Abstract
The concept of quality has moved to the top of the international healthcare agenda in the past 30 years. This has been driven by a growing awareness of the scale of variation in patient outcomes, influenced by both the paucity of and consistency in implementation of evidence-based actions or interventions performed during the delivery of patient care. Concurrently there has been growing interest on the part of healthcare professionals to use a wider range of knowledge and available techniques, from outside of medicine, to continuously improve standards of safe and effective patient care. This is the first in a series of three articles introducing Quality Improvement (QI) methodology and supporting concepts to multidisciplinary teams working in Urology departments in the United Kingdom. We start, in this article, by providing an overview of key QI principles and their industrial roots; we position QI in the context of other approaches to improvement, such as audit, and we outline the key organisations and infrastructure supporting QI work on the ground.
What is quality in healthcare?
What constitutes ‘quality’ in the context of healthcare provision is likely very different depending on who you ask. For patients it might relate to how quickly an appointment can be secured, the ease of communication or the outcome of a procedure; for clinicians perhaps it has more to do with access to state of the art equipment, dependable resources and decreasing risk; for the manager or commissioner, improving patient flow and the meeting of performance targets may be a greater consideration.
Within healthcare there is no universally accepted definition of ‘quality’, but those commonly used pick up on this multi-dimensionality. The following popular definition, from the US Institute of Medicine and also used by the World Health Organization, describes quality as ‘the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge’.1,2 It identifies six dimensions of quality, stating that healthcare must be:
These dimensions are a product of both the wider health systems environment and the actions of providers and individuals working within the system. In the United Kingdom’s National Health Service (NHS), they underpin a shared vision and commitment to delivering quality care on behalf of multiple stakeholders within the system, each with a different function, including commissioners, staff, providers, regulators, research and innovation partners and patients and communities. 3 (The specific roles of some of these bodies are discussed further later on.)
QI: definition and background
Alongside the recognition of what constitutes high-quality care has been the quest to understand how best to go about improving quality. We now know that to make the best use of available resources, to prevent the occurrence and recurrence of system failures, and to achieve excellence in care delivery requires continuous improvement of healthcare processes in a manner that is systematic and sustainable.4,5
QI approaches were introduced into healthcare following several decades of development and applications in other industries – most notably the manufacturing industry. QI approaches used in healthcare today date back almost 100 years and are often identified with Walter Shewhart, William Edwards Deming and Joseph Juran (and more latterly in healthcare Don Berwick), who all worked to quality assure industrial manufacturing processes through the use of standardised tools and measurements6–15 (Box 1).
Pioneers of Quality Improvement.

QI: Quality Improvement.
These practical approaches to improvement coalesced around the turn of the 21st century into what is now termed ‘Improvement Science’ in healthcare, which has emerged as a burgeoning science in its own right. While the terms QI and Improvement Science are often used interchangeably, there is an important distinction between the two. QI refers to practical efforts to make changes to healthcare configuration and delivery, usually in the form of discrete QI projects utilising QI tools and methodologies, whereas Improvement Science is the broader scientific discipline sitting behind it. Improvement science aims to inform QI practice by finding out how to improve and make changes in the most effective way. It is about systematically examining the methods and factors that best work to facilitate QI. 16 In the rest of this article, and indeed the broader series of papers, we focus on the practice of QI as opposed to the wider field of Improvement Science per se.
QI can be defined as ‘better patient experience and outcomes achieved through changing provider behavior and organization through using systematic change methods and strategies’. 17 This definition captures the core features of QI which are the combination of a ‘change’ (improvement), a ‘method’ (a systematic approach aided by appropriate tools) and a ‘context’ (the environment in which the improvement is made) in order to achieve better ‘outcomes’. 18 Importantly, ‘better outcomes’ might not refer to patient outcomes alone, but to additional factors related to high-quality care, such as system performance and professional development (learning). 4 Alternative definitions of QI propose that it should not only refer to the practice of making changes on the ground, but to a general outlook and ambition to continually strive to make things better for patients. 19 Practically, in most hospitals in high-income countries globally, and certainly in all UK hospitals, this ambition translates into the presence of QI departments and relevant expertise, which can be used in-house to help frontline clinicians improve their services.
