Abstract
The management of gastrointestinal complications in patients with complex medical history poses significant challenges to healthcare clinicians. A 42-year-old male patient was admitted to the emergency department with excruciating abdominal pain and signs of bowel obstruction. The patient had a previous history of schizophrenia and esophageal stricture, treated 6 years ago with colonic esophageal interposition. From the computed tomography scan, intussusception of the jejunum in the colonic graft was revealed, which resolved spontaneously after a few hours probably due to the oral contrast. Although, colonic esophageal interposition is a life-saving procedure for long-esophageal strictures, there are rare complications that are still not clearly reported. Jejunocolic intussusception should raise awareness of the clinicians, as one of the potential complications of colonic esophageal interposition.
Introduction
Intestinal intussusception in adults is a rare condition with an incidence of 5% of all intussusceptions and representing 1% of bowel obstruction. It often stems from underlying pathologies such as tumors, polyps, or postoperative changes altering bowel peristalsis. Unlike in children, where intussusception is usually idiopathic, in adults it frequently presents as a secondary complication. 1
Colonic interposition, a surgical procedure often performed to treat long esophageal strictures due to conditions such as corrosive injuries, is a complex intervention that can lead to rare but serious complications. Esophagectomy followed by reconstruction is considered one of the most challenging interventions on the alimentary tract. Although this procedure can be life-saving, its complications are not well recognized nor extensively documented in the literature. 2
This report describes a rare case of jejunocolic intussusception occurring in a patient with a history of colonic interposition for an esophageal stricture. The patient’s medical history, including prior caustic ingestion and schizophrenia, added to the diagnostic and management challenges. This case underscores the importance of considering intussusception as a potential, though rare, complication in patients with prior colonic interposition.
Case report
A 42-year-old male patient presented to the emergency room with the chief complaint of excruciating abdominal pain and abdominal distension persisting over the past 4 days. From his previous medical history, the patient suffered from schizophrenia and had undergone a retrosternal colonic interposition with the left colon 6 years ago for treating esophageal stricture due to caustic ingestion.
He described the onset of pain originating in the upper left abdomen, gradually escalating to a constant, crampy discomfort. Concurrently, he experienced persistent nausea and vomiting, primarily of saliva, alongside a cessation of bowel movements and passing gas.
On physical examination, the patient appeared calm with stable vital signs, including a blood pressure of 140/90 mmHg, a heart rate of 100 bpm, a respiratory rate of 20 bpm, and a febrile temperature of 37.8°C. Abdominal palpation revealed diffuse tenderness without rebound or guarding.
Laboratory investigations demonstrated a mild leukocytosis, with a white blood cell count of 12,000/mm3, while the electrolyte panel remained within normal limits.
A computed tomography (CT) scan, performed with both oral contrast medium (gastrografin) and intravenous contrast injection, revealed a notable finding. The oral contrast medium demonstrated unimpeded passage through the grafted colon until reaching the colon-jejunal anastomosis. At this juncture, a distinctive “bowel within a bowel” configuration was observed, characterized by concentric rings of high- and low-density layers in axial images and a sausage-like appearance in longitudinal images (Figure 1). Notably, no signs of pneumoperitoneum or free peritoneal fluid were identified.

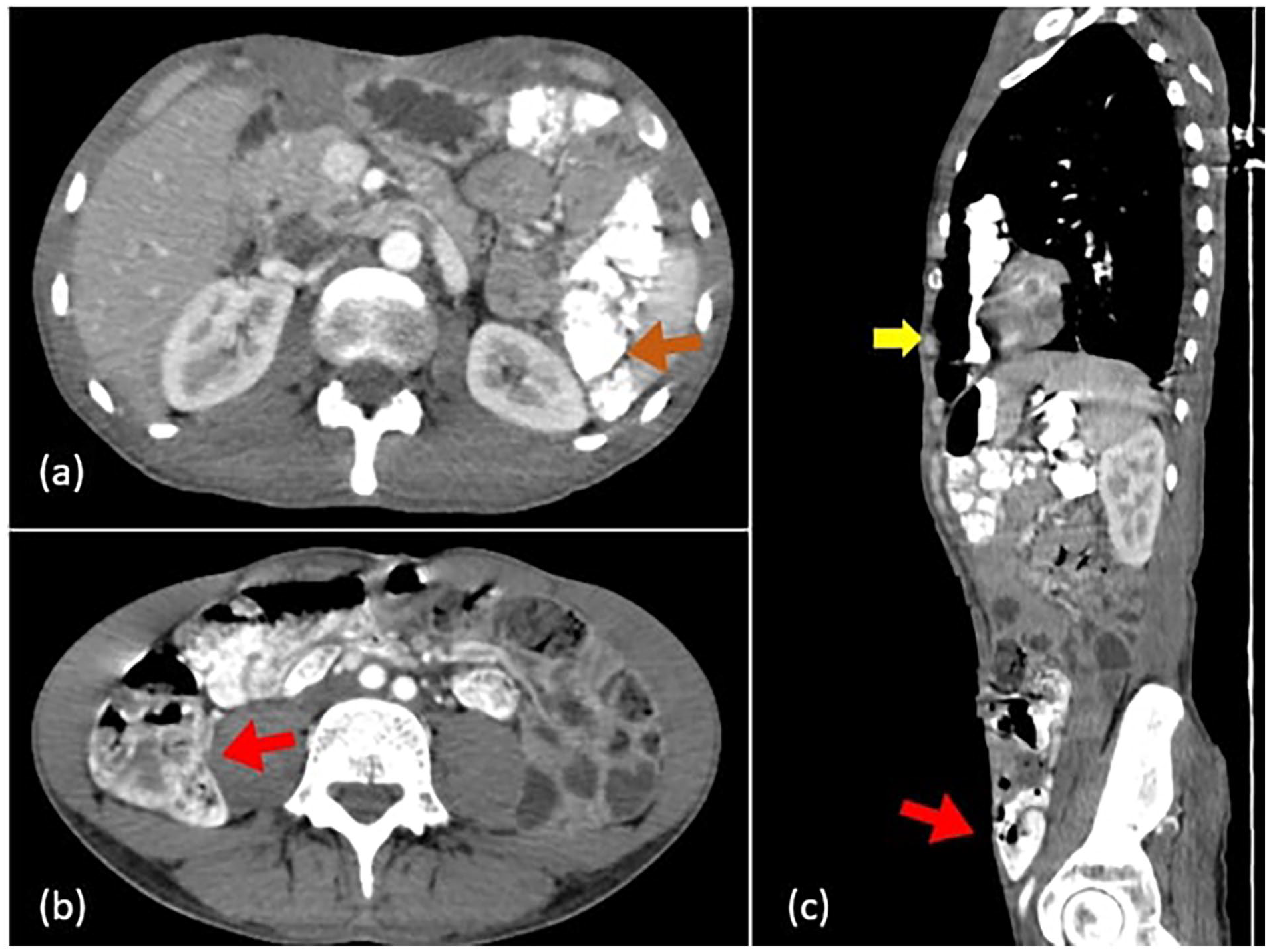
Computed tomography scan with oral and injected contrast mediums, axial (a), coronal oblique (b), and sagittal (c) images showing the oral contrast medium unimpeded passage through the grafted retrosternal colon (yellow arrows) until reaching the colon-jejunal anastomosis (orange arrows). At this juncture, a distinctive “bowel within a bowel” configuration was observed, characterized by concentric rings of high- and low-density layers in axial image (white arrow) and a sausage-like appearance in coronal and sagittal images at the juncture (orange arrows).
