Abstract
Perifolliculitis capitis abscedens et suffodiens, also known as dissecting cellulitis of the scalp, is a rare, chronic suppurative, inflammatory head hair follicle disease, which seriously affects the patient’s quality of life. Clearly, clinical treatment varies widely and is somewhat challenging. We report a case of a 19-year-old male patient who had good results through surgery combined with photodynamic therapy. Surgery combined with photodynamic therapy for perifolliculitis capitis abscedens et suffodiens is effective and safe, especially for patients with poor responses to previous traditional treatments.
Introduction
Perifolliculitis capitis abscedens et suffodiens (PCAS), also known as dissecting cellulitis of the scalp, is a chronic suppurative, inflammatory head hair follicle disease that manifests as fluctuating painful nodules of the scalp, abscesses, pus, sinuses, scarring, and cicatricial alopecia.1,2 Unknown etiology, similar to hidradenitis suppurativa, acne conglobata, including follicular hyperkeratosis, follicular duct obstruction, dilation and rupture, bacterial overgrowth, followed by neutrophils, histiocytes, lymphocytes, plasma cell infiltration and granulomatous inflammatory response, scarring, sinus tract formation, and later fibrosis.3,4 The clinical treatment is challenging, and the practice is quite different. The commonly used treatment methods include oral antibiotics, isotretinoin, hormones and other drugs, TNFα inhibitors, X-rays, lasers, and surgical resections, all of which have varying degrees of effect, but there are drug resistance, recurrence, or systemic side effects in all treatments. 5 In recent years, the use of 5-aminolevulinic acid photodynamic therapy (ALA-PDT) has good therapeutic effect on patients with poor drug therapy for PCAS.6,7 We report a case of successful treatment of PCAS with surgery combined with photodynamic therapy.
Case report
A 19-year-old Chinese male patient visited the Department of Dermatology of Guizhou Guiqian International General Hospital in Guiyang, China, for more than 1 year of scalp papules and pustules with pain.
Examination found multiple scattered nodules and cysts on the head, with obvious fluctuations, accompanied by pain and tenderness symptoms, the top of the head and the back of the occipital were heavier, and some of them fused to form a sinus (Figure 1). Squeeze gently on the lesion, and purulent and bloody secretions can be seen flowing out, and there is no obvious rash on the face, armpits, groin, or other parts.

Abscesses and nodules can be seen merging on the head to form sinus tracts and sulcus-like structures.
Apart from elevated white blood cell and neutrophil counts, routine laboratory tests and imaging showed no abnormalities. Prior treatment with antibiotics such as doxycycline and cefuroxime, as well as oral isotretinoin, yielded unsatisfactory results.
Complete relevant preoperative examinations after hospitalization rule out surgical contraindications and perform surgery under general anesthesia. Thoroughly dissect nodules and abscesses, fully dissociate the galeal aponeurotic layer, open sinuses, completely remove necrotic tissue and pus, and rinse with normal saline On the wound surface, a scalp clip is used to fix the edge of the incision to reduce intraoperative bleeding. The scalp is turned over and fixed on the surrounding normal scalp with sutures (Figure 2). The bleeding point is electrocoagulated. After checking that there is no active bleeding, a 20% concentration of 5-ALA solution is prepared. The 5-ALA was incubated on the inside of the scalp, protected from light for 3 h, and then irradiated with a narrow-band red light (633 ± 10 nm, LED-IB, Wuhan Yage photoelectric technology Co., Ltd, China), and part of the sinus area was irradiated with optical fiber for 30 min, with an energy intensity of 100 mw/cm2 (Figure 3), after the end of photodynamic therapy, the wound was washed again with normal saline, the scalp was turned over to its original position, a negative pressure drainage tube was placed, and local intermittent sutures were fixed. The drainage tube was removed 48 h after the operation. After the operation, the patient only experienced tolerable pain, the pain did not exceed 48 h, and there was no other adverse reaction. Three months after the operation, the patient’s abscess and nodules improved significantly (Figure 4), and he was very satisfied with the treatment results.
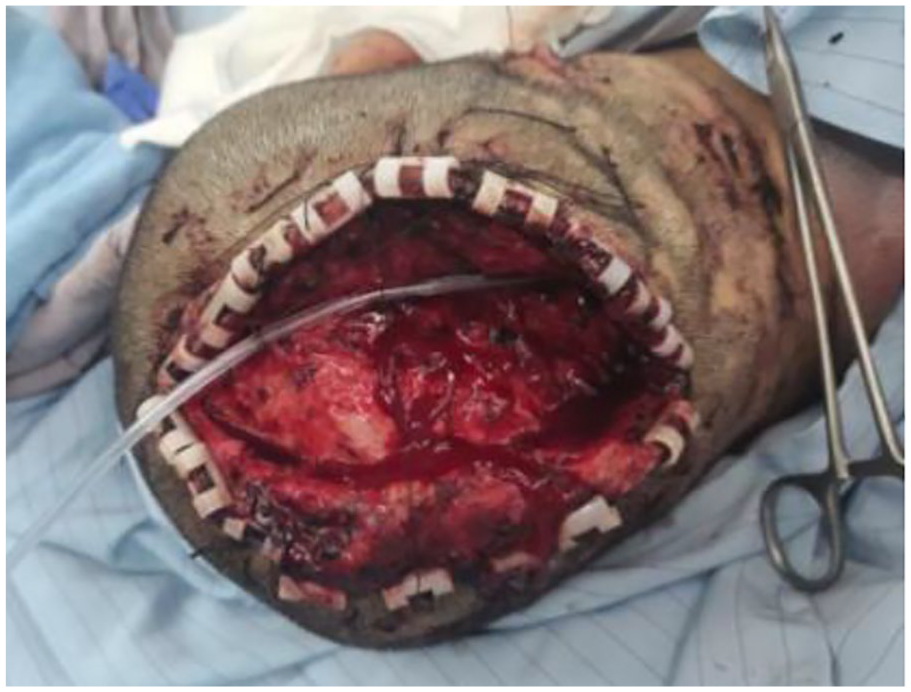
The scalp is fixed, the infected wound is exposed for easy application of medicine, and high-energy red light is irradiated.

