Abstract
Objectives
Evidence-based smoking cessation support tools (EBSTs) can double the quitting chances, but uptake among smokers is low. A digital decision aid (DA) could help smokers choose an EBST in concordance with their values and preferences, but it is unclear which type of smokers are interested in a digital DA. We hypothesized that smokers’ general decision-making style (GDMS) could be used to identify early adopters. This study therefore aimed to identify smoker profiles based on smokers’ GDMS and investigate these profiles’ association with intention to use a digital DA.
Design
A cross-sectional dataset (N = 200 smokers intending to quit) was used to perform a hierarchical cluster analysis based on smokers’ GDMS scores.
Methods
Clusters were compared on demographic and socio-cognitive variables. Mediation analyses were conducted to see if the relationship between cluster membership and intention was mediated through socio-cognitive variables (e.g., attitude).
Results
Two clusters were identified;
Conclusions
The GDMS can be used to identify smokers who are interested in a digital DA early on. As such, the GDMS can be used to tailor recruitment and DA content.
Keywords
Tobacco smoking continues to be the leading cause of preventable diseases and premature death. 1 It is estimated that 16% of all deaths in Europe and the Americas can be attributed to smoking. 2 In the Netherlands, smoking-related mortality is even higher (21%). 2 Evidence-based smoking cessation support tools (EBSTs) have been shown to be effective in facilitating quitting and maintaining smoking abstinence, i.e., pharmacotherapy, such as nicotine replacement therapy (NRT) 3 ; and behavioral support, such as counselling by health professionals. 4 Such EBSTs more than double successful cessation rates, 5 but are severely underused 6 and in the Netherlands uptake of non-evidence based support tools (e.g., acupuncture) is only slightly below that of EBSTs. 7 EBST uptake could therefore be significantly improved.
However, even if smokers are interested in using an EBST, they still have to choose between all the different EBSTs. It is known that individuals that face health-related decisions often encounter uncertainty about what to choose, which can result in a feeling of discomfort.8,9 Offering a decision support system (often called decision aid, DA) to smokers that helps them choose from the multitude of options could help reduce this discomfort.
10
DAs are specifically designed to facilitate informed decision making between different health-care options, by providing information and helping users to define their own values and preferences regarding these different options.10,11 Nowadays, many DAs are delivered online as this allows for a broad and sustainable dissemination.12–14 DAs have been used a lot concerning treatment or screening decisions,
10
and have in a few instances also been used for smoking cessation.
15
For example, Willemsen et al.
7
developed a paper-based DA, which was effective in promoting quitting attempts and abstinence. However, it failed to increase uptake of EBSTs and resulted in higher drop-out rates compared to the control group. Early drop-out may cause problems for smokers, as they will not benefit from the intervention,
16
and for researchers, as this makes it difficult to evaluate the effects.
17
Designing a digital DA instead of a paper-based DA could potentially already reach more people
12
and,
Methods
A cross-sectional study was conducted in January 2018. Participants were recruited through the internet research agency Flycatcher. 33 Panel members were preselected, based on their smoking status and if they were planning to stop smoking within six months. All preselected participants received an online questionnaire that lasted an average of 15.5 minutes. The questionnaire included an informed consent form, information about EBSTs and information about DAs in general. Participants were excluded if they were younger than 18, did not provide informed consent, or were not planning to quit smoking within six months. In total 250 smokers were invited. Due to the explorative nature of this study, no power analysis has been performed. Therefore, the sample size was based on the experience of the research team. Participants received €1.40 from the internet research agency to complete the questionnaire, which would equal about $1,54.
Measurements
A Dutch questionnaire was developed and pretested among eight experts and five (ex-)smokers. Pretesting took place with both native and second language Dutch speakers. If possible, validated scales were used that had been used in a Dutch context before. If this was not possible, English validated scales were initially translated by professional translators (forward translation), followed by back-translation by the research team (backward translation). 34
Demographics
Gender identity (0 = woman; 1 = man; 2 = other) and country of birth were measured with one question each, age was measured continuously. Education was measured via three questions. The first question was asked to identify which degree had already been awarded, the second question was asked to identify respondents who were currently enrolled in a degree granting program (0 = no; 1 = yes) and the third to identify which degree granting program they are currently following. Three variables were later transformed: country of origin (0 = Dutch, 1 = Non-Dutch), first and last educational question (0 = low; 1 = medium; 2 = high). No, primary and vocational education were regarded as a low educational attainment; secondary vocational education and a high school degree were regarded as a medium educational attainment and higher vocational education, college and university degrees were regarded as high educational attainment.
