Abstract
Fournier’s gangrene is characterized by an acute necrotic infection. The infection can occur in all parts of the body including the scrotum, penis, or perineum, and is a rare condition that is primarily reported in men and seldom in women. Existing literature suggests that it might be underreported, possibly leading to overlooked cases. Risk factors include diabetes, chronic illness, and trauma. This case involves a 52-year-old female with a 10-year medical history of diabetes mellitus, multiple healed skin lesions all over the body, and dermatitis. The presentation was a perianal swelling, which progressed into an extensive necrotizing soft tissue infection of the perineum, making a diagnosis of Fournier’s gangrene. She underwent wide local debridement and was managed with antibiotics in a timely manner. The patient’s clinical course and subsequent follow-up were uneventful. Uncontrolled diabetes and dermatitis significantly increase the risk of Fournier’s gangrene; therefore, it should be suspected in women with such comorbid conditions. This case highlights the need for increased awareness and vigilance regarding this condition among women.
Keywords
Introduction
Fournier’s gangrene (FG), an acute necrotic infection of the scrotum, penis, or perineum, is primarily associated with male patients according to the National Organization for Rare Diseases. 1 Causative organisms frequently documented in FG cases include Escherichia coli, Pseudomonas, and anaerobes, although cultures often reveal a mixture of aerobic and anaerobic organisms. While the condition predominantly affects males, it is noteworthy that FG does occur, although rarely, in females, with an incidence rate of 0.25 per 100,000 individuals. 2 Despite its rarity, FG in females is a condition that warrants attention. Patients with FG typically present with specific signs and symptoms, such as perineal swelling, pain, high-grade fever with rigors and chills, and in some cases, the formation of sinuses and foul serous discharge. Prompt recognition and appropriate management are crucial to prevent severe complications. FG can lead to severe complications, including widespread tissue necrosis, septic shock, and even mortality if not managed urgently. 1 Management includes resuscitation, broad-spectrum antibiotics, and emergency debridement. Early diagnosis and intervention are crucial to reduce mortality and improve outcomes. 1 To help improve the practices associated with this disease, we present a case of FG identified and successfully managed in a middle-aged female.
Case presentation
A 52-year-old female known case of diabetes mellitus for 10 years came via the outpatient department with a complaint of perianal swelling for the last 28 days. It was a bilateral painful swelling at the labia majora along with episodes of high-grade fever with rigors and chills. Initially, she went to another tertiary care hospital and was managed conservatively. No surgical intervention was done since the patient had raised blood sugars. Three days later, the swelling ruptured with purulent discharge. It was a tender swelling around the perianal region, more toward the left side with multiple sinuses and foul serous discharge (Figure 1). With these complaints, the patient landed in our outpatient department and was admitted to the surgical ward with the diagnosis of a perianal abscess. The patient developed multiple pustules on her anterior abdomen 12 years back which got ruptured on their own. Six months later, she developed a swelling on her left foot which was diagnosed as an abscess and surgically drained. The patient remained asymptomatic for 11 years until the presenting complaint started.
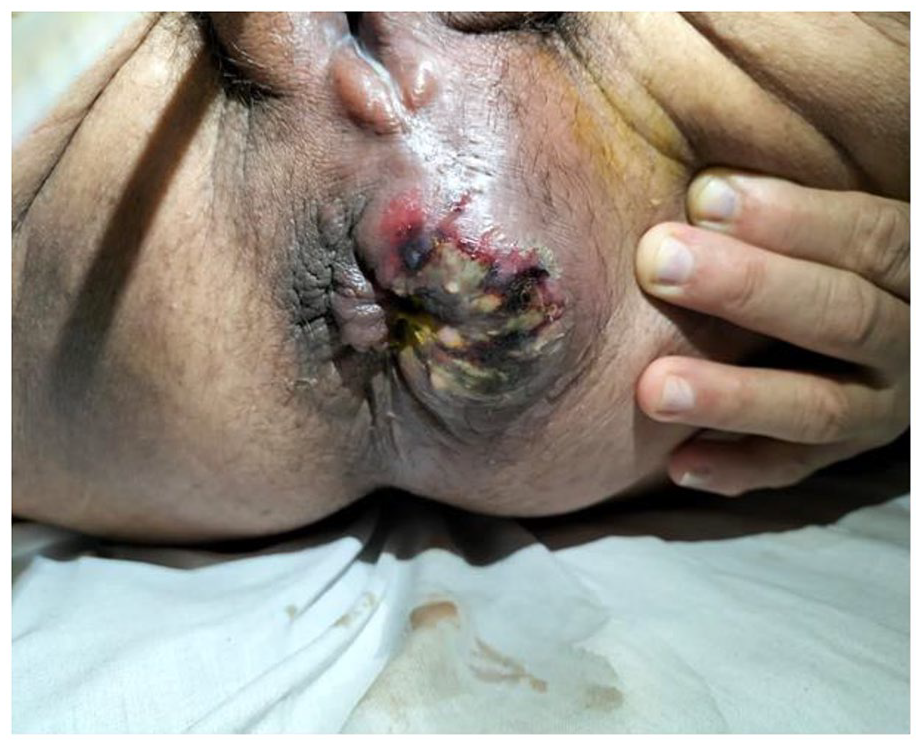
Presentation on admission shows a swelling at the perianal region more toward the left side with multiple sinuses and foul-smelling discharge.
