Abstract
Necrotizing fasciitis is a rare and life-threatening soft-tissue infection characterized by rapidly spreading inflammation and subsequent necrosis of the fascial planes and surrounding tissue. These children should be managed promptly with broad-spectrum antibiotics and possible surgical debridement. Here, we present a 5-week-old female infant who presented with fever and ulcer on right lower jaw. She had a sudden onset of darkening of the right lower jaw, which progressed to reddish discoloration, and then an ulcer developed in the middle of this area of discoloration. She had a tender swelling extending from the right pre-auricular area to the right upper neck, crossing the right jaw and extending toward the right cheek and maxillary area. Swelling had areas of hyperpigmentation with an ulcer measuring 2 by 3 cm at the center of the lesion, oozing purulent fluid, and Staphylococcus aureus was cultured. The surgeons conducted incision and debridement in theater after suspecting necrotizing fasciitis of the jaw and the baby was kept on intravenous antibiotics, antiretroviral therapy and was dressed daily. The child fared well thereafter.
Introduction
Necrotizing fasciitis (NF) is a rare and life-threatening soft-tissue infection characterized by rapidly spreading inflammation and subsequent necrosis of the fascial planes and surrounding tissue. 1 It is mostly caused by toxin-producing virulent bacteria such as Group A streptococcus, Entero-bacterales and non-group A streptococci. 1 The global prevalence of NF is around 0.40 cases per 100,000 population. 2 It is very rare in children and particularly in infants. The incidence of NF in children is around 0.08 per 100,000 population. On the contrary, it has a fulminant course in children. 3 The most common site of involvement in pediatric patients is the abdominal wall, followed by the thorax, back, scalp and extremities. Head and neck involvement is rare. 4 There is no gender variation but occurs slightly more often in males.5,6 Despite Staphylococcus aureus being an uncommon cause of NF, there have been reports of an alarming number of these infections caused by community-associated methicillin-resistant S. aureus (MRSA). 7 There are no similar cases of infant NF that have been reported in Tanzania. Here, we describe the course of illness and management of NF in an immunocompromised infant.
Case presentation
A 5-week-old female infant was admitted to the pediatric intensive care unit (ICU) with complaints of fever and ulcer on right lower jaw for 4 days. She had a sudden onset of darkening of the right lower jaw skin, which progressed to reddish discoloration, and then an ulcer developed in the middle of this area. Progressively, a hard, tender, warm swelling of the right lower jaw extending to the cheek, preauricular and neck region was noted along with serosanguinous extravasation on the ulcer bed. High-grade fever of 40°C without neurological deficits was associated with this presentation. The baby was born through vaginal delivery weighing 3 kg at birth to a HIV-positive mother who has been on antiretroviral therapy (ART) combination of tenofovir, lamivudine and efavirenz for 8 years. The baby was initiated on prophylactic nevirapine since birth.
On admission, the baby was conscious, ill-looking, mildly pale, and dyspneic with labored breathing and oral thrush. Her anterior fontanelle was bulging, measuring 6 by 6 cm with separation of sutures. On local examination, she had a tender swelling extending from the right pre-auricular area to the right upper neck, crossing the right jaw and extending toward the right cheek and maxillary area. Swelling had areas of hyperpigmentation with an ulcer measuring 2 by 3 cm at the center of the lesion and oozing serosanguinous discharge (Figure 1). On auscultation of the chest, there was a non-radiating grade 3 systolic murmur loudest at the left upper sternal border and bilateral fine crepitations. Baseline investigations done revealed a hemoglobin of 8.1 g/dL, which was microcytic and hypochromic. Liver enzymes, renal function tests and serum electrolytes were within normal range. Rapid antibody test serology for HIV was positive using dried blood spot (DBS) and analyzed by DNA polymerase chain reaction. Brain ultrasound revealed a mild hydrocephalus, Ultrasound of underlying soft tissues of the jaw showed features suggestive of an abscess. Echocardiogram showed an atrial-septal defect (ASD) of 5 mm with left to right shunt. Chest X-ray showed ground glass opacification of the right lung. There was no evidence of osteomyelitis on the X-ray of the jaw (Figure 2). Neck computed tomography scan could not be performed due to financial constraints. Blood culture and sensitivity isolated Staphylococcus aureus sensitive to clindamycin, gentamicin, meropenem and vancomycin and resistant to ceftriaxone and benzathine penicillin.
