Abstract
Minocycline-induced pigmentation is a rare dermatological condition that primarily affects the skin and thyroid gland, oral mucosa, nails, teeth, bones, and sclera leading to grayish-blue pigmentation in these areas. Early identification, discontinuation of the drug, and laser treatment are crucial in managing this condition. We reported a case involving a 72-year-old Chinese woman who developed diffuse blue-brown pigmentation after 1 year of minocycline treatment for pemphigus vulgaris. Histological examination revealed multiple pigment-laden macrophages and free pigment in the dermis at the skin lesions. According to our review of the literatures, the generalized skin involvement made our case very rare in comparison with those previously reported of Chinese patients.
Introduction
Minocycline hydrochloride is a broad-spectrum antibiotic belonging to the tetracycline class. It is commonly used in the treatment of various skin conditions such as acne, skin infections, sexually transmitted diseases, secondary syphilis, as well as other inflammatory skin diseases. 1 However, the use of minocycline may lead to some side effects, including dysbiosis, diarrhea, and enteritis. 2 Moreover, when the cumulative dose of minocycline exceeds 100 g, pigmentation may occur, most commonly affecting some organs in the human body, such as the skin and thyroid gland.3,4 Additionally, areas such as the oral mucosa, nails, teeth, bones, and sclera may also be affected. 5 Minocycline-induced pigmentation (MIP) was rare in Chinese population. 6 Here, we report a generalized case of MIP and review the medical literature of recent years.
Case report
A 72-year-old Chinese female presented with diffuse hyperpigmentation on her limbs. She has a history of pemphigus vulgaris for 3 years and has been taking 100 mg of minocycline hydrochloride twice daily for 1 year. Upon physical examination, diffuse gray-blue pigmentation was noted on her extremities (Figure 1 and Supplementary figure). No pigment deposition observed on mucous membranes, eyes, teeth, or nails. There were no typical pemphigus vulgaris rashes observed on the presentation. Skin biopsy taken from the anterior pigmentation lesion, and displayed numerous pigment-laden macrophages and free pigment in the mid to deep dermis. Immunohistochemical analysis revealed positive staining of CD68 of pigment-laden macrophages, and which were negative staining for SOX-10, Melan A, or HMB45 (Figure 2). The diagnosis of MIP was made. The decision to discontinue minocycline treatment for the patient has been made, and currently being closely monitored.
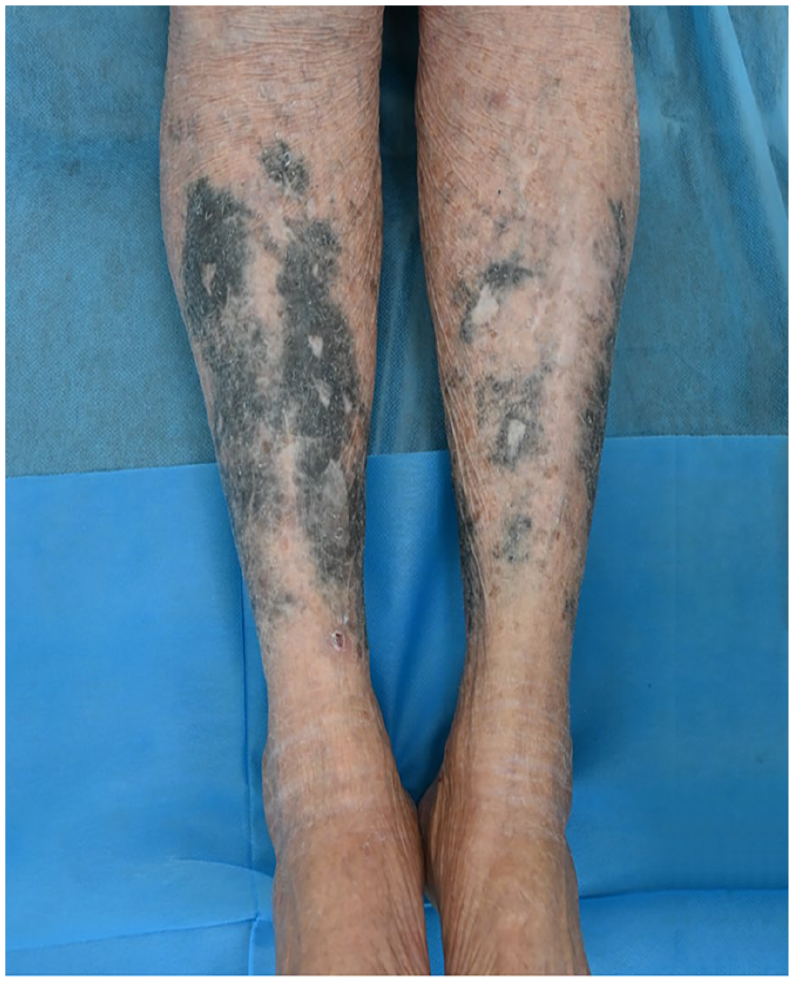
Widespread gray-blue pigmentation on the lower extremities.

