Abstract
Herpesvirus reactivates from a latent infection in older adults and critically ill and immunocompromised individuals. Herpes zoster ophthalmicus (HZO) is a latent infection that affects the fifth cranial nerve. It is an infrequent cause of increased intraocular pressure. We present the case of a 50-year-old man with a reactivation of latent varicella-zoster virus infection involving the ophthalmic branch of the fifth cranial nerve. The patient was initially managed as an outpatient with an antiviral, but his clinical evolution worsened and required urgent surgical decompression. Lateral canthotomy was performed with cantholysis of the inferior crus of the lateral canthal tendon. Only partial decompression was achieved, so cantholysis of the upper crus was performed with significant tissue tension release. The patient evolved well and was discharged after 6 days without symptoms for outpatient management.
Introduction
Orbital compartment syndrome (OCS) is a sudden increase in intraorbital pressure (IOP) that can reduce blood flow to the retina and optic nerve. If left untreated, vision loss may be irreversible. 1 The most relevant symptoms are oedema, periorbital pain/tension, proptosis, limitation of extrinsic ocular mobility, and decreased visual acuity.
Acute bleeding, trauma, or iatrogenic (particularly during bulbar procedures) are common causes of OCS. Orbital tumors, abscesses, cellulitis, oedema, or emphysema are less frequent causes. 2 The normal orbital volume is approximately 30 mL, and IOP is less than 20 mmHg.2–5
The orbital cavity is pyramidal, with the optic foramen at its apex. Its quadrangular base has rigid bony edges and walls that limit its capacity for expansion. IOP tends to be released anteriorly; however, it is contained by soft tissues with different levels of fixation and retention, such as the orbital septum, the orbicularis muscle system, the eyelids, and their fixing ligaments. The canthal ligaments have the greatest orbital containment force.
Herpes zoster (HZ), a rare cause of OCS, is characterized by the onset of stabbing pain or unilateral itching along the affected dermatome. Days later, redness and a vesicular rash, pathognomonic findings, appear. This condition results from latent varicella-zoster virus infection reactivation in the dorsal root ganglia.
Herpes zoster ophthalmicus (HZO) is a varicella-zoster infection in the trigeminal ganglion involving the ophthalmic branch. 6 Ocular involvement occurs in 20%–70% of patients with HZO and can manifest with blepharitis, keratoconjunctivitis, iritis, scleritis, and acute retinal necrosis. 7 Neurological complications are less common than ocular complications and may include ophthalmoplegia, optic neuritis, ptosis, and orbital apex syndrome.
An IOP for 60 to 100 minutes causes permanent vision loss.2,8,9 Emergency decompression should be performed if IOP > 40 mmHg.2–4,10,11 The treatment of acute OCS is lateral canthotomy (LTC) and cantholysis (LC) of the inferior crura of the lateral canthal ligament. Timely decompression reverses OCS and fundamentally preserves vision.
We present an unusual case of a patient with OCS secondary to HZO complicated by a large abscess in the eyelid and lower temporal fossa on the left side. Its unusual evolution and surgical treatment are described.
Case presentation
The patient is a 50-year-old man, a prison inmate with a history of smoking and moderate alcoholism. The latter was suspended 2 years ago. In addition, psoriasis for 10 years treated with prednisone 50 mg every 24 hours. Two weeks before hospitalization, he began with a fever and a mild burning pain on the left forehead. Three days later, he developed a blistering rash on the upper eyelid. The prison doctor indicated treatment with acyclovir 200 mg orally every 8 hours for 7 days.
Over the next 7 days, new vesicles appeared, with some progressing to scabs. The patient also presented dysesthesia and mild swelling of the lower forehead and upper eyelid with increased local temperature. The patient was brought to the ophthalmology service of our hospital.
Initial diagnostic intervention by ophthalmology
Based on the evolution and distinctive features of the well-defined skin lesions, HZO was diagnosed. The antiviral dosage was modified to an optimal dose of 800 mg 5 times daily for 7 days and subsequent outpatient management. During the following 5 days, palpebral oedema increased, and the patient returned to the ophthalmology service. On physical examination, cellulitis was found with great tension oedema involving the lower part of the forehead and the upper left eyelid, causing ptosis and total ocular closure with displacement of the ciliary edge at the level of the infraorbital rim. Tension oedema extended to the lower temporal fossa with a fluctuating central area (Figure 1). Ocular examination revealed chemosis, severe conjunctival hyperemia, and ophthalmoplegia with a significant reduction in eye movements. His visual acuity was RE 20/20, LE 20/50, and IOP, RE 13 mmHg, LE 32 mmHg.
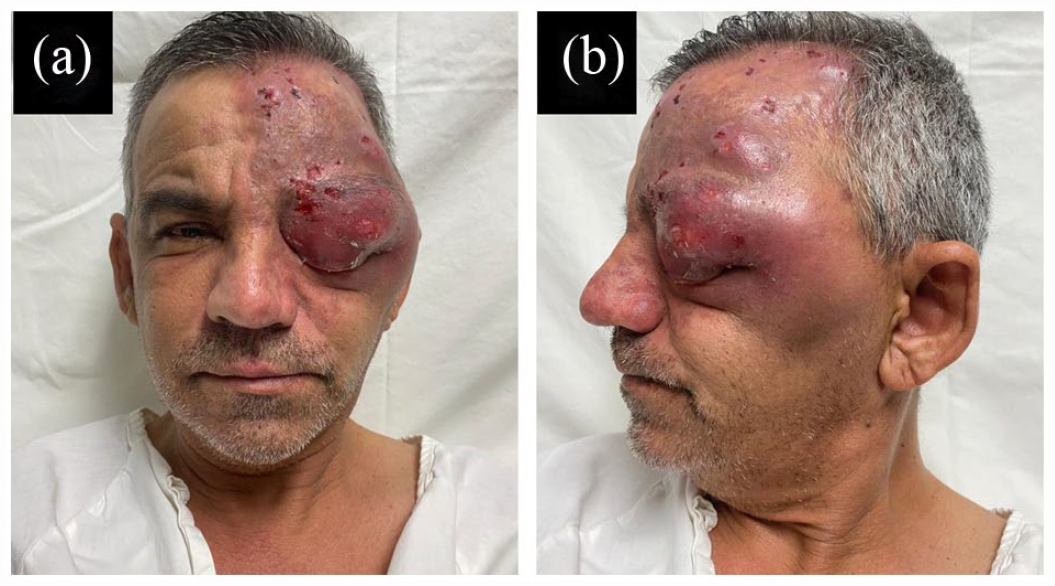
Clinical appearance of the patient before emergency surgery. (a) Fifty-year-old male with large edema and abscess of the left frontal and orbital area. (b) Close-up of the previous image that shows the lesions in different stages of Herpes Zoster in the affected area.
A magnetic resonance imaging (MRI) scan showed left proptosis (an interzygomatic line to the sclera of 24 mm conditioned by obliteration of extra and intraconal fat with involvement of the lacrimal gland; a thickened left trigeminal nerve, and the optic nerve in the intraorbital and intracanalicular segment with neuritis) (Figure 2). A diagnosis of OCS was made. A plastic surgery consultation was requested.

