Abstract
Objective
To examine the effects of online health information seeking (OHIS) behavior on five health behaviors (regular physical activity, less sedentary, calorie checking, no alcohol consumption, and no smoking) among adult cancer survivors in the United States.
Methods
A cross-sectional analysis was conducted with adult cancer survivors (≥18 years old) from Cycles 2, 3, and 4 of the Health Information National Trends Survey (HINTS). The respondents self-reported OHIS, and the data on the five health behaviors were pooled to perform descriptive and multivariable logistic regression analyses using Stata 17.0.
Results
Of the 1245 adult cancer survivors, approximately 74% reported OHIS behavior for themselves within the previous year of the survey. We found that OHIS was significantly and positively associated with the level of physical activity (odds ratio [OR] = 1.53,
Conclusions
Findings from this study suggest that most cancer survivors used various forms of digital tools and platforms to seek health information. The study also demonstrated an independent impact of OHIS behavior on physical activity and calorie checking. Healthcare professionals may need to encourage and guide cancer survivors to seek credible eHealth information and further utilize digital health tools as a platform for care delivery, promoting health behaviors and preventing adverse health outcomes among cancer survivors.
Introduction
Cancer survivors continue to grow due to the rapid development of diagnostic tools, early detection, and advanced therapeutic treatments.1,2 Optimizing patients’ long-term health and well-being after cancer treatments is being increasingly emphasized as part of their standard care of cancer.3,4 Risks for cancer recurrence and overall survival may be affected by modifiable behavioral risk factors, such as physical activity, diet, smoking, and alcohol intake.4–7 Studies have shown that poor lifestyle health behaviors are the leading preventable causes of death in the United States. 8 Lifestyle health behaviors are commonly influenced by sociodemographic factors and psychological well-being (e.g., depression and anxiety).9–11 The benefits of engaging in these health behaviors are clear; thus, the American Cancer Society has recently released its third nutrition and physical activity guideline for cancer survivors. 4 However, many cancer survivors are not meeting the recommended guidelines for these behaviors.12,13 Therefore, efforts are needed to identify ways in which healthcare professionals can encourage and support cancer survivors in adopting and maintaining health behaviors.
According to the health belief model,14,15 which explains and predicts health behaviors, cancer survivors need to perceive the risk of developing more chronic conditions, understand the severity of existing disease, recognize the benefits of health behaviors, feel the absence of barriers to health behaviors’ change, have confidence in their abilities to implement health behaviors, and require cues to change behaviors prior to adopting health behaviors. These cues can be either internal or external (e.g., advice from others, illness of family member, and news information). 14 Therefore, online health information not only offers an opportunity to increase their self-efficacy and knowledge about the benefits of health behaviors but is also considered as an external cue to action. Therefore, online health information seeking (OHIS: refers to the search for details on symptoms, diagnoses, and treatments for various diseases, or simply seeking general information on weight loss, healthy diets, or wellness tips online 16 ) behavior expands people's existing knowledge and change beliefs and attitudes about health behaviors,17,18 thus promoting the adoption of health behaviors.
Previous research provides evidence that OHIS positively affects dietary behaviors, physical activity, smoking, and alcohol consumption in the general adult population.9,10,19,20 Overall, most studies suggest the beneficial effects of OHIS on health behaviors. However, to our knowledge, there is a lack of research examining these associations in cancer survivors, a group that would benefit more from the promotion of health behaviors. Cancer survivors demonstrate lower prevalence rates of smoking, alcohol consumption, physical activity, and maintenance of a normal body mass index (BMI) compared to individuals without a history of cancer.21,22 In this study, we examined the associations of OHIS with five health behaviors (physical activity, sedentary behavior, calorie checking, alcohol consumption, and smoking) among cancer survivors. We hypothesized that OHIS could promote certain health behaviors among cancer survivors, such as regular physical activity, reduced sedentary behavior, calorie checking, decreased alcohol consumption, and smoking cessation.
