Abstract
Fournier’s gangrene is a urologic emergency secondary to a necrotizing soft tissue infection. Fournier’s gangrene is characterized by severe pain and features of Fournier’s gangrene may include edema, blisters and bullae, crepitus, subcutaneous gas, and systemic symptoms. Risk factors include male gender, alcohol abuse, immunocompromised state, uncontrolled diabetes mellitus, obesity, and malignancy. The diagnosis is made clinically but is often supported by radiography, ultrasound, computed tomography, and magnetic resonance imaging. Treatment consists of emergent hospitalization and surgery to debride the necrotic tissues. Morbidity and mortality for Fournier’s gangrene are very high if left untreated. Early surgical intervention is key to the successful treatment of Fournier’s gangrene. This case report presents a case of Fournier’s gangrene mimicking acute epididymitis and highlights the importance of a thorough physical examination with high clinical suspicion for Fournier’s gangrene.
Introduction
Fournier’s gangrene (FG) is a rare surgical emergency secondary to a necrotizing soft tissue infection. Risk factors for FG include male gender, alcohol abuse, immunocompromised state, uncontrolled diabetes mellitus, obesity, and malignancy. FG is characterized by severe pelvic pain along with perineal skin changes and systemic symptoms including fever, hypotension, and tachycardia. Differential diagnoses include epididymitis, testicular torsion, inflammatory conditions, malignancy, and others.1–4 Imaging of soft tissue structures can be useful to identify deep tissue changes when skin is intact. 5
Treatment of FG consists of surgery to debride necrotic tissues.1,2 The morbidity and mortality for FG can reach 88% if left untreated. Early surgical intervention can decrease mortality by 50%. 1 In this case report, we present a case of FG mimicking acute epididymitis. This case highlights the importance of a thorough physical examination with high clinical suspicion of FG.
Case presentation
A 61-year-old male with a past medical history of diabetes mellitus, dyslipidemia, and hypertension presented to the emergency department (ED) with pain and swelling of the left scrotum for 48 h. The pain was constant, throbbing, and exacerbated by movement. It was localized to the posterior left hemi-scrotum with radiation to the right hemi-scrotum. The patient reported a 3-day history of subjective fever, chills, dysuria, urgency, frequency, and urinary retention. He denied any trauma to the scrotum and had no history of sexually transmitted infections.
On initial evaluation, his temperature was 98.7 F, blood pressure 156/60 mm Hg, heart rate 69 beats per minute, respiratory rate 18 breaths per minute, 98% oxygen saturation on room air. On physical examination, he was in no acute distress. Cardiac, respiratory, and abdominal examinations were unremarkable. Urogenital exam revealed swelling and erythema of the left hemi-scrotum and significant tenderness to palpation and swelling of the left epididymis. The penis was swollen and erythematous (Figure 1). There was no crepitus, bullae, blisters, or skin discoloration. Prehn sign was negative. Cremasteric reflex was absent bilaterally. Blue dot sign was negative.

Examination on admission to the hospital.
Initial serum labs showed a white blood cell (WBC) count of 29,600/μL with 91.2% neutrophils, hemoglobin 9.7 g/dL, glucose 244 mg/dL, blood urea nitrogen 39 mg/dL, creatinine 1.9 mg/dL, c-reactive protein (CRP) 27.2 mg/dL, and creatinine kinase 345 U/L. Urinalysis was cloudy, negative for leukocyte esterase and nitrites, with 4+ protein, 2+ glucose, 1.0 EU/dL urobilinogen, 3+ blood, negative for ketones, few red blood cells, and rare WBCs. HIV and RPR were negative. Blood and urine cultures were negative. Ultrasound of the scrotum and testicles revealed that the left epididymis was extremely complex and hyper vascular, possibly secondary to epididymitis. Testicular duplex showed a normal testicular duplex scan. FG severity index 7. 6
He was started on levofloxacin for suspected epididymitis. Urology was consulted and saw him 22 h after admission; he had developed a 3 cm necrotic lesion with fluctuance on the posterior aspect of the left hemi-scrotum. He was emergently taken for incision and drainage. The entire dartos fascia and the lower half of the scrotum were removed with a wide swathe of the perineal area, as shown in Figure 2. Quarter inch Penrose drains were placed bilaterally extending from the bilateral inguinal area to the dependent area of the wound in the perineum. IV antibiotics were changed to piperacillin-tazobactam and linezolid. Two days later, general surgery performed a diverting colostomy at the level of the sigmoid colon. This was completed to allow for adequate healing of the affected area. Urology then performed another debridement as the remaining scrotal skin edges were necrotic. A vacuum dressing, set at 125 mm Hg, was utilized for 12 days to decrease pressure over the wound, to gently extract fluids from the wound, to help pull the edges of the wound together, and to improve overall healing.
