Abstract
Eccrine angiomatous hamartoma is a rare, benign condition. Patients typically present with a solitary, sometimes enlarging nodule of the extremities usually appearing at birth or arising during childhood. Eccrine angiomatous hamartoma is usually sporadic, but one familial case of the multifocal variant has been reported. It is recognized histologically by increased numbers of eccrine elements as well as numerous vascular channels and proliferation of other dermal elements such as adipose tissue and hair follicles. When symptomatic, eccrine angiomatous hamartoma may be associated with hyperhidrosis or pain. We report a case of a 52-year-old woman with eccrine angiomatous hamartoma on the face and share our experience with botulinum toxins in the treatment of this condition.
Introduction
Eccrine angiomatous hamartoma (EAH) is a rare, benign malformation that is usually congenital or prepubertal and there is no preference related to patients’ sex. It presents as a solitary flesh-colored lesion, either asymptomatic or causing mild pain, and hyperhidrosis on extremities. Enlargement typically occurs commensurate with growth of the patient’s limb. Histologically, an increased number of sweat glands (eccrine) and numerous capillaries characterizes EAH. The condition is usually benign and requires no intervention unless the patient is bothered with the shape and hyperhidrosis. At this point, surgical intervention is established. Dermatologists have used botulinum toxins to treat many EAH cases successfully.
Case report
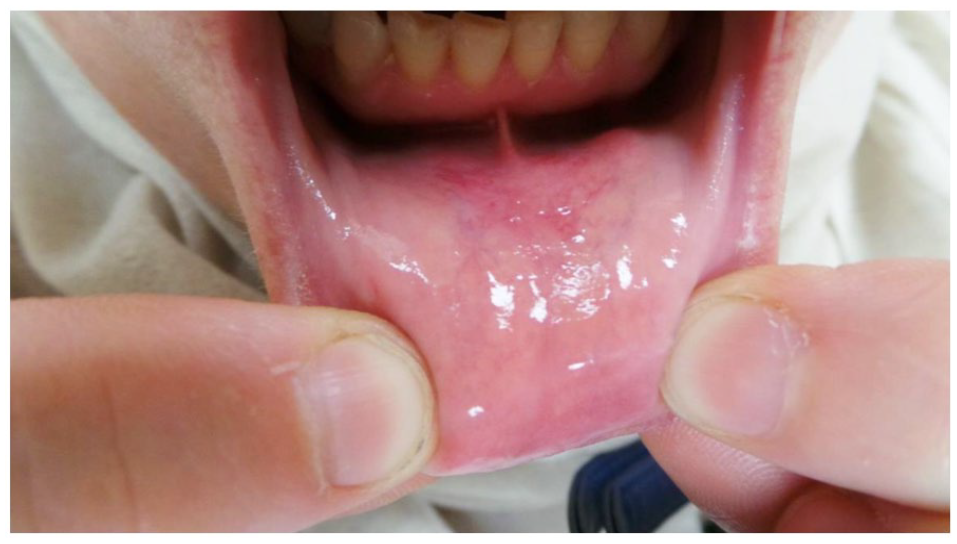
A previously healthy 52-year-old woman presented to the clinic with a lesion on the chin. She reported that the lesion started as pinkish plaques 7 years ago. The lesion slowly enlarged and became tender to touch. The color changed from pink to purple with overlying telangiectasia and increased perspiration associated with the lesion. As the lesion was enlarging, it interfered with speech. On physical examination, we noticed a pinkish infiltrated plaque on the chin with overlying telangiectasia. The plaque was about 4 × 4 cm (Figures 1 and 2). There is extension of the lesion into the intraoral gingival mucosa (Figure 3). Her general and systemic examination were normal.

A bulky poorly circumscribed flesh-colored tumor, around 4 × 4 cm2, infiltrating the chin with overlying telangiectasia.

Lateral view of the lesion, showing its multi-lobulated nature.
Iodine-starch test of the lesion, showing profuse hyperhidrosis.
An iodine starch test has been used to confirm hyperhidrosis overlying the lesion. Figure 4 depicts where a 5-mm punch biopsy was taken from the lesion and the histopathology examination revealed nodular clusters of dilated vessels intimately associated with an increased number of mature eccrine glands while the epidermis is unremarkable as shown in Figures 5 and 6.

H&E stain shows nodular clusters of dilated vessels intimately associated with an increased number of mature eccrine glands while the epidermis is unremarkable.

Closer view shows ectatic blood vessels admixed with dilated sweat glands and mature fat cells.

Figure shows fat cells in the dermis admixed with multiple eccrine glands and ectatic blood vessels.
The constellation of clinical and pathological features is consistent with the diagnosis of EAH.
The pain and hyperhidrosis moderately improved after injecting the lesion with 30 U botulinum toxin diluted in 2.5 mL normal saline in superficial dermis.
Discussion
EAH is a rare, benign condition that is usually congenital or arises during prepubertal years, 1 though it has also been reported in older patients. 2 Our case involves a 52-year-old woman presenting with EAH. The unusual location of EAH in this case and the paucity of its mention in the literature prompted us to report this case. The infiltrated plaque presented on the face, particularly the chin.
EAH was first described by Lotzbeck 3 as an angiomatous-appearing lesion on the cheek of a child. True incidence is yet unknown. It is a rare, benign tumor characterized by proliferation of eccrine and vascular components. It usually presents as a solitary lesion; however, multiple lesions have sometimes been reported. 4 Generally, the lesions enlarge very gradually; more rapid growth and pain during pregnancy and adolescence have been described and suggest hormonal influence. 5 Other authors have suggested that fluid retention associated with menstruation and pregnancy might cause the pain. 5 Eighty percent of the cases were reported over the extremities, 2 with a predilection for palms and soles. The exact pathogenesis is unknown; however, various theories like abnormal induction of heterotypic dependency with resultant malformation of adnexal as well as mesenchymal elements have been proposed. 6
The hamartoma is usually asymptomatic, but some patients experience pain due to infiltration of the small nerves. The vascularity in the lesions may raise the temperature 7 and induce hyperhidrosis as in our case. Since hyperhidrosis is a relatively common finding associated with this condition, various other terms have been used to describe this entity, including sudoriparous angioma 8 and functioning sudoriparous angiomatous hamartoma. 9 Focal hypertrichosis and the association of EAH with Cowden’s syndrome, 10 and neurofibromatosis 11 have all been reported.
Radiographic modalities such as magnetic resonance imaging and ultrasound may help to confirm clinical suspicion of an angioma, but accurate diagnosis of EAH remains with histology. 7
The histopathologic hallmarks of EAH include the presence of an increased number of eccrine glands in the mid- and lower dermis along with ectatic or collapsed vessels that are seen in close approximation to the hyperplastic eccrine units. The overlying epidermis may be normal or may show acanthosis or papillomatosis.1,12
Physicians should consider other differential diagnoses when dealing with EAH, such as eccrine nevus, blue rubber bleb nevus syndrome, tufted angioma, glomus tumor, smooth muscle cell hamartoma, nevus flammeus, and angioma serpiginosum.13–15 Although aggressive treatment is generally unwarranted, simple excision is usually curative. Recently, botulinum toxin 16 and intralesional sclerosants 17 have been successfully used in the treatment of this condition.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The authors certify that the patient has given her consent for her images and other clinical information to be reported in the journal.