Methods
Study population
We used the combined survey data from Cycle 2, Cycle 3, and Cycle 4 of the National Cancer Institute's Health Information National Trends Survey (HINTS) 5. HINTS is a cross-sectional survey conducted on a nationally representative sample of non-institutionalized US (United States) adults and weighted to represent the US population. 23 The three survey cycles were conducted in 2018, 2019, and 2020, with 12,807 respondents. Details on sample selection, data collection, and data management of the HINTS are described in previous articles.23–25 HINTS was reviewed by the Westat Institutional Review Board. Participant consent was waived because HINTS was classified as exempt by the US National Institutes of Health Office of Human Subjects Research Protections. The HINTS data is de-identified and publicly available from the HINTS website: https://hints.cancer.gov/.
We restricted our study to respondents who had diagnosis of cancer (2075). We also excluded respondents with missing values on any of the following variables: physical activity, sedentary behavior, cigarette smoking, drinking status, calorie checking, and covariates, resulting in a final sample size of 1245 cancer survivors.
Measurements
The key independent variable is OHIS. To assess OHIS behavior, cancer survivors were asked: “In the past 12 months, have you used a computer, smart phone, or other electronic means to look for health or medical information for yourself?” (1 =
The outcome of interest includes five health behaviors: physical activity, sedentary behavior, calorie checking, smoking status, and alcohol consumption. Cancer survivors were asked two questions to measure their physical activity: (a) “In a typical week, how many days do you do any physical activity or exercise of at least moderate intensity, such as brisk walking, bicycling at a regular pace, and swimming at a regular pace?” and (b) “On the days that you do any physical activity or exercise of at least moderate intensity, how long do you typically do these activities? Minutes per day.” We multiplied these two items and grouped participants into three categories based on the self-reported moderate physical activities in a week: no (no physical activity), light physical activity (participated moderate physical activity but less than 150 min per week), and moderate physical activity and meeting guidelines (moderate physical activity with greater than 150 min per week). 26
Sedentary behavior was assessed with one item: “During the past 7 days, how much time did you spend sitting on a typical day at home or at work?” Because the distribution of sedentary time was positively skewed (skewness = .802,
Calorie checking was measured by asking “Think about the last time you ordered food in a fast food or sit-down restaurant; did you notice calorie information listed next to the food on the menu or menu board?” (1 =
Cigarette smoking status was measured by asking two smoking-related questions “Have you smoked at least 100 cigarettes in your entire life?” and “How often do you now smoke cigarettes?” Respondents were then grouped into three categories: former smokers, current smokers, and never smokers.
Alcohol consumption was assessed using the following two questions: (a) “During the past 30 days, how many days per week did you have at least one drink of any alcoholic beverage?” and (b) “During the past 30 days, on the days when you drank, about how many drinks did you drink on average?” Respondents’ average weekly alcohol consumption was calculated by multiplying these two items. We further grouped participants into three categories according to the definition of the National Institute on Alcohol Abuse and Alcoholism 27 : non-drinker, moderate drinker (females who drank 1–7 glasses or males who drank 1–14 glasses of alcoholic beverage per week), and heavy drinker (females who drank more than 7 glasses or males who drank more than 14 glasses of alcoholic beverage per week).
In line with previous studies,9–11 the following covariates were included: BMI, education, race, household income, marital status, sex, depression, and/or general health and also age (in years), sex (1 =
Statistical analyses
We used Stata 17.0 to perform all data analyses and set the α level at .05. First, we conducted descriptive analyses to understand the characteristics of the study population. Second, traditional visual inspection and several statistical tests (e.g., variance inflation factor, Durbin–Watson statistic, and Cook's distance) were performed to ensure that ordinary least squares (OLS) assumptions were met adequately. There was no multicollinearity problem between predictors, and the variance inflation factors of all predictors were 2.52. Next, linear or logistic regression models depending on whether the outcome was categorical or continuous were applied to test associations between OHIS and physical activity, calorie checking, cigarette smoking status, and drinking status, after controlling for age, sex, education, race/ethnicity, marital status, household income, BMI, depression, and general health.