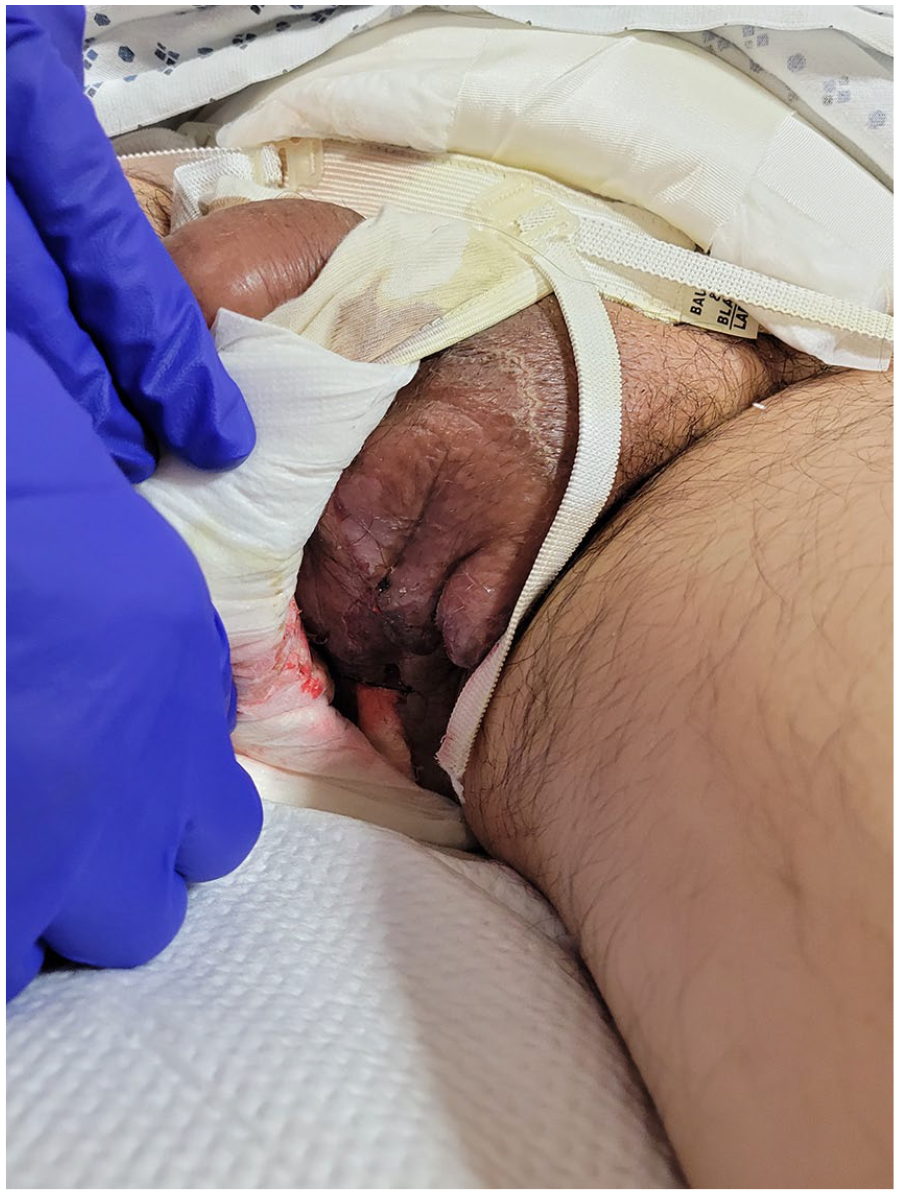
Examination following surgical debridement of Fournier’s gangrene.
