Abstract
Objectives
In solving the global challenge of sleep disorders, Mobile Health app is one of the important means to monitor, diagnose, and intervene in sleep disorders. This study aims to (1) summarize the status and trends of research in this field; (2) assess the production and usage of sleep mHealth apps; (3) calculate the conversion rate of grants that the proportion of newly developed apps from being funded and developed to published on application stores.
Methods
Using bibliometric and content analysis methods, based on “Research Paper-Product Output-Product Application” chain and considering the “Research Grants” of articles, we conducted a systematic review of eight databases, to identify relevant studies over the last decade.
Results
Over the past decade, 1399 authors published 313 papers in 182 journals and conferences. The number of publications increased with an average annual growth of 41.6%. The current focus area is research using cognitive behavioral therapy to intervene in sleep. Sleep-staging tracking is a shortcoming of this field. A total 368 sleep mHealth apps (233 newly developed and 135 existing) were examined in 313 papers; 323 grants supported 178 articles (56.9%). Only 12 of the newly developed apps are used in the real world, resulting in a 9% grant conversion rate.
Conclusions
In the last decade, the field of tracking, diagnosing, and intervening in sleep disorders using mHealth apps has shown a trend of rapid development. However, the conversion rate of products from being funded and developed for use by end-users is low.
Introduction
Sleep disorders are a global issue with severe hazards that are difficult to mitigate. The American Psychiatric Association (APA) defines sleep disorders as “sleep disorders (or sleep–wake disorders) that involve problems with the quality, timing, and amount of sleep, which result in daytime distress and impairment in functioning.” 1 The third edition of the International Classification of Sleep Disorders (ICSD) has seven major categories: insomnia disorders, sleep-related breathing disorders, central disorders of hypersomnolence, circadian rhythm sleep–wake disorders, sleep-related movement disorders, parasomnias, and other sleep disorders. 2 Research determined that sleep disorders not only increase an individual's risk of developing diseases such as diabetes,3,4 hypertension,5,6 and metabolic syndrome 7 but also cause traffic accidents, 8 and even lead to economic losses to society. 9 The RAND Corporation in 2017 reported that five OECD countries (Canada, the United States, the United Kingdom, Germany, and Japan) collectively lost more than $600 billion annually owing to sleep disorders, for example, $400 billion for the United States and $60 billion for Germany. 9 Unfortunately, the combined prevalence of sleep disorders is between 10% and 45%,10–14 and this number may continue to increase in the future.
Mobile health applications (mHealth apps) are a new type of tool considered efficient for relieving sleep disorders. The popularity of smartphones and the inherent immediacy, accuracy, and low learning costs of the internet have contributed to the unique advantages of the mHealth apps in providing health services. 15 In 2020, over 300,000 mHealth apps worldwide, 16 and more than 500 different sleep-related apps were available in the Apple iTunes app store. 17 These applications can assist users in monitoring and tracking multiple physiological indicators and provide relevant health knowledge and services to treat a range of health problems,18–21 including sleep disorders. Many studies show that mHealth apps can provide continuous and remote sleep tracking as well as diagnostic and intervention services for people suffering from sleep disorders, which can be effective in mitigating or resolving sleep disturbances. Edita Fino and Giuseppe Plazzi et al. 22 used four sleep-tracking apps to monitor the sleep of 21 participants for 42 nights in a real-sleep-environment and compared the accuracy with the “gold standard” polysomnogram (PSG). All apps correlated significantly with the PSG and were highly similar to PSG. 22 Moreover, Hasana et al. 23 conducted a systematic review and meta-analysis of 54 randomized controlled trials including 11,815 participants. Their findings showed that the mobile app-based cognitive behavioral therapy for insomnia (CBTi) sleep intervention significantly increased users’ total sleep time, reduced sleep latency time, and improved sleep efficiency and quality when compared to conventional sleep interventions. 23 From a diagnostic perspective, Omboni and Campolo et al.24 collected evidence from 1471 Italian healthcare facilities and 135,333 patients that have documented the usefulness of an app-based telecare platform for improving access to care and enhancing screening and management of various diseases, including obstructive sleep apnea syndrome. 24 The increased acceptance of mHealth technology in the sleep domain and the continuous iteration of mobile internet technologies have led to a simultaneous surge in the number of sleep mHealth apps and related research. Many review studies have been conducted in this field to elucidate the current research status and trends.17,23,25–28 However, most of these studies have limitations. First, most studies focus on a single type of mHealth app or a single category of sleep disorders. Therefore, the inclusion–exclusion criteria of those studies are particularly stringent, the coverage is not comprehensive, and the conclusions obtained are restrictive. Second, most review studies were dedicated to the performance of mHealth apps (effectiveness, accuracy, etc.) and neglected their applications. An analysis of the applications of mHealth apps would provide insight into how the apps are used in real-world circumstances while providing additional perspectives on the reasons for their failures (low user engagement, etc.). Third, most studies do not integrate the article with the product and do not consider the grant information of the articles. Analyzing these factors can deepen the understanding of a field from a unique perspective and provide references and recommendations to researchers and relevant companies. Finally, some review studies published in earlier periods have findings that are no longer applicable to the current development status. For example, Ko et al. 17 searched multiple app stores for apps that support sleep management and discussed the methodological transparency, the effect on clinical sleep medicine, and various social, legal, and ethical issues of those apps. Considering the aforementioned limitations, the rapid development of mobile internet technology, and the serious hazards and high prevalence of sleep disorders, we believe it is necessary to comprehensively review and summarize the field of research on tracking, diagnosing, and intervening in sleep disorders with mHealth apps.
Using bibliometric and content analysis methods, this study provides a complete and detailed description of the field of tracking, diagnosing, and intervening in sleep disorders using mHealth apps over the past decade. It is the first bibliometric study in this field to comprehensively examine the production, sources, authors, countries, institutions, and research themes of publications. In addition, the analysis of this study is based on a special “Research Paper - Product Output - Product Application” chain, in which the funding status, trends, and conversion rate of research grants were explored creatively from the perspective of “Research Grants” of articles.
Methods
Database selection and search strategy
To cover a comprehensive and complete publication, eight databases were searched to ensure completeness (three in medical health: PubMed, EMBASE, and CINAHL; two in general science: Web of Science and Scopus; three in social psychology: PsycInfo, Psychology and Behavioral Sciences Collection, and APA PsycArticles), the search time range of 2010–2021 (see Appendix 1 for the search formulas and results).
Inclusion and exclusion criteria
From January 1, 2010, to December 31, 2021, 13,106 articles were retrieved, leaving 4436 articles after deduplication. Based on the inclusion and exclusion criteria, 313 articles were selected. The PRISMA flowchart for the selection of articles is shown in Figure 1.