Results
Table 1 presents the descriptive characteristics of cancer survivors. They were primarily female, never smokers, reported no alcohol consumption, had some college education, identified as non-Hispanic White, were married, had a household income ranging from $20,000 to $49,999, participated in physical activity, reported no depression, no calorie checking, and had a general good health status. The mean self-reported sedentary time, BMI, and age of the cancer survivors were 7.21 h (
Characteristics of cancer survivors.

Abbreviations: PA: physical activity; M: mean; SD: standard deviation.
Table 2 shows the results of initial regression models predicting physical activity, calorie checking, alcohol consumption, smoking, and sedentary behavior from OHIS behavior before adjusting for covariates. Among the five health behaviors, physical activity, calorie checking, and alcohol consumption were all significantly associated with OHIS (
Regression models assessing OHIS on health behaviors prior to adjusting for covariates.
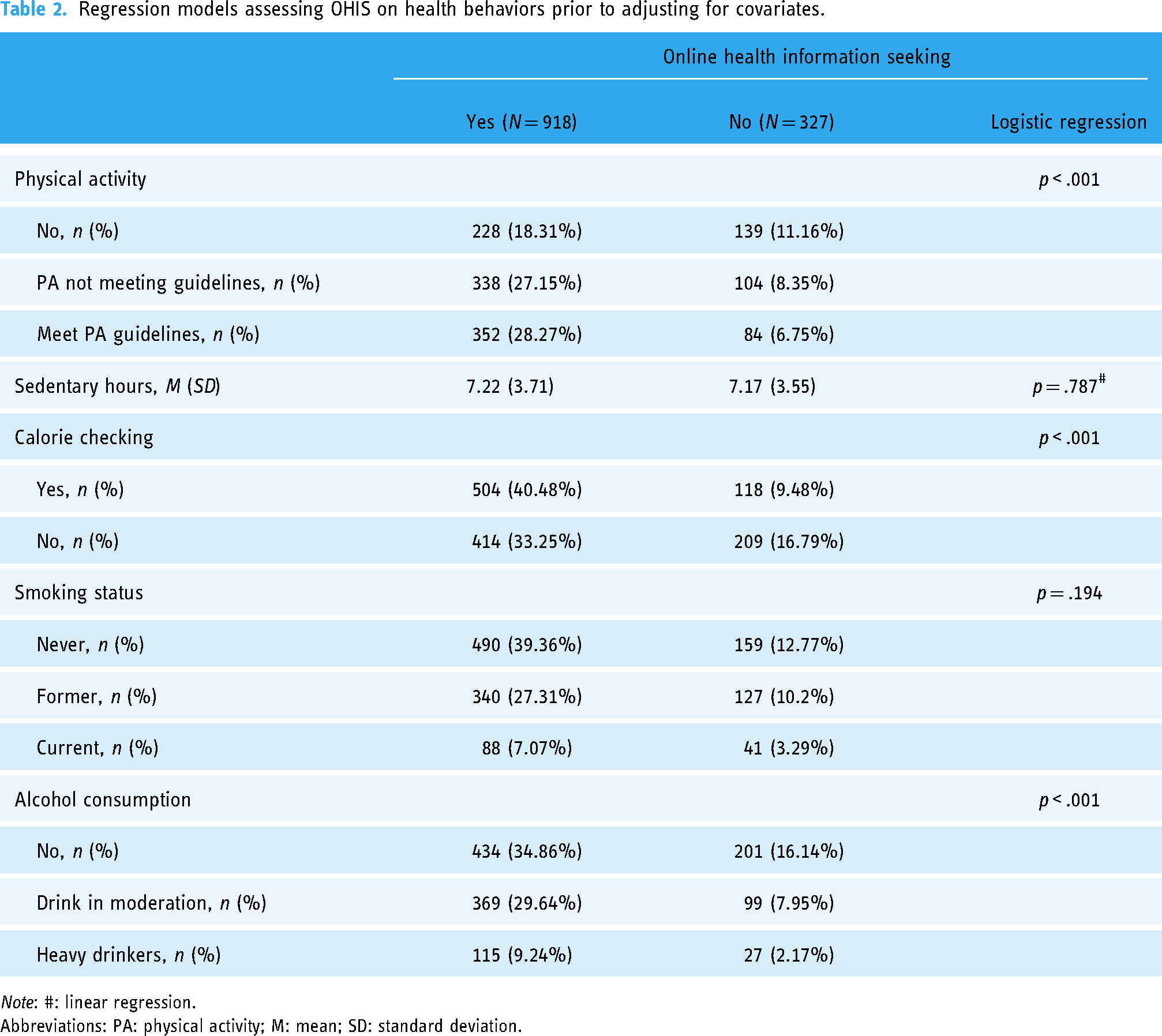
Abbreviations: PA: physical activity; M: mean; SD: standard deviation.
