Abstract
Chronic ulcer management is often a frustrating experience not only for the patient but for the clinician as well. Many times, conservative local wound management with good supportive care alone may bring about desirable outcomes. We report the healing of long-standing multiple leg ulcers, with dedicated long-term local wound care and supportive management, in a patient suffering from multiple comorbidities – filarial lymphedema, varicose veins and hepatitis C infection. Cutaneous ulcers in association with hepatitis C infection are rarely reported in the literature. We highlight the importance of investigating rare underlying causes that delay wound healing, apart from stressing the significance of local wound care in inducing healing.
Keywords
Introduction
Lower limb lymphedema is a common sequela of filarial infection and is quite prevalent in endemic areas. 1 Lymph stasis may result in recurrent episodes of skin and soft tissue infections termed adenolymphangitis. 2 In these patients, infection or minor trauma may lead to leg ulcers. However, ulcer development in chronic lymphedema is less frequent compared to venous ulcers of the leg. 3 The management of ulcers becomes challenging when lymphedema co-exists with conditions like diabetes or varicose veins. Patients with poor economic status often ignore the treatment and medical advice. Many do not turn up for follow-up care, which delays wound healing, and the ulcer becomes chronic. We present the case of a patient with multiple nonhealing leg ulcers who has bilateral lymphedema and varicose veins. In the course of ulcer management, she was incidentally detected to have hepatitis C virus infection. This case report aims to document the challenges in managing non-healing ulcers in a patient with filarial lymphedema associated with unusual comorbidities. Further, the report highlights the effectiveness of conservative management and family home-based care in improving wound healing. Hence, this report contributes valuable insights to the limited literature on ulcer management in this specific patient population, aiming to enhance clinical awareness and improve the management of filarial lymphedema.
Case description
A 52-year-old woman presented to our Filariasis Management Clinic with the complaint of swelling of her right lower limb for 10 years and the left lower limb for 3 months. She has been suffering from multiple nonhealing leg ulcers on both legs for the past one year, before her presentation to our clinic. She had consulted multiple general practitioners and took treatment on and off, but the ulcers persisted. She had varicose veins in both legs and was operated on in 2013; she had undergone Trendelenburg’s procedure on the right lower limb with ligation of perforators. In 2014, perforator ligation was carried out again on the right lower limb. She did not have any history of diabetes, hypertension or cardiac illness. The patient presented to us in the month of September 2023. On examination, her lower limbs were found swollen, the right one more than the left. There was pitting edema in both legs. Hyperpigmentation of the skin was also noted. An ulcer of size 6 × 4 × 0.5 cm (Figure 1(a)) was noted on the right medial malleolus. Two ulcers were noted on the left leg, one measuring 3.5 × 2 × 0.5 cm (Figure 2(a)) on the anterior aspect of the lower one-third of the leg and the other one on the lateral aspect of the lower leg measuring 1 × 1 × 0.2 cm (Figure 3(a)). The ulcers were unhealthy with slough and discharge. There was tenderness around the ulcers. Her general physical and systemic examination did not reveal any other findings. Her blood sugar level was normal. Since Puducherry is an endemic region for lymphatic filariasis4,5 and as per WHO guidelines, 6 we came to the diagnosis of a clinical case of filarial lymphedema with associated varicose veins. Duplex ultrasound examination showed the presence of subcutaneous edema and varicose veins were noted in bilateral lower limbs confined to the great saphenous veins. The arteries of the lower limbs were found to be normal.

