven percent (
Discussion
This mixed-methods study aimed to evaluate the patients' acceptability of being offered choice from a suite of digital health services to support diet and exercise behaviors in complex chronic conditions by using the TFA. The results found a high acceptability towards several key dimensions for the intervention group, including affective attitudes (seeing the benefit for others and long term use), ethicality (alignment with core values, particularly convenience), minimal burden (ease of use, particularly the exercise app), perceived effectiveness (positive impact on motivation and behavior change), intervention coherence (understanding and valuing that the services aligned with each other), self-efficacy (confidence, particularly with exercising unsupervised), and perceived safety. Lower areas of acceptability included self-efficacy specifically in terms of individualization and digital literacy while opportunity costs associated with competing life demands were a limiting factor. There was no significant difference between participant groups in terms of the quantitatively reported perceived effectiveness in enhancing comprehension, confidence, and motivation.
Our study indicates that heterogeneous patient cohorts with complex clinical needs show varied levels of perceived acceptability for digital health services. Indeed, the diversity of experiences for our study may have been the result of intervention participants selecting different digital health options and having varied levels of engagement with their own choices. However, research shows that ambivalence is typical of digital health interventions in various chronic disease populations. 12 It suggests there is likely no one size fits all approach; which appears to be a common theme within the literature related to digital health. 47 Therefore, individualized patient care and flexible delivery options are key factors for effective digital health interventions. Participants highlighted the need for individualized care to enhance their acceptability of the digital health services they used or had access to. The survey results revealed that most participants in the intervention group found the exercise information relevant while less found this to be the case for the dietary information they were provided. This was further supported by the interviews where several participants felt they already knew the information that was provided by the digital health services, particularly in relation to nutrition.
Previous studies have suggested that digital health services for lifestyle behavior management are especially suitable for those recently or newly diagnosed48,49 or in an acute recovery phase. 50 Furthermore, some research also argues that individualizing healthcare goes beyond acceptability research and needs to consider patient-reported psychological and quality-of-life measures.18,51 This highlights a need to consider individualizing services based on the various stages of a treatment journey, which might impact participants’ adherence to the proposed interventions and sustainability of behavioral changes.
A high percentage of participants reported in the survey that the information about how to use digital health services was perceived to be effective which was predominantly provided at the beginning of the study. Few also reported in the survey experiencing technical difficulties. However, the interviews revealed varying levels of digital literacy and a real challenge for participants who were less digitally competent. Kidney transplant recipients involved in other digital health lifestyle interventions have valued the information received at the commencement of the study 50 ; however, some participants have had concerns with the procedures that followed. 52 In the current study, some participants admitted to not reaching out for assistance if they had technical issues; and therefore, did not engage with the digital health services they selected. Therefore, actively checking with the user and providing the option for technical support throughout the duration of use should be considered. However, implementing this in clinical practice would be challenging as an additional demand on the workforce. Some research has suggested a digital health support officer role may evolve from this landscape, which has already been identified as of high value among healthcare providers involved in nutrition care. 53
Strengths and limitations
In this study the qualitative results provided further depth to the quantitative results and thus it may be considered a more comprehensive assessment. A further strength was surveying both randomized groups (intervention and comparator), to allow for comparisons in perceived effectiveness of the innovative digital services and non-digital usual care services. Using an established framework to guide the analysis helped to structure meaning within the multiple components of acceptability. However, this study had some important limitations. As a result of COVID-19 health pandemic related disruptions, the nondigital usual care comparator group may have been exposed to more telephone services than was usual or expected; therefore, it is not an accurate reflection of usual care within this clinical setting. Furthermore, not surveying, or interviewing participants halfway through the study did not allow comparisons between these time points to identify any differences and/or similarities in these time points could be considered a limitation. Assessment halfway may have captured perspectives of participants more closely to peak engagement which is evidently at the beginning of most mHealth interventions. 54 Standardized or validated intervention acceptability surveys exist in digital health55,56; however, they are highly context-specific and not appropriate for this cohort whereby the research question specifically related to the acceptability of digital health services that were accessed and utilized in this study. The study was conducted in an Australian tertiary hospital context and focused on a specific patient group; and therefore, not generalizable to other countries, or the private sector or relevant to other patient groups.
