Abstract
A 24-year-old male presented with asymptomatic penile papules for 1 month. Dermatology examination showed pink, soft papules on the ventral side of the penis, with a clear boundary and rough surface, and papillary hyperplasia could be seen. Dermoscopy revealed multiple finger-like projections without vessels in the center of the lesion under polarized light, and linear and crown-like vessels could be seen at the edge of the lesion. Histopathological examination revealed endophytic infundibular hyperplasia with keratinocytes containing Henderson–Patterson bodies. A diagnosis of molluscum contagiosum was made. Molluscum contagiosum can present with several atypical presentations including giant, cystic, ulcerated, or condyloma acuminatum-like, especially in immunosuppressed patients. Here, we report a case of atypical genital molluscum contagiosum with novel dermoscopic findings in an otherwise-healthy adult.
Introduction
Molluscum contagiosum (MC) is an infectious dermatosis caused by molluscum contagiosum virus (MCV), frequently affecting children, sexually active adults, and immunocompromised individuals. 1 MC may have atypical presentations mimicking other conditions including warts, basal cell carcinoma, and intradermal nevus, especially in immunocompromised patients. 2 Dermoscopy can be a diagnostic tool in such cases. Here, we describe a case of atypical genital molluscum contagiosum with novel dermoscopic findings in an otherwise-healthy adult, which is rarely reported before.
Case
The patient was a 24-year-old male who presented with asymptomatic penile papules for 1 month, and he denied unprotected sexual contact before the onset of the lesions. Dermatology examination showed three pink, soft papules of 2–5 mm in size on the ventral side of the penis, with a clear boundary and rough surface, and papillary hyperplasia could be seen, with no umbilicated surface (Figure 1). Dermoscopy revealed multiple finger-like projections without vessels in the center of the lesion under polarized light, and linear and crown-like vessels could be seen at the edge of the lesion (Figure 2(a), under polarized light, ×65), while under unpolarized light, shiny finger-like projections could be seen, without umbilicated surface (Figure 2(b), under unpolarized light, ×65). Differential diagnoses of MC and condyloma acuminatum were considered. Blood tests for human immunodeficiency virus, syphilis, and hepatitis B and C were negative. The biggest lesion was excised for histopathological examination, and it revealed epidermal hyperkeratosis and endophytic infundibular hyperplasia with keratinocytes containing Henderson–Patterson bodies (Figure 3(a) and (b)). The diagnosis was MC. The residual lesions were removed by carbon dioxide laser, and the patient was followed up for 6 months without recurrence.

Clinical photo of pink, soft papules of 2–5 mm in size on the ventral side of the penis, with a clear boundary and rough surface with no umbilicated surface.
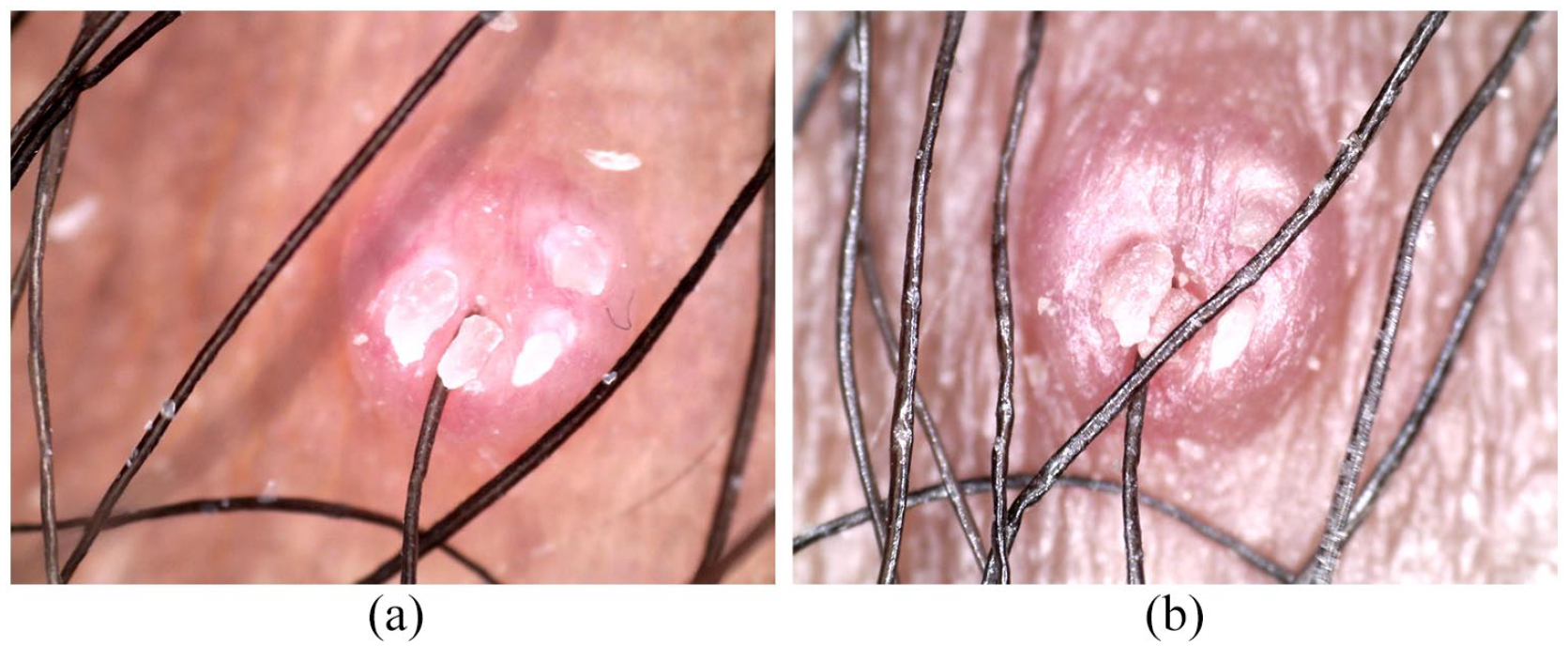
(a) Dermoscopy revealed multiple finger-like projections without vessels in the center of the lesion and linear and crown-like vessels at the edge of the lesion (under polarized light, ×65). (b) Dermoscopy revealed shiny finger-like projections without umbilicated surface (under unpolarized light, ×65).