She was kept on intravenous antibiotics and daily dressing with pyodine until she was optimized by the physician for surgery. On the second day of admission, during a dressing change, the presence of edema, erythema, and extensive area of necrosis of 2 cm × 1 cm was identified in the wound with no crepitation. The erythema, pain, and necrosis involved the perineum region (Figure 2). Therefore, based on these clinical findings and history, FG was diagnosed and the patient was urgently moved for wide local debridement and management. The serological indicators for hepatitis B, hepatitis C, and human immunodeficiency virus were all found to be non-reactive.

On the first post-admission day, a gangrenous patch was noted at the perineum with surrounding erythema.
After induction of spinal anesthesia, the patient was placed in a lithotomy position, and all aseptic measures were completed. Gangrenous skin with a necrotic patch extending from 12 to 3 o’clock with a small amount of pus was noted at the perineum. There was surrounding edema extending up to the left labia (Figure 2). An incision was made around the demarcation of the anal skin, just lateral to the anal sphincter. The pus was drained and an excision of gangrenous skin was done. Loculi were broken using finger manipulation and the cavity was washed with hydrogen peroxide and pyodine solution. Pyodine-soaked gauze was placed in the wound and an aseptic dressing was applied.
The patient was kept on an injection of linezolid 600 mg twice daily and the injection of metronidazole 500 mg twice daily for 2 days along with the daily dressing. Postoperatively, the wound healed with regular dressings, and no reconstruction was required. The patient was advised to strictly monitor blood glucose levels and seek medical consultation accordingly. In addition, she was advised to maintain proper hygiene. She was discharged on oral linezolid and metronidazole with daily dressing for 8 days. The wound was left open for healing by secondary intention. She was followed weekly for 3 weeks and had no further complications.
Discussion
FG is a life-threatening emergency that primarily affects men but rarely women. 3 The risk factors include uncontrolled blood sugar (20%–70%), alcohol (25%–50%), 4 intravenous drug abuse (if heroin is directly injected into the pelvic, penile, or inguinal veins), advanced age (50–79 years, affecting 3.3% of the population), obesity, immunosuppression (secondary to cancers), chronic illnesses, autoimmune diseases, and steroid therapy. 5 Several studies have shown that increasing patient age is the strongest independent predictor of mortality. 3 However, the manifestation of perianal abscess in the clinical picture can impede the timely suspicion of the severity of the condition. Hence, it is crucial to recognize such factors when assessing patient history in conjunction with the clinical presentation of FG.
Utilizing imaging modalities such as computed tomography and magnetic resonance imaging can aid in verifying deep tissue involvement, including the assessment of edema, fascia thickening, and the presence of gas. However, the procurement and waiting period for these procedures takes time. If timely diagnosis and interventions are not initiated, indications of sepsis may emerge, leading to a deterioration in the patient’s condition. 6 In this case report, given the urgent nature of the disease, the diagnostic suspicion of FG was primarily established based on the patient’s history and clinical and dermatological examinations. Therefore, it is imperative to document various clinical presentations of FG for future reference for early diagnosis and management.