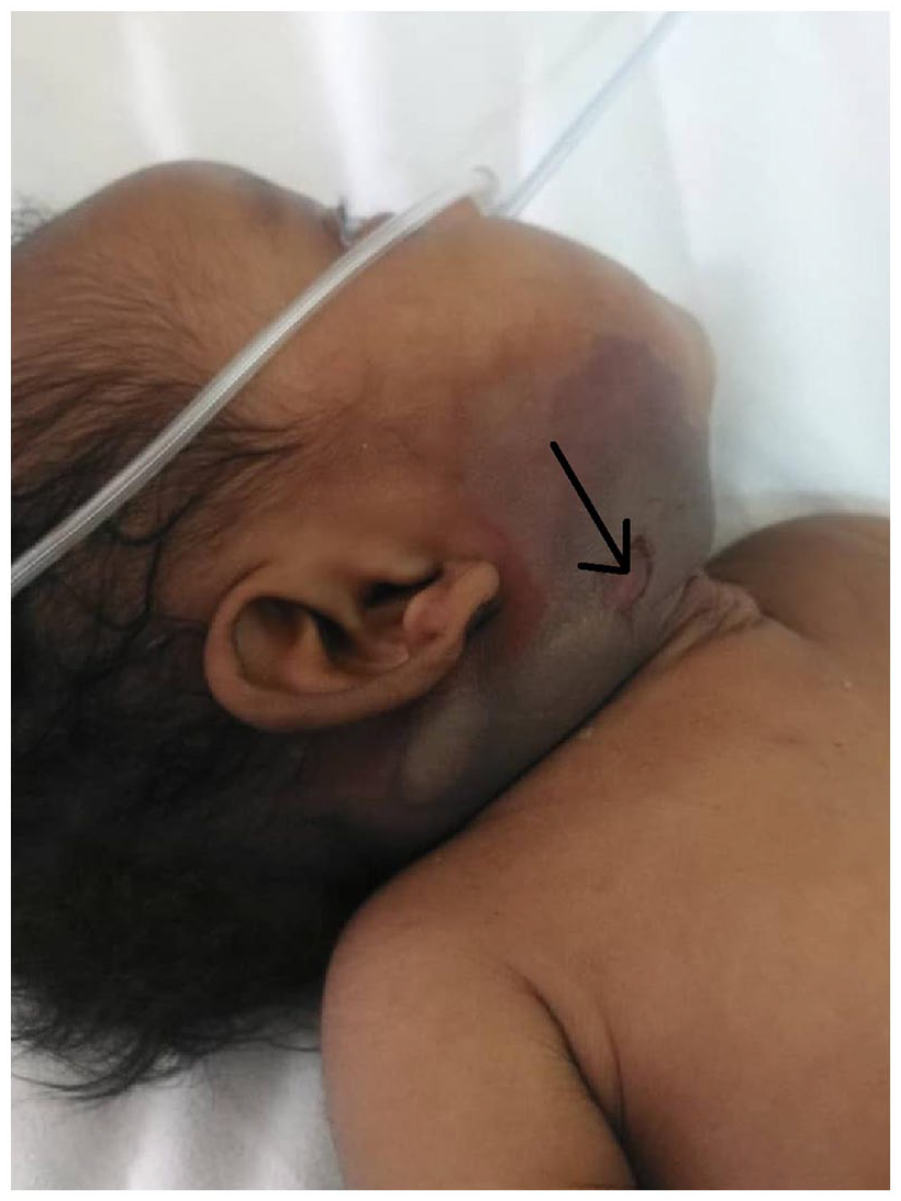
Hyperpigmented area with an ulcer (arrow).