After the CT scan (in less than 12 h), the patient spontaneously resumed his intestinal transit. A subsequent CT scan control was performed, revealing a notable improvement in his condition. The previously observed “bowel within a bowel” configuration had disappeared, indicative of a resolution of the obstruction (Figure 2). Additionally, there was a clear progression of the oral contrast medium through the gastrointestinal (GI) tract (Figure 2), signifying restoration of normal bowel function and passage.
Computed tomography (CT) scan with oral and injected contrast mediums after 12 h of the first CT scan, axial image at the level of the anastomosis (a), axial image at the level of the caecum (b) and sagittal (c) image showing the oral contrast medium unimpeded passage through the grafted retrosternal colon (yellow arrows), the colon-jejunal anastomosis (orange arrow), and reaching the caecum (red arrow). And the disappearance of “bowel within a bowel” configuration that was initially observed in the jejunal colonic anastomosis.
The patient, feeling considerably better, declined further investigations, including endoscopy, to rule out underlying masses or ulcers contributing to the intussusception. With no recurrence of symptoms or complications, his condition stabilized and improved. After 2 days of continued observation and with the medical team’s approval, he was discharged. However, due to his refusal to pursue further investigation such as endoscopy, he was advised to return to the emergency room promptly if symptoms recurred.
Discussion
Intussusception in adults is a rare phenomenon, with only 5% of reported cases documented in medical literature, responsible for just 1% of all bowel obstructions. Remarkably, it has never been recorded as a complication following colonic interposition. In the vast majority of instances (90%), intussusception is associated with an underlying pathology, including postoperative adhesions, inflammatory bowel disease, tumors, congenital anomalies such as Meckel’s diverticulum, or even iatrogenically.3,4 Additionally, gastroduodenal intussusception has been reported as a complication following certain types of bariatric surgery, such as gastric plication. 5
Here, we present an exceptionally unusual case where intussusception occurred as a late complication at the site of a functional end-to-end jejunal-colonic anastomosis, 6 years after colonic interposition for corrosive esophageal stricture. This occurrence is exceedingly rare, as evidenced by our search of the PubMed database using keywords “intussusception,” “anastomosis,” and “colonic interposition,” which yielded no relevant articles. Interestingly, we found only one reported instance of intussusception developing at the site of ileocolic anastomosis after laparoscopic right hemicolectomy, occurring on the 9th day post-surgery. 6 And another two cases of post-operative intussusception following free jejunum transfer. 7
Present knowledge suggests that idiopathic intussusception in adults occurs when the circular muscle contracts convulsively, causing it to invaginate into the neighboring relaxed bowel. Factors such as a highly mobile and relatively large diameter of the proximal small intestine can increase the risk.6,7
Unlike in infants, adults with intussusception often present with nonspecific and chronic symptoms. Research indicates that 75% of patients experience obstructive symptoms at presentation, consistent with the current case. 3
Diagnostic imaging reveals characteristic findings. Abdominal ultrasonography may show the “donut sign,” “target sign,” or “multiple concentric ring sign,” all indicative of intussusception. Similarly, abdominal CT scans may reveal the “multiple concentric ring sign,” characterized by concentric circular repeats of high- and low-density layers. These findings aid in the diagnosis, particularly via abdominal CT scans, with the target sign observed in the present case. 8
Treatment typically begins with a barium enema or pneumatic/hydrostatic reduction. 9 In the current case, spontaneous reduction occurred after a CT scan with oral contrast. However, if endoscopic reduction proves challenging, surgery becomes necessary.