PRISMA flowchart for the selection of articles.
The following inclusion criteria were used for study eligibility: Studies of mHealth technology as a means of tracking, diagnosing, or intervening in sleep disorders. The systematic review excluded studies that met the following exclusion criteria: (1) Reviews, commentaries, letters, and errata; (2) Literature not in English, literature with incomplete information, and literature for which the full text was not available; (3) Studies in which sleep disorders were not the primary target of the article or in which the target was a patient with another disease, and sleep disorders were only used as indicators of patient characteristics; (4) Minor mention of mHealth or mobile internet technology in the background, being used as a tool to track, diagnose, or as an intervention in sleep disorders; (5) Studies that did not use mobile apps as a means of tracking, diagnosing, or intervening in sleep disorders.
Data analysis
This study used bibliometric and content analysis methods, based on the “Research Paper - Product Output - Product Application” chain. [Research Paper] Extract and summarize the characteristics of the included paper, including production of the publication, journal of publication, author of publication, country, institution of publication, and theme of publication. [Product Output] Record the number, type, name, targeted sleep disorder, and function of mHealth sleep apps studied by included papers and divide those apps into two groups (newly developed apps and existing apps that have been licensed or downloaded for research purposes). [Product Application] Based on the article content and online information about the apps, explore the apps’ maturity levels from Level I (apps that exist only in a laboratory environment and have no real-world validation of their effectiveness or accuracy) to Level IV (apps that have been used in the real world). We also considered the “Research Grants” of articles, to review and summarize research on tracking, diagnosing, and intervening in sleep disorders based on mHealth apps.
In the bibliometric section, we quantitatively analyzed the external characteristics of the literature to understand the current research status and trends in the field. The characteristics included were: title, abstract, keywords, first author, author's nationality, author's affiliation, time of publication, name of the published journal, and impact factor of the published journal. We used the R bibliometrix package to analyze literature data, 29 the ggplot2 package for statistical plotting, 30 and the VOS viewer for network visualization. 31
In the content analysis section, we first built a qualitative content analysis framework according to the studies of Aji et al. 28 and Jian et al. 32 Second, based on the analysis framework, we extracted the relevant information about the apps from the content of articles, including the type, name, and function of the app, the app targeted sleep disorder, and the maturity level of app. We also extracted grant information from the acknowledgments section of the article, including the number and name of the grants and the country to which it belongs. Then, based on the extracted information about the apps, we analyzed the product output and product application in this area. Finally, based on grant information, we explored the grant trends and calculated the conversion rate of grants in this field based on the proportion of newly developed apps that are eventually published within application stores. The analysis chain and process of this study are illustrated in Figure 2. To ensure consistency of the extracted information, two graduate students independently extracted the same 100 randomly selected papers and calculated the IAA (consistency of the extracted content between the two individuals). A subject matter expert then arbitrated disagreements in the analysis results, identified potential problems, and modified the predefined analysis framework if necessary.

Analysis chain and process of this study.
Results
Research paper
In this section, we used a bibliometric approach to analyze the included articles from five perspectives: production of publication, journal of publication, author of publication, country and institution of publication, and theme of publication.
Production of publication
From January 1, 2010, to December 31, 2021, 1399 authors published 313 relevant publications in 182 different journals, conferences, and meetings. Trends in annual scientific production are shown in Figure 3. An overall upward trend was observed in the number of annual publications, with an average annual growth rate of 41.6%.

Annual scientific production from 2010 to 2021.
Source of publication
According to the Law of Bradford, 33 the sources of publications in a field can be divided into core, related, and peripheral zones according to the number of articles carried, the ratio of the number of sources in the three zones is 1:a:a2, which is approximately 5. Core sources were calculated to be 13 and occupied approximately 1/3 of the total number of sources. The articles published in these 13 sources accounted for 36.4% of all articles, as shown in Table 1.
Name, number of articles, JCR classification and ranking, and impact factor of 13 core scours.

By plotting the annual publication trends of the core sources, as shown in Figure 4, the Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBS) and Sensors are far ahead of the other journals in growth rate and the number of articles published.

Growth trends of the 13 core sources from 2010 to 2021.
Additionally, the number of citations of articles published in SLEEP far exceeds that of the other journals, with a cumulative total of 497, as shown in Figure 5.

Top 10 most local cited sources.
Author of publication
According to Lotka's law, 34 the authors who publish more than 0.749 times the square root of the number of papers published by the most prolific scientists are top-authors. We defined authors with more than or equal to three publications as top-authors, and these authors represent 2.3% of all authors and produced 1/3 of all papers. In Table 2, Castillo-Escario Y, Ferrer-Lluis I, and Montserrat JM are among the most prolific authors with seven publications each.
Top authors ranking by the number of published articles.

A graph of the annual publication trends of the top-authors was drawn based on the annual publication data and annual citation frequency of the top-authors, as shown in Figure 6. The size of the circle indicates the annual publication volume and the shade of the color indicates the annual citation frequency. Half of the 22 top-authors were found to have focused on mHealth app-based sleep research after 2016 and have produced a steady output each year.

22 top authors’ production over the time (2010–2021).
Country and institution of publication
The 1399 authors come from 31 countries, and the top 10 countries with the most publications are shown in Figure 7. The USA produced the highest number of publications (53), followed by China, Korea, Australia, and Spain. The USA and China produced the highest number of articles through single-country publications and multiple-country publications.

