Abstract
Morbihan’s disease is a rare form of facial lymphedema often associated with chronic rosacea and other skin diseases such as acne. It presents as indurated erythematous plaques in the upper face, which can be challenging to treat. We report a 69-year-old male of Asian background with a 4-year history of facial swelling and redness, unresponsive to prior treatments. After a clinical diagnosis of Morbihan’s disease, the patient was treated with oral isotretinoin 10 mg daily, leading to an 80% reduction in symptoms after 9 months. Mild side effects, including cheilitis and xerosis, were well managed. This case highlights low-dose isotretinoin’s potential as a therapeutic option for Morbihan’s disease. Previous studies have demonstrated the efficacy of treating Morbihan’s disease with isotretinoin at high doses between 40 and 80 mg po daily for 12–24 months.
Introduction
Morbihan’s disease (MD), also known as solid persistent facial edema, or rosacea lymphedema, is a rare condition that may arise spontaneously and typically does not resolve without treatment. 1 It occurs during a prolonged course of chronic rosacea 2 and is characterized by non-depressive swelling in the upper two-thirds of the face, with facial redness that may appear diffuse and poorly defined, or present with distinct patches or plaques. 3 The condition can cause facial disfigurement, significantly affecting patients’ quality of life and mental health. 1 While specific data on its incidence and prevalence are unavailable, MD is classified as a rare condition. 1 Most reported cases occur in middle-aged Caucasian adults, but it has also been documented in individuals with skin of color. 4 We present a case of a 69-year-old Asian man with MD who showed improvement with low-dose oral isotretinoin.
Case report
A 69-year-old Asian male of Filipino descent presented to dermatology with complaints of persistent facial swelling. The onset of his symptoms occurred 4 years prior and included mid-cheek facial redness and swelling withsignificant lower eyelid edema. He reported minimal pruritus and no obvious triggers, such as alcohol or spicy foods. The patient had previously been treated with metronidazole 1% gel, pimecrolimus 1% cream, and oral doxycycline without any improvement in his symptoms. He had also been evaluated by an allergist, who ruled out an immunoglobulin E-mediated cause for the facial swelling such as angioedema. At the time of his initial dermatology visit, physical examination revealed erythema and edematous plaques involving the glabella, nose, and bilateral cheeks (Figure 1). A clinical diagnosis of MD was made.
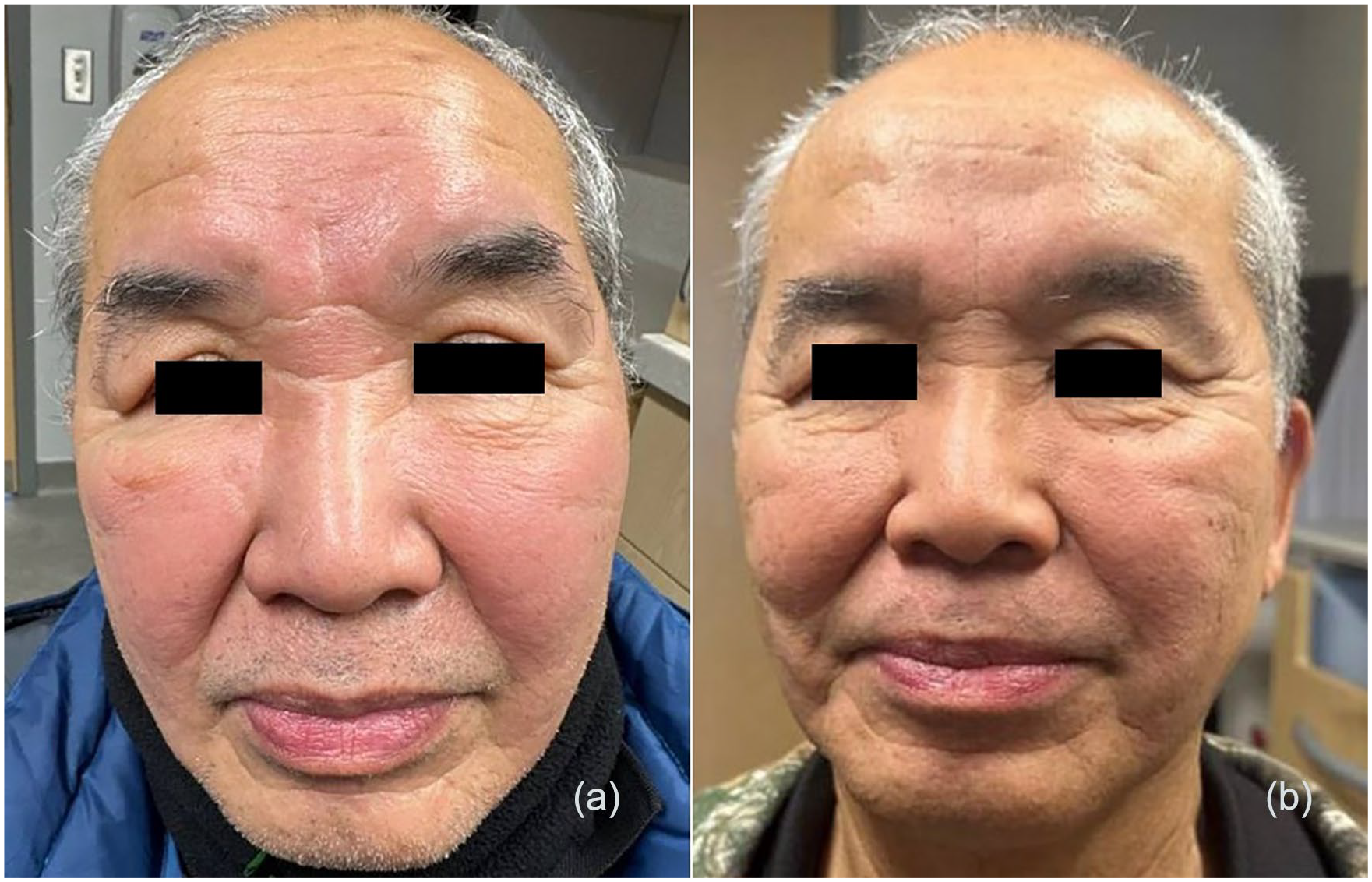
(a) Sixty-nine-year-old Asian man with erythema and edematous plaques involving the glabella, nose, and bilateral cheeks. (b) One year later after successful treatment with isotretinoin 10 mg for 9 months.
The patient was started on low-dose isotretinoin 10 mg daily. He was advised that the sun can worsen rosacea and that photosensitivity can be a side effect of isotretinoin. The patient was also prescribed ivermectin 1% cream to apply topically for maintenance. Blood work, including liver and lipid panels, was monitored after the first month of treatment and then every 6 months.