Underlying QI principles
A number of key principles underlie QI approaches in healthcare which are listed here and elaborated on in subsequent articles of this series:
Why QI is a valuable addition to clinical audit, research and other approaches to improvement
To understand the value of QI it is useful to compare it to similar approaches that seek to introduce or evaluate improvement in healthcare, most commonly clinical audit, research, service evaluation and clinical transformation (Figure 1). In reality, these approaches have many overlaps but also some very important differences.
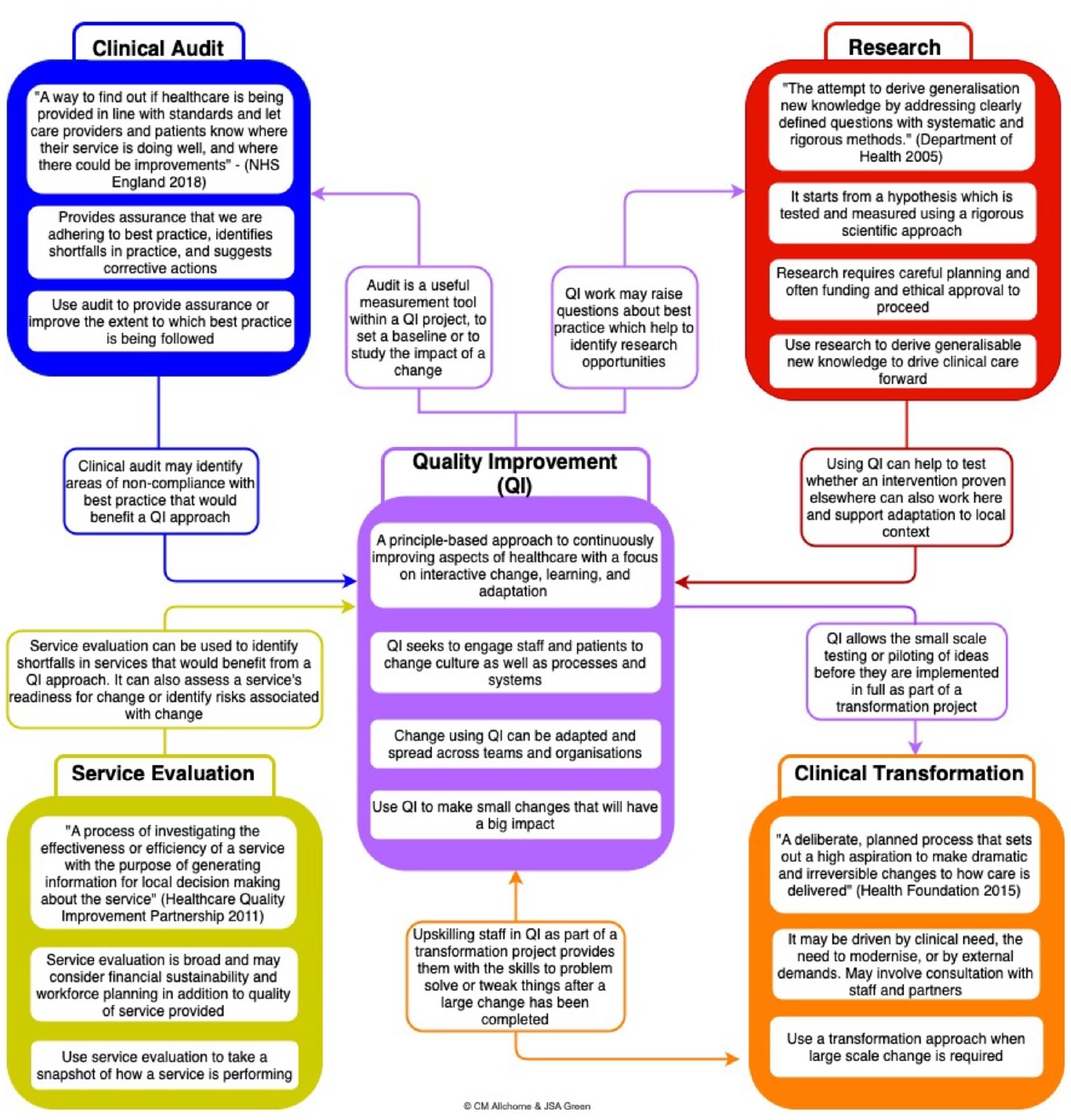
The intersection between Quality Improvement, Audit, Research, Service Evaluation and Clinical Transformation.