Top 10 countries with the most publications.
The authors were recruited from 586 institutions. The top ten institutions in terms of a number of publications are in the order of Oxford University, University of California, Newcastle University, Arizona State University, New York University, Seoul National University, The University of Sydney, University of Pittsburgh, Harvard Medical School, and Institute for Bioengineering of Catalonia, shown in Figure 8.

Top 10 institutions with most publications.
The research institution collaboration network was plotted based on author institution data, as shown in Figure 9, from which most papers are produced by academic collaborations between domestic institutions or between domestic schools.

Institutions collaboration network.
Theme of publication
The themes of publications were analyzed from three aspects. First, high-frequency keywords were extracted from the abstracts of the included articles. The relationships between high-frequency keywords were analyzed through the high-frequency keyword co-occurrence network to identify the main research themes from the clustering results. Second, we used the thematic map method proposed by Cobo et al. 35 to cluster and map the themes according to density and centrality to explore the current research focus area. Finally, the trend of theme evolution in this field was analyzed from the time dimension.
First, a visual analysis of the high-frequency keyword co-occurrence networks was performed. The abstracts of the included articles were divided, deactivated, and lexically normalized using Python to obtain all keywords from the relevant studies. Then, the high-frequency keyword threshold was calculated according to the 80/20 rule, 36 and those with word frequencies seven times and above were identified as high-frequency keywords. The high-frequency keyword co-occurrence network was produced using VOS viewer, as shown in Figure 10. The high-frequency keywords were clustered into two categories: red and green. The red category represented traditional sleep disorder research with polysomnography, while the green category represented the new generation of sleep disorder research led by the mHealth apps.

High-frequency keyword co-occurrence networks.
The red category high-frequency words included the physiological indicators of interest (electroencephalography, heart rate, breath rate, etc.), the main targeted type of sleep disorders (sleep-disordered breathing, etc.), the main sleep-related indicators of interest (sleep stage, etc.), and the technology applied (deep learning, etc.). The green category high-frequency words included sleep-related indicators (sleep quality, sleep efficiency, etc.), the main targeted sleep disorders (insomnia, etc.), the main research and experimental methods (controlled study, randomized controlled trial, CBT, etc.), and other supporting research tools (questionnaires, etc.). We determined that a connection between the two categories exist, mainly in targeted sleep disorders, such as “sleep disorder breathing,” and the technologies applied, such as “artificial intelligence” and “actigraphy.”
Second, thematic map analysis was conducted. 2011, Cobo et al. 35 proposed the thematic map method using the quadrant in which the themes were in the thematic map to analyze the hotness and importance of the themes. The upper-right quadrant represents themes that are both well developed and important for structuring a research field. They are known as motor themes of the specialty, given that they present strong centrality and high density. The upper-left quadrant represents themes that have well-developed internal ties but unimportant external ties and are only marginally important to the field. The lower-left quadrant represents themes that are both weakly developed and marginal. The lower-right quadrant represents themes that are important for research but are not developed. The density and centrality of the co-word matrix were calculated, and the main categories of aggregation were separately placed into two-dimensional coordinates for visualization, as shown in Figure 11.

Thematic map in domain.
From the upper-right quadrant, we see that research for breathing-related sleep disorders has been well developed, but its importance is insufficient. From the upper-left quadrant, we see that sleep quality and CBT are current focus areas and are of high importance. From the lower-left quadrant, we see that sleep indicators such as total sleep time and sleep latency time are less important and not well developed. From the lower-right quadrant, we see the importance of staged sleep tracking using mobile apps that are currently poorly developed.
Finally, thematic evolution trend analysis was performed using co-word network analysis and clustering, incorporating the temporal dimension, to analyze the evolution of research themes from 2010 to 2021, as shown in Figure 12.

Sankey diagram of trends in the evolution of research themes from 2010 to 2021.
The results showed that, before 2015, researchers mainly focused on sleep apnea. In 2015, researchers began conducting studies on phased tracking of sleep. Between 2016 and 2018, researchers began to focus on approaches to treat sleep disorders, such as CBT. Simultaneously, researchers began utilizing methods such as machine learning to improve the accuracy of sleep tracking and began to design and develop user-oriented phone applications. Additionally, in 2019, new artificial intelligence techniques such as deep learning and neural networks were widely used by researchers and have gradually become powerful tools for sleep staging tracking and recording snoring sounds. Simultaneously, researchers began to design mobile phone applications based on CBT, and a number of pilot studies have been conducted based on these apps.
Product output
Based on studies by Aji et al. 28 and Du Jian et al., 32 we conducted a qualitative content analysis of the included articles with four dimensions: type, name, targeted sleep disorder, and function of the mHealth app.
Type and name of mHealth app
In this study, we classified mHealth apps into two categories by type: newly developed apps, which have been developed in-house by the authors’ research team, and existing apps, which have been licensed or downloaded for research purposes. In 313 included papers, researchers studied 368 sleep mHealth apps, comprising 233 new and 135 existing apps. Additionally, approximately 50% of the studies did not provide names, and the remaining articles studied 185 sleep mHealth apps that provided names, as shown in Figure 13. The CBT-I Coach37–42 is the most popular app, followed by SnoreLab and Calm.

Names of included sleep mHealth apps.
Function and targeted sleep disorder of mHealth app
We divided mHealth apps into three categories by function, including apps that focus on sleep disorder tracking, diagnosing sleep disorders, and intervening. Apps were classified by targeted sleep disorders according to the third edition of the ICSD. The results showed that tracking apps accounted for the largest proportion at 56.3% (207), followed by intervening apps (119) and diagnosing apps (42). A total of 275 Apps were explicitly mentioned for the targeted sleep disorders category. The number of apps for breathing-related sleep disorders (116) and insomnia sleep disorders (122) far exceeded others, while only one app supported the diagnosis of parasomnias.
Product application
We represented the product application based on the maturity levels of apps from I to IV. Level I refers to apps that exist only in a laboratory environment and have no real-world validation of their effectiveness or accuracy. Level II refers to apps that have single-center validation of their effectiveness or accuracy in a real-world environment. Level III refers to apps that have multi-center validation of their effectiveness or accuracy in a real-world environment. They are usually those products that have been upgraded iteratively, and their effectiveness or accuracy may have been validated multiple times. Level IV refers to apps that can be downloaded from application stores, that is, apps that are already used in the real world. We determined the maturity level of the apps from the article content and online information about the apps.
Our findings show that the number of products with Level IV and Level II maturity was the highest with 141 and 134 apps, respectively. While the number of products with Level III maturity was the lowest at 20 apps. Among them, 84.7% of the existing products reached maturity level IV, and 95.5% of the newly developed products reached maturity level II.
Research grants
Number, name, and affiliation of grants
Of the 313 included papers, 178 were supported by 323 grants from 319 different institutions, with a grant rate of 56.9% and an average of 1.8 grants per paper. While the most funded paper was supported by 14 grants from 6 institutions. The top ten institutions provided the highest number of grants, as shown in Figure 14.

