Abstract
Necrotizing fasciitis is one of the most serious and deadly infections in surgery. The tissue defects that result after a severe infection with necrotizing fasciitis are often not easy to resolve surgically. The importance of this article is to show the reconstructive efficacy of the lotus petal flap based on two perforators. We present a 71-year-old female case with necrotizing fasciitis infection and defect of the region of the vulva (labia major) and perineum. We solved the reconstruction of the defect of the lower half of the labia major and the perineum, on the left side, by raising a fascio-cutaneous lotus petal flap along the gluteal fold, based on two perforators. Considering that the necrotizing fasciitis infection is very serious, it is also accompanied by large soft tissue defects. Raising the flap based on two perforators gives it greater vascular security and, at the same time, greater success in survival. We can conclude that the reconstruction of defects of the vulva and perineum with a lotus petal flap is a satisfactory solution and acceptable to the patient.
Introduction
Necrotizing fasciitis is one of the most serious infections in surgery, which manifests itself as an infection of the soft tissues, which includes wide anatomical surfaces, with high morbidity and mortality, and finally with large tissue defects that require surgical treatment.
Until now, many surgical techniques have been described for the closure and reconstruction of defects of the vulva and perineum, from direct closure to musculocutaneous flaps. For defects of the vulva, labia major, and perineum, a good choice is the lotus petal flap. The lotus petal flap is a fascio-cutaneous flap based on the rich network of perforating vessels of the internal and external pudendal arteries. 1 The design of the flaps resembles the petals of the lotus flower, and preferably use the lowermost petal flaps designed along the gluteal folds, relying on perforators of the internal pudendal artery. The flap is then raised including the fascia. This has been our current flap of choice for vulvovaginal reconstruction as it offers several advantages. 2 Overall, the lotus petal flap has lower complication rates at both the donor and the recipient site compared with the vertical rectus abdominis muscle flap. When both options seem viable, the lotus petal flap procedure may be preferred based on the reported lower complication rates. 3
Case report
The 71-year-old female patient presents with a defect in the soft tissues of the vulva (labia major) and perineum as a result of necrotizing fasciitis infection. The patient was admitted to our department with signs of necrotizing fasciitis infection in the region of the suprapubic, vulva, and perineum on the left side. She had about 15 years of diabetes mellitus and was treated with metformin tablets.
The patient’s signs of infection started about 2 weeks ago, in the form of pain in the left perineum, for which the patient was treated at the regional family outpatient clinic with antibiotics (amoxiclav) and analgesic (paracetamol). After 11 days, the patient goes again for a visit to the family doctor, who, after ascertaining that her condition has worsened, directs her to the University Clinical Center, in the Emergency Department, for further treatment. We visited there, and in the patient’s admission, we noticed signs of necrotizing fasciitis in the suprapubic, the perineal region, and the vulva on the left side. Due to uncontrolled diabetes, and a non-rigorous diet, the patient notices signs of infection. The patient on admission was in a serious general condition, with high temperature, fever, apathy, and lethargy, as the patient had difficulty communicating. To correct these laboratory values, we prescribed albumin, plasma, and an antibiotic (Imipenem) to the patient, for hyperglycemia, the endocrinologist was consulted who prescribes insulin. Immediately after admission to the ward, she is sent to the operating room, under general anesthesia, radical debridement of all soft tissues affected by the infection is performed, so the infected skin, subcutaneous tissue, and fascia are removed. In the operating room, before radical debridement, a swab is taken from the wound and sent to the microbiological laboratory for isolation of the cause and an antibiogram. After 3 days, from the microbiological laboratory, the result of the swab from the wound shows that the cause of the infection is

Defects of labia major and perineum after necrotizing fasciitis infection.
After 3 weeks of treatment, surgical intervention is indicated for the closure and reconstruction of the suprapubic region, labia major, and perineum defect. Suprapubic defect closed with direct closure. We decided to close the labia major and perineum defect by raising a lotus petal fascio-cutaneous flap. Initially, two skin perforators of a. pudenda interna are identified by a handheld Doppler device, on and around the ischiorectal fossa, which will determine the base of the flap (Figure 2).