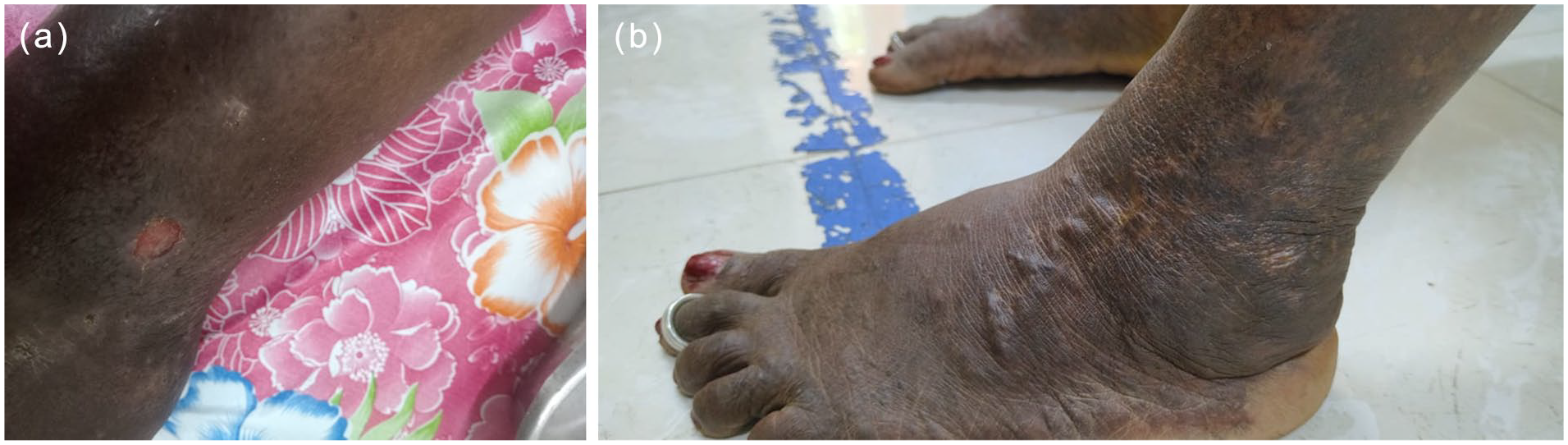
Ulcer 1. (a) At the time of presentation, September 2023, (b) 3 months, (c) 5 months, and (d) 9 months.

Ulcer 2. (a) At the time of presentation, September 2023, (b) 3 months, (c) completely healed, 6 months.
Ulcer 3. (a) At the time of presentation, September 2023. (b) Completely healed, 6 months.
Mechanical debridement of the ulcers was carried out to remove the slough tissue. Patient was started on doxycycline and the topical antibiotic framycetin (Soframycin). We have collected swabs from the ulcers and subjected them to culture. Pseudomonas aeruginosa was isolated and it was sensitive to doxycycline and the drug was continued. Cleaning and dressing of the ulcer were carried out once a day on alternate days, under aseptic precautions. The wound is washed with normal saline and betadine lotion. We also used Bactigras (chlorohexidine gauze dressing). Later, we used the topical antibiotic mupirocin.
Patient was advised to attend our clinic on alternate days and wound cleaning and dressing were continued (Figure 1(b)). The patient was advised on the importance of a balanced diet and vitamin C and multivitamin tablets were prescribed once a day. We counseled the patient to take adequate rest avoiding prolonged standing and the need for long-term care is explained to her.
Once the acute infection subsided, we trained her on morbidity management and disability prevention (MMDP) practices for lymphedema which include limb washing with soap and tap water twice a day, preferably in the morning and in the nighttime. Patient is advised not to scrub using a brush, coconut fibers or any other material as this may injure the skin and lead to further infections. Patient should clean the skin folds and area between the toes using a soft cloth. After limb washing, mopping needs to be carried out with a dry, soft cotton cloth. The affected limb needs to be kept elevated during leisure time and whenever possible, and also during sleep with a pillow underneath the limb. The patient is advised on limb exercises and manual massage to improve the lymphatic and venous return. After the limb massage, a crepe bandage is applied from the feet to the leg during the daytime, before starting the household work to improve lymphatic flow. These simple measures help to improve lymphatic and venous drainage and thus prevent repeated episodes of skin infection. We taught her the self-care of the ulcer as well. With these measures, there was an improvement, and the ulcer base became clean and healthy granulation tissue started to appear (Figure 1(c)). We initiated her pneumatic compression therapy using the Lymphapress Optimal Plus device (12 channels). 40-55 mm/Hg pressure was applied for 30 minutes daily for 2 weeks. The patient was not willing to have surgery for varicose veins or any surgical procedures for the ulcers.