Top 10 institutions that offered the most grants.
The National Institutes of Health (NIH) - USA provided the most grant support, with 47 grants over a 10-year period; 32 countries provided grant support, with the United States and China as the main funding countries.
Conversion rate of grants
We took inspiration from the research of Du jian et al. 32 to calculate the conversion rate of grants. Focusing on the proportion of those funded apps which eventually reach maturity level IV (i.e., already used in real world). The input–output triangles were then plotted, as shown in Figure 15.
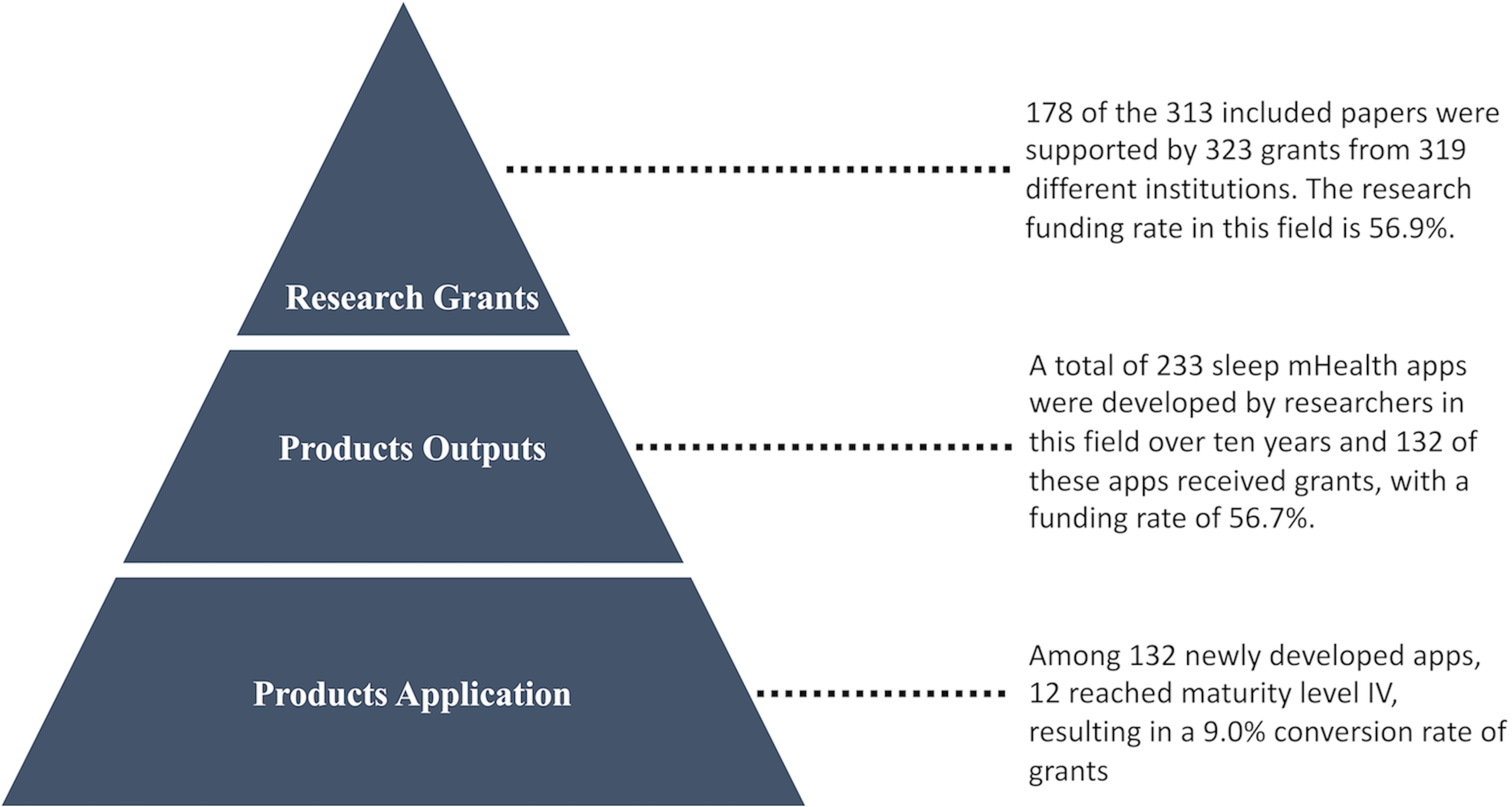
Grants input–output triangles.
As can be seen from the triangle diagram, 233 sleep mHealth apps were developed by researchers in this field over ten years; 132 of these apps received grants, with a funding rate of 56.7%. Only 12 of these apps reached maturity level IV, resulting in a 9.0% conversion rate of grants.
Discussion
Research status and trends
The number of published papers in the field of tracking, diagnosing, and intervening for sleep disorders using mHealth apps, has increased with an average annual growth rate of 41.6%. Particularly after 2017, with 66 papers published in 2021 (see Figure 3). The journals, in which these articles were included, were of moderate quality. However, the acceptance of these articles by top medical journals was disappointing; 84.5% of the research papers are recorded in the Web of Science core collection, an online index that covers core journal articles published in the physical and life sciences, health sciences, social sciences, and arts and humanities. The conference articles account for approximately 15.8%. The average impact factor of journals in the literature was 3.189, with the highest impact factor being Sleep Medicine Reviews (11.609). Most of the current research is published on Sensors and the IEEE Engineering in Medicine and Biology Society conference. With a combined total of 50 articles over ten years, representing 16.0% of the total (50/313). However, the acceptance of these articles by top medical journals is also poor. For example, there are no relevant papers published in The New England Journal of Medicine (NEJM), The Lancet, The Journal of the American Medical Association (JAMA), or British Medical Journal (BMJ).
Highly productive authors have a stable annual output but a short research duration. According to Lotka's law, 34 we found that 1/3 of the papers are produced by 22 top authors, and those authors have had consistent output over the last three years. The top three authors were particularly productive, generating two to three relevant papers per year (see Figure 6). Most of the top authors have entered this field in the last five years, and 12 of them are still conducting relevant research. This implies that the field is growing at a high and steady rate.
Most authors were from the USA and China, with 53 articles published by authors from both countries, accounting for 17% of the total number of articles (see Figure 7). Additionally, an analysis of research institutions publishing articles shows that there is a lack of international collaboration in the field, with most research being dominated by domestic inter-institutional or domestic institution-to-institutional collaborations.
The second quadrant of the thematic map (see Figure 12) includes CBT and sleep quality. Implying that the current research focus area is based on CBT and the use of sleep quality to assess the effectiveness of the intervention and is already well developed. This echoes the thematic evolution trend mulberry map (see Figure 12), that is, after 2016, researchers used CBT extensively for the treatment of sleep disorders and applied sleep indicators, such as sleep quality, to assess the effectiveness of the treatment.
Sleep staging tracking is a shortcoming in the field. However, with the adoption of new artificial intelligence techniques by researchers, this problem is likely to be addressed in the future. The fourth quadrant of the thematic map (see Figure 12) includes sleep tracking and sleep stages. This indicates the importance of relying on mobile apps for sleep staging tracking in this field. However, it is not well developed at this stage. According to our mulberry map of thematic evolution trends (see Figure 12), an increasing number of new artificial intelligence techniques, such as machine learning, deep learning, and neural networks, have been applied to mHealth apps over the last three years. This was to provide more accurate and consistent tracking of sleep and, in turn, more accurate diagnosis and effective treatment of sleep disorders. Therefore, mobile apps can be relied upon for the accurate phased tracking of sleep in future research.
Product output
Most products in this area are newly developed applications that functionally support the tracking and intervention of sleep disorders. Over the last decade, 368 sleep apps have been studied in 313 articles, including 233 newly developed and 135 existing sleep mHealth apps. The number of sleep tracking mHealth apps was the highest at 207, approximately 56.3% of the total, followed by intervening apps (119), while diagnosing apps were only 11.4% of the total (42). This may be related to the fact that diagnosing apps tend to have higher requirements for assistive devices. In sleep-related breathing disorders, for example, polysomnography is the only definitive way to obtain a diagnosis of sleep apnea. 43 However, it is difficult to achieve an accurate diagnosis of sleep apnea by relying solely on mobile phone sensors or wearable devices. Thus, the number of diagnostic apps that are available is low compared with other types of apps and sleep disorders were fairly underdiagnosed. 44 This is unfortunate since most sleep disorders can be successfully treated. 45