Histopathological and immunohistochemical features of MIP. (a) Skin biopsy specimen of tibial anterior lesions showed dense dermal infiltration of pigment-laden macrophages (Hematoxylin and Eosin (H&E), original magnification ×40). (b) Pigment-laden macrophages better appreciated at higher magnification (H&E, ×100). (c, d) Numerous pigment-laden macrophages in the dermis showed CD68 positive staining (×40, ×100). (e–g) Immunohistochemistry revealed negative staining for SOX-10, Melan A, or HMB45 (×100). (h) S-100 staining showed localized positivity (×100).
Discussion
MIP has an extremely low incidence rate in Chinese population, especially in individuals aged 52 and above peoples. 7 This type is more common in areas where the skin has undergone elastosis due to UV exposure. Based on the location of occurrence, there are four types: Type I presents as blue-black or gray-blue pigmentation near inflamed areas; Type II manifests as blue-gray pigmentation on normal skin of the lower legs or forearms; Type III appears as diffuse muddy brown pigmentation in sun-exposed areas, also known as “dirty skin syndrome” or “muddy skin syndrome”; and Type IV occurs as muddy brown pigmentation on pre-existing scars not exposed to sunlight. 8 In our study, we described a Type II MIP case and speculate that the pigmentation might be associated with excessive sun exposure.
The exact cause of MIP is still unclear, but minocycline, as a photosensitive drug, can increase melanin production by melanocytes independently of UV exposure and may also disrupt melanosome maturation. UV exposure can enhance this effect.9,10 It is also noteworthy that skin discoloration may be caused by the formation of a tetracycline–melanin complex, which contributes to the accumulation of the drug in pigmented tissues.11,12 Earlier, Sato utilized radiomicrographic techniques to confirm that pigmentation is closely related to minocycline derivatives chelated with iron stored in macrophage lysosomes. Additionally, the degree of iron particle deposition in dermal tissue cells is also considered a primary factor leading to the bluish-black skin discoloration. 13 In our case, the patient with pemphigus vulgaris was treated with minocycline for over 1 year, which also validates the findings of La Placa, 14 that pigmentation is most likely to occur in patients undergoing long-term treatment with minocycline. In our cases, the pigment-laden histiocytes expressed CD68 positivity, while Melan A, SOX-10, or HMB45 were negative. Disorders of pigmentation are usually due to the deposition of melanin and an increase in active melanocytes, and these negative results confirmed our diagnosis of MIP.
Currently, there is no standardized treatment for MIP, so its management remains in the exploratory stage. 3 Early studies have suggested that combining Medlite Q-switched laser with Vbeam pulsed dye laser technology can significantly improve symptoms. 15 Additionally, Green and Friedman used nanosecond Q-switched laser treatment as a mainstream approach for MIP, achieving satisfactory results in nine patients. 16 Subsequently, considering the potential side effects of laser treatment, such as post-inflammatory hyperpigmentation or hypopigmentation and scarring, Jakus and Kailas proposed optimizing the use of picosecond laser for treatment. 17 Due to widespread pigmentation and the low demand for skin esthetics of the elderly patient, she had not undergone laser treatment. At the 1-year follow-up visit after discontinuing minocycline, the pigmentation still persisted, but the edges had slightly faded. It is worth noting that although tetracycline antibiotics such as minocycline have shown certain efficacy in the treatment of some diseases, prolonged use of these drugs may lead to multiple side effects.2–4 Therefore, when deciding to use tetracycline antibiotics for treatment, the patient’s specific condition must be fully considered, weighing the pros and cons, and closely monitoring the occurrence of drug side effects.
Conclusion
In summary, we report a rare type II MIP case in a Chinese female undergoing long-term minocycline treatment for pemphigus vulgaris. The medication has been discontinued, no treatment was given for the widespread lesions.
Supplemental Material
sj-docx-1-sco-10.1177_2050313X241297214 – Supplemental material for Generalized type II minocycline-induced pigmentation: A case report
Supplemental material, sj-docx-1-sco-10.1177_2050313X241297214 for Generalized type II minocycline-induced pigmentation: A case report by Wumei Zhao, Haijing Fu, Tianyi Xu and Shi-Jun Shan in SAGE Open Medical Case Reports
Footnotes
Acknowledgements
None.
Author contributions
S.-J.S. and W.Z. designed research; H.F. and T.X. performed research; S.-J.S. revised the manuscript.
Data availability statement
In this document, all image data presented have undergone rigorous privacy protection measures and have been obtained with the informed consent of the relevant patients. We solemnly pledge to adhere to ethical and privacy principles at all times, ensuring the lawful and compliant use of image data.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Supported by National Natural Science Foundation of China (81972953, S.-J.S.).
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