Surgical tissue cultures were negative and gram stain showed rare gram-negative rods and rare gram-positive cocci. He was eventually switched to oral antibiotics (linezolid, levofloxacin, and metronidazole) and transferred to a subacute medical facility where he could undergo hyperbaric oxygen therapy. The patient has healed well with no complications and is scheduled for a colostomy reversal this month.
Discussion
This case highlights an atypical presentation of FG mimicking acute epididymitis. Acute epididymitis is classically described as slowly increasing pain with an average of 2–4 days from first symptoms to medical consultation.4,7 Physical examination findings include unilateral swelling and tenderness of the epididymis which can range from mild epididymal tenderness to severe systemic disease. Clinical and laboratory findings include fever, erythema of the scrotal skin, leukocytosis > 11,000/mm3, elevated CRP, urethritis (>4 WBCs/hpf), and involvement of the adjacent testis. Clinical findings are sufficient to diagnose epididymitis; however, ultrasound is important in severe cases, persistent disease, or unclear physical examination findings. In most patients with epididymitis, ultrasound reveals epididymal enlargement associated with epididymal hyper-perfusion.7–9 Escherichia coli and Chlamydia trachomatis are most common pathogens, and these should be considered when deciding on treatment. 10
Our patient presented with localized testicular pain, tenderness and swelling of the epididymis, secondary testicular pain, and scrotal wall edema and erythema with leukocytosis, elevated CRP, and urinalysis with leukocytes as well as ultrasound findings suggestive of acute epididymitis. The ultrasound did not show subcutaneous thickening, air, fascial fluid, “cobblestoning” of the subcutaneous soft tissue, or “snow globe” or “dirty shadowing,” or other signs suggestive of FG.1,5,9 Due to the severity of pain in a patient with multiple risk factors for FG, urology was urgently consulted.
When urology saw the patient 22 h later, he had developed a new necrotic lesion consistent with FG. This necrotic spot, also known as Brodie’s sign, is the first appearance of inflammation in FG. From there, necrosis spreads quickly along the fascial planes and causes rapid deterioration and progression to death if surgical debridement is delayed. 3 This case highlights the needs to keep a high suspicion for FG in patients with multiple risk factors presenting with severe scrotal pain. Our patient had multiple risk factors for FG including male sex, age greater than 50, diabetes, hypertension, and being overweight (body mass index (BMI): 29.7 kg/m2).1,3 In such patients when there is a high suspicion for FG, one must repeat physical examination frequently.
The only way to definitively diagnose FG is intra-operatively. The diagnosis can be difficult to make, especially in early-stage FG. Auerbach et al. report that FG is misdiagnosed in up to 75% of cases which leads to higher morbidity and mortality. 1 FG can begin as a simple abscess or cellulitis and rapidly progress to a necrotizing soft tissue infection involving necrosis of deep contiguous tissues and pelvic organs. With deep infections, there may not be any evidence of the infection on skin examination.1,3
Conclusion
This case illustrates the importance of continued assessment and physical examination and urgent treatment in a patient with severe scrotal pain. Our patient’s history, physical examination findings, and imaging results were suggestive of acute epididymitis but given his multiple risk factors, FG was maintained as a differential diagnosis. FG was diagnosed 22 h after admission, and he had a favorable outcome probably due to the early intervention.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