(a) Histopathological examination of the lesion revealed epidermal hyperkeratosis and endophytic infundibular hyperplasia with keratinocytes containing Henderson–Patterson bodies (H&E staining, ×40). (b) Histopathological examination of the lesion revealed epidermal hyperkeratosis and endophytic infundibular hyperplasia with keratinocytes containing Henderson–Patterson bodies (H&E staining, ×100).
Discussion
MC is a benign cutaneous viral infection with an increasing incidence worldwide. In adults, the frequently affected areas are the lower abdomen, thighs, genitals, and perianal area, and most of the cases are transmitted by sexual contact. 1
The diagnosis of MC is often made clinically, with the characteristic lesions of dome-shaped, smooth-surfaced, pearly, skin-colored, or white papules with central umbilication and 2–5 mm in diameter. However, atypical presentations of MC can bring diagnostic challenges to clinicians. Atypical presentations may include giant, cystic, ulcerated, or condyloma acuminatum-like, and they tend to be discovered more in immunosuppressed patients, 2 while atypical MC in immunocompetent hosts was described as well. 3 In our case, the clinical presentation and the site of the lesions mimicked genital warts.
Dermoscopy can be very helpful in diagnosing clinically difficult cases. The characteristic findings of MC under the dermoscopy include a central pore or umbilication, polylobular or roundish white-to-yellow amorphous structures, accompanied with peripheral crown, punctiform or radial vascular patterns. 4 Different vascular patterns with or without an orifice detected at dermoscopy have been described before, which can assist the clinicians in the identification of MC lesions that are difficult to diagnose. 5 In the previous literature, both single and mixed vascular patterns have been reported, among which crown and crown plus radial arrangements were the most common patterns, respectively. White structures under dermoscopy were found in most lesions, including types of roundish, polylobular, four-leaved clover-like, and nonspecific. 4 In our case, only linear and crown-like vascular structures were seen, while there were no white-to-yellow amorphous structures, and finger-like projections resembling condyloma acuminatum could be seen, but there were no vessels observed in the projections. Histopathological examination revealed epidermal hyperkeratosis and endophytic infundibular hyperplasia with keratinocytes containing Henderson–Patterson bodies, which confirmed the diagnosis of MC. The finger-like projections without vessels revealed under dermoscopy may be explained by epidermal hyperkeratosis. The dermoscopic findings in this case mimicked genital warts and showed a novel dermoscopic feature of molluscum contagious that has never been described before. We reviewed the literature on dermoscopic features of genital warts, and the finger-like patterns of the genital warts under dermoscopy were mostly accompanied with hairpin, glomerular, or dotted vascular features within the finger-like projections. 6 We may speculate from our case that some atypical MC in genital areas can be verrucous-like and may also have finger-like projections under dermoscopy. But whether there are vascular structures in the projections may be the key to distinguish between genital warts and verrucous-like MC.
Conclusion
Atypical MC can also present in immunocompetent individuals, and MC in genital areas can be verrucous-like and imitate genital warts. Dermoscopy can be a helpful tool in diagnosing such cases, and whether there are vascular structures in the projections may be the key to distinguish between genital warts and verrucous-like MC under dermoscopy.
Footnotes
Acknowledgements
The study has obtained the patient’s consent, and we thank the patient’s cooperation during the treatment. The authors also thank the editors and reviewers for the valuable comments and suggestions.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent for the publication of the clinical details and images was obtained from the patient.
