Abstract
Fahr’s disease is a rare neurodegenerative disorder that involves bilateral calcifications within the brain, most notably affecting areas such as the basal ganglia, thalami, and cerebellum. It is typically identified through its association with movement abnormalities, cognitive decline, or psychiatric symptoms; however, asymptomatic cases may be underrecognized, with studies suggesting a substantial proportion of patients remain without symptoms.³ In this report, a 45-year-old male came to the emergency department after experiencing a fall, complaining of rib pain and dizziness. During his trauma workup, a noncontrast computed tomography scan of the head incidentally revealed widespread bilateral calcifications in the basal ganglia, thalami, subcortical white matter, and cerebellar dentate nuclei. Subsequent magnetic resonance imaging supported the computed tomography findings, offering a clearer view of the extent of the calcifications. Laboratory tests, including assessments of calcium, phosphate, parathyroid hormone, magnesium, vitamin D, and thyroid function, returned normal results. Furthermore, comprehensive neurological and psychiatric evaluations found no abnormalities. Despite the extensive radiological evidence of brain calcification, the patient had no clinical symptoms. There was also no relevant family history of Fahr’s disease. These findings point to an idiopathic, asymptomatic form of the disease. This case emphasizes the importance of recognizing radiographic findings in the absence of clinical symptoms. Although identification and follow-up of such cases is often suggested, there is currently no evidence that this improves patient outcomes. Moreover, documenting asymptomatic cases helps expand understanding of the disease’s variability, natural course, and prognostic implications.
Keywords
Introduction
Terminology note
Throughout this manuscript, we use “Fahr’s disease” to refer to idiopathic or genetic primary brain calcification, and “Fahr’s syndrome” for secondary causes. This case, given the absence of a secondary cause, is consistent with Fahr’s disease.1,2
Fahr disease, also known as bilateral striopallidodentate calcinosis or idiopathic basal ganglia calcification, is a rare and heterogeneous neurological disorder characterized by pathological calcium deposition in key brain regions, including the basal ganglia, thalami, dentate nuclei, and subcortical white matter.1,2 While traditionally associated with neuropsychiatric and movement disturbances, a growing body of evidence reveals that many individuals harbor these calcifications asymptomatically, with the diagnosis often incidentally made during neuroimaging for unrelated complaints. 3
The pathogenesis of Fahr disease remains incompletely elucidated. In its primary form—commonly referred to as Fahr disease—the disorder typically follows an autosomal dominant inheritance pattern, suggesting a genetic predisposition. Conversely, secondary forms have been linked to diverse etiologies, including endocrine disturbances (most notably hypoparathyroidism), infections, and toxic exposures. 2 These findings suggest that abnormal calcium deposition results from a complex interplay among disrupted mineral metabolism, blood–brain barrier dysfunction, and genetic factors.
Noncontrast computed tomography (CT) is widely regarded as the diagnostic modality of choice for Fahr disease, owing to its superior sensitivity in detecting calcifications and its ability to delineate their characteristic bilateral and symmetric distribution. 2 Although magnetic resonance imaging (MRI) can provide additional insights—particularly regarding subtle white matter changes—its sensitivity for identifying calcific deposits is comparatively lower. In the present case, the patient underwent both CT and MRI, with the latter corroborating the CT findings and clearly demonstrating the spatial extent of calcification.
It is important to note that the extent of radiological calcification does not consistently correlate with clinical severity; some reports suggest that patients may remain neurologically intact for extended periods, though long-term outcome data remain limited. 3 Therefore, recognizing such imaging findings in asymptomatic individuals is crucial, as these may have significant implications for future management. However, it remains unclear whether routine identification and follow-up of asymptomatic individuals has a positive impact on prognosis. In this case study, we present an asymptomatic patient whose incidental CT and MRI findings suggest Fahr disease. Through a comprehensive review of the imaging characteristics, a discussion of the diverse etiologies, and an exploration of potential pathophysiological mechanisms, we aim to provide deeper insights into the clinical implications of this intriguing condition.
Case
A 45-year-old male presented to the emergency department with left-sided rib pain and intermittent dizziness following a fall 2 days prior while at a playground with his daughter. The patient reported that he fell onto his left side, resulting in persistent rib pain and continuous dizziness, which prompted his visit.
Initial imaging with a noncontrast CT of the thorax revealed fractures of the left 7th, 8th, 9th, and 10th ribs. As part of the trauma workup, a noncontrast CT scan of the head was performed and incidentally demonstrated multifocal, bilateral mineralization within the basal ganglia, thalami, and subcortical white matter—findings highly suggestive of Fahr’s disease. Subsequent MRI of the brain corroborated these findings, further delineating the extent of calcification (Figures 1 and 2).
