Abstract
Acute myocarditis is a rare complication of
Introduction
Bacteremia due to
Case presentation
A previously healthy 55-year-old female presented to our emergency department with 2-day history of severe, non-bloody, watery diarrhea associated with crampy abdominal pain. On examination, she was afebrile with a temperature of 36.5°C, heart rate of 95 beats per minute, and respiratory rate of 22 breaths per minute. She was hypotensive with a blood pressure of 86/47 mm Hg. Her abdomen was soft, with generalized tenderness, and cardiovascular and chest examinations were unremarkable. Laboratory values showed leukocytosis with a white blood cell (WBC) of 21.2 × 109/L (4.5–11 × 109/L), neutrophils of 19.44 × 109/L (1.8–7.7 × 109/L), high C-reactive protein of 262.69 mg/L (⩽5 mg/L), elevated creatinine of 256 µmol/L (44–80 µmol/L), urea of 14.50 mmol/L (2.8–8.1 mmol/L), and lactate of 2.65 mmol/L (⩽2.2 mmol/L). ECG done on admission showed normal sinus rhythm. The initial diagnosis was sepsis secondary to severe
The following morning, the patient spiked a temperature of 38.6°C associated with rigors and shortness of breath with a respiratory rate of 30 breaths per minute and oxygen saturation of 89%. Chest auscultation revealed bilateral crepitations, and the cardiovascular examination was unremarkable with no jugular venous distention. Chest X-ray showed pulmonary edema, ECG showed sinus tachycardia, and brain natriuretic peptide was 6217.0 ng/L (⩽287 ng/L). The patient was placed on Bilevel Positive Airway Pressure (BiPAP) and received one dose of furosemide 80 mg IV due to pulmonary edema and respiratory distress. Blood and urine cultures grew
The patient developed acute central chest pain 2 days post-admission, with diffuse ST-segment elevation (Figure 1), and a troponin T level of 0.791 µg/L (⩽0.014 µg/L), which raised a concern for acute ST-elevation myocardial infarction. The patient received a loading dose of aspirin (300 mg) and ticagrelor (360 mg) and underwent a coronary angiogram, which showed normal coronaries.

A 12-lead ECG showing diffuse ST-segment elevation.
A cardiac magnetic resonance imaging (CMRI) was suggested to rule out myopericarditis but was deferred due to the patient’s acute kidney injury. Over the course of the week, the patient’s condition improved with resolution of fever, dyspnea, and improvement in inflammatory markers and renal function. No inotropes were used as the patient continued to be hemodynamically stable. Antibiotics susceptibility showed pan-sensitive