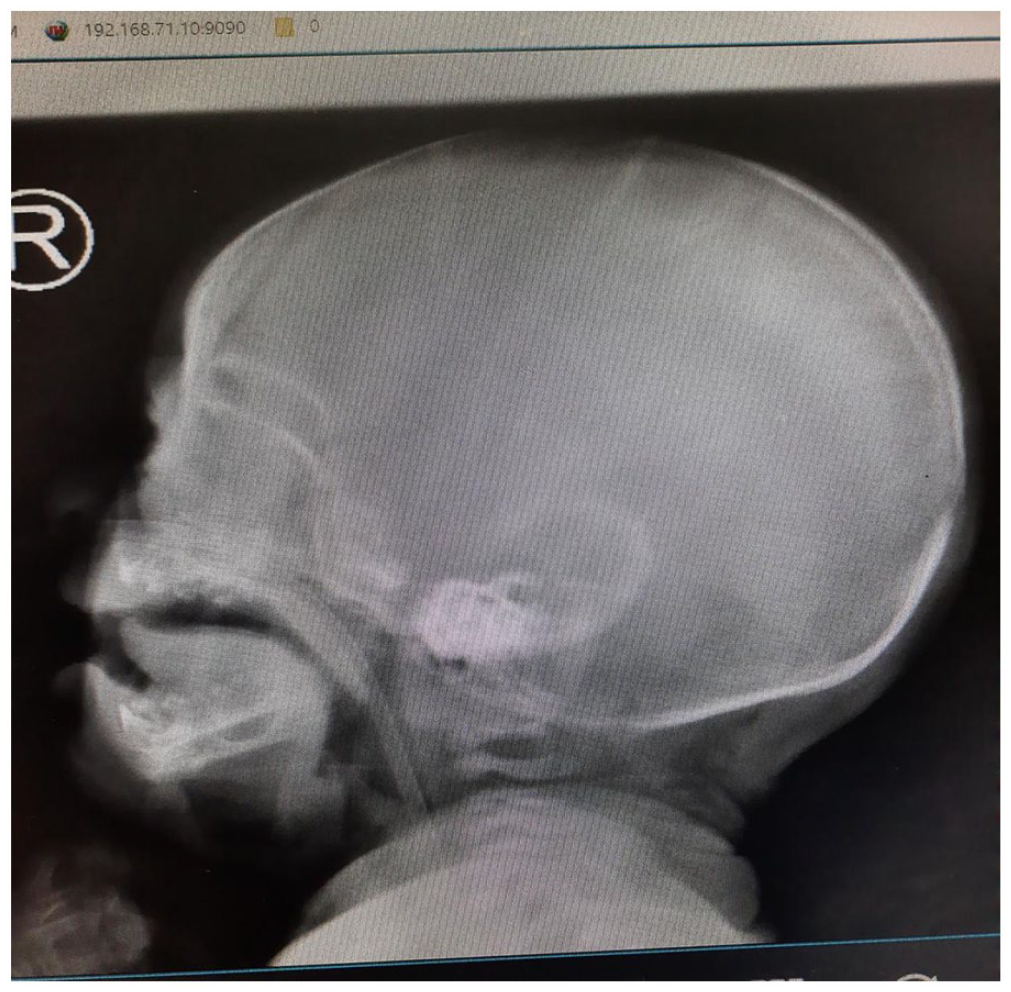
Normal jaw X-ray.
With the suspicion of NF of the jaw, surgical debridement under general anesthesia was carried out. Necrotic skin, and superficial and deep fascia were excised, leaving healthy looking tissues with fresh margins (Figure 3). Contents were sent for culture and sensitivity, which revealed S. aureus sensitive to ceftriaxone, gentamicin, meropenem, tetracycline and vancomycin (methicillin-susceptible S. aureus (MSSA)). There were no MRSA isolated.
