Abstract
Foreign body anywhere in the body can be a diagnostic challenge to a doctor, especially if it is wooden and hardly symptomatic. A foreign body in the parotid gland, whether from the oral cavity or through the skin is extremely uncommon. We are presenting a case of a wooden foreign body in the parotid gland of a 61-year-old patient who did not want to be examined or treated initially as it was not causing him any troublesome symptoms.
Keywords
Introduction
Foreign body (FB) of the parotid gland is not very commonly seen. Toothbrush bristles, slivers of finger nails, wood splinters, hair, blades of grass and fish bones have been reported. 1
Usually, the cause of such an injury is work accident or firearm injury. 2 FBs can penetrate directly through the skin or they can reach the gland through the salivary gland ducts leading to complications such as sialocele, cutaneous fistulas and facial paralysis.2,3 FB retention in the gland secondary to penetrating injury is an even rarer clinical entity. 2
A PubMed search using the keywords ‘foreign body’ and ‘parotid gland’ could only reveal 24 such cases.
Computed tomography (CT) imaging is best for detecting deeply lodged wooden foreign 4 bodies. Prophylactic antibiotics need to be started as wooden FBs, being dirty, can be a nidus for growth of microorganisms. Surgical removal of the FB has to be done in order to get a complete cure. 5 We are presenting a case of a wooden FB in the parotid gland in a 61-year-old patient with history of trauma, who did not want to be examined or treated initially as it wasn’t bothering him much but later on underwent surgery to remove it.
Case report
A 61-year-old male with fracture of right femur was referred from the department of orthopaedic surgery with complaints of painless discharge from the right preauricular region since last 3 days. He was reluctant to give detailed history or get examined as his major concern was the fractured painful right leg. After much deliberation about the possibility of a deep wound and its complications, he consented to give proper history and get evaluated. He gave history of fall on ground when walking at night about 5 days back but did not remember of any trauma over his right face.
On inspection, there was about 5 mm opening anterior to the right tragus with pus oozing out. There was also some crust around the opening (Image 1). There was minimal swelling around the wound and no other opening was visible. On palpation, the local skin temperature was not raised. The region anterior to the opening was mildly tender and firm on palpation. Pus came out from the opening on applying pressure in the parotid region. The opening of the ipsilateral stensen’s duct appeared normal and there was no pus or discharge coming through it. There were no palpable neck nodes. All the peripheral motor branches of the ipsilateral facial nerve were intact. Ear, nose and intra-oral examination were uneventful. There was no trismus.
