Abstract
Niacin (Vitamin B3) plays a crucial role as a vitamin in cellular energy production, metabolism, and DNA repair. A severe deficiency of this vitamin can lead to pellagra, which is characterized by dermatitis, dementia, diarrhoea and eventually death if untreated. A 68-year-old woman with a poor socioeconomic background presented with photosensitive dermatitis, fever, abdominal pain, and diarrhoea. Her urine changed to port wine colour following sun exposure. Porphyria cutanea tarda was excluded in the absence of demonstrable urine spectrophotometry. A diagnosis of pellagra was made, and timely management led to a complete cure. Proper diagnosis and effective treatment of pellagra are imperative as this condition can be life-threatening if left untreated.
Introduction
Pellagra occurs due to a deficiency of niacin (vitamin B3) and/or its precursor amino acid, tryptophan. 1 The etymology originates from ‘agra’ and ‘pelle’ which in Italian denotes roughness of skin. 2 In modernity, dietary provision is sufficient to prevent deficiency although certain populations in developing countries are still at risk. Primary pellagra occurs due to a pure deficiency of both nutrients, whereas secondary disease originates from medical conditions such as cirrhosis, HIV, malignancies, gastrointestinal tract diseases and alcoholism due to poor absorption. Furthermore, certain medications such as azathioprine, isoniazid and phenobarbitone can also lead to secondary pellagra 3 Pellagra is a public health problem in maize-consuming countries such as Africa and South America. 4 In neighbouring India, niacin deficiency was observed among 13% of girls 10–13 years. 5 Outbreaks of pellagra are encountered among refugees in African countries as well as in Nepal. 4 In the United States, pellagra is rare due to the enrichment of processed flour with B vitamins and with multi-vitamin-rich food sources. 1
The disease results in an acute, symmetrical, well-demarcated, tender, erythematous rash in sun-exposed regions. Chronic disease gives rise to hyperpigmentation with desquamation generating a cracked, scaly appearance. 3 Patients with porphyria cutanea tarda (PCT) develop photosensitivity with blisters, hyperpigmentation and scarring, thus making it a differential diagnosis. 6 Diagnosis of pellagra requires thorough clinical reasoning. Oral supplementation of nicotinamide with a balanced diet is pivotal in the management. 1 Inadequate treatment leads to higher levels of mortality although adequate treatment gives promising outcomes. 3 We report a presentation of pellagra disease in the background of chronic alcoholism and alcoholic hepatitis mimicking PCT.
Case report
A 68-year-old woman presented with a 3-day history of low-grade fever, and generalized abdominal pain with multiple episodes of vomiting and watery diarrhoea. There was a pruritic rash on bilateral extensor regions of the upper limb and on the neck that developed over 2 weeks duration. She had a poor socioeconomic background, employed as an unskilled worker in a quarry being exposed to hot sun in a tropical country. She regularly consumed illicit alcoholic brews of varied alcohol content, 1 l per week for more than 20 years. There was no consumption of tobacco or other narcotics nor a history of sexual promiscuity. There was no history suggestive of food poisoning or exposure to dirty water in terms of leptospirosis. The patient did not have a significant medical or psychiatric history. Furthermore, her family history was insignificant for dermatological, rheumatological or metabolic disease.
A scaly rash around the neck and extensors of upper limbs in sun-exposed areas was observed (Figure 1). She was pale and icteric. The blood pressure was 130/85 mmHg, and there were no cardiac murmurs. Abdominal examination revealed right hypochondriac tenderness without hepatosplenomegaly. The respiratory examination and neurological examination were unremarkable.