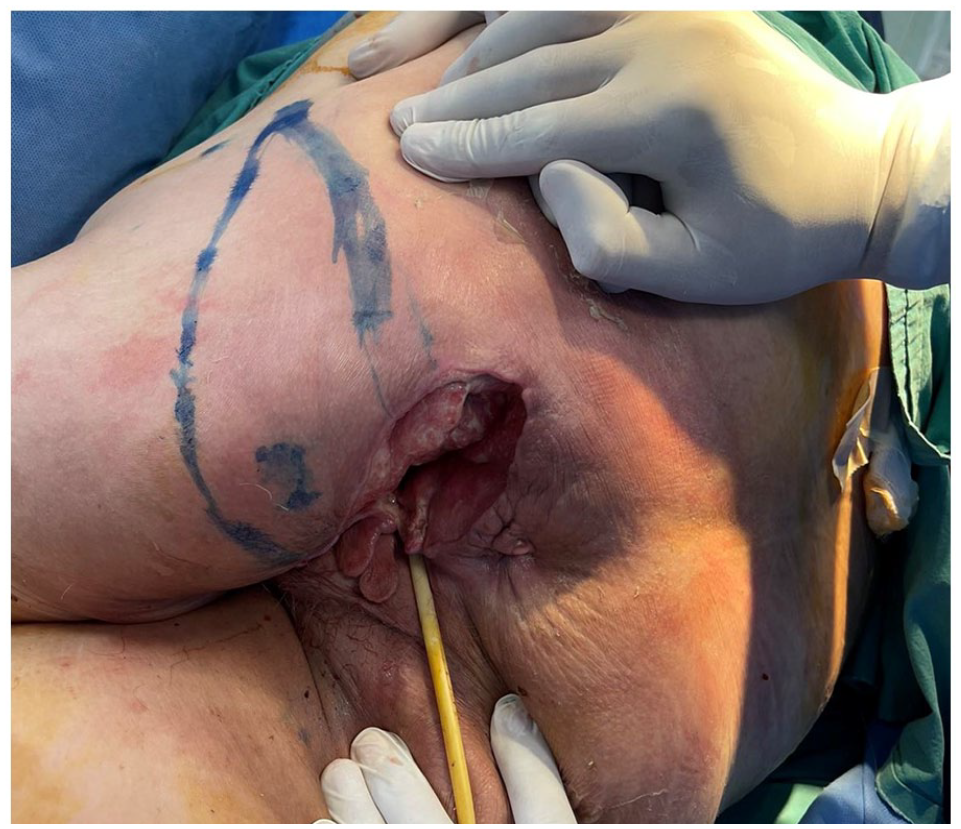
Marking the flap, and two skin perforators of a. pudenda interna.
Then the flap is drawn with a marker along the gluteal fold, adapting the dimensions to the defect of the labia major and the perineum, 15 × 7 cm. It continues with raising the flap by incising the skin, and subcutaneous tissue up to the fascia. The fascia is also incorporated into the flap and is incised along the edges of the flap to the lateral edge of the defect, preserving the two perforators at the base of the flap (Figure 3).

Full raising of the fascio-cutaneous lotus petal flap.
After raising in full fascio-cutaneous lotus petal flap, its rotation is done by 90°, and the covering of the defect of the lower half of the labia major and the perineum, a defect which was previously excised along its entire lips.
The flap is sutured with direct sutures, in two layers, without tension, drained, and the donor region is also closed primarily. The postoperative course of the flap was good, without complications. We have had no signs of infection or flap ischemia. Even after the operation, the flap remains well vascularized, which enables satisfactory healing of the wound (Figure 4). And 6 months after the operation, we see that the reconstruction of the labia major and the perineum with lotus petal flap gives a satisfactory reconstructive and aesthetic result, and is very acceptable by the patient (Figure 5).
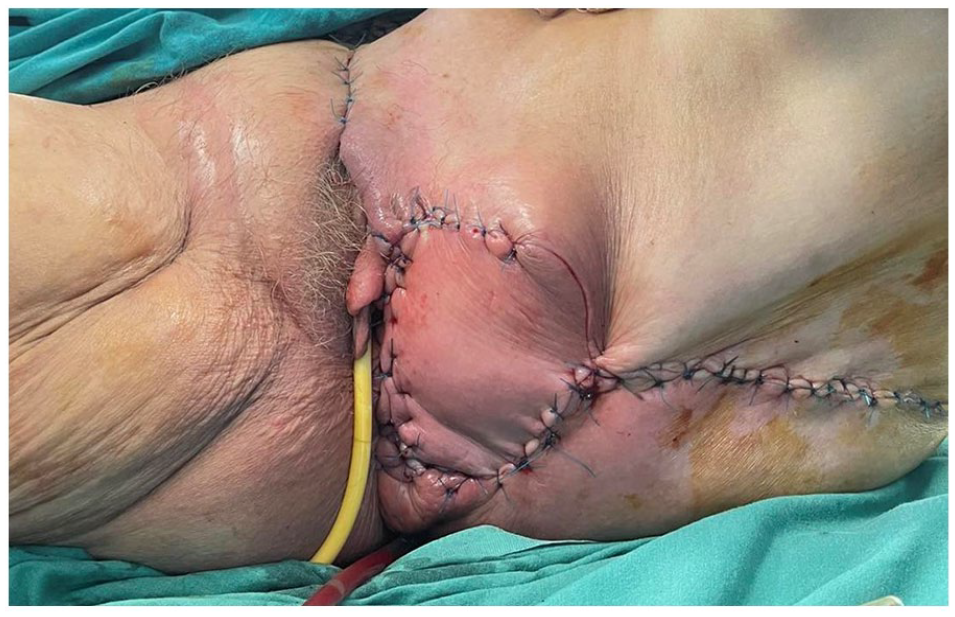
The clinical picture of the labia major reconstruction with lotus petal flap.