It should be noted that Improvement Science (i.e. the scientific discipline underlying and informing practical QI work) is where research and QI coalesce. Improvement research projects which are typically well-designed and with some form of control groups and comparators can both address improvement priorities and generate generalisable research data at the same time. Such projects tend to be larger, often funded through research budgets and undergoing research governance processes (e.g. ethical approvals), compared to the usually smaller scale, more modest QI projects. Improvement science falls under the ‘research’ panel of Figure 1.
QI and service evaluation
In contrast to QI, which aims to make changes to drive improvements in care, service evaluation aims to assess how well a service is achieving its intended aims. While bearing similarities to QI, research and audit in particular, service evaluation usually operates over a longer time-frame and has the purpose of evaluating an already established change to a service, or the introduction of a new service (an example would be the use of virtual clinics during the covid-19 pandemic). Service evaluation is used to determine whether a service is fit for practice and will usually be used to inform local decision-making about a service where particular issues need solving. As such it may be used to initiate QI activity by identifying areas for improvement or readiness for change. Conversely it may be used to evaluate the impact of changes made as a result of QI.20,34
QI and clinical transformation
Clinical transformation is a term used to describe radical approaches to change which involve dramatically re-engineering or re-designing how health care is delivered, usually irreversibly, based on a clearly articulated vision of the desired end-state. Clinical transformation is therefore usually driven by a top-down approach, involving shifting mindsets, changing relationships and re-distributing power, in contrast to the bottom-up, collaborative approach taken for QI. By definition, the iterative tests of change that characterise QI cannot take a transformational approach, as they involve making continuous adaptations, as opposed to implementing an already agreed solution. Despite these differences, QI methods and measurement can be used to support clinical transformation, for example, by testing ideas before full-scale transformation takes place, or following-up transformation with QI to drive continuous improvement of the new ways of working. 20
Support for QI: local and national infrastructure
With growing awareness and prioritisation of QI in healthcare, the infrastructure for supporting it at a practical level has also evolved rapidly. In the United Kingdom and other high-income countries, this can be seen at the level of individual healthcare providers (e.g. Trusts) and also at a national level.
Many hospital Trusts in the United Kingdom now have hospital QI departments and personnel specialising in improvement techniques. A recent report by the Care Quality Commission (CQC) – the independent regulator for health and social care in England – found that Trusts with an established improvement culture were most often characterised by having a central QI team or hub who facilitated improvement work across the organisation, with an explicit focus of transferring expertise in improvement methodologies to frontline staff, managers and senior leaders. This was often supported by regular open-access QI project meetings and reinforced in organisational processes including performance management, induction and governance. Other features of these trusts included having a clearly articulated strategic intent for QI with commitment and a hands-on approach at senior leadership level, a culture for QI that engages clinical leaders and empowers all staff to become involved in making improvements, easily accessible channels for patient involvement in QI, and the adoption of a systems approach resulting in improvements being made beyond organisational or functional boundaries. 35
At a national level, numerous organisations have a specific focus on QI and support it in various practical respects. These include organisations who set standards for QI and those who provide guidance and assistance in achieving these standards. Examples from the United Kingdom include the following.