Smoking behavior and smoking-related cognitions
Smoking behavior assessment was based on the Dutch version of the Fagerström test for nicotine dependence.35,36 However, it was adapted to include all smoking behavior, e.g., the original “How soon after you wake up do you smoke your first cigarette?” was changed to “How soon after you wake up do you smoke?” to reflect that not all smokers smoke cigarettes. Vapers (i.e., e-cigarette users) were considered smokers for this study, which was reflected in all measuring instruments, as e-cigarettes are not treated as EBSTs in the Netherlands. The Fagerström test for nicotine dependence had a sufficient level of internal consistency within our sample (α = 0.75). Additionally, used nicotine products (“Which products do you smoke regularly? Multiple answers are possible.”, 0 = cigarette; 1 = hand-rolled cigarette; 2 = e-cigarette; 3 = pipe; 4 = other product) as well as previous cessation attempts (e.g., “How many times have you made a serious quit attempt? By this we mean that you have not smoked for at least 24 hours.”, could be answered on a continuous scale) were examined with four questions based on Mudde et al.
37
as common in Dutch studies focused on tobacco use/smoking (e.g.,
36
Decision-related cognitions
A modified version of the general decision-making style (GDMS) questionnaire22–24 was used to assess respondents’ decision-making styles in order to perform a hierarchical cluster analysis. The modified version included questions to measure the regret style mentioned in the introduction. Thus, the scale consists of six subscales each measuring a decision-making style: rational (α = 0.70), intuitive (α = 0.77), dependent (α = 0.81), avoidant (α = 0.86), spontaneous (α = 0.67), and regret (α = 0.79). Answering categories were given on a 5-point scale, ranging from 1 =“strongly disagree” to 5 =“strongly agree”.
Other cognitions
The treatment self-regulation questionnaire (TSRQ) was used to assess the degree to which respondents’ motivation for a future cessation attempt is relatively autonomous (autonomous-regulated style) or determined by external control (controlled-regulated style). 39 The scale consisted of two scales; one measuring the autonomous-regulated style (1 = not at all true, 7 = very true; α = 0.87), one the controlled-regulated style (1 = not at all true, 7 = very true; α = 0.76). Secondly, the perceived competence scale (PCS) 40 was used to measure how confident respondents felt in their ability to quit smoking 41 (1 = not at all true, 7 = very true; α = 0.90). Thirdly, the health care climate questionnaire (HCCQ), 40 was used to capture respondents’ perceptions of the degree to which their health care providers were autonomy-supportive regarding smoking cessation (1 = not at all true, 7 = very true; α = 0.92), i.e., whether they support behaviors that their patients want to do of their own volition. The HCCQ was only administered to respondents that had contact with a health-care professional in the past 12 months.
To assess health locus of control, the multidimensional health locus of control scale (MHLC) was applied to measure the extent to which people believed that they, their physician, or chance have direct control over their own health.26,42 The Dutch version of the MHLC consists of three subscales: internal health locus of control (ILOC; α = 0.77), physicians’ health locus of control (PLOC; α = 0.78) and chance health locus of control (CLOC; α = 0.76). Answering categories were given on 6-point scales as originally validated, ranging from 1 =“strongly disagree” to 6 =“strongly agree”. 26
Finally, we measured intention to use an EBST DA via three items by asking the respondents whether a hypothetical DA would be used if it was available using a 7-point scale (α = 0.96), e.g., “I want to use an online DA during a next quit attempt (if available).”
