Abstract
Gastric volvulus and wandering spleen are two rare and uncommon conditions. Gastric volvulus is characterized by the rotation of the stomach around itself, causing a closed obstruction. It was first described in the 19th century and is classified according to the axis, etiology, or chronicity. A wandering spleen is defined by the absence of one or all of the splenic ligaments, which occurs either for congenital or acquired reasons. An enlarged spleen may contribute to the wandering spleen and, in turn, lead to gastric volvulus and infarction of the stomach, requiring emergency surgical intervention. In this report, we present a case of a 19-year-old female who presented to the emergency department with severe abdominal pain and epigastric distension. After performing the necessary investigations, she was diagnosed with a wandering spleen and acute gastric volvulus. An immediate laparotomy was performed and both the spleen and the stomach were resected to save the patient’s life at the right time.
Introduction
Gastric volvulus following a wandering spleen is considered one of the rare surgical cases that require immediate surgical intervention because of its danger to the patient’s life. Gastric volvulus occurs when the stomach rotates more than 180° on its long or short axis, which leads to obstruction in the stomach cavity and serious complications such as gastric necrosis, infarction, gangrene, perforation, and death. This condition was first diagnosed in medical literature by Berti, who performed an autopsy of a woman in 1866. 1 Gastric volvulus can be classified into acute and chronic types, but the mortality rate is higher in acute cases, reaching 30%–50%. 2 An ectopic or wandering spleen is a rare condition and unusual entity characterized by abnormal migration of the spleen from its normal anatomical location to the lower abdomen or pelvis. 3 Both gastric volvulus and wandering spleen share a common factor, which is the absence of visceral ligaments within the intraperitoneum. 4
Herein, we report an extremely rare case of acute gastric volvulus and ectopic spleen in a 19-year-old female with no significant medical history. The patient underwent prompt surgical intervention and was discharged in stable condition.
Case presentation
A 19-year-old female presented to the emergency department complaining of epigastric abdominal pain and nausea with no other symptoms.
The pain started abruptly the day before and was gradually increasing throughout the day. The patient’s relatives mentioned a history of non-Hodgkin lymphoma in the patient’s father from 3 years ago. They also mentioned that the patient suffered from bloating and early satiety after meals, approximately twice a month in the last 2 years.
In the emergency room, the patient appeared in acute distress due to pain. Vital signs were significant for tachycardia (130 bpm) and fever (37.5). Blood pressure was within normal ranges and the patient saturated well on room air. A focused physical examination revealed asymmetrical abdominal distension, epigastric tenderness, and a large palpable mass in the left hypochondrium.
Laboratory tests revealed leukocytosis (15,000 WBCs/microliter) and the abdominal X-ray showed a large epigastric air–fluid level as shown in Figure 1.

A simple abdominal X-ray with a lateral view of the diaphragm was performed upon the patient’s immediate admission to the hospital. The X-ray revealed a single large gas–fluid level approximately in the area of the stomach, without the presence of gas distribution in the rest of the abdomen. The lung bases were within normal limits, and there were no other remarkable findings, the arrow indicates the gas–fluid level.
The doctor attempted to insert a nasogastric tube but the procedure failed. After 1 h of admission, the patient developed acute abdominal pain with dyspnea, tachypnea (32/min), and hypoxemia. Both chest and abdominal X-rays were re-performed and revealed severe pneumoperitoneum which suspected viscus perforation as seen in Figure 2. The doctors decided to perform a surgical opening of the abdomen.

A simple chest X-ray, obtained 2 h after the patient’s admission, revealed large gas crescent signs of the lateral aspects of the diaphragm and outlined the anatomical configuration of the liver on the right side (pneumoperitoneum), with the gas–fluid level remaining in the epigastric area but with a smaller size as the arrows show. The remainder of the image was within normal limits (a). A simple abdominal and pelvic X-ray obtained several hours after the patient’s admission showed the gas–fluid level, pneumoperitoneum, and the absence of gas distribution in the rest of the abdomen (b).