Colonic interposition complications
Colonic interposition is a crucial surgical method for managing severe esophageal strictures caused by caustic substance ingestion, prevalent in regions such as Eastern Europe, South America, and Asia due to suicide attempts. 10 Despite prompt treatment, about 85% of patients develop corrosive esophageal strictures, often necessitating esophageal reconstruction to avoid long-term feeding tube dependence. 10 This technique involves using a segment of colon, chosen based on vascular supply and stricture level, for reconstruction, with pioneers establishing its efficacy since the mid-20th century. While offering advantages such as length and acid resistance, colon interposition presents challenges such as lengthy preparation, prolonged surgery, and multiple anastomoses. Complications include early issues such as respiratory problems and transplant necrosis, 11 and late complications such as stenosis and reflux, necessitating complex management strategies, and occasional revision surgeries to ensure long-term success and patient safety.12–15
Post operative intussusception
Postoperative intussusception (POI) in adults is a relatively rare yet increasingly recognized complication following abdominal surgery. While well documented in pediatric practice, where it constitutes up to 11% of all intussusception cases, reports in adult populations have been sparse until recent years. This lack of comprehensive literature has contributed to its underrecognition in clinical settings. 16
POI typically presents with symptoms of partial bowel obstruction within days to weeks after abdominal surgery, including intermittent abdominal pain, nausea, vomiting, and occasionally palpable masses. In contrast to primary intussusception, which often presents acutely with hematochezia and a palpable mass, POI tends to follow a more subacute or chronic course. 16
Studies indicate that approximately one-third of adult patients with intussusception experience it either immediately postoperatively or within 5 years following surgery. This underscores the importance of considering POI in the differential diagnosis of postoperative complications, especially in patients showing signs of bowel obstruction. 16
The pathogenesis of POI is multifaceted, involving factors such as altered bowel motility, surgical manipulation, and the formation of adhesions. Experimental models and clinical observations suggest that postoperative adhesions play a pivotal role in triggering bowel telescoping, particularly in cases lacking an identifiable lead point. Understanding these mechanisms is crucial for guiding therapeutic interventions. 16
Management strategies for POI aim to alleviate obstruction, restore normal bowel function, and prevent recurrence. Initial approaches may include conservative measures such as bowel rest, intravenous hydration, and nasogastric decompression for stable patients. However, surgical intervention such as laparoscopic reduction or bowel resection may be necessary in cases of persistent obstruction, bowel ischemia, or suspected malignancy. 16
In our specific case, the likely lead point for intussusception was identified as the anastomosis site due to the patient’s history of colonic interposition surgery. Peristaltic movements at the surgical site likely contributed to the telescoping phenomenon leading to intussusception. While other causes such as tumor or foreign body could not be entirely ruled out, the patient’s symptoms resolved without immediate intervention.
Consideration of endoscopy post-surgery could have been beneficial to rule out potential causes such as ulceration or residual foreign bodies, although it was not performed in this case due to the patient’s refusal of further intervention. The role of oral contrast in symptom resolution suggests a potential mechanism involving enhanced bowel motility induced by the contrast agent, facilitating spontaneous reduction of intussusception and potentially avoiding more invasive treatments.
Further research is warranted to elucidate the precise mechanisms underlying POI and to optimize diagnostic and therapeutic strategies for this challenging complication of abdominal surgery.
Conclusion
In conclusion, clinicians should remain vigilant of the rare and obscure complication of adult intussusception following colonic interposition. The diagnosis poses a challenge due to the complex anatomy and alteration of the GI tract. While the anastomosis likely serves as the lead point, considering other potential causes through endoscopy could be prudent. This case underscores the importance of thorough evaluation and awareness of GI complications in patients with complex medical histories undergoing esophageal reconstruction and colonic interposition.
Footnotes
Acknowledgements
The authors are grateful for the reviewer’s valuable comments that improved the manuscript.
Author contribution
All authors have accepted responsibility for the entire content of this manuscript and approved its submission.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