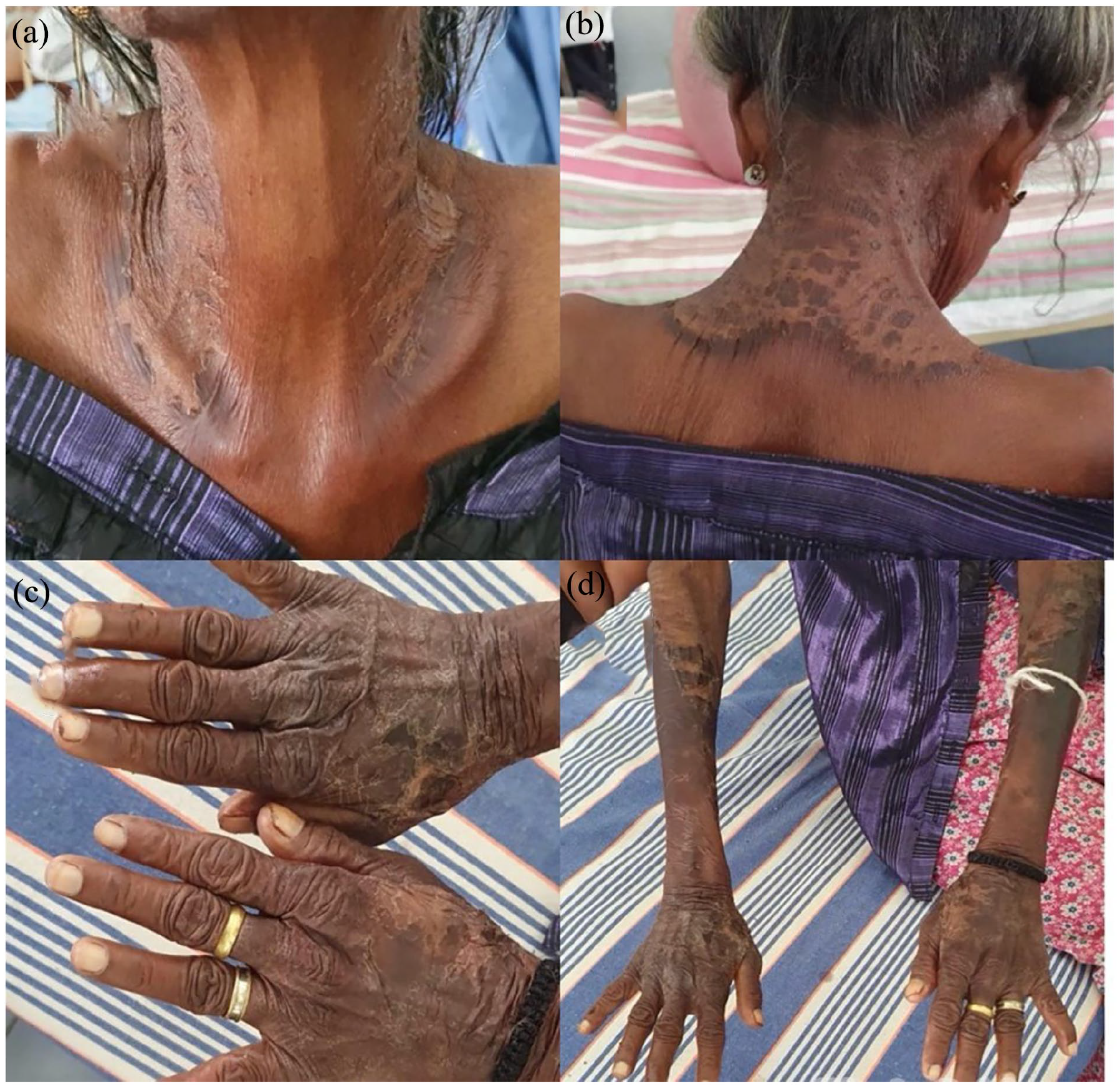
Rashes that resemble a sunburn, then progresses to rough, scaly, hyper-pigmented plaques over the front of the neck (a), back of the neck (b), dorsum of the hands (c) and forearms (d).
In consideration of possible PCT with photosensitive dermatitis, a sample of urine was kept directly subject to sunlight which changed to port wine colour (Figure 2). However, Hoesch test for urine for porphobilinogen was negative. PCT was excluded therefore along with the absence of the characteristic wavelength of 390 nm and 420 nm in urine spectrophotometry. However, basic investigations performed demonstrated normocytic normochromic anaemia, direct hyperbilirubinemia and transaminitis. The latter were suggestive of hepatitis.

Urine colour before the sun exposure (a) and the same urine colour change after the sun exposure (b).
Biochemical analysis of nicotinamide levels was unavailable in the current setting. A therapeutic trial of oral niacin 100 mg three times per day was commenced. Iron, folic acid and vitamin B complex supplementation were also initiated with dietary advice and intervention. The patient responded to the treatment very well and was discharged from care with emulsifying local applications to the skin rash. The patient was followed up for 3 months during which she had a marked clinical improvement. This led to confirmation of pellagra due to niacin deficiency.
Discussion
Pellagra as a chronic multi-system disease primarily affects the skin, gastrointestinal system and nervous system. This is explained by the significant role of vitamin B3 in cell signalling, DNA repair pathway, metabolism of proteins, carbohydrates and fat, and detoxification of drugs, alcohol and reactive oxygen species. 7 The liver and kidneys also contribute to nicotinamide production by tryptophan. Thus diseases of the liver and kidney can contribute to niacin deficiency. 8
Our patient, a manual labourer with low socioeconomic status frequently skipped meals as well as consumed a frugal diet due to limited income. She overindulged in alcohol, which also contributed to poor nutrition including niacin deficiency. 9 Furthermore, acute alcoholic hepatitis would have exacerbated the severity of deficiency due to poor hepatic production.