The Surgical Procedure: An exploratory laparotomy was performed with a midline incision and the doctors found a bulky and huge wandering spleen reaching the pelvis and the right iliac fossa, as seen in Figure 3. In addition, the stomach was completely necrotic and gangrenous, and a gastric fundal rupture of 5–7 cm in diameter was detected. The peritoneal cavity was full of food debris, mucosal, and necrotic clots. An organoaxial gastric volvulus due to a large wandering spleen was confirmed as the first cause. A splenectomy, total gastrectomy with esophagojejunal anastomosis, duodenal stump closure, and Roux-en-Y jejunojejunostomy were performed. In addition, the technique of temporarily feeding jejunostomy was performed.
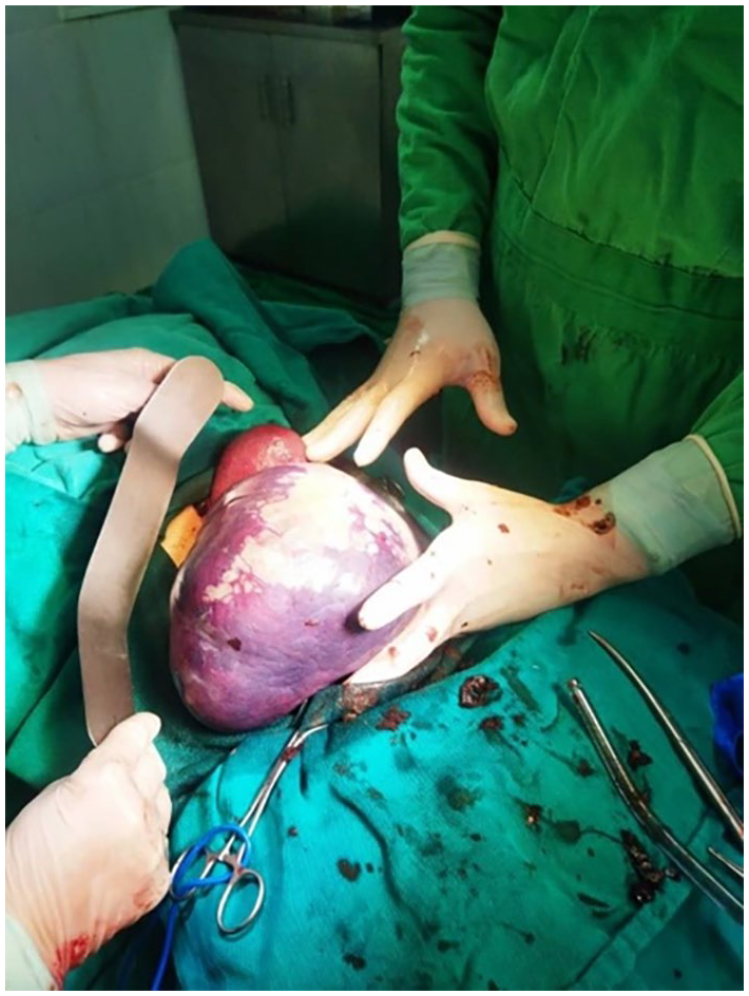
A large bulk spleen was seen in the exploratory laparotomy.
Postoperatively, we followed up with the patient who received IV fluids, total parenteral nutrition, broad-spectrum antibiotics, and albumin along with daily laboratory monitoring, enabling jejunostomy feeding from day 5. An excisional biopsy and tissue studies were performed on the patient and they were normal, the biopsy did not show any abnormalities in the cells.
The patient was discharged home after 2 weeks with the following recommendations:
(1) Removing the feeding tube after 4–6 weeks, performing contrast radiography.
(2) Following up with a nutritionist to make an appropriate nutritional program that suits the condition.
After that period, the patient’s symptoms gradually improved, and we did not notice any relapses or complications.