Statistical analysis
All analyses were conducted using SPSS 24.0, 43 p-values lower than 0.05 were considered significant. Firstly, descriptive analyses were conducted to assess sample characteristics. Secondly, cluster analyses were performed based on the GDMS subscales. Ward’s hierarchical method with Euclidean distance as metric distance was used as clustering algorithm with GDMS scores standardized into z-scores. 44 Multiple methods were employed to investigate the number of clusters within the sample: (1) cluster profiles were visually inspected to assess shape, level, scatter, and interpretability; (2) inverse scree tests were employed to indicate the optimal number of clusters; and (3) analyses were replicated within three random subsamples to investigate the stability of the cluster solutions.25,45
Thirdly, identified clusters were externally validated by comparing them on all measured variables using Mann-Whitney U tests, Kruskal-Wallis H tests or chi-squared tests. For this (and all other analyses that follow) we created a new variable named “cluster membership” based on the cluster analysis described above. Nonparametric tests were used as most variables showed heterogeneity of variance and a substantial number of outliers. For categorical variables chi-square tests were conducted.
Fourthly, we investigated whether cluster membership was associated with intention to use a DA (main outcome variable) by conducting both a simple linear regression (unadjusted) and multiple linear regression (adjusted for other psychological constructs). As no previous studies have investigated the topic at hand before, variables were added to the adjusted model if their respective theoretical backgrounds (e.g., SDT) linked them to decision making and if they were statistically significantly associated with both intention (main outcome variable) and cluster membership (independent variable). A log transformation was applied to the scale measuring the controlled regulated style to not violate the linearity assumption.
Fifthly, mediation analyses were conducted post hoc with the technique as described by Preacher and Hayes 46 to test for possible mediation to explain the results from the linear regressions. Testing took place for all variables that clusters significantly differed on and/or appeared to be significant in the previous regressions. We tested each possible mediator separately. Results were interpreted using bootstrapped analyses. 46 As we carried out these mediation analyses in order to better understand the results from the analyses that were planned a priori, they do not correspond to any of the RQs mentioned in the introduction.
Results
Of the 250 invited smokers, 200 completed the questionnaire and provided informed consent (response rate = 80%). Table 1 displays all sample characteristics.
Sample characteristics.
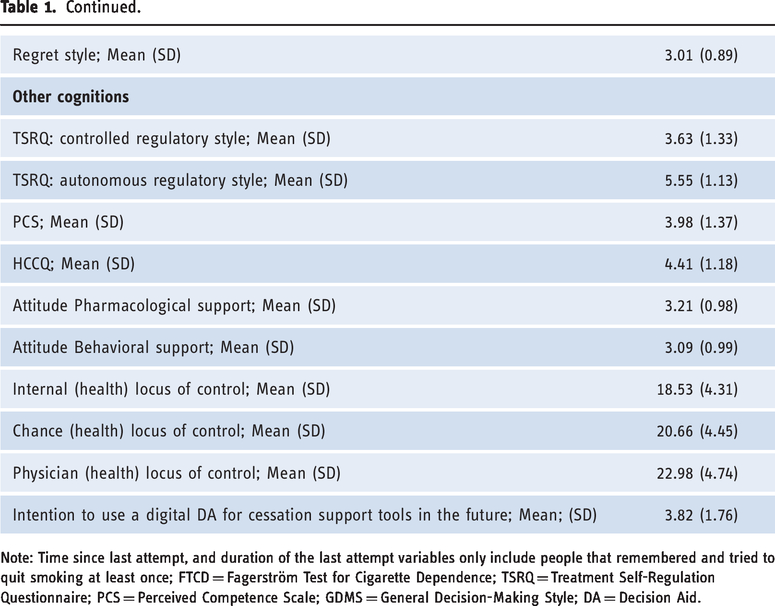
Note: Time since last attempt, and duration of the last attempt variables only include people that remembered and tried to quit smoking at least once; FTCD = Fagerström Test for Cigarette Dependence; TSRQ = Treatment Self-Regulation Questionnaire; PCS = Perceived Competence Scale; GDMS = General Decision-Making Style; DA = Decision Aid.
Cluster analysis
Visual inspection of both the whole and random subsamples’ dendrograms indicated that two clusters were formed, but that those two clusters seemed to split into smaller clusters. Inverse scree tests indicated that the two-cluster solution was best supported by the data, while both the three- and four-cluster-solution seemed feasible. In all three possible solutions, participants differed significantly on most of the GDMS subscales. Comparing the cluster analysis of the whole sample to the cluster analyses of the subsamples showed that clusters replicated most consistently in the two-cluster solution. Based on all available tests, we therefore selected the two-cluster solution for further analysis.