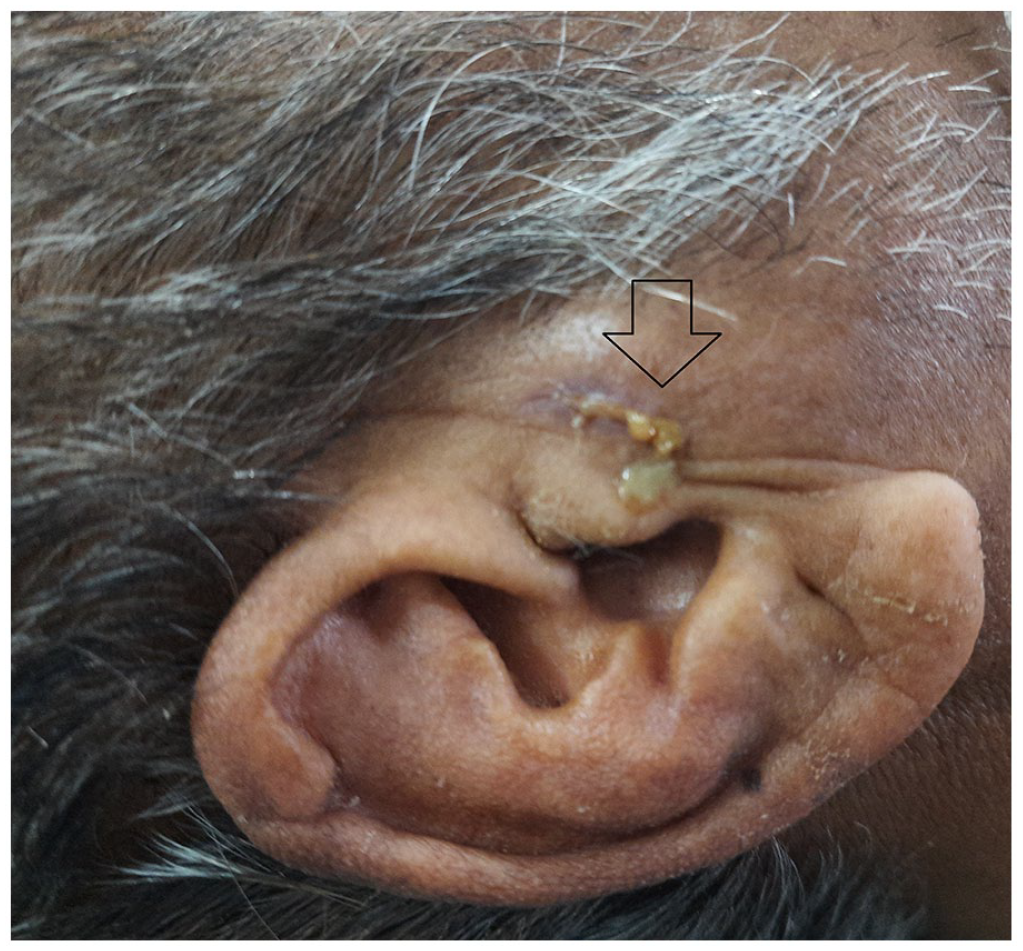
Entry wound of the foreign body in the right preauricular region with pus extruding from the opening as shown by the arrow.
Suspecting an FB impaction, a contrast enhanced CT (CECT) scan of right parotid region was done for further evaluation. It showed a linear hypodense lesion, probably an FB, measuring 5.2 cm, extending from the right preauricular region and traversing the anterior part of parotid gland, running anteroinferiorly and reaching the masseter muscle. Right masseter muscle was bulky. There was minimal collection in the right cheek anterior to masseter muscle (Images 2 and 3).

Axial CT scan of the head showing a linear hypodense shadow extending from the right preauricular region and traversing the anterior part of the parotid gland as shown by the black arrow.

Axial CT scans of the head in continuity showing the linear hypodense shadow traversing the anterior part of right parotid gland running anteroinferiorly and reaching the masseter muscle as shown by the arrow.
As suggested by the CT reports, a diagnosis of FB impaction in the right parotid gland was made. The patient was scheduled for exploration with/without right superficial parotidectomy under general anaesthesia. The patient was started on empirical IV clindamycin in appropriate dosage and pus was sent for culture and sensitivity.
After lignocaine with adrenaline infiltration at the incision site, modified Blaire’s incision was made. As soon as the flap was raised, blackish tip of the FB was visualized at the superficial surface of the superficial lobe. On further exploration, it was going anteriorly and medially. The FB was grasped with an artery forceps and removed gently taking care not to further injure the surrounding tissues. As soon as the FB was removed, pus exuded from the tract. The tract was flushed with povidine iodine diluted with normal saline followed by normal saline multiple times until no further pus or debris was visible. The gland was also palpated for any remnant FB. As the wash was clear and no FB was palpable anymore, we decided not to perform superficial parotidectomy. A number 10 romovac drain was placed, secured, wound closed in layers and dressing applied. There was no unusual bleeding during the entire procedure. The FB was approximately 5× 0.5-cm-black pencil-shaped wooden splinter with pointed end piercing the gland and reaching up to the masseter muscle. It was removed in one piece (Image 4).

Black wooden foreign body after removal from the right parotid gland measuring 5 cm in length.