Among the 368 apps, 275 clearly indicated the targeted sleep disorders. Of these, the largest number of mHealth apps targeted insomnia disorders and sleep-related breathing disorders, accounting for approximately 86.5% of all apps, which is consistent with the results of our thematic analysis (see Figures 12 and 13). Contrarily, only one app focused on parasomnias. Although insomnia and sleep-related breathing disorders are the most common types of sleep disorders, 46 too much focus on these two types of sleep disorders is detrimental to the long-term development of the field, and greater attention should be paid to other types of sleep disorders.
Product application
Product applications are poor, with most of the newly developed apps not being used in the real world. A weak integration of theory and practice in the field is suggested by only 12 newly developed apps reaching maturity level IV. Although many sleep apps have been developed by experts over the last decade, most have only been used in the laboratory, without being applied in the real world. This may be attributed to other aspects of the apps, such as usability. The International Organization for Standardization defines usability as “the extent to which a system, product or service can be used by specified users to achieve specified goals with effectiveness, efficiency and satisfaction in a specified context of use.” 47 If researchers design an app with high usability, users will be more likely to continually use the app and even recommend it to peers.48–50
Grants and translation rate
The overall funding support rate for research in this area is moderate, with studies that developed new apps being favored by foundations, but the conversion rate is low. This is consistent with our analysis of product applications in this area, where most developed apps are not used in the real world.
The reason for this phenomenon, we are convinced that researchers may aim to produce sleep apps that can provide more accurate sleep monitoring services or more effective sleep intervention measures, for solving medical problems, rather than focus on their application in the real world. Then lead to most of these sleep apps only being used in the laboratory and the low conversion rate of research grants. For avoiding this situation and enabling mHealth sleep apps to be better used in the real world, we propose that researchers should pay more attention to translational research and applied research on sleep apps, then scientific research foundations should financially encourage such research on mHealth sleep apps.
Limitations
This review is subject to a few limitations. Firstly, we identified the maturity levels of apps from I to IV, based on the content of articles and information on the app store, which might cause bias, for example, we might omit some apps that have been removed from the app store. Secondly, our analysis only included articles in English, which made the analysis incomplete to some extent, but we included 313 individual papers, so there is reason to believe that the results of this study are sufficient to explore the status and trends of research, as well as identify the output and application of the sleep mHealth apps. Thirdly, we could not cite all articles included in our study, because of the amount of articles. However, all articles can be found based on our search formulas.
Conclusions
In the last decade, the field of tracking, diagnosing, and intervening in sleep disorders using mHealth apps has shown a trend of rapid development, with an increase in the number of publications annually. Studies using CBT to intervene in sleep and measure the effects of the intervention based on sleep quality, as well as studies focusing on insomnia and breathing-related sleep disorders, have made good progress and have some applications. However, the conversion rate of products from being funded and developed for use by end-users is low. In future research, new AI technologies should be used to address the shortcomings of staged sleep tracking, and researchers should focus on other sleep disorders. Simultaneously, research on other attributes of the apps, such as usability, needs to be strengthened. Efforts should be made to improve the research conversion rate of mHealth apps, to encourage widespread adoption and use in the real world.
Footnotes
Acknowledgments
The authors would like to thank the Beijing Municipal Natural Science Foundation, the National TCM innovation team and talent support projects, the National Natural Science Foundation of China, Zhejiang Provincial Natural Science Foundation of China for offering grants for this work.
Consent statement
All contributing authors of this manuscript have given the submission consent. In addition, patient consent is not necessary for this manuscript, as it is a review study, and the research data were collected from 313 studies of mHealth technology as a means of tracking, diagnosing, or intervening in sleep disorders.
Contributorship
Nuo, Fang, Wang, Han, and Lei participated in the study concept and design. Nuo and He collected and pre-processed the data. Nuo, Wang, Liang, and Lei participated in the acquisition, analysis, or interpretation of data. Liang and Lei obtained the funding for this work. Nuo drafted the manuscript. All authors critically revised the manuscript, as well as read and approved the final manuscript. Nuo and Lei had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
No ethical approval was needed for this type of study.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Beijing Municipal Natural Science Foundation [grant number 7222306]; National TCM innovation team and talent support projects [grant number ZYYCXTD-C-202210]; National Natural Science Foundation of China [grant number 81871455]; Zhejiang Provincial Natural Science Foundation of China [grant number LY22H180001].
Guarantor
JL.
Search formulas and results.