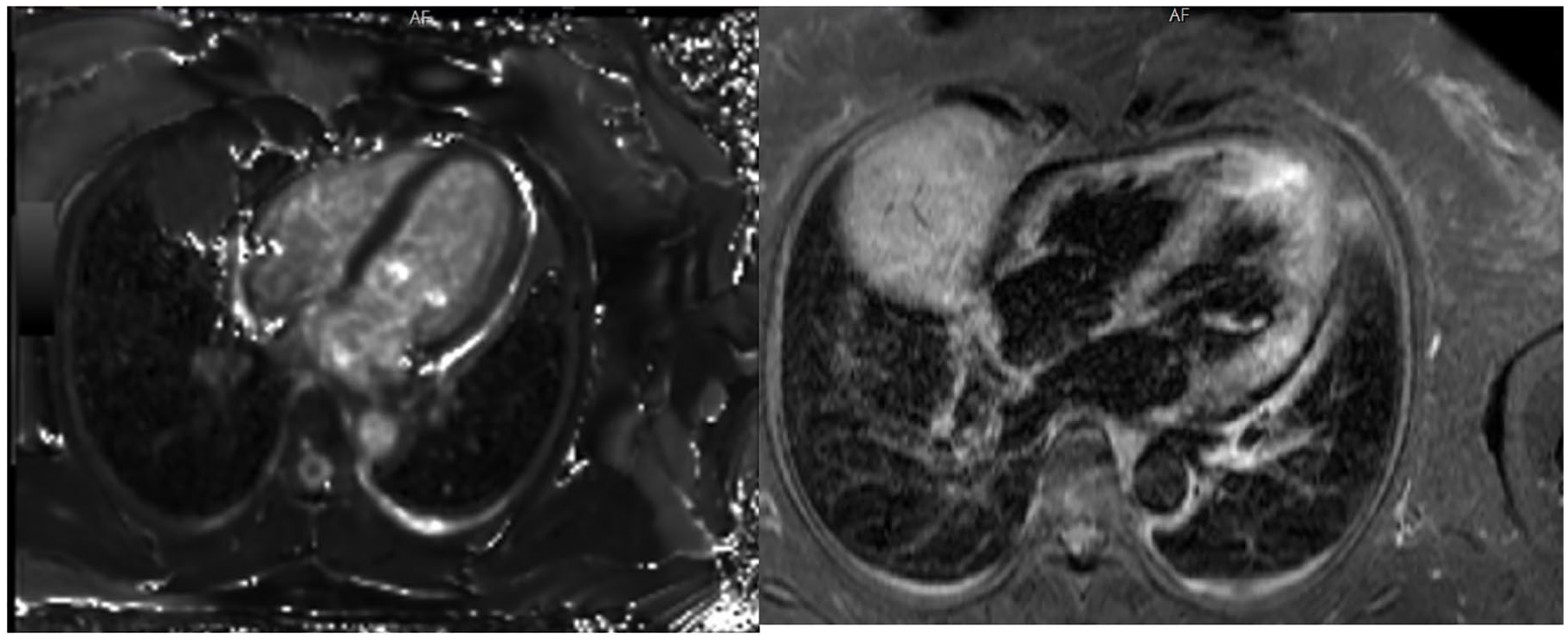
CMRI findings that are highly suggestive of inflammation involving the myocardium and pericardium.
The patient was discharged on the 8th day of admission after making a complete recovery, with a 2-week tapering dose of aspirin and a 3-month prescription for colchicine as a treatment for acute pericarditis. On follow-up 1-week post-discharge, the patient continued to do well with no recurrence of symptoms.
Discussion
Myopericarditis is a rare complication of
In an experiment done on mice mimicking septic shock, cardiomyocytes, which express TLR4 on their membranes, showed cardiac dysfunction after injection of LPS intraperitoneally. This interaction resulted in the production of proinflammatory cytokines, such as tumor necrosis factor-alpha (TNF-α) and interleukin-1β (IL-1β) that led to local inflammation and contractile dysfunction. 6
Our patient had sepsis secondary to
Myocarditis can have a wide range of clinical presentations, including chest pain, palpitations, dyspnea, and heart failure symptoms. A constellation of a typical clinical presentation of chest pain, with diffuse ST-segment elevation and PR-segment depression on ECG, elevation in inflammatory markers, and a normal coronary angiogram, often helps in making the diagnosis of myopericarditis. CMRI is a useful noninvasive imaging modality in identifying myocardial and pericardial disease.2,9
There are no specific guidelines for managing bacterial myopericarditis. Management of bacterial myopericarditis requires specific and appropriate management of the bacterial pathogen and sepsis, as well as supportive measures with the use of non-steroidal anti-inflammatory medications to reduce inflammation and control pain. 8
Conclusion
Myocarditis represents a rare complication of
Footnotes
Acknowledgements
The authors thank Dr. Jassin Hamed for his clinical assistance in managing the patient. They also thank Heart and Vascular Institute at Sheikh Khalifa Medical City for performing and providing the coronary angiogram images, and Radiology Department at Sheikh Khalifa Medical City for reporting the cardiac magnetic resonance imaging (CMRI) and providing the images.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval was obtained from Institutional Review Board at Sheikh Khalifa Medical City. Reference No. 07.12.2020 [RS-650].
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Consent
Patient’s written consent has been obtained before writing and submitting this manuscript.