Conclusion
This study evaluated the acceptability of patient self-selected digital health diet and exercise services to support people living with complex chronic conditions. The study found that components of these digital health services were perceived to be useful, safe and effective for changing diet and exercise behavior. However, competing life demands, low digital literacy and a desire for more individualized care impacted acceptability of these digital health services. Overall, perceived acceptability of these digital health services varied with this patient group; and therefore, flexibility in care and user choice is important. These findings can assist with the future design and implementation of digital health diet and exercise services in this population.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076241245278 - Supplemental material for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study
Supplemental material, sj-docx-1-dhj-10.1177_20552076241245278 for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study by Amandine Barnett, Soraia de Camargo Catapan, Dev K Jegatheesan, Marguerite M Conley, Shelley E Keating, Hannah L Mayr, Lindsey Webb, Riley C C Brown, Jeff S Coombes, Graeme A Macdonald, Nicole M Isbel, Nicola W Burton, Katrina L Campbell, Ingrid J Hickman and Jaimon T Kelly in DIGITAL HEALTH
Supplemental Material
sj-docx-2-dhj-10.1177_20552076241245278 - Supplemental material for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study
Supplemental material, sj-docx-2-dhj-10.1177_20552076241245278 for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study by Amandine Barnett, Soraia de Camargo Catapan, Dev K Jegatheesan, Marguerite M Conley, Shelley E Keating, Hannah L Mayr, Lindsey Webb, Riley C C Brown, Jeff S Coombes, Graeme A Macdonald, Nicole M Isbel, Nicola W Burton, Katrina L Campbell, Ingrid J Hickman and Jaimon T Kelly in DIGITAL HEALTH
Supplemental Material
sj-docx-3-dhj-10.1177_20552076241245278 - Supplemental material for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study
Supplemental material, sj-docx-3-dhj-10.1177_20552076241245278 for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study by Amandine Barnett, Soraia de Camargo Catapan, Dev K Jegatheesan, Marguerite M Conley, Shelley E Keating, Hannah L Mayr, Lindsey Webb, Riley C C Brown, Jeff S Coombes, Graeme A Macdonald, Nicole M Isbel, Nicola W Burton, Katrina L Campbell, Ingrid J Hickman and Jaimon T Kelly in DIGITAL HEALTH
Supplemental Material
sj-docx-4-dhj-10.1177_20552076241245278 - Supplemental material for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study
Supplemental material, sj-docx-4-dhj-10.1177_20552076241245278 for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study by Amandine Barnett, Soraia de Camargo Catapan, Dev K Jegatheesan, Marguerite M Conley, Shelley E Keating, Hannah L Mayr, Lindsey Webb, Riley C C Brown, Jeff S Coombes, Graeme A Macdonald, Nicole M Isbel, Nicola W Burton, Katrina L Campbell, Ingrid J Hickman and Jaimon T Kelly in DIGITAL HEALTH
Supplemental Material
sj-docx-5-dhj-10.1177_20552076241245278 - Supplemental material for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study
Supplemental material, sj-docx-5-dhj-10.1177_20552076241245278 for Patients’ acceptability of self-selected digital health services to support diet and exercise among people with complex chronic conditions: Mixed methods study by Amandine Barnett, Soraia de Camargo Catapan, Dev K Jegatheesan, Marguerite M Conley, Shelley E Keating, Hannah L Mayr, Lindsey Webb, Riley C C Brown, Jeff S Coombes, Graeme A Macdonald, Nicole M Isbel, Nicola W Burton, Katrina L Campbell, Ingrid J Hickman and Jaimon T Kelly in DIGITAL HEALTH
Footnotes
Acknowledgments
We would like to thank all the participants who shared their experience with being part of the U-DECIDE study. AB was supported by an Australian Government Research Training Program stipend for a Doctor of Philosophy program. JTK was supported by a Postdoctoral Fellowship from the National Heart Foundation of Australia (106081). Availability of data and materials: The datasets used and/analyzed during this study are available from the corresponding author upon reasonable request.
Contributorship
IJH, GAM, KLC, JSC, NMI, MMC, HLM, DKJ, RCCB, LW and SEK conceived the study. AB, IJH, SCC, JTK, NWB and KLC contributed to the mixed-methods study design and data analysis. AB wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the last version of the manuscript.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The Human Research Ethics Committees of Metro South Health (HREC/2019/QMS/58285) and The University of Queensland (2020000127).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Queensland Health, Health Practitioners Research Scheme, and the Metro South Health Research Support Scheme (Grant No. N/A).
Guarantor
IJH.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.