External validation
The two clusters differed statistically significantly on all of the clustering variables except the rational style. Respondents in cluster 1 (n = 134) indicated that they were more avoidant, dependent and regretful in or after decision-making situations, while respondents in cluster 2 (n = 66) reported a greater tendency to be spontaneous and intuitive. Therefore, cluster 1 was termed
Cluster characteristics.
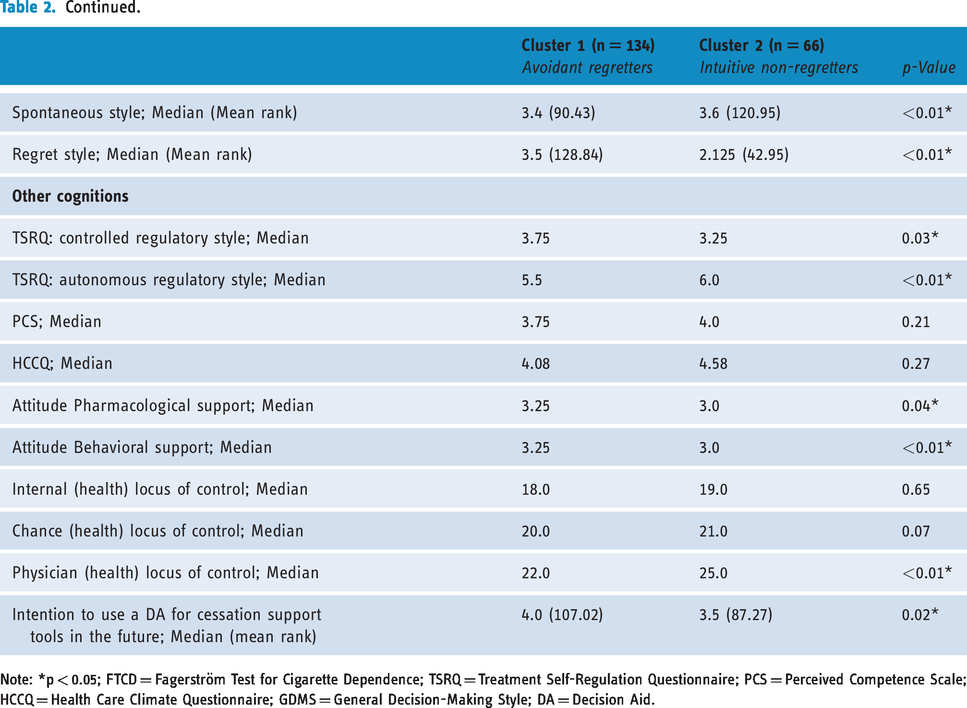
Note: *p < 0.05; FTCD = Fagerström Test for Cigarette Dependence; TSRQ = Treatment Self-Regulation Questionnaire; PCS = Perceived Competence Scale; HCCQ = Health Care Climate Questionnaire; GDMS = General Decision-Making Style; DA = Decision Aid.
Direct effects of cluster membership
Cluster membership (i.e., if participant belonged to either the
Multiple linear regression identifying determinants of intention to use an EBST DA.

Note: *p < 0.05; B = unstandardized regression coefficient; SE = Standard error of the coefficient; β = standardized coefficient; DA = Decision Aid; TSRQ = Treatment Self-Regulation Questionnaire.
Indirect effects of cluster membership
Indications were found that attitude and the controlled regulatory style seemed to fully mediate the effect of cluster membership, while the autonomous regulatory style seemed to mediate the effect only partially. No such indications were found for the internal and physician locus of control scales. Table 4 shows the results of the mediation analyses.
Mediation analyses.

Note: *p<0.05; IV = Cluster Membership; DV = Dependent variable; M = Behavioral Attitude, Pharmacological Attitude, Internal locus of control, Physician locus of control, Controlled regulatory style, Autonomous regulatory style.