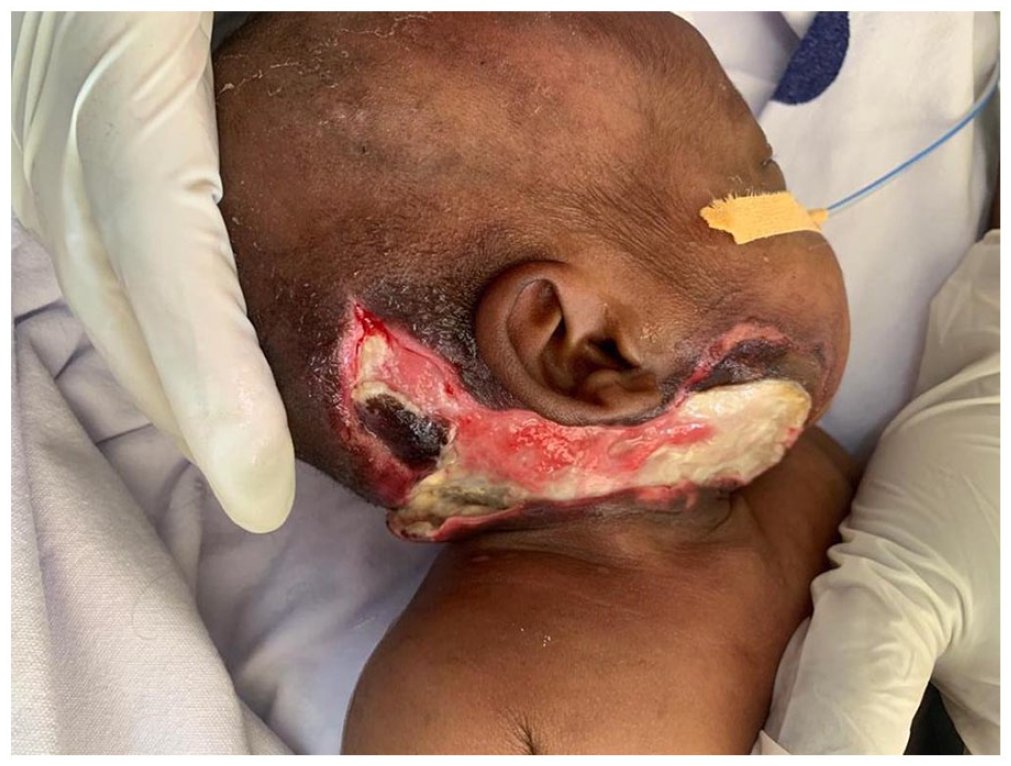
Post-surgical debridement.
The baby underwent an intensive medical management with our working diagnoses of pediatric AIDS, NF of the jaw, ASD, hydrocephalus and oral candidiasis. The baby was started on intravenous meropenem, metronidazole, furosemide, captopril, cotrimoxazole, oral miconazole and antiretroviral therapy combination of abacavir, lamivudine and lopinavir/ritonavir. In the subsequent days after debridement, the wound progressed well. Residual slough and minimal serosanguinous discharge were managed by a twice-daily wound dressing with diluted, one to nine parts, acetic acid. The baby completed medical therapy and continued with breast-feeding and ART. The wound had healthy granulation tissue (Figure 4). Currently, the baby is continuing with follow-up at outpatient unit and has been discharged from the ward due to financial constraints.

On-going dressing with dilute acetic acid.
Discussion
NF is associated with a high mortality rate, with estimates approximately 25% in children. 8 Cervical infection can be particularly devastating owing to mediastinal extension, which is associated with a high mortality rate.9,10 Contrast-enhanced computed tomography scan is particularly useful in identifying cervical disease and in delineating spread of infection, and early surgical debridement is the mainstay of treatment along with empirical antibiotic regimens to cover gram-positive, gram-negative and anaerobic bacteria pending culture results.4,8,11
NF was first recognized by Hippocrates in 500 BC and was termed by Wilson in 1950. 12 The common underlying predisposing factors for NF in children are omphalitis, balanitis, fetal scalp monitoring, post-surgical complication, necrotizing enterocolitis, bullous impetigo, maternal mastitis, septicemia, prematurity and immunodeficiency.12,13 The obvious reason in our case was the fact that the infant was born to an HIV-positive mother with transmission. Common pathogens are poorly understood and tend to be polymicrobial in nature, but the common ones include group B streptococcus, group A streptococcus and S. aureus; hence, empiric treatment with broad-spectrum antibiotics is needed. 13
Kumar et al. state that surgery should not be delayed after the diagnosis of NF is made; surgery was done as emergency in the index case. Debridement of the necrotic material was removed as reported by the authors. Nutrition is equally important in the healing process, and at times parenteral support is needed. 12 In another report by Gheuens et al., the authors also state and performed surgical debridement to obtain the best possible outcome. Although they isolated Streptococcus pyogenes which was different from our case and used vacuum-assisted dressing for wound closure, this was not available in our setting. 14 Clinicians can also opt for a less conservative approach, but this depends on the severity of the illness, extent of skin involved, progression of the pathology and response to the microbial therapy. 13
Conclusion
NF is an uncommon dangerous infection of the skin and subcutaneous tissue caused by bacteria. Aggressive antibiotics and surgical management are the mainstay of management.
Footnotes
Authors’ contributions
J.L. and D.M. conceptualized and drafted the manuscript. E.N., L. Laizer., L. Leonard and D.C. reviewed the patient records. All authors have read and approved the final script.
Availability of data and material
We have not shared patient’s hospital record as they contain personal identification information.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from a legally authorized representative(s)for anonymized patient information to be published in this article.