| Database | Search formulas | Result | Time |
|---|---|---|---|
| PubMed | (sleep[TIAB] OR insomnia[TIAB] OR snoring[TIAB] OR hypersomnia[TIAB] OR narcolepsy[TIAB] OR parasomnia[TIAB] OR somnambulism[TIAB] OR “sleep walking”[TIAB] OR “sleep talking”[TIAB] OR polysomnography[TIAB] OR “sleep difficult*"[TIAB] OR “sleep problems"[TIAB] OR “sleep disorders"[TIAB] OR “sleep disturbances"[TIAB] OR “sleep breathing disorders"[TIAB] OR “sleep apnea"[TIAB] OR “Kleine-Levin syndrome"[TIAB] OR “excessive daytime somnolence"[TIAB] OR “circadian rhythm sleep disorders"[TIAB] OR “REM sleep behavior disorder"[TIAB] OR “isolated sleep paralysis"[TIAB] OR “nightmare disorder"[TIAB] OR “sleep enuresis"[TIAB] OR “restless legs syndrome"[TIAB] OR “periodic limb movements during sleep"[TIAB] OR “sleep bruxism"[TIAB] OR “sleep myoclonus"[TIAB] OR insomnia[MeSH Terms] OR sleep apnea [MeSH Terms] OR narcolepsy[MeSH Terms] OR sleep disorder [MeSH Terms] OR Sleep Deprivation [MeSH Terms] OR Polysomnography [MeSH Terms]) AND (treat*[tiab] OR therap*[tiab] OR cure*[tiab] OR remedy*[tiab] OR intervention*[tiab] OR modif*[tiab] OR educat*[tiab] OR counsel*[tiab] OR manag*[tiab] OR CBT[tiab] OR control*[tiab] OR prevent*[tiab] OR diagnos*[tiab] OR identif*[tiab] OR judg*[tiab] OR track*[tiab] OR monitor*[tiab] OR supervis*[tiab] OR observe*[tiab]) AND (mHealth*[TIAB] OR m-health*[TIAB] OR mobile-health*[TIAB] OR smartphone*[TIAB] OR iPhone*[TIAB] OR android[TIAB] OR blackberry*[TIAB] OR cellphone*[TIAB] OR cell phone*[TIAB] OR cellular phone*[TIAB] OR mobile phone*[TIAB] OR mobile App*[TIAB] OR mobile device*[TIAB] OR mobile echnolog*[TIAB] OR tablet computer*[TIAB] OR mobile tablet*[TIAB] OR electronic tablet*[TIAB] OR tablet PC[TIAB] OR iPad*[TIAB] OR iPod*[TIAB] OR wearable technolog*[TIAB] OR consumer wearable*[TIAB] OR sleep tracker* OR sleep monitor*[TIAB] OR activity trackers[TIAB] OR fitbit[TIAB] OR smart watch[TIAB] OR smartwatch[TIAB] OR cell phones[MeSH:noexp] OR mobile Applications[MeSH] OR computer, handheld[MeSH] OR smartphone[MeSH] OR consumer health informatics[MeSH]) | 2411 | 2022.1.1 |
| WOS core collection | TS = (sleep OR insomnia OR snoring OR hypersomnia OR narcolepsy OR parasomnia OR somnambulism OR “sleep walking” OR “sleep talking” OR polysomnography OR “sleep difficult*” OR “sleep problems” OR “sleep disorders” OR “sleep disturbances” OR “sleep breathing disorders” OR “sleep apnea” OR “Kleine-Levin syndrome” OR “excessive daytime somnolence” OR “circadian rhythm sleep disorders” OR “REM sleep behavior disorder” OR “isolated sleep paralysis” OR “nightmare disorder” OR “sleep enuresis” OR “restless legs syndrome” OR “periodic limb movements during sleep” OR “sleep bruxism” OR “sleep myoclonus”) AND TS = (treat* OR therap* OR cure* OR remedy* OR intervention* OR educat* OR counsel*OR manag* OR CBT OR control* OR prevent* OR diagnos* OR identif* OR judg* OR track* OR monitor* OR supervis* OR observe*) AND TS = (mHealth* OR m-health* OR mobile-health* OR smartphone* OR iPhone* OR android OR blackberry OR cellphone* OR cell phone* OR cellular phone* OR mobile phone* OR mobile App* OR mobile device* OR mobile echnolog* OR tablet PC OR iPad* OR iPod* OR wearable technolog* OR consumer wearable* OR fitbit) | 2917 | 2022.1.1 |
| Scopus | (TITLE-ABS-KEY (sleep) OR TITLE-ABS-KEY (insomnia) OR TITLE-ABS-KEY (snoring) OR TITLE-ABS-KEY (hypersomnia) OR TITLE-ABS-KEY (narcolepsy) OR TITLE-ABS-KEY (parasomnia) OR TITLE-ABS-KEY (somnambulism) OR TITLE-ABS-KEY (“sleep walking”) OR TITLE-ABS-KEY (“sleep talking”) OR TITLE-ABS-KEY (polysomnography) OR TITLE-ABS-KEY (“sleep difficult*”) OR TITLE-ABS-KEY (“sleep problems”) OR TITLE-ABS-KEY (“sleep disorders”) OR TITLE-ABS-KEY (“sleep disturbances”) OR TITLE-ABS-KEY (“sleep breathing disorders”) OR TITLE-ABS-KEY (“sleep apnea”) OR TITLE-ABS-KEY (“Kleine-Levin syndrome”) OR TITLE-ABS-KEY (“excessive daytime somnolence”) OR TITLE-ABS-KEY (“circadian rhythm sleep disorders”) OR TITLE-ABS-KEY (“REM sleep behavior disorder”) OR TITLE-ABS-KEY (“isolated sleep paralysis”) OR TITLE-ABS-KEY (“nightmare disorder”) OR TITLE-ABS-KEY (“sleep enuresis”) OR TITLE-ABS-KEY (“restless legs syndrome”) OR TITLE-ABS-KEY (“periodic limb movements during sleep”) OR TITLE-ABS-KEY (“sleep bruxism”) OR TITLE-ABS-KEY (“sleep myoclonus”)) AND (TITLE-ABS-KEY (treat*) OR TITLE-ABS-KEY (therap*) OR TITLE-ABS-KEY (cure*) OR TITLE-ABS-KEY (remedy*) OR TITLE-ABS-KEY (intervention*) OR TITLE-ABS-KEY (educat*) OR TITLE-ABS-KEY (counsel*) OR TITLE-ABS-KEY (manag*) OR TITLE-ABS-KEY (CBT) OR TITLE-ABS-KEY (control*) OR TITLE-ABS-KEY (prevent*) OR TITLE-ABS-KEY (diagnos*) OR TITLE-ABS-KEY (identif*) OR TITLE-ABS-KEY (judg*) OR TITLE-ABS-KEY (track*) OR TITLE-ABS-KEY (monitor*) OR TITLE-ABS-KEY (supervis*) OR TITLE-ABS-KEY (observe*)) AND (TITLE-ABS-KEY (mhealth*) OR TITLE-ABS-KEY (m-health*) OR TITLE-ABS-KEY (mobile-health*) OR TITLE-ABS-KEY (smartphone*) OR TITLE-ABS-KEY (iphone*) OR TITLE-ABS-KEY (android) OR TITLE-ABS-KEY (blackberry) OR TITLE-ABS-KEY (cell?phone*) OR TITLE-ABS-KEY (cellular?phone*) OR TITLE-ABS-KEY (mobile?phone*) OR TITLE-ABS-KEY (mobile?App*) OR TITLE-ABS-KEY (mobile?device*) OR TITLE-ABS-KEY (mobile?echnolog*) OR TITLE-ABS-KEY (tablet?computer*) OR TITLE-ABS-KEY (mobile?tablet*) OR TITLE-ABS-KEY (electronic?tablet*) OR TITLE-ABS-KEY (tablet?pc) OR TITLE-ABS-KEY (ipad*) OR TITLE-ABS-KEY (ipod*) OR TITLE-ABS-KEY (wearable?technolog*) OR TITLE-ABS-KEY (consumer?wearable*) OR TITLE-ABS-KEY (sleep?trackers) OR TITLE-ABS-KEY (sleep?monitor*) OR TITLE-ABS-KEY (fitbit) OR TITLE-ABS-KEY (smart?watch)) | 1929 | 2022.1.1 |
| embase | (‘sleep':ab OR ‘insomnia':ab OR ‘snoring':ab OR ‘hypersomnia':ab OR ‘narcolepsy':ab OR ‘parasomnia':ab OR ‘somnambulism':ab OR ‘sleep walking':ab OR ‘sleep talking':ab OR ‘polysomnography':ab OR ‘sleep difficult*':ab OR ‘sleep problems':ab OR ‘sleep disorders':ab OR ‘sleep disturbances':ab OR ‘sleep breathing disorders':ab OR ‘sleep apnea':ab OR ‘kleine-levin syndrome':ab OR ‘excessive daytime somnolence':ab OR ‘circadian rhythm sleep disorders':ab OR ‘rem sleep behavior disorder':ab OR ‘isolated sleep paralysis':ab OR ‘nightmare disorder':ab OR ‘sleep enuresis':ab OR ‘restless legs syndrome':ab OR ‘periodic limb movements during sleep':ab OR ‘sleep bruxism':ab OR ‘sleep myoclonus':ab) AND (treat*:ab OR therap*:ab OR cure*:ab OR remedy*:ab OR intervention*:ab OR educat*:ab OR counsel*:ab OR manag*:ab OR CBT OR control*:ab OR prevent*:ab OR diagnos*:ab OR identif*:ab OR judg*:ab OR track*:ab OR monitor*:ab OR supervis*:ab OR observe*:ab) AND ((‘mhealth*':ab OR ‘m-health*':ab OR ‘mobile health*':ab OR ‘smartphone*':ab OR ‘iphone*':ab OR ‘android':ab OR ‘blackberry':ab OR ‘cellphone*':ab OR cell) AND phone*:ab OR ‘cellular phone*':ab OR ‘mobile phone*':ab OR ‘mobile App*':ab OR ‘mobile device*':ab OR ‘mobile echnolog*':ab OR ‘tablet computer*':ab OR ‘mobile tablet*':ab OR ‘electronic tablet*':ab OR ‘ipod*':ab OR ‘wearable technolog*':ab OR ‘consumer wearable*':ab OR ‘commercial wearable*':ab OR ‘smart watch':ab OR ‘smartwatch':ab OR ‘sleep trackers':ab OR ‘sleep monito*':ab) | 2354 | 2022.1.1 |
| CINAHL | AB(sleep OR insomnia OR snoring OR hypersomnia OR narcolepsy OR parasomnia OR somnambulism OR “sleep walking” OR “sleep talking” OR polysomnography OR “sleep difficult*” OR “sleep problems” OR “sleep disorders” OR “sleep disturbances” OR “sleep breathing disorders” OR “sleep apnea” OR “Kleine-Levin syndrome” OR “excessive daytime somnolence” OR “circadian rhythm sleep disorders” OR “REM sleep behavior disorder” OR “isolated sleep paralysis” OR “nightmare disorder” OR “sleep enuresis” OR “restless legs syndrome” OR “periodic limb movements during sleep” OR “sleep bruxism” OR “sleep myoclonus”) AND AB (treat* OR therap* OR cure* OR remedy* OR intervention* OR educat* OR counsel*OR manag* OR CBT OR control* OR prevent* OR diagnos* OR identif* OR judg* OR track* OR monitor* OR supervis* OR observe*) AND AB (mHealth* OR m-health* OR mobile-health* OR smartphone* OR iPhone* OR android OR blackberry OR cellphone* OR cell phone* OR cellular phone* OR mobile phone* OR mobile App* OR mobile device* OR mobile echnolog* OR tablet computer* OR mobile tablet* OR electronic tablet* OR tablet PC OR iPad* OR iPod* OR wearable technolog* OR consumer wearable* OR sleep track* OR sleep monitor* OR activity trackers OR smart watch) | 1393 | 2022.1.1 |