Photodynamic therapy (20% concentration of 5-aminolevulinic acid solution (Shanghai Fudan Zhangjiang Bio-Pharmaceutical Co. Ltd. Shanghai, China)), applied to the inner side of the scalp, protected from light for 3 h, then 633 ± 10 nm Large spot irradiation, part of the sinus area combined with optical fiber irradiation for 30 min, the energy intensity is 100 mw/cm2.

Three months after surgery combined with 5-aminolevulinic acid photodynamic therapy treatment.
Discussion
PCAS is a rare chronic, inflammatory disease of head hair follicles of unknown etiology. The cause of the disease is unknown, and it has certain genetic factors. At present, it is believed that this disease is related to hyperkeratosis of hair follicles and pilosebaceous unit occlusion, followed by dilatation and rupture of hair follicle ducts, and the release of its contents, such as keratin and bacteria, leading to the emergence of neutrophilic and granulomatous inflammatory reactions, the formation of abscesses, etc.3,4 The pathological manifestations are characterized by folliculitis and perifollicular inflammation, accompanied by the infiltration of dense lymphocytes, histiocytes, and multinucleated cells, the formation of abscesses, and granulomatous inflammation in the deep dermis and subcutaneous adipose layer, etc., resulting in follicular sebaceous units and skin appendages damages, leads to a series of clinical manifestations such as nodules, cysts, sinus tracts, and fibrosis.2,3 It can occur alone or as part of follicular occlusion tetrad, namely PCAS, acne conglobata, hidradenitis suppurativa, and pilonidal sinus. 8
The treatment of PCAS is challenging, and the clinical treatment varies greatly, causing varying degrees of distress to both doctors and patients. 3 Oral isotretinoin is a clinically used treatment method, but the therapeutic effect is limited and there is a certain recurrence rate. 8 Considering that PCAS and hidradenitis suppurativa have a similar pathogenesis, in patients with hidradenitis suppurativa in the skin, elevated levels of TNF-α, IL-1β, and IL-10 can be detected.3,8 TNF-α inhibitors are used clinically, such as adalimumab, infliximab, etc., and the treatment of PCAS has improved to varying degrees.9,10 Oral zinc preparations can reduce NF-kB-mediated inflammatory response, 4 other treatments include oral antibiotics, including doxycycline, minocycline, clindamycin, rifampicin, dapsone, etc. alone or in combination with isotretinoin treatment, etc., all have different degrees of improvement, but they are prone to relapse after drug withdrawal,8,11 X-ray irradiation, ND:YAG laser, photodynamic therapy, surgery, and other methods have also been used in the treatment of PCAS. 5
5-ALA is the precursor of porphyrin and other photosensitizers. Under the irradiation of a specific excitation light source, it can generate reactive oxygen species and other substances, and play a photodynamic effect. 6 In the treatment of acne, mediated photodynamics can inhibit sebaceous gland activity, reduce sebum secretion, significantly inhibit the expression of inflammatory cytokines IL-1α, TNF-α, IL-8, etc. inhibit the proliferation of keratinocytes, and induce apoptosis, death, reduce hair follicle blockage, and have the characteristics of broad antibacterial spectrum.12–14 At the same time, red light can also stimulate matrix metalloproteinases, promote collagen reconstruction, and promote skin lesion repair and healing. In view of the fact that PCAS has similar pathophysiological processes with acne and hidradenitis suppurativa, it provides a certain theoretical basis for the treatment of PCAS. Ye et al. 7 first used ALA-PDT to treat refractory PCAS and achieved good results. Yuxin et al. 15 and Hao et al. 6 used pyonex and 22G needles to perform acupuncture on the head lesions to facilitate drainage of secretions and the penetration of ALA (Shanghai Fudan Zhangjiang Bio-Pharmaceutical Co. Ltd. Shanghai, China), and photodynamic therapy after drug application has achieved good therapeutic effect on patients whose previous traditional drug treatment was not effective.
Cui et al. 1 combined with photodynamic therapy for PCAS after flipping the scalp through skin surgery had a good therapeutic effect without obvious adverse reactions. Considering the limited penetration depth of ALA-PDT, in patients with PCAS, the smallest protruding nodule can reach a depth of 8 mm. 3 In our case, the necrotic tissue was fully and completely removed through surgery, and the scalp was turned over and fixed. The application of ALA and light irradiation makes photodynamic therapy more precise, effective, and direct, achieving a faster and more obvious therapeutic effect.
Each case of PCAS is different, and individualized treatment depends on the severity of the condition and the patient’s willingness to treat, ranging from topical application of benzoyl peroxide, clindamycin, isotretinoin, oral steroids, antibiotics, retinoic acid drugs, intralesional injection of hormones into biological agents, lasers, X-rays, photodynamics, and surgery,5,16 through single or combined treatment so that patients can achieve a better therapeutic effect, surgery combined ALA-PDT is suitable for more serious patients, 4 and it is effective for patients who have not responded well to previous oral medications, offering quick and notable results.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Consent was obtained from the patient for publication of this case report and images.