Standard-setting organisations
Organisations providing assistance in achieving QI standards
A number of additional external influences complement the work of these organisations to drive improvements in quality. These include economic drivers, such as the Commissioning for Quality and Innovation (CQUINs) payment framework, which enables commissioners to reward excellence by linking a proportion of service providers’ income to the achievement of national and local QI goals. 46 The publication of annual ‘Quality Accounts’ – reports about the quality of services and improvements that have or will be made – has also, since 2009, been mandatory for NHS providers, making QI a requirement as opposed to a ‘nice to have’. 47 There are also various national campaigns and programmes aiming to drive a reduction in variation in the quality of care and share best practice sit alongside these initiatives, for example., ‘1000 Lives Plus’ – the Welsh national improvement programme – and Getting it Right First Time (GIRFT) – a national initiative to improve the quality of surgical care in the United Kingdom.48,49
Application to urology
Urology has moved from a focus on audit (quality control) to one of continuous improvement (QI). A good recent example of this in Urology is GIRFT.50,51 Up until now GIRFT has reviewed large national data sets (big data) in order to identify areas of variation in care delivered by different departments. Now this variation has been established there is a pressing need to remedy it and GIRFT (Urology), NHSi, the British Association of Urological Surgeons (BAUS), the British Association of Urological Nurses (BAUN) and The Urology Foundation (TUF) are supporting this initiative going forward. It works on the premise that if the level of care provided by Urology departments in the lower deciles was able to attain the performance of the top decile departments, then significant gains in patient care would be achieved. The recent GIRFT National Specialty Report for Urology outlined 18 recommendations for improving the quality of Urological care at both a departmental and national level. 50 These included priorities such as
Reducing average length of stay across the specialty through enhanced recovery and increased use of day case pathways, while monitoring causes and rates of emergency readmissions.
Improving the secondary care pathway for patients with urinary tract stones;
Ensuring high-quality emergency urological care is available in all areas 7 days a week by focusing available resources at weekends on a smaller number of departments, while allowing some departments to operate on a 5-day basis.
The vision for Urology and other healthcare specialties is that multi-disciplinary teams receive training in the practice of QI throughout their professional careers, beginning at the undergraduate level and being reinforced throughout post-graduate education and continuous professional development. This will enable teams to identify and systematically address the improvement needs of their own departments as well as improving the implementation of best practice 52 and increasing the likelihood of GIRFT successfully delivering on its aim to improve patient care. The outlook is that continuous improvement is embedded as standard practice in Urology departments and QI becomes part of the enduring armoury of Urology teams.
Conclusion
QI is the practice of using systematic change methods and strategies originating from other industries to make measurable improvements to the configuration and delivery of healthcare services. Distinct from other approaches to improvement, such as audit and research, QI relies on the use of iterative cycles to introduce and evaluate change, combining a thorough analysis of care processes with pragmatic yet systematic measurement, and strong engagement of frontline staff, hospital management and service users. The infrastructure for supporting QI work in the United Kingdom and other developed health systems is rapidly evolving, both within organisations and at a national level, driven by an ambition to embed continuous and sustainable improvement work into the everyday practice of healthcare teams. In the next edition of this series of articles we provide an introduction to QI approaches, tools and measurement to guide multidisciplinary Urology teams in planning and delivering robust QI projects of their own.
Footnotes
Conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: N.S. is the director of the London Safety and Training Solutions Ltd, which offers training in patient safety, implementation solutions and human factors to healthcare organisations and the pharmaceutical industry. The other authors have no conflicts of interest to declare.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This article series and the EQUIP research programme are funded by The Urology Foundation. The Urology Foundation gratefully acknowledges further funding from the Schroder Foundation.
S.J.R. research is supported by the NIHR through a Knowledge Mobilisation Fellowship. N.S. and S.J.R. research is supported by the National Institute for Health Research (NIHR) Applied Research Collaboration (ARC) South London at King’s College Hospital NHS Foundation Trust. N.S. is a member of King’s Improvement Science, which offers co-funding to the NIHR ARC South London and is funded by King’s Health Partners (Guy’s and St Thomas’ NHS Foundation Trust, King’s College Hospital NHS Foundation Trust, King’s College London and South London and Maudsley NHS Foundation Trust), and Guy’s and St Thomas’ Charity. N.S.’ research is further supported by the ASPIRES research programme (Antibiotic use across Surgical Pathways – Investigating, Redesigning and Evaluating Systems), funded by the Economic and Social Research Council. N.S. is further funded by the National Institute of Health Research (NIHR) Global Health Research Unit on Health System Strengthening in Sub-Saharan Africa, King’s College London (GHRU 16/136/54) using UK aid from the UK Government to support global health research. The views expressed in this publication are those of the author(s) and not necessarily those of the NIHR, the charities, the ESRC or the Department of Health and Social Care.
Guarantor
JG.
Contributorship
S.J.R. and J.G. drafted the manuscript which was then reviewed and amended by the remaining authors. All authors are members of the EQUIP steering group which spearheaded the work leading to this special series of articles.