The small ulcer on the left leg (Figure 3(a)) healed completely in a few weeks (Figure 3(b)). There was improvement in the other ulcer on the left leg (Figure 2(b)) and the one on the medial malleolus on the right leg (Ulcer 1). However, after the initial improvement, these two ulcers remained the same for several weeks. At this point in time, we investigated her to rule out any systemic diseases. Her hemogram and renal function tests were within normal limits. However, the albumin/globulin ratio was found to be reversed in the month of November 2023, which is a feature of chronic diseases. On further evaluation, hepatitis C serology was found positive in the month of February 2024, and the patient was referred to a specialist for treatment of hepatitis C infection. Albumin/globulin ratio re-tested in the month of April 2024 was found to be normal. Antivirals were not indicated as the HCV RNA test was negative (done in May, 2024). USG abdomen showed a normal liver. Patient is advised to have regular follow-up at 6-month intervals. In the meantime, we continued with the local wound care and supportive measures. We suggested she keep herself away from household and domestic work for a few weeks and strictly adhere to the MMDP practices. The patient had the ulcers for about a year before presenting to us. After our conservative management ulcer 1 took 9 months to heal (Figure 1(d)) and ulcer 2 (Figure 2(c)) healed in 5 months and ulcer 3 in 2 months. Figures 1 to 3 show clinical images at the time of presentation in our clinic and at different time points post-treatment.
Discussion
We described the healing of multiple chronic leg ulcers in a patient suffering from multiple comorbidities – filarial lymphedema, varicose veins and hepatitis C infection and stressed the importance of local wound care and supportive management in inducing healing. The prognosis for lymphedema and lymphangitis differs depending on the clinical presentation. Lymphedema, while incurable, can be efficiently managed with early intervention to alleviate symptoms and progression can be delayed. Uncomplicated lymphangitis typically resolves with the timely administration of antibiotic therapy, but untreated cases can advance to serious infections such as cellulitis or sepsis, considerably increasing morbidity and mortality. Therefore, prompt, adequate and appropriate care remains essential in such cases.7,8
Counseling the patient and gaining trust are essential in the management of chronic ulcers. The role of the caretaker cannot be overemphasized. We noted significant improvement in our patient when she stopped doing domestic work, and had adequate rest when she got good supportive care from a relative. Consistent and dedicated local wound care and supportive measures brought out the desirable results. In a published case series of ulcers in chronic lymphedema, stage I ulcers were reported to heal with conservative management alone, but those beyond stage I required surgical interventions. 3
Furthermore, existing literature has stated that chronic inflammation followed by cutaneous manifestations such as hyperkeratosis, hyperpigmentation and warty changes are hallmarks of lymphoedema. Further, chronic venous insufficiency also presents with superficial dilation with associated skin changes and ulceration. Both conditions mimic each other, although the treatment is different. The diagnosis needs to be confirmed prior to the institution of treatment.9–11
Another point that we wish to highlight in this case is the presence of hepatitis C virus infection. We believe it might have also contributed to the development and delayed healing of ulcers. Extrahepatic manifestations are not uncommon in hepatitis C infection and skin conditions like cutaneous vasculitis, urticaria, oral lichen planus and Raynaud’s phenomenon are known, but rarely reported.12,13 Vasculitis form of hepatitis C infection commonly presents with immune complexes mediated vasculitis involving small vessels associated with or without cryoglobulinemia. 14 Our patient tested negative for cryoglobulinemia. There are only a few reports of cutaneous ulcers in association with hepatitis C infection in the medical literature.12–18 Healing of chronic ulcers with sodium hypochlorite 0.05% and iodopovidone 0.5% application with regular dressing with collagenase plus hyaluronic acid ointment alone in patients with chronic hepatitis C infection has been reported. 17 One study reports the benefit of rituximab in the treatment of vasculitic leg ulcers associated with hepatitis C infection. 19 We believe that in our patient there was spontaneous clearance of HCV infection as the HCV RNA test was found to be negative and the abnormal albumin globulin ratio was found to be normal when re-tested after a few months.
In short, we reported the co-existence of multiple conditions leading to delayed healing of ulcers highlighted the importance of investigating underlying causes, and stressed the significance of consistent and dedicated supportive measures and local wound management in inducing healing.
Conclusion
The case report highlighted the challenges in the management of lymphedema in patients with comorbidities, thereby addressing the paucity of literature specifically addressing ulcer management in HCV co-infection. This case emphasizes the critical role of consistent and dedicated supportive care through abstinence from household and domestic work and strict adherence to MMDP practices in improving the quality of life of patients with filarial lymphedema.
Footnotes
Acknowledgements
We gratefully acknowledge the assistance of N. Nagarajan, Technician-1, Unit of Clinical and Molecular Medicine, ICMR–Vector Control Research Centre, in wound care.
Ethical considerations
Ethical approval to report this case was obtained from the Institutional Human Ethics Committee of ICMR–Vector Control Research Centre (IHEC-0522/N/J).
Consent for publication
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this case report and accompanying images.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