Table 3 presents the results from an ordered logistic regression model predicting levels of physical activity from OHIS behavior. The results indicated that cancer survivors who engaged in OHIS were 53% (
Ordered logistic regression assessing OHIS impact on levels of physical activity.
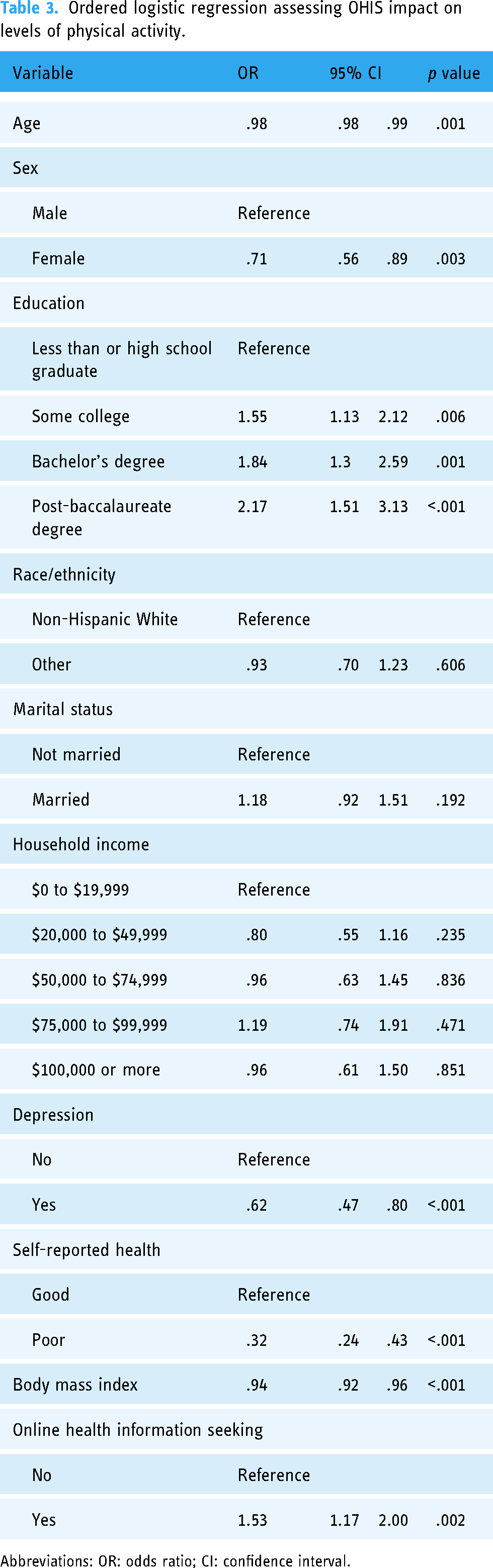
Abbreviations: OR: odds ratio; CI: confidence interval.
Table 4 presents the results from a binary logistic regression model predicting calorie checking based on OHIS. The odds of calorie checking among online health information seekers increased by a factor of 1.65 (
Binary logistic regression assessing OHIS impact on health behavior in calorie checking.