Discussion
In this study, it was investigated if clusters of smokers could be identified based on their decision-making styles and how those clusters differed to identify people that were interested in a digital DA for EBSTs.
Two distinct clusters were identified. “
Additionally, it was found that “
On the other hand,
Based on the aforementioned findings it could be argued that both clusters could be targeted with a digital DA developed to facilitate choosing an EBST, but that it might be smart to tailor either both the DA itself and/or the recruitment strategy to smokers’ cluster membership. For example, advertisements for the EBST DA could highlight that DAs have been proven to reduce decisional regret. This would probably be especially appealing for “
While the results of the multivariable regression indicate that the differences in intention may be explained by other variables than cluster membership (such as attitude), mediation analyses show that there is a possibility that the effect of cluster membership on intention is in fact mediated through said variables. While this has not been tested before, this is in line with integrated models that are used to predict behavior (change) in contemporary behavioral science.51,52 Those models commonly state that personality characteristics are one of the most distal variables that influence behavior, (partly) mediated through other socio-cognitions. This possibly suggests that belonging to a particular group of decision makers has an impact on socio-cognitions, which in turn influences one’s intention to use a DA.
Implications for future research
Since our study was explorative in nature and could rather be described as hypothesis-generating (as opposed to hypothesis-testing), efforts should be made to test whether the identified results can be replicated. Ideally, to this end researchers should use a longitudinal design, as our post-hoc results indicate a mediation path may exist from decision-making styles through socio-cognitive variables (e.g., attitude) to intention to use a digital DA. Given the cross-sectional nature of our study, we were unfortunately unable to confirm this mediation path based on the data collected. In view of the so-called “intention-behavior gap”,
53
it would also be particularly interesting to test whether the identified paths also apply to the actual uptake of a digital DA and not only to the intention to do so. In the discussion we also highlighted a number of ways in which our results can be used to inform either the recruitment of DA participants (e.g., in recruitment materials it could be highlighted that DAs are known to reduce regret) or the (digital) DA design itself (e.g., by including intuitive elements). Researchers could investigate whether suggested recruitment strategies and potential improving alterations to the DA have positive effects (e.g., on DA uptake or on the quality of the decision-making process
54
) and how these effects relate to decision-making styles – e.g., based on our results, one could assume that highlighting regret-reducing in recruitment materials would be especially attractive and effective for
Strength and limitations
This study was mainly limited due to its cross-sectional and explorative nature. As conclusions regarding causality cannot be drawn based on our cross-sectional data, findings should be confirmed by longitudinal data (see also
Conclusion
Our explorative study has shown that it is indeed possible to identify smoker clusters based on their decision-making styles and that cluster membership has at least some impact on smokers’ intention to use a digital EBSTs DA. Future studies in the field of digital DAs would therefore benefit from including decision-making style in their design, and it would be interesting to see if our findings could be replicated in longitudinal studies. In addition, it would be interesting to see how decision-making style could be used in digital DA development, as well as recruitment of participants for a study on digital DA effectiveness. Practitioners and developers of digital DAs might use our findings to initially tailor their recruitment strategies and identify early adopters, who might be able to contribute to the development of more attractive interventions that are ultimately appealing for smokers from all adopter categories.
Footnotes
Acknowledgements
The authors wish to thank Mr. Martijn Stroom, MSc, who contributed to the first draft of the questionnaire.
Contributorship
ES, CD and CH designed the study, wrote the protocol and provided feedback on all steps. RH contributed to all practical steps, such as questionnaire development and translation. TG conducted literature searches, developed the questionnaire, conducted all statistical analyses and wrote the first draft of the manuscript. All authors contributed to the manuscript and approved its final version.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The study was assessed by the Medical Ethics Committee Zuyderland, the Netherlands (16-N-227). According to this committee, the study did not fall under the scope of the Medical Research Involving Human Subjects Act.
Funding
Financial support for this study was provided entirely by a grant from the Dutch Cancer Society (UM2015-7744). The funding agreement ensured the authors’ independence in designing the study, interpreting the data, writing, and publishing the report.
Guarantor
CH.
Peer review
Dorothy Szinay, University of East Anglia has reviewed this manuscript.