Ipsilateral facial nerve branches evaluated postoperatively were intact. The postoperative period was uneventful. The patient completed 1 week of IV antibiotics. Drain was removed on the third postoperative day and sutures were removed on the seventh postoperative day. Pus culture showed no growth. He was called on follow-up after 1 week of discharge and 1 month of surgery. The wound had healed completely and there was no salivary fistula or facial weakness on both the follow-ups.
Discussion
FB retention in the parotid gland due to penetrating injury is a rare clinical entity. 6 The first published case was in 1958. 7 Different materials such as metal, wood, glass, pencil tip, toothbrush bristle, fish bone, hair, grass and seed have been reported in the literature.3,8–10
Parotid gland FBs are caused either by retrograde migration through stensen’s duct or by direct penetration through the skin.3,8 In our case, like most other cases of FB in the parotid gland, the mechanism of entry of the FB seemed to be through direct skin penetration.
Radiographic imaging is often done to confirm the suspicion of a FB. However, appropriate imaging modality needs to be used. Ultrasonography can be preferred in appropriate cases but the experience of the radiologist performing ultrasonography may affect the result. 8 FBs with soft consistency can be confused with other parotid lesions. 10 A relatively shallow wooden FB which is not obscured by bone or gas may be detected by ultrasonography but it is not appropriate for detecting deeply lodged wooden FB. 5 Among the radiological investigations, computed tomography is the most valuable as it can help to detect deeply located foreign bodies, distinguish between different pathologies as well as plan the surgical procedure. Conventional radiographs are limited in use because all the FBs are not radiopaque. 11 Wide window width CT scan, which is usually the recommended modality, may reveal the characteristic striated appearance of wood.5,12 Elongated, well-defined areas of uniform attenuation or swelling of the deeper soft tissues may also give a clue to the presence of a wooden FB inside. 12 In our case, a CECT of the parotid gland was done to visualize the location and extent of the pus as well as the suspected foreign body.
In the differential diagnosis of parotid FBs, sialadenitis, sialolithiasis, mucous plugs and tumoral lesions should be considered. 13
Prophylactic antibiotics need to be started as wooden FB, being dirty, can be a nidus for growth of microorganisms. Agents with good anaerobic coverage such as clindamycin and metronidazole are preferred since these organisms are the ones most commonly isolated from wound cultures. 7 Being a frequent wood contaminant, Clostridium tetani should also be covered prophylactically to safeguard against tetanus. 11 Sometimes, wooden foreign bodies are associated with an aseptic inflammatory process leading to FB granuloma formation. 14
Treatment of penetrating FBs of the parotid gland is early surgical exploration. 3 Fistulation to the skin may occur in untreated cases. 10 Sialendoscopy has a well-recognized role in removal of parotid calculi but its role in foreign body retrieval has not been reported yet. 15 Removal of the foreign body presents a challenge. Formerly, traditional parotidectomy incision and identification of the facial nerve was undertaken before removal of the foreign body but nowadays, less invasive and gland sparing methods are preferred. 16
After removal of the FB, all the abscess cavities need to be drained followed by thorough irrigation of the wound. 7 We managed our case by following the above-mentioned principles leading to a quick and complication-free recovery.
Conclusion
FB, especially in an atypical location like the parotid gland, can be a diagnostic challenge. Thorough history taking complemented by appropriate imaging modality can help in prompt diagnosis, treatment and a complication-free recovery.
Footnotes
Acknowledgements
I would like to express my gratitude to my coauthor Dr Tulika Dubey for assisting me during the surgery and providing me the case related photographs and Dr Dipesh Shakya for helping me in writing this manuscript. I would also like to thank the radiologist as well as my scrub nurse, anaesthetist and the entire operation theatre staffs who assisted me in the diagnosis and treatment of my patient.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series
Informed consent
The written informed consent was taken from the patient’s daughter as she was the only family member available who could read and write (sign the consent form). However, the contents of the consent form were explained to the patient also.