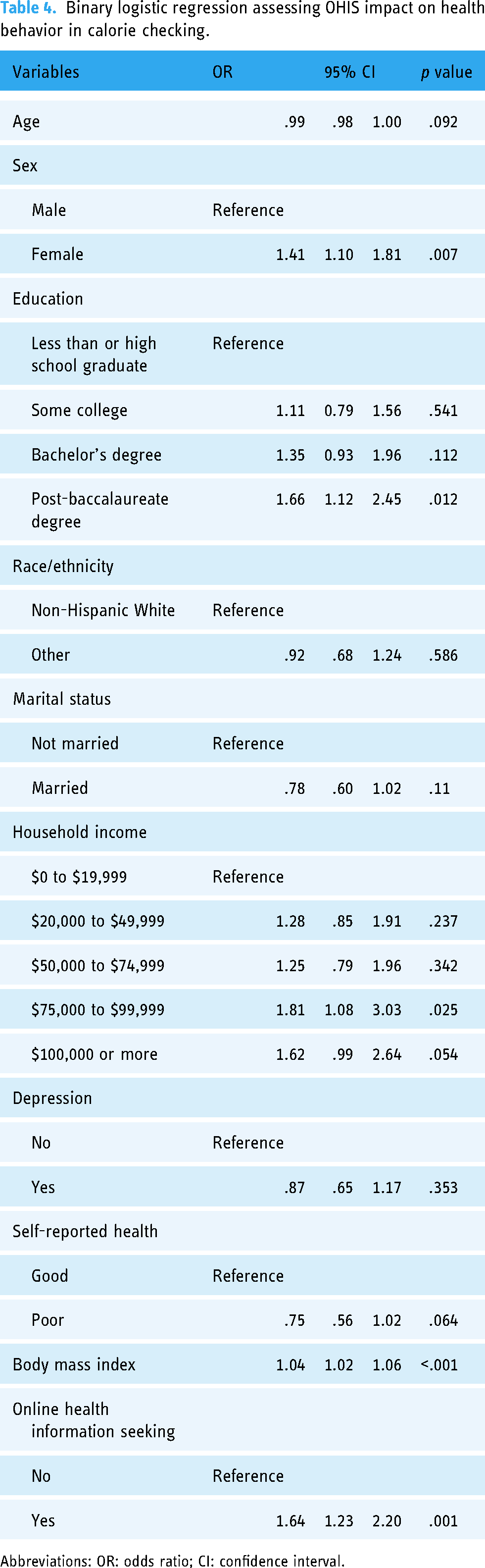
Abbreviations: OR: odds ratio; CI: confidence interval.
Discussion
The present study examined the association between OHIS and five lifestyle health behaviors among cancer survivors. We found that OHIS behavior was significantly associated with an increased physical activity participation and calorie checking among cancer survivors, but not with sedentary behavior, alcohol consumption, or smoking, after adjusting for covariates. To our knowledge, this is one of the first studies to investigate the effects of OHIS on health behaviors specifically among cancer survivors. Previous studies have explored the association between OHIS and various lifestyle health behaviors. For instance, a community-based cross-sectional study found that OHIS behavior was positively associated with fruit and vegetable consumption and physical activity among Hispanics. 19 Another cross-sectional survey study demonstrated that OHIS was positively associated with fruit/vegetable intake but negatively associated with smoking. 9 Chae et al. 28 also reported that online health-related activities were positively associated with two dietary behaviors including calorie checking on menu and fruit/vegetable consumption. Additionally, nearly half of health internet users expressed a desire to change their diet and increase physical activity based on the health information obtained online. 29 Moreover, individuals who utilized the internet for assistance with their diet, weight management, and physical activity exhibited higher vegetable/fruit consumption and engaged in more moderate exercise. 30 Overall, our findings suggests that cancer survivors with OHIS behavior are more likely to be more physically active and be aware of their caloric intake.