At his follow-up visit 9 months later, the patient reported an 80% improvement in his symptoms, with significantly less facial swelling (Figure 1). He tolerated isotretinoin well, with only mild cheilitis and xerosis. The erythema and edematous plaques had nearly resolved, and his facial swelling had markedly decreased (Figure 1).
He continued to improve on low-dose oral isotretinoin, which represents a good and well-tolerated line of therapy for challenging or treatment-resistant types of rosacea such as MD. He is now being trialed on isotretinoin 10 mg every other day for maintenance treatment.
Discussion
MD presents diagnostic and treatment challenges, as no published clinical practice guidelines exist for its management. 1 While MD is classified as a rare disease, it may be underreported particularly in individuals with skin of color, potentially due to diagnostic challenges and lower access to dermatologic care.
The exact pathophysiology of MD remains unclear. However, it is believed to result from an imbalance between fluid accumulation and drainage in the upper face, with damage to vascular and lymphatic networks, leading to persistent, non-transient edema. 1 Due to diagnostic challenges and variability in clinical presentation, it is also likely underdiagnosed in many populations.
The condition significantly impacts patients’ quality of life and contributes to mental and emotional distress. This highlights the importance of early and effective intervention. Systemic immunomodulators such as corticosteroids, antibiotics, and antihistamines have often been ineffective in managing MD. 5 In addition, more invasive procedures such as surgical reduction, carbon dioxide laser blepharoplasty, and radiotherapy have shown inconsistent results and can be costly. 5
Isotretinoin, a synthetic retinoid, has emerged as an important treatment modality for difficult-to-treat cases of facial edema associated with MD. 5 Isotretinoin’s efficacy in MD is thought to stem from its ability to inhibit fibroblast and inflammatory mediator proliferation 4 , decrease chronic inflammation and prevent further damage to the dermal tissue. 5 Other studies in the literature have treated MD with isotretinoin at high doses between 40 and 80 mg po daily for 12–24 months.5,6 Our study is novel in demonstrating the efficacy of low-dose isotretinoin in effectively treating MD, which offers patients a more favorable side effect profile.
MD is a chronic and recurrent condition; management should not only focus on the resolution of symptoms but also emphasize the prevention of relapses. Continued sun protection and avoidance of triggers are key to maintaining clinical stability and ensuring long-term disease control. Further research and controlled studies, with larger numbers of patients, are needed to improve efficient diagnostic accuracy in all skin types and establish standardized treatment protocols for the most effective therapies.
Footnotes
Acknowledgements
None.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
IRB approval status Not applicable.
Patient consent
Written consent was provided for the use of clinical information and photos for publication and research.