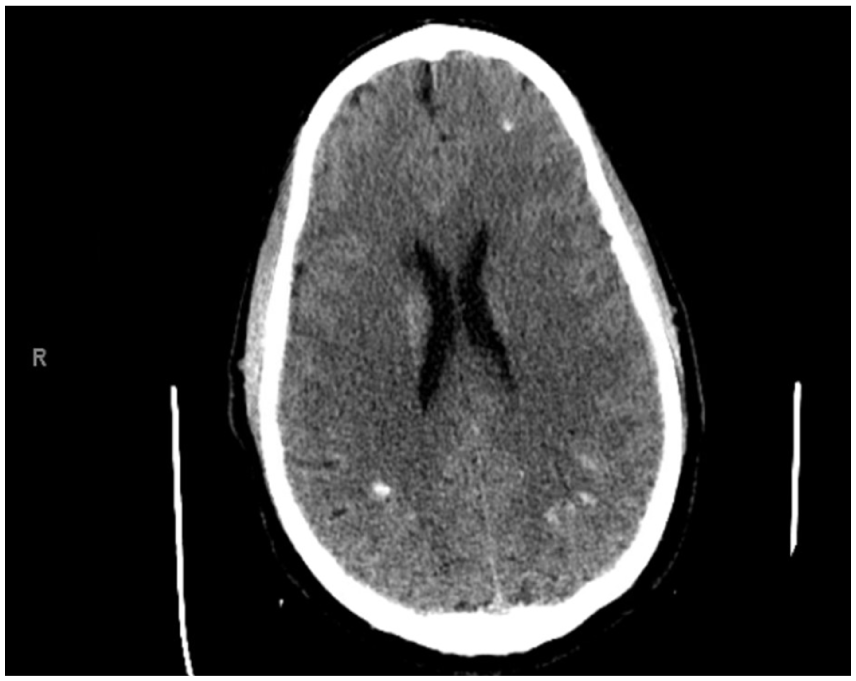
Axial noncontrast CT scan with findings of small, punctate calcifications visible in the subcortical white matter of the bilateral parietal lobes. Ventricles are mildly prominent but symmetrical.

Axial noncontrast CT scan showing multiple foci of calcification noted in the bilateral frontal and parietal subcortical white matter.
Laboratory investigations, including a complete blood count and comprehensive metabolic panel, were within normal limits. Serum calcium was 9.1 mg/dL, phosphorus 4.4 mg/dL, magnesium 2.1 mg/dL, and thyroid-stimulating hormone was 0.88. Parathyroid hormone levels were obtained at a follow-up visit and were 25 pg/mL (normal: 15–65 pg/mL). Vitamin D, 25OH was 33 ng/mL (normal: 30–100 ng/mL). All values were within normal limits.
The patient denied any known family history of Fahr disease and reported no history of significant head trauma, meningitis, HIV, or prior neurological deficits such as impaired concentration, memory loss, motor dysfunction, seizures, stiffness, spastic paralysis, speech difficulties, or abnormal eye movements. His past medical history was notable for a previously diagnosed vitamin D deficiency, for which he is currently taking multivitamins. Additionally, he mentioned a history of high-frequency hearing loss in his left ear, attributed to previous military service.
A thorough physical and neurological examination was unremarkable, with no acute findings or chronic deficits noted. The incidental neuroimaging findings, in the context of an otherwise asymptomatic neurological history, suggest an incidental presentation of Fahr’s disease in this patient.
Discussion
Fahr disease is characterized by bilateral, symmetric calcifications involving the basal ganglia, thalami, dentate nuclei, and subcortical white matter and represents a rare neurodegenerative disorder with a highly heterogeneous clinical presentation. 1 In the present case, a 45-year-old male was incidentally found to have extensive intracerebral calcifications on a CT scan performed without contrast, with these findings subsequently confirmed by MRI, despite an unremarkable neurological examination. The observed clinical and radiological dissociation—where significant calcific deposits do not correlate with overt neurological deficits—has been well documented.4–6
The etiopathogenesis of Fahr disease is multifactorial. Primary forms, often referred to as Fahr disease, have been linked to autosomal dominant mutations such as those affecting the SLC20A2 gene and other genetic alterations, including mutations in XPR1.2,6,7 Conversely, secondary forms may result from metabolic disturbances (e.g., hypoparathyroidism), infectious etiologies, or toxic exposures. 4 In our patient, normal serum levels of calcium, phosphorus, magnesium, and thyroid function, along with an absence of family history, support a diagnosis of an idiopathic or sporadic variant. This is consistent with emerging literature that suggests a spectrum of severity even among patients with similar imaging profiles. 8
Imaging is crucial in establishing the diagnosis of Fahr disease. Noncontrast CT remains the gold standard for detecting intracerebral calcifications due to its high sensitivity and its ability to delineate the classical bilateral, symmetric pattern.1,9 Although MRI is less sensitive for directly visualizing calcium, it provides complementary information regarding associated white matter changes and overall brain structure. 10 In this case, the combined use of CT and MRI facilitated a comprehensive assessment of calcific involvement, which may have prognostic implications regarding disease progression.
Emerging literature has also underscored the potential significance of vascular calcifications in neurological disorders. Intracranial arterial calcifications, for example, are increasingly recognized as potential biomarkers for stroke risk and may bear relevance in the context of Fahr disease.11,12 Although our patient did not demonstrate vascular calcifications, these findings suggest a broader role for calcification as a neuropathological marker.
Given the unpredictable clinical course of Fahr disease, especially in asymptomatic individuals, management is primarily conservative. While regular neurological monitoring and periodic follow-up imaging are often recommended, there is currently no evidence to suggest that such surveillance improves long-term outcomes in asymptomatic patients. In addition, genetic counseling may be considered as ongoing research continues to reveal the diverse molecular mechanisms underlying the disorder. 6
Conclusion
This case study describes the incidental detection of extensive intracerebral calcifications consistent with Fahr disease in an asymptomatic 45-year-old male. Despite marked radiologic abnormalities on both CT and MRI, the patient demonstrated no neurological deficits and maintained normal laboratory values, underscoring the discordance frequently observed between imaging findings and clinical presentation in Fahr disease. The evidence suggests an idiopathic or sporadic variant, emphasizing the importance of careful long-term observation, while acknowledging that current evidence does not support routine surveillance for improved outcomes in asymptomatic individuals. Future research is needed to further elucidate the genetic and molecular basis of Fahr
Footnotes
Acknowledgements
The authors gratefully acknowledge the use of Grammarly for language editing and polishing after the initial manuscript draft was completed.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Open access publication of this article will be supported by funds available through the Read and Publish agreement between SAGE and the University of Texas Medical Branch.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