On the other hand, we found no correlations between OHIS and sedentary behavior, alcohol consumption, or smoking status. The health belief model suggests that OHIS behavior is influenced by risk perceptions and affective risk responses.15,31 Perceived benefits play a role in the relationship between OHIS and health behaviors among cancer survivors. Engaging in physical activity and reducing sedentary behavior not only lowers the incidence and mortality of cancer but also helps alleviate the negative effects associated with cancer treatment, enhances the effectiveness of cancer treatment, improves cancer prognoses, and reduces risks of cancer metastases.32–38 However, compared to the well-recognized benefits of physical activity, cancer survivors may not adequately perceive the risks associated with sedentary behavior.34,35,39–41 This lack of risk perception could explain why our study did not find a significant correlation between OHIS and sedentary behavior. Previous studies have shown inconsistent associations between OHIS and smoking. While some studies found no significant associations, others revealed that smokers were more likely to use the internet for behavioral support.9,19 Similarly, prior research lacks substantial evidence supporting the effectiveness of digital health in reducing alcohol consumption. 42 Given that alcohol and smoking represent significant risk factors for multiple cancers, offline resources (e.g., patient–provider communication) may mitigate the impact of OHIS among cancer survivors.
It is worth noting that in this study, approximately three-quarters of cancer survivors rely on the internet for health information, highlighting its importance as a valuable source of information. In 2013, only one-third of US adults used the internet for health information. 32 The rise of digital technology has led to an increasing number of individuals seeking health information online to assist them in making informed decisions. 43 A recent study discovered that newly diagnosed cancer patients were more likely to seek health information online, even after adjustment for age. 44 These findings have important implications for the development of interventions aimed at promoting health behaviors among cancer survivors. Web-based interventions have proven effective in increasing physical activity levels among individuals with various chronic conditions, including cancer.44–47 Factors such as gender differences, BMI, and mental health should be considered when promoting and supporting the use of eHealth and mobile health tools.
By broadening our understanding of the associations between OHIS and modifiable lifestyle health behaviors among cancer survivors, this study offers opportunities to guide cancer survivors in developing healthier behaviors that can prevent disease progression and improve outcomes. As informational support can stimulate OHIS, leading to intentions for healthier lifestyles health behaviors, 48 healthcare professionals should actively engage in discussions to facilitate the adoption of health behaviors among cancer survivors. Given the inconsistent and conflicting nature of health information found on the internet, 49 healthcare professionals play an essential role in providing guidance and empowering cancer survivors to engage in OHIS activities.
This study has several limitations. Firstly, the cross-sectional design of this study prevents our ability to establish causal relationships between OHIS and health behaviors. Therefore, we cannot preclude the possibility that individuals who engage in health behaviors are more likely to seek health information online. Secondly, relying on self-reported measures from respondents introduces the potential for misclassification, recall bias, and response bias. Thirdly, due to the retrospective nature of this study and the large sample size (
Conclusions
This study provides compelling evidence supporting the association between OHIS and the adoption of specific health behaviors among cancer survivors, including physical activity and calorie checking. It is crucial for health professionals to actively promote the use of trustworthy online health information and provide appropriate guidance and support to ensure its effective utilization. Considering that a considerable number of cancer survivors are already utilizing online tools to access health-related information, future behavioral interventions can explore innovative ways to leverage eHealth and mHealth platforms to facilitate long-term positive behavioral changes in this population. In summary, the findings of this study suggest that eHealth holds great potential as a valuable tool for promoting and sustaining lifestyle health behaviors among cancer survivors who are particularly vulnerable.
Supplemental Material
sj-docx-1-dhj-10.1177_20552076241238074 - Supplemental material for Associations of online health information seeking with health behaviors of cancer survivors
Supplemental material, sj-docx-1-dhj-10.1177_20552076241238074 for Associations of online health information seeking with health behaviors of cancer survivors by Zhaoli Liu, Yue Liao, Chueh-Lung Hwang, Chad D. Rethorst and Xiaoli Zhang in DIGITAL HEALTH
Footnotes
Contributorship
ZL contributed to the study conception, methodology, data analysis, manuscript draft, and editing of the manuscript. YL contributed to the study conception, methodology, manuscript review, and editing. CLH contributed to funding acquisition, manuscript review, and editing. CDR contributed to the manuscript review and editing. XZ contributed to the data analysis, validation, manuscript review, and editing. All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by NIAAA R00 AA028537 to CLH and the National Institute on Alcohol Abuse and Alcoholism (grant number AA028537).
Guarantor
ZL.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