The clinical presenting symptoms of pellagra can be described by three D’s: dermatitis, diarrhoea and dementia. If neglected, it can progress to the fourth D: death. Dermatitis primarily manifests in sun-exposed areas and may resemble sunburn. It initially appears as blisters and progresses into rough, scaly skin. 10 The eruptions can cause vesicles and bulla, unlike typical dry scaly rash termed as wet pellagra. 3 Diarrhoea is an early symptom, accompanied by poor appetite, nausea and abdominal pain. Neurological symptoms occur later and can range from minor symptoms like memory loss, poor sleep and mood changes to severe symptoms such as hallucinations, psychosis and stupor (pellagra encephalopathy). 10 Our patient was unique due to the atypical presentation of dermatitis and diarrhoea with urine changes without dementia.
Differential diagnoses of pellagra include PCT, inflammatory bowel disease, drug eruptions, discoid lupus erythematosus and acute cutaneous lupus erythematosus. 1 Further investigations and exclusion of these differentials are necessary to confirm the diagnosis if the clinical picture is suggestive. The clinical context led to a primary suspicion of PCT, which was ruled out by the negative Hoesch test and the spectrophotometer for urine porphyrins showing a wavelength of 380–390 nm, instead of the typical wavelength of excitation 395–420 nm and emission 580–620 nm seen in porphyria. 11 Serum or urine porphyrin level analysis is not available in our clinical setting.
Confirmation of the diagnosis of niacin deficiency requires laboratory testing for tryptophan and niacin levels, urinary excretion of N1-methyl nicotinamide levels or the most sensitive testing method, high-pressure liquid chromatography of niacin metabolite levels in urine. However, a marked therapeutic response to niacin in a patient with the typical features consistent with pellagra establishes the diagnosis in a 1 resource-limited setting like Sri Lanka. 1 Therefore, a clinical diagnosis of pellagra was made retrospectively after exclusion of other differentials with this clinical response. The change into dark colour of urine can be attributed to high urobilinogen levels due to acute liver injury secondary to alcohol consumption as the other causes causing colour change of urine into dark stain such as cresol poisoning, consumption of rhubarb or fava beans, myoglobinuria, methyldopa, chloroquine and primaquine, furazolidone, metronidazole, sorbitol and levodopa consumption was excluded.12–14 The colour of the urine changed back to normal with the improvement of the liver injury.
Alcohol dependence or chronic alcoholism can induce and aggravate pellagra in many ways. Excessive alcohol can lead to absolute niacin deficiency mainly by inducing malnutrition, gastrointestinal disturbances and B vitamin deficiencies, inhibiting the conversion of tryptophan to niacin. Alcoholic pellagra encephalopathy should be managed with niacin, other B vitamins and adequate protein nutrition. In alcohol-dependent patients, pellagrous encephalopathy can also occur in combination with Wernicke’s encephalopathy which can cause underdiagnosis of the condition. 15
The World Health Organization recommends nicotinamide as 300 mg orally or 100 mg parentally in divided doses with the maintenance dose of 50–100 mg/day after the disappearance of the acute symptoms along with the initiation of other vitamin supplementation to address possible concurrent dietary deficiencies. 5 Following the treatment most people begin to improve in a few days. Gastrointestinal symptoms are the first to heal, usually within the first week. Followed by healing of skin and mouth ulcers within 2 weeks. Patients in advanced clinical stages may take longer to heal. Severe nerve damage and dementia may be irreversible. Early detection and prompt treatment improve the prognosis of disease. 2 The resolution of the dermatological findings in our patient further supports the diagnosis of pellagra patients should be counselled on avoiding sun exposure and also alcohol consumption to achieve optimal treatment outcomes. 1
Conclusion
Pellagra resembles PCT as in both, patients present with a photosensitive skin rash in acute illness. Furthermore, it can also give rise to urine that turns dark like PCT due to urobilinogen in the background of acute hepatic failure. The resolution of colour to normalcy with treatment of liver injury refutes PCT. Furthermore, the marked response of the illness with vitamin replenishment confirms pellagra clinically in the absence of niacin or tryptophan analysis in a resource-limited setting. If left untreated, pellagra can lead to devastating consequences leading to fatality. Proper treatment, can lead to promising outcomes. Nevertheless, pellagra continues to be underdiagnosed. Continuous awareness programmes and guidelines are essential to equip healthcare professionals with the necessary skills to effectively identify and manage cases of pellagra.
Limitations and future perspectives
Long-term patient follow-up after 3 months was not possible due to the poor socioeconomic conditions of the patient limiting hospital visits. Although nutrition clinic follow-up was arranged, there were limitations in sustainability due to poverty. This case report highlights the importance of diagnosis of this old disease.
Footnotes
Acknowledgements
We extend our thanks to the patient who provided us with the consent to publish this case report.
Author contributions
C. L. M. is a physician trainee under the supervision of S.S., a consultant internal medicine specialist. Both C. L. M. and S.S. were involved in the management of the patient and the composition of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