(a) MRI shows large edema’s extension with a temporal abscess in the left side. (b) MRI shows left proptosis.
Plastic and reconstructive surgery treatment
Urgent surgical decompression was indicated. LTC was performed using an extended approach (2 cm) just beyond the lateral orbital rim. An initial LC of the lower pillar was performed using Littler scissors. Partial decompression was achieved, so an LC of the upper pillar was performed, quickly achieving significant tissue tension release (Figure 3). An abscess was drained, obtaining 25 mL of secretion, which was sent for culture. At the end of the procedure, the patient partially recovered ocular movements and sensitivity in the V1 cranial nerve.

Transoperative view. (a) Cantholysis of the upper pillar of the canthal tendon. (b) Cantholysis of the lower pillar of the canthal tendon. (c) Drawing representing both cantholysis.
The patient was hospitalized for surveillance and medication. Vancomycin 2 g intravenous (IV) every 12 h, acyclovir IV, ophthalmic ointment with ciprofloxacin, lubricants, and steroid drops were prescribed. Culture reported Methicillin-resistant

Clinical appearance of the patient 2 weeks after procedure. (a) Temporary ptosis of the left upper eyelid. (b) Residual hyperpigmentation of the affected area can be seen.
Discussion
This case is an OCS secondary to HZO complicated by a large soft tissue abscess. The torpid evolution could be associated with initial treatment with antivirals at a suboptimal dose, in addition to chronic use of prednisone and other variables such as personal hygiene, diet, and the environment within the prison. It is important to note that multidisciplinary management must integrate a comprehensive treatment.
Patients who present retinal ischemia for more than 90–120 min have a high risk of presenting permanent blindness. 10 In our case, the IOP was 32 mmHg for approximately 110 min. Undoubtedly, the timely surgical treatment prevented a progressive increase in IOP and the latent complication of blindness. Consensus establishes that LTC and LC should be performed once OCS has been diagnosed. 11 An LTC alone can reduce the IOP by approximately 14 mmHg; LC alone can reduce pressure by approximately 19 mmHg. Combined, they can achieve a pressure reduction of up to 30 mmHg.2–5
We did not find a similar case of active HZ-related OCS complicated with HZO. The unusual evolution conditioned great inflammation and an abscess in the palpebral and temporal areas. Lima et al. documented 77 cases of OCS. Of these, 81% occurred in patients older than 20 years; 45% were secondary to trauma, and 32% to surgery. 2 We found 12 HZO case reports. Four were reported rare complications of HZO with apex syndrome. In our case, it was due to the patient’s pre-existing condition of being a carrier of HZ.
HZ has a global incidence of 20% to 30%. HZO occurs in 10% to 20%. Its challenging ocular complication, OCS is a rare entity, occurs in 3.5% to 10% of cases. Urgent orbital decompression via LTC and inferior LC continues to be the gold standard of treatment. In this case, performing LC of the upper crura was also necessary. In others, inferomedial orbital bone decompression may be indicated.
We consider this a truly atypical case due to the affected areas, the great dimension of oedema, and the infectious process. Adequate recognition of progression and multidisciplinary management allowed us to act promptly to prevent complications or serious sequelae.
Footnotes
Acknowledgements
We thank Sergio Lozano for his review of the manuscript, and the patient and the hospital staff for their help.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The patient gave his authorization for surgery and research exposition.