| APA PsycInfo | AB(sleep OR insomnia OR snoring OR hypersomnia OR narcolepsy OR parasomnia OR somnambulism OR “sleep walking” OR “sleep talking” OR polysomnography OR “sleep difficult*” OR “sleep problems” OR “sleep disorders” OR “sleep disturbances” OR “sleep breathing disorders” OR “sleep apnea” OR “Kleine-Levin syndrome” OR “excessive daytime somnolence” OR “circadian rhythm sleep disorders” OR “REM sleep behavior disorder” OR “isolated sleep paralysis” OR “nightmare disorder” OR “sleep enuresis” OR “restless legs syndrome” OR “periodic limb movements during sleep” OR “sleep bruxism” OR “sleep myoclonus”) AND AB (treat* OR therap* OR cure* OR remedy* OR intervention* OR educat* OR counsel*OR manag* OR CBT OR control* OR prevent* OR diagnos* OR identif* OR judg* OR track* OR monitor* OR supervis* OR observe*) AND AB (mHealth* OR m-health* OR mobile-health* OR smartphone* OR iPhone* OR android OR blackberry OR cellphone* OR cell phone* OR cellular phone* OR mobile phone* OR mobile App* OR mobile device* OR mobile echnolog* OR tablet computer* OR mobile tablet* OR electronic tablet* OR tablet PC OR iPad* OR iPod* OR wearable technolog* OR consumer wearable* OR sleep track* OR sleep monitor* OR activity trackers OR smart watch) | 1783 | 2022.1.1 |
| Psychology and Behavioral Sciences Collection | AB(sleep OR insomnia OR snoring OR hypersomnia OR narcolepsy OR parasomnia OR somnambulism OR “sleep walking” OR “sleep talking” OR polysomnography OR “sleep difficult*” OR “sleep problems” OR “sleep disorders” OR “sleep disturbances” OR “sleep breathing disorders” OR “sleep apnea” OR “Kleine-Levin syndrome” OR “excessive daytime somnolence” OR “circadian rhythm sleep disorders” OR “REM sleep behavior disorder” OR “isolated sleep paralysis” OR “nightmare disorder” OR “sleep enuresis” OR “restless legs syndrome” OR “periodic limb movements during sleep” OR “sleep bruxism” OR “sleep myoclonus”) AND AB (treat* OR therap* OR cure* OR remedy* OR intervention* OR educat* OR counsel*OR manag* OR CBT OR control* OR prevent* OR diagnos* OR identif* OR judg* OR track* OR monitor* OR supervis* OR observe*) AND AB (mHealth* OR m-health* OR mobile-health* OR smartphone* OR iPhone* OR android OR blackberry OR cellphone* OR cell phone* OR cellular phone* OR mobile phone* OR mobile App* OR mobile device* OR mobile echnolog* OR tablet computer* OR mobile tablet* OR electronic tablet* OR tablet PC OR iPad* OR iPod* OR wearable technolog* OR consumer wearable* OR sleep track* OR sleep monitor* OR activity trackers OR smart watch) | 263 | 2022.1.1 |
| APA PsycArticles | AB(sleep OR insomnia OR snoring OR hypersomnia OR narcolepsy OR parasomnia OR somnambulism OR “sleep walking” OR “sleep talking” OR polysomnography OR “sleep difficult*” OR “sleep problems” OR “sleep disorders” OR “sleep disturbances” OR “sleep breathing disorders” OR “sleep apnea” OR “Kleine-Levin syndrome” OR “excessive daytime somnolence” OR “circadian rhythm sleep disorders” OR “REM sleep behavior disorder” OR “isolated sleep paralysis” OR “nightmare disorder” OR “sleep enuresis” OR “restless legs syndrome” OR “periodic limb movements during sleep” OR “sleep bruxism” OR “sleep myoclonus”) AND AB (treat* OR therap* OR cure* OR remedy* OR intervention* OR educat* OR counsel*OR manag* OR CBT OR control* OR prevent* OR diagnos* OR identif* OR judg* OR track* OR monitor* OR supervis* OR observe*) AND AB (mHealth* OR m-health* OR mobile-health* OR smartphone* OR iPhone* OR android OR blackberry OR cellphone* OR cell phone* OR cellular phone* OR mobile phone* OR mobile App* OR mobile device* OR mobile echnolog* OR tablet computer* OR mobile tablet* OR electronic tablet* OR tablet PC OR iPad* OR iPod* OR wearable technolog* OR consumer wearable* OR sleep track* OR sleep monitor* OR activity trackers OR smart watch) | 46 | 2022.1.1 |