Flap appearance 6 months post-op.
Discussion
Considering that the necrotizing fasciitis infection is very serious, it is also accompanied by large soft tissue defects, at the same time in many body parts. Therefore, the closure and reconstruction of these defects is not an easy challenge for the plastic surgeon. Our patient with necrotizing fasciitis and soft tissue defects of the perineum and vulva, such as the genital and specific regions, required a more complicated reconstructive approach compared to the abdominal or femoral regions. This is explained by the fact that the vulva as a genital organ, to preserve the patient’s normal sexual life, is much more difficult to reconstruct and requires more complicated flaps in terms of their elevation.
The use of the lotus petal flap remains an effective solution in the reconstruction of labia major and perineum defects.
Many authors have presented cases of vulva and perineum reconstruction with this flap, especially in oncology patients with carcinoma of this region. Since the first presentation of the concept of designing flaps around the genital region by Horton in 1973, different variants of the lotus petal flap design have been presented. 4 Yii proposes “lotus petal” fascio-cutaneous flaps as one versatile alternative to the many flaps available in vulvovaginal reconstruction and flaps designed along the gluteal folds are recommended as offering good reconstructive results with minimal donor site morbidity. 2
We have used the lotus petal flap described according to Yii, which technique requires flap elevation with a perforator of the internal pudendal artery. 2 While the literature describes that the rise of the lotus petal flap is based on a perforator, we have applied the technique of harvesting the lotus petal flap with two perforators to close the defect. This technique with two flap perforators provides greater vascular safety and a much lower failure rate.
This vascular safety can also be considered an advantage of our technique with two perforators, but as a small disadvantage, it would be a limitation in its full rotation during the closure of the defect. Also, the reconstruction of the vulva with the lotus petal flap is easier, safer, and less bleeding, compared to the musculocutaneous flap reconstruction, in which reconstruction gives a larger shape and size (emphasis) to the vulva. Therefore, the reconstruction of the vulva with a lotus petal flap is much more aesthetically acceptable for the patient.
Herraiz Roda presented nine patients with vulvar carcinoma presenting the use of lotus petal supra fascial flap a simple procedure that can be done during the same surgery as the radical vulvectomy, improving the aesthetic results and reducing both the rate of complications and hospital stay. 5 While A. Giannini presented 62 patients surgically treated for vulvar cancer and closed these defects with V-Y fascio-cutaneous gluteal fold advancement flap. V-Y gluteal fold advancement technique is a safe procedure, performed in a single surgical session with minimal increase in surgical time and low wound healing complications. 6
All these modified lotus petal flap reconstruction techniques described by different authors present a modern achievement in the most advanced treatment of defects in the vulva-perineal region. This results in a good aesthetic result, which can also be seen in our technique, which satisfies both the patient and the surgeon. Also, this reconstructive technique can be used for people with female genital mutilation, which mutilation can be considered a serious violation of human rights.
Conclusion
Radical debridement is essential in the treatment of necrotizing fasciitis, and soft tissue defects created by this serious infection in the genital regions. The vulva requires reconstruction with flaps that adapt to the anatomical structure, tissue thickness, and skin color of the vulva.
We can conclude that the fascio-cutaneous lotus petal flap can be used quite successfully in the reconstruction of defects of the labia major and perineum as a result of necrotizing fasciitis infection. Our dual-perforator flap-raising technique provides high vascular safety and minimizes the possibility of flap failure. Likewise, the use of this flap gives quite acceptable and satisfactory reconstructive and aesthetic results from the patient’s side as well.
Footnotes
Acknowledgements
We thank all staff of the Clinic of Plastic Surgery for their technical support.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article.