This infection spreads along the pathway of the fascial planes, sparing the penile shaft (protected by the urethra and corpora cavernosa), while the scrotum is most commonly affected. It is believed that females are less prone to the disease due to a better drainage system in the pelvis. 7 However, in females, it may extend to the anterior abdominal wall, known as Colles’ fascia, which is not anteriorly attached, and this is referred to as Meleney’s gangrene. The perineum is the most commonly affected area by necrosis, which can extend to the thigh, inguinal region, buttocks, vulva, or perianal region due to the progression of urogenital or vulvar abscesses, bartholinitis, episiotomy, hysterectomy, abortions, and anorectal abscess. 8 Moreover, previous literature searches showed perianal involvement, which is an uncommon occurrence in females with FG.9,10 The typical initial presentation of perianal FG in females often comprises symptoms such as fever, perianal pain, extensive necrosis, and shock. 5 However, in our case, the perianal abscess progressed to perineum FG with edema and erythema extending up to the left labia. In males, testicular necrosis is rare due to the independent blood supply of the internal spermatic artery from the abdominal aorta. 11
The management is based on intensive care to maintain hemodynamic and respiratory stability and a synergistic broad-spectrum tri-antibiotic therapy. 11 Generally, double- or triple-combination therapy is recommended, which includes a third-generation cephalosporin, an aminoglycoside, and metronidazole. The existing literature supported the use of two antibiotics, namely linezolid and metronidazole, for the treatment of necrotizing fasciitis. Therefore in our case, the patient was started on this antibiotic combination as an initial treatment. Furthermore, these medications are not only cost-effective but also have minimal side effects, and they are readily accessible within our healthcare system. Furthermore, new drugs like meropenem and piperacillin–tazobactam can also be tried for better distribution with fewer chances of renal toxicity, 11 although treatment should be modified according to the culture results. 7 Urgent surgical exploration and aggressive debridement, up to the healthy bleeding margins, are the mainstays of treatment, along with thorough washing using hydrogen peroxide and betadine to reduce the incidence of recurrence. 12 The extensive debridement of necrotic tissue necessary in cases of FG often results in a significant skin defect. Patients undergoing this procedure may require multiple “relook” surgeries and additional debridement sessions. Finding a temporary solution for covering the open wound and reducing the risk of fecal contamination is important. 13 Therefore, we also used a technique involving lengths of povidone-iodine-soaked gauze rolls, placed in the wound, and provided an aseptic dressing. In addition, colostomies and urinary diversions by cystostomy or bladder catheterization are indicated in cases secondary to a urological cause, extensive perianal lesions, or those involving the anal sphincter.5,10 Repeated debridement and necrosectomy may be needed in the postoperative follow-up period. Various studies have reported 100% mortality without surgical debridement. 7
Postoperative management is based on daily dressing changes, maintaining effective antibiotic therapy adapted according to culture reports, and the use of hyperbaric oxygen therapy. 12 This helps limit the multiplication of anaerobic organisms, promotes phagocytosis, and improves the growth of fibroblasts and angiogenesis, leading to good healing. 11 After the resolution of the acute phase, the scrotum, known for its tremendous capacity to regenerate, can be allowed to heal via secondary intention. Reconstructive procedures, if indicated, can be performed during the same admission and must be completed within 37 days,7,11,12 with the primary concern being the closure of the scrotal defect. Skin grafts are avoided due to contraction and abrasion. 7 Negative pressure wound therapy is the most commonly applied method of dressing, providing physiological effects in wound healing, and can be applied when there is involvement of the scrotum, penis, abdomen, thigh, or perianal region. 5
The authors also found during the literature review that mortality is significantly higher among females (50% in females vs 7.7% in males), and patients with uncontrolled diabetes may be associated with a poor prognosis. 7 A decrease in the mortality rate in FG patients after hyperbaric oxygen therapy has also been reported. 11
Conclusion
In conclusion, suspicion and prompt treatment of FG in an immunocompromised woman with a history of diabetes and skin infections are essential for ensuring patient safety and improving outcomes. Given its rarity as a medical-surgical emergency, particularly in women, clinical diagnosis is crucial. Swift management, including resuscitation measures, broad and effective antibiotic therapy, and emergency debridement, plays a crucial role in reducing the risk of mortality.
Footnotes
Acknowledgements
None.
Author contributions
R.Z., A.M.A., M.F., and M.M.A. made substantial contributions to the conception and design of the work. All authors (A.M.S., M.A.R.K., and U.Y.) were involved in drafting the work and revising it critically for important intellectual content and final approval of the version to be published. They agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Availability of data and material
All data underlying the results are available as part of the article and no additional source data are required.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval to report this case was obtained from the Ethical Review Committee of the Department of Surgery, Hamdard University Hospital (Approval Number VP(C)/HCM&D/2022/063).
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