Discussion
Gastric volvulus, a rare and life-threatening surgical condition, demands swift diagnosis and immediate surgical intervention due to its potentially fatal consequences. 5 It involves the abnormal rotation of the stomach by more than 180°, leading to a closed-loop obstruction. The first recorded observation of this condition dates back to 1866 when Berti examined a deceased woman’s corpse. However, it was not until 1896 that Berg performed the first successful surgical repair on a patient with gastric volvulus. Later, in 1920, Rosselet provided a comprehensive systematic and radiological description of the condition. 6 Gastric volvulus is categorized based on the axis of rotation, primary and secondary causes, and chronicity. The axis-based classification comprises four types. The first type, organoaxial volvulus, involves the stomach rotating on an axis shared by the pylorus and the gastroesophageal junction. This type is associated with complications like diaphragm defects, necrosis, or stomach strangulation. The second type, mesenteroaxial volvulus, occurs when the mesenteric axis branches into the greater and lesser curvatures of the stomach, leading to typical and chronic clinical features and diaphragm defects. 7 The third type, termed mixed, combines features from the first two types and is the rarest. The fourth and final type, unclassified, accounts for 10% of cases. In terms of etiology-based classification, primary causes are largely unknown, while secondary causes are attributed to anatomical issues or problems in adjacent organs such as the spleen. However, the exact cause remains obscure in most cases. 8 Gastric volvulus occurs in infants, children, adults, and in both sexes and for all races, with a peak occurrence in the fifth decade of life. 9 As described by Borchardt, the typical symptoms of gastric volvulus include epigastric pain, nausea, and an inability to insert a nasogastric tube, which he termed the classic triad in 1904. These symptoms were consistent with our case and prompted suspicion when the doctor attempted to intubate the patient unsuccessfully after multiple tries. 2 In many previous cases (look at Table 1) documented in medical literature, computed tomography was often regarded as the most precise diagnostic method. However, in our situation, we opted for a plain abdominal X-ray, which revealed a significant gas–liquid level in the epigastrium. This decision was driven by the urgency to act swiftly and save the patient’s life. When it comes to addressing gastric volvulus, there are two main options: surgery or conservative treatment. It is important to note that conservative treatment carries a significant risk of gastric perforation. Therefore, surgical intervention, either through laparotomy or laparoscopy, serves as the primary approach. In cases where serious complications like gastric perforation or gangrene are present, partial or total gastrectomy is often considered the optimal treatment. 10 In our case, because of the presence of necrosis and gastric gangrene, we performed a total gastrectomy with jejunal anastomosis, utilizing a gastric tube and closing the esophageal hiatus, along with jejunojejunal anastomosis. Wandering spleen is an uncommon condition that arises from the absence of one or more splenic ligaments, allowing the spleen to move to the pelvis or any part of the abdomen. It can occur at various ages but is more prevalent in infants under 1 year old due to developmental issues during fetal life. In adults, it may result from splenic enlargement or pregnancy in females. 11 So far, about 500 cases of wandering spleen have been reported in the medical literature. 12 In a prior case report, authors presented a case of wandering spleen in a woman with Hodgkin’s lymphoma, implying a potential link between lymphoma and wandering spleen. This connection is further underscored by our patient’s family history; her father has non-Hodgkin’s lymphoma. Consequently, there is a necessity to monitor our patients closely, as the presence of a wandering spleen may serve as an early indicator of lymphoma development. 13 Wandering spleen is treated either by fixation or splenectomy and due to its association with gastric gangrene, splenectomy was the appropriate choice in our report.
Illustration for some coexistent acute gastric volvulus and wandering spleen cases.

Conclusion
Severe abdominal pain is an emergency condition that requires rapid diagnosis and urgent surgical intervention in general. Gastric volvulus and wandering spleen are two rare conditions associated with a very high mortality rate. The two conditions share the absence of peritoneal ligaments. We highlight in this case the need for more studies to understand the relationship between lymphoma and wandering spleen, as well as the importance of the time factor in treatment.
Footnotes
Acknowledgements
None.
Correction (July 2024):
The article has been updated to correct the heading style of “Discussion”.
Author contributions
H.H., K.A., T.A., J.A., M.A., and H.M., have participated in writing the manuscript and reviewing the literature. H.H. and K.A. critically and linguistically revised the manuscript. T.G. conceived and supervised the conduct of the study. All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval to report this case was obtained from the Faculty of Medicine at the University of Kalamoon with a serial number (669/24).
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
